Abstract
Purpose
Chemotherapy-induced taste alteration is a side effect that can result in malnutrition and reduced quality of life in cancer patients. However, the underlying causes of this phenomenon remain unclear, and evidence-based treatments have not been established. This study focused on patients’ subjective symptoms of taste alterations aimed to explore how the sensitivity to basic tastes changes due to anticancer agents and how alterations in one taste perception are associated with changes in other tastes during chemotherapy.
Methods
A cross-sectional questionnaire-based interview survey was conducted on 215 patients undergoing chemotherapy. The subjective sensitivity to each basic taste was assessed using a visual analog scale, and the incidence of taste alterations due to different chemotherapy regimens was calculated. Multivariate logistic regression analysis was performed to determine whether there were associations between changes in one taste sensitivity and changes in other taste sensitivities.
Results
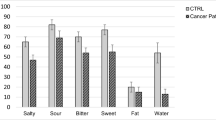
Approximately half (49.5%) of the patients experienced chemotherapy-induced taste alterations. An analysis of subjective changes in basic tastes revealed that the salt and umami taste systems were more sensitive to chemotherapy than other taste systems. Patients with altered sensitivity to sweet taste were significantly more likely to report altered sensitivity to salt, bitter, and sour tastes. Moreover, umami–salt and bitter–sour taste sensitivities were significantly related to each other.
Conclusion
This study suggests that changes in subjective sensitivities to one basic taste during chemotherapy may be accompanied by changes in other tastes in specific combinations. Considering taste associations in dietary guidance may help improve the nutritional status of cancer patients experiencing taste alterations due to chemotherapy.

Similar content being viewed by others
Data availability
The datasets analyzed during the current study are available from the corresponding author on reasonable request.
References
Mosel DD, Bauer RL, Lynch DP, Hwang ST (2011) Oral complications in the treatment of cancer patients. https://doi.org/10.1111/j.1601-0825.2011.01788.x
Hovan AJ, Williams PM, Stevenson-Moore P et al (2010) A systematic review of dysgeusia induced by cancer therapies. Support Care Cancer 18:1081–1087. https://doi.org/10.1007/s00520-010-0902-1
Zabernigg A, Gamper E-M, Giesinger JM et al (2010) Taste alterations in cancer patients receiving chemotherapy: a neglected side effect? Oncologist 15:913–920. https://doi.org/10.1634/theoncologist.2009-0333
Sánchez-Lara K, Sosa-Sánchez R, Green-Renner D et al (2010) Influence of taste disorders on dietary behaviors in cancer patients under chemotherapy. Nutr J 9:15. https://doi.org/10.1186/1475-2891-9-15
Bernhardson BM, Tishelman C, Rutqvist LE (2007) Chemosensory changes experienced by patients undergoing cancer chemotherapy: a qualitative interview study. J Pain Symptom Manage 34:403–412. https://doi.org/10.1016/j.jpainsymman.2006.12.010
Boltong A, Aranda S, Keast R et al (2014) A prospective cohort study of the effects of adjuvant breast cancer chemotherapy on taste function, food liking, appetite and associated nutritional outcomes. Plos One 9:e103512. https://doi.org/10.1371/journal.pone.0103512
McLaughlin L, Mahon SM (2012) Understanding taste dysfunction in patients with cancer. Clin J Oncol Nurs 16:171–178. https://doi.org/10.1188/12.CJON.171-178
Pellegrini M, Merlo FD, Agnello E et al (2023) Dysgeusia in patients with breast cancer treated with chemotherapy—a narrative review. Nutrients 15:226. https://doi.org/10.3390/nu15010226
Rehwaldt M, Wickham R, Purl S et al (2009) Self-care strategies to cope with taste changes after chemotherapy. Oncol Nurs Forum 36:E47–E56. https://doi.org/10.1188/09.ONF.E47-E56
Gamper EM, Zabernigg A, Wintner LM et al (2012) Coming to your senses: detecting taste and smell alterations in chemotherapy patients. A systematic review. J Pain Symptom Manage 44:880–895. https://doi.org/10.1016/j.jpainsymman.2011.11.011
Sevryugin O, Kasvis P, Vigano M, Vigano A (2021) Taste and smell disturbances in cancer patients: a scoping review of available treatments. Support Care Cancer 29:49–66. https://doi.org/10.1007/s00520-020-05609-4
Roper SD, Chaudhari N (2017) Taste buds: cells, signals and synapses. Nat Rev Neurosci 18:485–497. https://doi.org/10.1038/nrn.2017.68
Bachmanov AA, Bosak NP, Lin C et al (2014) Genetics of taste receptors. Curr Pharm Des 20:2669–2683. https://doi.org/10.2174/13816128113199990566
Lemon CH (2017) Modulation of taste processing by temperature. Am J Physiol-Regul, Integr Comp Physiol 313:R305–R321. https://doi.org/10.1152/ajpregu.00089.2017
Keast RSJ, Breslin PAS (2003) An overview of binary taste-taste interactions. Food Qual Prefer 14:111–124. https://doi.org/10.1016/S0950-3293(02)00110-6
Yamamoto T, Inui-Yamamoto C (2023) The flavor-enhancing action of glutamate and its mechanism involving the notion of kokumi. NPJ Sci Food 7:3. https://doi.org/10.1038/s41538-023-00178-2
Vincis R, Fontanini A (2019) Central taste anatomy and physiology. Handb Clin Neurol 164:187–204. https://doi.org/10.1016/b978-0-444-63855-7.00012-5
Sandri A, Cecchini MP, Riello M et al (2021) Pain, smell, and taste in adults: a narrative review of multisensory perception and interaction. Pain Ther 10:245–268. https://doi.org/10.1007/s40122-021-00247-y
Diepeveen J, Moerdijk-Poortvliet TCW, van der Leij FR (2022) Molecular insights into human taste perception and umami tastants: a review. J Food Sci 87:1449–1465. https://doi.org/10.1111/1750-3841.16101
Wise PM, Breslin PAS (2011) Relationships among taste qualities assessed with response-context effects. Chem Senses 36:581–587. https://doi.org/10.1093/chemse/bjr024
McGettigan N, Dhuibhir PU, Barrett M et al (2019) Subjective and objective assessment of taste and smell sensation in advanced cancer. Am J Hosp Palliat Med® 36:688–696. https://doi.org/10.1177/1049909119832836
Bernhardson BM, Tishelman C, Rutqvist LE (2008) Self-reported taste and smell changes during cancer chemotherapy. Support Care Cancer 16:275–283. https://doi.org/10.1007/s00520-007-0319-7
Nolden AA, Hwang LD, Boltong A, Reed DR (2019) Chemosensory changes from cancer treatment and their effects on patients’ food behavior: a scoping review. Nutrients 11:2285. https://doi.org/10.3390/nu11102285
Chaveli-López B (2014) Oral toxicity produced by chemotherapy: a systematic review. J Clin Exp Dent 6:e81–e90. https://doi.org/10.4317/jced.51337
van Bokhorst-de van der Schueren MAE (2005) Nutritional support strategies for malnourished cancer patients. Eur J Oncol Nurs 9:S74–S83. https://doi.org/10.1016/j.ejon.2005.09.004
Yamaguchi S, Ninomiya K (2000) Umami and food palatability. J Nutr 130:S921–S926. https://doi.org/10.1093/jn/130.4.921S
Atsumi N, Yasumatsu K, Takashina Y et al (2023) Chloride ions evoke taste sensations by binding to the extracellular ligand-binding domain of sweet/umami taste receptors. eLife 12:e84291. https://doi.org/10.7554/eLife.84291
Obayashi N, Sakayori N, Kawaguchi H, Sugita M (2023) Effect of irinotecan administration on amiloride‐sensitive sodium taste responses in mice. Eur J Oral Sci 131:e12922. https://doi.org/10.1111/eos.12922
Shigemura N, Iwata S, Yasumatsu K et al (2013) Angiotensin II modulates salty and sweet taste sensitivities. J Neurosci 33:6267–6277. https://doi.org/10.1523/JNEUROSCI.5599-12.2013
Oka Y, Butnaru M, von Buchholtz L et al (2013) High salt recruits aversive taste pathways. Nature 494:472–475. https://doi.org/10.1038/nature11905
Chamoun E, Liu AAS, Duizer LM et al (2019) Taste sensitivity and taste preference measures are correlated in healthy young adults. Chem Senses 44:113–121. https://doi.org/10.1093/chemse/bjy082
Acknowledgements
The authors gratefully acknowledge Professor Kazuhiko Sugiyama of the Department of Medical Oncology at Hiroshima University Hospital for providing the opportunity to collect valuable data. They also thank Nurse Miyuki Kiyomoto and the staff of the Outpatient Chemotherapy Unit for their support.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by Nami Obayashi and Mariko Naito. The first draft of the manuscript was written by Nami Obayashi and Makoto Sugita. All authors commented on the subsequent versions of the manuscript. All authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Ethics Committee of Hiroshima University Hospital.
Consent to participate
Written informed consent was obtained from all individual participants included in the study.
Consent for publication
The authors affirm that human research participants provided informed consent for publication.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Obayashi, N., Sugita, M., Shintani, T. et al. Taste–taste associations in chemotherapy-induced subjective taste alterations: findings from a questionnaire survey in an outpatient clinic. Support Care Cancer 31, 552 (2023). https://doi.org/10.1007/s00520-023-08013-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00520-023-08013-w