Abstract
Purpose
To investigate the relationship between preoperative and postoperative spinopelvic alignment and occurrence of DJK/DJF.
Study design/setting
This was a retrospective observational cohort study.
Patient sample
The sample included 40 patients who underwent posterior correction of SK from January 2006 to December 2014.
Outcome measures
Correlation analysis between the preoperative and postoperative spinopelvic alignment parameters and development of DJK over the course of the study period were studied.
Methods
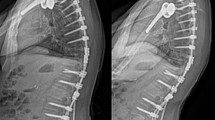
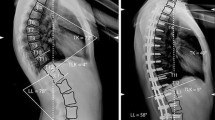
Whole spine X-rays obtained before surgery, 3 months after surgery and at the latest follow-up were analyzed. The following parameters were measured: maximum of thoracic kyphosis (TK), lumbar lordosis (LL), sagittal vertical axis (SVA), pelvic incidence (PI), pelvic tilt (PT), sacral slope (SS), lower instrumented vertebra (LIV) and LIV plumb line. Development of DJK was considered as the primary end point of the study. The patient population was split into a control and DJK group, with 34 patients and 6 patients, respectively. Statistic analysis was performed using unpaired t test for normal contribution and Mann–Whitney test for skew distributed values. The significance level was set to 0.05.
Results
DJK occurred in 15% (n = 6) over the study period. There was a significantly lower postoperative TK for the group with DJK (42.4 ± 5.3 vs 49.8 ± 6.7, p = 0.015). LIV plumb line showed higher negative values in the DJK group (−43.6 ± 25.1 vs −2.2 ± 17.8, p = 0.0435). Furthermore, postoperative LL changes were lower for the DJK group (33.84 ± 13.86% vs 31.77 ± 14.05, p < 0.0001.) The age of the patients who developed DJK was also significantly lower than that of the control group (16.8 ± 1.7 vs 19.6 ± 4.9, p = 0.0024.)
Conclusions
SK patients who developed DJK appeared to have a significantly higher degree of TK correction and more negative LIV plumb line. In addition, there may be a higher risk for DJK in patients undergoing corrective surgery at a younger age.


Similar content being viewed by others
References
Lowe TG, Line BG (2007) Evidence based medicine: analysis of Scheuermann kyphosis. Spine 32(19):S115–S119
Wood KB, Melikian R, Villamil F (2012) Adult Scheuermann kyphosis: evaluation, management, and new developments. J Am Acad Orthop Surg 20(2):113–121
Lowe T (1990) Scheuermann disease. J Bone Jt Surg Am 72(6):940–945
Hosman AJ, Langeloo DD, de Kleuver M, Anderson PG, Veth RP, Slot GH (2002) Analysis of the sagittal plane after surgical management for Scheuermann’s disease: a view on overcorrection and the use of an anterior release. Spine 27(2):167–175
Mehdian H, Khurana A, Stokes OM (2015) Posterior spinal fusion and correction of Scheuermann kyphosis. Eur Spine J 24(5):660–663
Coe JD, Smith JS, Berven S, Arlet V, Donaldson W, Hanson D, Mudiyam R, Perra J, Owen J, Marks MC (2010) Complications of spinal fusion for Scheuermann kyphosis: a report of the Scoliosis Research Society Morbidity and Mortality Committee. Spine 35(1):99–103
Cho K-J, Lenke LG, Bridwell KH, Kamiya M, Sides B (2009) Selection of the optimal distal fusion level in posterior instrumentation and fusion for thoracic hyperkyphosis: the sagittal stable vertebra concept. Spine 34(8):765–770
Denis F, Sun EC, Winter RB (2009) Incidence and risk factors for proximal and distal junctional kyphosis following surgical treatment for Scheuermann kyphosis: minimum five-year follow-up. Spine 34(20):E729–E734
Lowe TG, Kasten MD (1994) An analysis of sagittal curves and balance after Cotrel-Dubousset instrumentation for kyphosis secondary to Scheuermann’s disease: a review of 32 patients. Spine 19(15):1680–1685
Yanik HS, Ketenci IE, Coskun T, Ulusoy A, Erdem S (2016) Selection of distal fusion level in posterior instrumentation and fusion of Scheuermann kyphosis: is fusion to sagittal stable vertebra necessary? Eur Spine J 25(2):583–589
Sørensen KH (1964) Scheuermann's juvenile kyphosis: clinical appearances, radiography, aetiology, and prognosis. Munksgaard
Bradford DS (1977) Juvenile kyphosis. Clin Orthop Relat Res 128:45–55
Nasto LA, Perez-Romera AB, Shalabi ST, Quraishi NA, Mehdian H (2016) Correlation between preoperative spinopelvic alignment and risk of proximal junctional kyphosis after posterior-only surgical correction of Scheuermann kyphosis. Spine J 16(4):S26–S33
Geck MJ, Macagno A, Ponte A, Shufflebarger HL (2007) The Ponte procedure: posterior only treatment of Scheuermann’s kyphosis using segmental posterior shortening and pedicle screw instrumentation. J Spinal Disord Tech 20(8):586–593
Lonner BS, Newton P, Betz R, Scharf C, O’Brien M, Sponseller P, Lenke L, Crawford A, Lowe T, Letko L (2007) Operative management of Scheuermann’s kyphosis in 78 patients: radiographic outcomes, complications, and technique. Spine 32(24):2644–2652
Lowe TG, Lenke L, Betz R, Newton P, Clements D, Haher T, Crawford A, Letko L, Wilson LA (2006) Distal junctional kyphosis of adolescent idiopathic thoracic curves following anterior or posterior instrumented fusion: incidence, risk factors, and prevention. Spine 31(3):299–302
Sturm PF, Dobson JC, Armstrong GW (1993) The surgical management of Scheuermann’s disease. Spine 18(6):685–691
Arlet V, Aebi M (2013) Junctional spinal disorders in operated adult spinal deformities: present understanding and future perspectives. Eur Spine J 22(2):276–295
Yagi M, Akilah KB, Boachie-Adjei O (2011) Incidence, risk factors and classification of proximal junctional kyphosis: surgical outcomes review of adult idiopathic scoliosis. Spine 36(1):E60–E68
Lonner BS, Toombs CS, Guss M, Braaksma B, Shah SA, Samdani A, Shufflebarger H, Sponseller P, Newton PO (2015) Complications in operative Scheuermann kyphosis: do the pitfalls differ from operative adolescent idiopathic scoliosis? Spine 40(5):305–311
Lundine K, Turner P, Johnson M (2012) Thoracic hyperkyphosis: assessment of the distal fusion level. Glob Spine J 2(02):065–070
Papagelopoulos PJ, Klassen RA, Peterson HA, Dekutoski MB (2001) Surgical treatment of Scheuermann’s disease with segmental compression instrumentation. Clin Orthop Relat Res 386:139–149
Schwab F, Lafage V, Boyce R, Skalli W, Farcy J-P (2006) Gravity line analysis in adult volunteers: age-related correlation with spinal parameters, pelvic parameters, and foot position. Spine 31(25):E959–E967
Schwab F, Patel A, Ungar B, Farcy J-P, Lafage V (2010) Adult spinal deformity—postoperative standing imbalance: how much can you tolerate? An overview of key parameters in assessing alignment and planning corrective surgery. Spine 35(25):2224–2231
Boulay C, Tardieu C, Hecquet J, Benaim C, Mouilleseaux B, Marty C, Prat-Pradal D, Legaye J, Duval-Beaupère G, Pélissier J (2006) Sagittal alignment of spine and pelvis regulated by pelvic incidence: standard values and prediction of lordosis. Eur Spine J 15(4):415–422
Roussouly P, Gollogly S, Berthonnaud E, Dimnet J (2005) Classification of the normal variation in the sagittal alignment of the human lumbar spine and pelvis in the standing position. Spine 30(3):346–353
Duval-Beaupere G, Marty C, Barthel F, Boiseaubert B, Boulay C, Commard M, Coudert V, Cosson P, Descamps H, Hecquet J (2002) Sagittal profile of the spine prominent part of the pelvis. Stud Health Technol Inform 88:47
Vialle R, Levassor N, Rillardon L, Templier A, Skalli W, Guigui P (2005) Radiographic analysis of the sagittal alignment and balance of the spine in asymptomatic subjects. J Bone Jt Surg 87(2):260–267
Legaye J, Duval-Beaupere G, Hecquet J, Marty C (1998) Pelvic incidence: a fundamental pelvic parameter for three-dimensional regulation of spinal sagittal curves. Eur Spine J 7(2):99–103
Roussouly P, Gollogly S, Noseda O, Berthonnaud E, Dimnet J (2006) The vertical projection of the sum of the ground reactive forces of a standing patient is not the same as the C7 plumb line: a radiographic study of the sagittal alignment of 153 asymptomatic volunteers. Spine 31(11):E320–E325
Lafage R, Schwab F, Challier V, Henry JK, Gum J, Smith J, Hostin R, Shaffrey C, Kim HJ, Ames C (2016) Defining spino-pelvic alignment thresholds: should operative goals in adult spinal deformity surgery account for age? Spine 41(1):62–68
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that there is no conflict of interest.
Additional information
A. Ghasemi and T. Stubig contributed equally to this work.
An erratum to this article is available at http://dx.doi.org/10.1007/s00586-017-4994-x.
Rights and permissions
About this article
Cite this article
Ghasemi, A., Stubig, T., A. Nasto, L. et al. Distal junctional kyphosis in patients with Scheuermann’s disease: a retrospective radiographic analysis. Eur Spine J 26, 913–920 (2017). https://doi.org/10.1007/s00586-016-4924-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-016-4924-3