Abstract
Purpose
To identify the factors that may affect outcome in C-ADR and provide the pooled results of postoperative success rate of implanted segment range of motion (ROM), incidence of heterotopic ossification (HO), incidence of radiographic adjacent segment degeneration (r-ASD)/adjacent segment disease (ASD), and surgery rate for ASD.
Methods
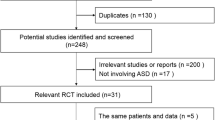
We systematically searched in PubMed, Embase, Cochrane library and Web of knowledge from 2001 to May 2015. Two independent reviewers screened the primary records. Eleven questions regarding the effect of patient selection issues and radiographic parameters issues on outcome were posed previously. Studies addressing the framed questions were included for analysis.
Results
Twenty-two studies were included for the final analysis. Results showed that number of surgical level (single versus double-level) had no effect on primary clinical outcome and radiographic outcome, surgical level had no effect on clinical and radiographic outcome, and smoking habits had negative effect on clinical outcome. No evidence for the effect of patient’s age and pathology category (radiculopathy or myelopathy) on outcome was found. The overall success rate of ROM was 79.4 %. ROM of the implanted segment and cervical sagittal alignment had no effects on clinical outcome. The pooled incidences of grade 1–4 HO and grade 3–4 HO were 27.7 and 7.8 %, respectively. The pooled incidence of r-ASD and surgery rate for ASD were 42.4 and 3.8 %, respectively.
Conclusions
The available evidence showed that most of the pre-selected factors had no effect on outcome after C-ADR, and the ROM success rate, incidence of HO and r-ASD/ASD, and surgery rate for ASD are acceptable. There is a lack of evidence from RCTs for some factors.






Similar content being viewed by others
References
Acosta FL Jr, Ames CP (2005) Cervical disc arthroplasty: general introduction. Neurosurg Clin N Am 16:603–607
Jawahar A, Cavanaugh DA, Kerr EJ 3rd, Birdsong EM, Nunley PD (2010) Total disc arthroplasty does not affect the incidence of adjacent segment degeneration in cervical spine: results of 93 patients in three prospective randomized clinical trials. Spine J 10:1043–1048
Zindrick MR, Tzermiadianos MN, Voronov LI, Lorenz M, Hadjipavlou A (2008) An evidence-based medicine approach in determining factors that may affect outcome in lumbar total disc replacement. Spine 33:1262–1269
Liao Z, Gao R, Xu C, Li ZS (2010) Indications and detection, completion, and retention rates of small-bowel capsule endoscopy: a systematic review. Gastrointest Endosc 71:280–286
Skeppholm M, Lindgren L, Henriques T, Vavruch L, Löfgren H, Olerud C (2015) The Discover artificial disc replacement versus fusion in cervical radiculopathy-a randomized controlled outcome trial with 2-year follow-up. Spine J [Epub ahead of print]
Bae HW, Kim KD, Nunley PD, et al (2015) Comparison of clinical outcomes of one and two-level total disc replacement: 4-year results from a prospective, randomized, controlled, multicenter ide clinical trial. Spine [Epub ahead of print]
Park JJ, Quirno M, Cunningham MR, Schwarzkopf R et al (2010) Analysis of segmental cervical spine vertebral motion after prodisc-C cervical disc replacement. Spine 35:E285–E289
Sasso RC, Metcalf NH, Hipp JA, Wharton ND, Anderson PA (2011) Sagittal alignment after Bryan cervical arthroplasty. Spine 36:991–996
Murrey D, Janssen M, Delamarter R et al (2009) Results of the prospective, randomized, controlled multicenter Food and Drug Administration investigational device exemption study of the ProDisc-C total disc replacement versus anterior discectomy and fusion for the treatment of 1-level symptomatic cervical disc disease. Spine J 9:275–286
Coric D, Nunley PD, Guyer RD et al (2011) Prospective, randomized, multicenter study of cervical arthroplasty: 269 patients from the Kineflex|C artificial disc investigational device exemption study with a minimum 2-year follow-up: clinical article. J Neurosurg Spine 15:348–358
Burkus JK, Traynelis VC, Haid RW Jr (2014) Mummaneni PV (2014) Clinical and radiographic analysis of an artificial cervical disc: 7-year follow-up from the Prestige prospective randomized controlled clinical trial: clinical article. J Neurosurg Spine 21:516–528
Hisey MS, Bae HW, Davis RJ et al (2015) Prospective, randomized comparison of cervical total disk replacement versus anterior cervical fusion: results at 48 months follow-up. J Spinal Disord Tech 28:E237–E243
Sasso RC, Best NM, Metcalf NH, Anderson PA (2008) Motion analysis of bryan cervical disc arthroplasty versus anterior discectomy and fusion: results from a prospective, randomized, multicenter, clinical trial. J Spinal Disord Tech 21:393–399
Xu JX, Zhang YZ, Shen Y, Ding WY (2009) Effect of modified techniques in Bryan cervical disc arthroplasty. Spine 34:1012–1017
Hisey MS, Davis RJ, Hoffman GA et al (2014) Sagittal alignment of one-level tdr and acdf patients: an analysis of patient outcomes from a randomized, prospective, clinical trial. Spine J 14:S124–S125
McAfee PC, Cunningham BW, Devine J, Williams E, Yu-Yahiro J (2003) Classification of heterotopic ossification (HO) in artificial disk replacement. J Spinal Disord Tech 16:384–389
Zhang X, Zhang X, Chen C et al (2012) Randomized, controlled, multicenter, clinical trial comparing BRYAN cervical disc arthroplasty with anterior cervical decompression and fusion in China. Spine 37:433–438
Phillips FM, Lee JY, Geisler FH et al (2013) A prospective, randomized, controlled clinical investigation comparing PCM cervical disc arthroplasty with anterior cervical discectomy and fusion. 2-year results from the US FDA IDE clinical trial. Spine 38:E907–E918
Zhang HX, Shao YD, Chen Y et al (2014) A prospective, randomised, controlled multicentre study comparing cervical disc replacement with anterior cervical decompression and fusion. Int Orthop 38:2533–2541
Kellgren JH (1957) Lawrence JS (1957) Radiological assessment of osteo-arthrosis. Ann Rheum Dis 16:494–502
Walraevens J, Liu B, Meersschaert J et al (2009) Qualitative and quantitative assessment of degeneration of cervical intervertebral discs and facet joints. Eur Spine J 18:358–369
Spivak JM, Delamarter RB, Murrey DB, Zigler JE, Janssen ME, Goldstein JA (2012) Adjacent level radiographic degenerative changes following single-level artificial disc replacement or ACDF at five- to seven- year follow-up. Spine J 12:S62
Hilibrand AS, Carlson GD, Palumbo MA, Jones PK, Bohlman HH (1999) Radiculopathy and myelopathy at segments adjacent to the site of a previous anterior cervical arthrodesis. J Bone Joint Surg Am 81:519–528
Nunley PD, Jawahar A, Cavanaugh DA, Gordon CR, Kerr EJ 3rd, Utter PA (2013) Symptomatic adjacent segment disease after cervical total disc replacement: re-examining the clinical and radiological evidence with established criteria. Spine J 13:5–12
Sasso RC, Anderson PA, Riew KD, Heller JG (2011) Results of cervical arthroplasty compared with anterior discectomy and fusion: four-year clinical outcomes in a prospective, randomized controlled trial. J Bone Joint Surg Am 93(18):1684–1692
Upadhyaya CD, Wu JC, Trost G et al (2012) Analysis of the three United States Food and Drug Administration investigational device exemption cervical arthroplasty trials. J Neurosurg Spine 16(3):216–228
Delamarter RB, Zigler J (2013) Five-year reoperation rates, cervical total disc replacement versus fusion, results of a prospective randomized clinical trial. Spine 38(9):711–717
Coric D, Kim PK, Clemente JD, Boltes MO, Nussbaum M, James S (2013) Prospective randomized study of cervical arthroplasty and anterior cervical discectomy and fusion with long-term follow-up: results in 74 patients from a single site. J Neurosurg Spine 18:36–42
Blumenthal SL, Ohnmeiss DD, Guyer RD, Zigler JE (2013) Reoperations in cervical total disc replacement compared with anterior cervical fusion: results compiled from multiple prospective food and drug administration investigational device exemption trials conducted at a single site. Spine 38:1177–1182
Myer J, Beutler W, McConnell JR, Lindley JG (2014) The incidence of symptomatic adjacent segment disease requiring treatment: cervical arthroplasty versus ACDF. Spine J 14:S160
Cepoiu-Martin M, Faris P, Lorenzetti D, Prefontaine E, Noseworthy T, Sutherland L (2011) Artificial cervical disc arthroplasty: a systematic review. Spine 36:E1623–E1633
Chen J, Wang X, Bai W, Shen X, Yuan W (2012) Prevalence of heterotopic ossification after cervical total disc arthroplasty: a meta-analysis. Eur Spine J 21:674–680
Gao Y, Liu M, Li T, Huang F, Tang T, Xiang Z (2013) A meta-analysis comparing the results of cervical disc arthroplasty with anterior cervical discectomy and fusion (ACDF) for the treatment of symptomatic cervical disc disease. J Bone Joint Surg Am 95:555–561
Zhou HH, Qu Y, Dong RP, Kang MY, Zhao JW (2015) Does heterotopic ossification affect the outcomes of cervical total disc replacement? A meta-analysis. Spine 40:E332–E340
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Additional information
C. Shi and J. Kang contributed equally to this work and should be considered as Co-first author.
C. Yang and R. Gao contributed equally to this work and should be considered as Co-corresponding author.
Rights and permissions
About this article
Cite this article
Kang, J., Shi, C., Gu, Y. et al. Factors that may affect outcome in cervical artificial disc replacement: a systematic review. Eur Spine J 24, 2023–2032 (2015). https://doi.org/10.1007/s00586-015-4096-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-015-4096-6