Abstract
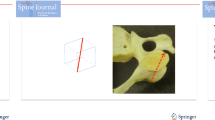
Different methods of lateral mass screw placement in the cervical spine have been described with separate trajectories for each technique in the sagittal and parasagittal planes. In the latter, plane 30° has been recommended in the modified Magerl’s technique as the optimum angle to avoid injury to the vertebral artery and nerve root. The estimation of this angle remains arbitrary and very much operator dependant. The aim of this study was to assess how accurately the lateral trajectory angle of 30° is achieved by visual estimation amongst experienced surgeons in a tertiary spinal unit and to determine the likelihood of neurovascular injury during the procedure. We chose an anatomical ‘sawbone’ model of the cervical spine with simulated lordosis. The senior author marked the entry points. Five spinal consultants and five senior spinal fellows were asked to insert 1.6-mm K wires into the lateral masses of C3 to C6 bilaterally at 30° to the midsagittal plane using the marked entry points. The lateral angulation in the transverse plane was measured using a custom protractor and documented for each surgeon at each level and side. The mean and standard deviation (SD) of the data were obtained to determine the inter observer variability. Utilising this data, measurements were then made on a normal axial computerised tomography (CT) scan of the cervical spine of an anonymous patient to determine if there would have been any neurovascular compromise. Among the 10 surgeons, a total of 80 insertion angles were measured from C3 to C6 on either side. The overall mean angle of insertion was 25.15 (range 20.4–34.8). The overall SD was 4.78. Amongst the 80 measurements between the ten surgeons, two episodes of theoretical vertebral artery violation were observed when the angles were simulated on the CT scan. A moderate but notable variability in trajectory placement exists between surgeons during insertion of cervical lateral mass screws. Freehand estimation of 30° is not consistently achieved between surgeons and levels. In patients with gross degenerative or deformed cervical spine anatomy, this may increase the risk of neurovascular injury. The use of the ipsilateral lamina as an anatomical reference plane is supported.


Similar content being viewed by others
References
Roy-Camille R, Saillant G, Berteaux D, Serge MA (1989) Method of posterior screw placement techniques. In: McKibbin B (ed) Early management of spinal injuries: recent advances in orthopaedics. Churchill-Livingstone, Edinburgh, pp 57–87
Roy-Camille R, Saillant G, Mazel C (1989) Internal fixation of the unstable cervical spine by a posterior osteosynthesis with plates and screws. In: Cervical Spine Research Society (ed) The cervical Spine, 2nd edn. JB Lippincott, Philadelphia, pp 390–403
Bayley E, Zia Z, Kerslake R, Klezl Z, Boszczyk BM (2010) The lamina as a guide for safe lateral mass screw placement in the sub-axial cervical spine—a computerised tomography study. Eur Spine J 19(4):660–664
An HS, Gordin R, Renner K (1991) Anatomic considerations for plate screw fixation of the cervical spine. Spine 16(10S):S548–S551
Anderson PA, Henley MD, Grady MS, Montesano PX, Winn HR (1991) Posterior cervical arthrodesis with AO reconstruction plates and bonegraft. Spine 16(3):72–79
Ebraheim NA, Klausner T, Xu R, Yeasting RA (1998) Safe lateral mass screw lengths in the Roy-Camille and Magerl techniques. An anatomic study. Spine 23(16):1739–1742
Heller GD, Carlson JG, Abitbol JJ, Garfin S (1991) Anatomic comparison of the Roy-Camille and Magerl techniques for screw placement in the lower cervical spine. Spine 16:S552–S557
Xu R, Haman SP, Ebraheim NA, Yeasting RA (1999) The anatomic relation of lateral mass screws to the spinal nerves: a comparison of the Magerl, Anderson, and An techniques. Spine 24(19):2057–2061
Jeanneret B, Magerl F, Ward EH et al (1991) Posterior stabilization of the cervical spine with hook plates. Spine 16(Suppl):S56–S63
Merola AA, Castro BA, Alongi PR, Mathur S, Brkaric M, Vigna F, Riina JP, Gorup J, Haher TR (2002) Anatomic consideration for standard and modified techniques of cervical lateral mass screw placement. Spine J 2(6):430–435
Montesano PX, Juach EC, Anderson PA, Benson DR, Hanson PB (1991) Biomechanics of cervical spine internal fixation. Spine 16(Suppl):10–16
Ebraheim NA, Xu R, Stanescu S, Yeasting RA (1999) Anatomic relationship of the cervical nerves to the lateral masses. Am J Orthop 28(1):39–42
Heller JG, Silcox DH, Sutterlin CE (1995) Complications of posterior cervical plating. Spine 20(22):2442–2448
Xu R, Ebraheim NA, Klausner T, Yeasting RA (1998) Modified Magerl technique of lateral mass screw placement in the lower cervical spine: an anatomic study. J Spinal Disord 11(3):237–240
Seybold EA, Baker JA, Criscitiello AA, Ordway NR, Park CK, Connolly PJ (1999) Characteristics of unicortical and bicortical lateral mass screws in the cervical spine. Spine 24(22):2397–2403
Chin KR, Eiszner JR, Roh JS, Bohlman HH (2006) Use of spinous processes to determine drill trajectory during placement of lateral mass screws: a cadaveric analysis. J Spinal Disord Tech 19:18–21
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Pal, D., Bayley, E., Magaji, S.A. et al. Freehand determination of the trajectory angle for cervical lateral mass screws: how accurate is it?. Eur Spine J 20, 972–976 (2011). https://doi.org/10.1007/s00586-011-1694-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-011-1694-9