Abstract
Purpose
Acute graft versus host disease (aGVHD) is a major cause of non-relapse morbidity and mortality post-allogenic hematopoietic stem cell transplant (HSCT). Using conventional literature search and computational approaches, our objective was to identify oral and gut bacterial species associated with aGVHD, potentially affecting drug treatment via lipopolysaccharide (LPS) pathways.
Methods
Medline, PubMed, PubMed Central, and Google Scholar were searched using MeSH terms. The top 100 hits per database were curated, and 25 research articles were selected to examine oral and gut microbiomes associated with health, HSCT, and aGVHD. Literature search validation, aGVHD drug targets, and microbial metabolic pathway identification were completed using BioReader, MACADAM, KEGG, and STRING programs.
Results
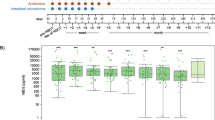
Our review determined that (1) oral genera Rothia, Solobacterium, and Veillonella were identified in HSCT patients’ stool and associated with aGVHD; (2) shifts in gut enterococci profiles were determined in HSCT-associated aGVHD; (3) gut microbiome dysbiosis prior or during HSCT and lower Shannon diversity index at time of HSCT were also associated with increased risk of aGVHD and transplant related death; and (4) Coriobacteriaceae family was negatively correlated with gut aGVHD, whereas Eubacterium limosum was associated with decreased risk of chronic GVHD relapse.
Additionally, we identified molecular pathways related to TLR4/ LPS, including candidate aGVHD drug targets, impacted by oral and gut bacterial taxa.
Conclusion
Reduced microbial diversity reflects higher severity and mortality rate in HSCT patients with aGVHD. Multi-omics approaches to decipher oral and gut microbiome associations will be critical for developing aGVHD preventive therapies.



Similar content being viewed by others
Availability of data
N/A
References
D'Souza A, Lee S, Zhu X, Pasquini M (2017) Current use and trends in hematopoietic cell transplantation in the United States. Biol Blood Marrow Transplant 23(9):1417–1421. https://doi.org/10.1016/j.bbmt.2017.05.035
Wojnar J, Giebel S, Krawczyk-Kulis M, Markiewicz M, Kruzel T, Wylezol I, Czerw T, Seweryn M, Holowiecki J (2006) Acute graft-versus-host disease. The incidence and risk factors. Ann Transplant 11(1):16–23
Yu J, Parasuraman S, Shah A, Weisdorf D (2019) Mortality, length of stay and costs associated with acute graft-versus-host disease during hospitalization for allogeneic hematopoietic stem cell transplantation. Curr Med Res Opin 35(6):983–988. https://doi.org/10.1080/03007995.2018.1551193
Dignan FL, Scarisbrick JJ, Cornish J, Clark A, Amrolia P, Jackson G, Mahendra P, Taylor PC, Shah P, Lightman S, Fortune F, Kibbler C, Andreyev J, Albanese A, Hadzic N, Potter MN, Shaw BE, Haemato-oncology Task Force of British Committee for Standards in H, British Society for B, Marrow T (2012) Organ-specific management and supportive care in chronic graft-versus-host disease. Br J Haematol 158(1):62–78. https://doi.org/10.1111/j.1365-2141.2012.09131.x
Kohler N, Zeiser R (2018) Intestinal microbiota influence immune tolerance post allogeneic hematopoietic cell transplantation and intestinal GVHD. Front Immunol 9:3179. https://doi.org/10.3389/fimmu.2018.03179
Sun Y, Tawara I, Toubai T, Reddy P (2007) Pathophysiology of acute graft-versus-host disease: recent advances. Transl Res 150(4):197–214. https://doi.org/10.1016/j.trsl.2007.06.003
Strong Rodrigues K, Oliveira-Ribeiro C, de Abreu Fiuza Gomes S, Knobler R (2018) Cutaneous graft-versus-host disease: diagnosis and treatment. Am J Clin Dermatol 19(1):33–50. https://doi.org/10.1007/s40257-017-0306-9
Funke VA, Moreira MC, Vigorito AC (2016) Acute and chronic graft-versus-host disease after hematopoietic stem cell transplantation. Rev Assoc Med Bras (1992) 62(Suppl 1):44–50. https://doi.org/10.1590/1806-9282.62.suppl1.44
Levine JE (2014) Less (bacterial diversity) is more (deaths). Blood 124(7):995–996. https://doi.org/10.1182/blood-2014-07-583906
Baron F, Storb R, Storer BE, Maris MB, Niederwieser D, Shizuru JA, Chauncey TR, Bruno B, Forman SJ, McSweeney PA, Maziarz RT, Pulsipher MA, Agura ED, Wade J, Sorror M, Maloney DG, Sandmaier BM (2006) Factors associated with outcomes in allogeneic hematopoietic cell transplantation with nonmyeloablative conditioning after failed myeloablative hematopoietic cell transplantation. J Clin Oncol 24(25):4150–4157. https://doi.org/10.1200/JCO.2006.06.9914
Ghimire S, Weber D, Mavin E, Wang XN, Dickinson AM, Holler E (2017) Pathophysiology of GvHD and other HSCT-related major complications. Front Immunol 8:79. https://doi.org/10.3389/fimmu.2017.00079
Jagasia M, Arora M, Flowers ME, Chao NJ, McCarthy PL, Cutler CS, Urbano-Ispizua A, Pavletic SZ, Haagenson MD, Zhang MJ, Antin JH, Bolwell BJ, Bredeson C, Cahn JY, Cairo M, Gale RP, Gupta V, Lee SJ, Litzow M, Weisdorf DJ, Horowitz MM, Hahn T (2012) Risk factors for acute GVHD and survival after hematopoietic cell transplantation. Blood 119(1):296–307. https://doi.org/10.1182/blood-2011-06-364265
Sorror ML, Martin PJ, Storb RF, Bhatia S, Maziarz RT, Pulsipher MA, Maris MB, Davis C, Deeg HJ, Lee SJ, Maloney DG, Sandmaier BM, Appelbaum FR, Gooley TA (2014) Pretransplant comorbidities predict severity of acute graft-versus-host disease and subsequent mortality. Blood 124(2):287–295. https://doi.org/10.1182/blood-2014-01-550566
Schmidt TS, Hayward MR, Coelho LP, Li SS, Costea PI, Voigt AY, Wirbel J, Maistrenko OM, Alves RJ, Bergsten E, de Beaufort C, Sobhani I, Heintz-Buschart A, Sunagawa S, Zeller G, Wilmes P, Bork P (2019) Extensive transmission of microbes along the gastrointestinal tract. Elife 8. https://doi.org/10.7554/eLife.42693
Groeger S, Meyle J (2019) Oral mucosal epithelial cells. Front Immunol 10:208. https://doi.org/10.3389/fimmu.2019.00208
Taur Y, Jenq RR, Perales MA, Littmann ER, Morjaria S, Ling L, No D, Gobourne A, Viale A, Dahi PB, Ponce DM, Barker JN, Giralt S, van den Brink M, Pamer EG (2014) The effects of intestinal tract bacterial diversity on mortality following allogeneic hematopoietic stem cell transplantation. Blood 124(7):1174–1182. https://doi.org/10.1182/blood-2014-02-554725
Cooke KR, Olkiewicz K, Erickson N, Ferrara JL (2002) The role of endotoxin and the innate immune response in the pathophysiology of acute graft versus host disease. J Endotoxin Res 8(6):441–448. https://doi.org/10.1179/096805102125001046
Le Boulch M, Dehais P, Combes S (2019) Pascal G (2019) the MACADAM database: a MetAboliC pAthways DAtabase for microbial taxonomic groups for mining potential metabolic capacities of archaeal and bacterial taxonomic groups. Database (Oxford) 2019. https://doi.org/10.1093/database/baz049
Ferrara JLM, Chaudhry MS (2018) GVHD: biology matters. Blood Adv 2(22):3411–3417. https://doi.org/10.1182/bloodadvances.2018020214
Tu S, Zhong D, Xie W, Huang W, Jiang Y, Li Y (2016) Role of toll-like receptor signaling in the pathogenesis of graft-versus-host diseases. Int J Mol Sci 17(8). https://doi.org/10.3390/ijms17081288
Sivula J, Cordova ZM, Tuimala J, Jaatinen T, Partanen J, Volin L, Turpeinen H (2012) Toll-like receptor gene polymorphisms confer susceptibility to graft-versus-host disease in allogenic hematopoietic stem cell transplantation. Scand J Immunol 76(3):336–341. https://doi.org/10.1111/j.1365-3083.2012.02737.x
Biological Research Article Distiller v1.2 http://www.cbs.dtu.dk/services/BioReader/
Simon C, Davidsen K, Hansen C, Seymour E, Barnkob MB, Olsen LR (2019) BioReader: a text mining tool for performing classification of biomedical literature. BMC Bioinformatics 19(Suppl 13):57. https://doi.org/10.1186/s12859-019-2607-x
MetAbolic pAthways DAtabase for Microbial taxonomic groups http://macadam.toulouse.inra.fr/
Lu YC, Yeh WC, Ohashi PS (2008) LPS/TLR4 signal transduction pathway. Cytokine 42(2):145–151. https://doi.org/10.1016/j.cyto.2008.01.006
Kyoto Encyclopedia of Genes and Genomes (KEGG) database https://www.genome.jp/kegg/
Szklarczyk D, Gable AL, Lyon D, Junge A, Wyder S, Huerta-Cepas J, Simonovic M, Doncheva NT, Morris JH, Bork P, Jensen LJ, Mering CV (2019) STRING v11: protein-protein association networks with increased coverage, supporting functional discovery in genome-wide experimental datasets. Nucleic Acids Res 47(D1):D607–D613. https://doi.org/10.1093/nar/gky1131
Galloway-Pena JR, Smith DP, Sahasrabhojane P, Wadsworth WD, Fellman BM, Ajami NJ, Shpall EJ, Daver N, Guindani M, Petrosino JF, Kontoyiannis DP, Shelburne SA (2017) Characterization of oral and gut microbiome temporal variability in hospitalized cancer patients. Genome Med 9(1):21. https://doi.org/10.1186/s13073-017-0409-1
Ames NJ, Sulima P, Ngo T, Barb J, Munson PJ, Paster BJ, Hart TC (2012) A characterization of the oral microbiome in allogeneic stem cell transplant patients. PLoS One 7(10):e47628. https://doi.org/10.1371/journal.pone.0047628
Golob JL, Pergam SA, Srinivasan S, Fiedler TL, Liu C, Garcia K, Mielcarek M, Ko D, Aker S, Marquis S, Loeffelholz T, Plantinga A, Wu MC, Celustka K, Morrison A, Woodfield M, Fredricks DN (2017) Stool microbiota at neutrophil recovery is predictive for severe acute graft vs host disease after hematopoietic cell transplantation. Clin Infect Dis 65(12):1984–1991. https://doi.org/10.1093/cid/cix699
Parco S, Benericetti G, Vascotto F, Palmisciano G (2019) Microbiome and diversity indices during blood stem cells transplantation - new perspectives? Cent Eur J Public Health 27(4):335–339. https://doi.org/10.21101/cejph.a5393
Holler E, Butzhammer P, Schmid K, Hundsrucker C, Koestler J, Peter K, Zhu W, Sporrer D, Hehlgans T, Kreutz M, Holler B, Wolff D, Edinger M, Andreesen R, Levine JE, Ferrara JL, Gessner A, Spang R, Oefner PJ (2014) Metagenomic analysis of the stool microbiome in patients receiving allogeneic stem cell transplantation: loss of diversity is associated with use of systemic antibiotics and more pronounced in gastrointestinal graft-versus-host disease. Biol Blood Marrow Transplant 20(5):640–645. https://doi.org/10.1016/j.bbmt.2014.01.030
Galloway-Pena JR, Peterson CB, Malik F, Sahasrabhojane PV, Shah DP, Brumlow CE, Carlin LG, Chemaly RF, Im JS, Rondon G, Felix E, Veillon L, Lorenzi PL, Alousi AM, Jenq RR, Kontoyiannis DP, Shpall EJ, Shelburne SA, Okhuysen PC (2019) Fecal microbiome, metabolites, and stem cell transplant outcomes: a single-center pilot study. Open Forum Infect Dis 6(5):ofz173. https://doi.org/10.1093/ofid/ofz173
Biagi E, Zama D, Rampelli S, Turroni S, Brigidi P, Consolandi C, Severgnini M, Picotti E, Gasperini P, Merli P, Decembrino N, Zecca M, Cesaro S, Faraci M, Prete A, Locatelli F, Pession A, Candela M, Masetti R (2019) Early gut microbiota signature of aGvHD in children given allogeneic hematopoietic cell transplantation for hematological disorders. BMC Med Genet 12(1):49. https://doi.org/10.1186/s12920-019-0494-7
Han L, Zhang H, Chen S, Zhou L, Li Y, Zhao K, Huang F, Fan Z, Xuan L, Zhang X, Dai M, Lin Q, Jiang Z, Peng J, Jin H, Liu Q (2019) Intestinal microbiota can predict acute graft-versus-host disease following allogeneic hematopoietic stem cell transplantation. Biol Blood Marrow Transplant 25(10):1944–1955. https://doi.org/10.1016/j.bbmt.2019.07.006
Mancini N, Greco R, Pasciuta R, Barbanti MC, Pini G, Morrow OB, Morelli M, Vago L, Clementi N, Giglio F, Lupo Stanghellini MT, Forcina A, Infurnari L, Marktel S, Assanelli A, Carrabba M, Bernardi M, Corti C, Burioni R, Peccatori J, Sormani MP, Banfi G, Ciceri F, Clementi M (2017) Enteric microbiome markers as early predictors of clinical outcome in allogeneic hematopoietic stem cell transplant: results of a prospective study in adult patients. Open Forum Infect Dis 4(4):ofx215. https://doi.org/10.1093/ofid/ofx215
Weber D, Oefner PJ, Hiergeist A, Koestler J, Gessner A, Weber M, Hahn J, Wolff D, Stammler F, Spang R, Herr W, Dettmer K, Holler E (2015) Low urinary indoxyl sulfate levels early after transplantation reflect a disrupted microbiome and are associated with poor outcome. Blood 126(14):1723–1728. https://doi.org/10.1182/blood-2015-04-638858
Bansal T, Alaniz RC, Wood TK, Jayaraman A (2010) The bacterial signal indole increases epithelial-cell tight-junction resistance and attenuates indicators of inflammation. Proc Natl Acad Sci U S A 107(1):228–233. https://doi.org/10.1073/pnas.0906112107
Jenq RR, Ubeda C, Taur Y, Menezes CC, Khanin R, Dudakov JA, Liu C, West ML, Singer NV, Equinda MJ, Gobourne A, Lipuma L, Young LF, Smith OM, Ghosh A, Hanash AM, Goldberg JD, Aoyama K, Blazar BR, Pamer EG, van den Brink MR (2012) Regulation of intestinal inflammation by microbiota following allogeneic bone marrow transplantation. J Exp Med 209(5):903–911. https://doi.org/10.1084/jem.20112408
Jenq RR, Taur Y, Devlin SM, Ponce DM, Goldberg JD, Ahr KF, Littmann ER, Ling L, Gobourne AC, Miller LC, Docampo MD, Peled JU, Arpaia N, Cross JR, Peets TK, Lumish MA, Shono Y, Dudakov JA, Poeck H, Hanash AM, Barker JN, Perales MA, Giralt SA, Pamer EG, van den Brink MR (2015) Intestinal Blautia is associated with reduced death from graft-versus-host disease. Biol Blood Marrow Transplant 21(8):1373–1383. https://doi.org/10.1016/j.bbmt.2015.04.016
Liu C, Frank DN, Horch M, Chau S, Ir D, Horch EA, Tretina K, van Besien K, Lozupone CA, Nguyen VH (2017) Associations between acute gastrointestinal GvHD and the baseline gut microbiota of allogeneic hematopoietic stem cell transplant recipients and donors. Bone Marrow Transplant 52(12):1643–1650. https://doi.org/10.1038/bmt.2017.200
Biagi E, Zama D, Nastasi C, Consolandi C, Fiori J, Rampelli S, Turroni S, Centanni M, Severgnini M, Peano C, de Bellis G, Basaglia G, Gotti R, Masetti R, Pession A, Brigidi P, Candela M (2015) Gut microbiota trajectory in pediatric patients undergoing hematopoietic SCT. Bone Marrow Transplant 50(7):992–998. https://doi.org/10.1038/bmt.2015.16
Lee YK, Kang M, Choi EY (2017) TLR/MyD88-mediated innate immunity in intestinal graft-versus-host disease. Immune Netw 17(3):144–151. https://doi.org/10.4110/in.2017.17.3.144
Peled JU, Devlin SM, Staffas A, Lumish M, Khanin R, Littmann ER, Ling L, Kosuri S, Maloy M, Slingerland JB, Ahr KF, Porosnicu Rodriguez KA, Shono Y, Slingerland AE, Docampo MD, Sung AD, Weber D, Alousi AM, Gyurkocza B, Ponce DM, Barker JN, Perales MA, Giralt SA, Taur Y, Pamer EG, Jenq RR, van den Brink MRM (2017) Intestinal microbiota and relapse after hematopoietic-cell transplantation. J Clin Oncol 35(15):1650–1659. https://doi.org/10.1200/JCO.2016.70.3348
Peled JU, Gomes ALC, Devlin SM, Littmann ER, Taur Y, Sung AD, Weber D, Hashimoto D, Slingerland AE, Slingerland JB, Maloy M, Clurman AG, Stein-Thoeringer CK, Markey KA, Docampo MD, Burgos da Silva M, Khan N, Gessner A, Messina JA, Romero K, Lew MV, Bush A, Bohannon L, Brereton DG, Fontana E, Amoretti LA, Wright RJ, Armijo GK, Shono Y, Sanchez-Escamilla M, Castillo Flores N, Alarcon Tomas A, Lin RJ, Yanez San Segundo L, Shah GL, Cho C, Scordo M, Politikos I, Hayasaka K, Hasegawa Y, Gyurkocza B, Ponce DM, Barker JN, Perales MA, Giralt SA, Jenq RR, Teshima T, Chao NJ, Holler E, Xavier JB, Pamer EG, van den Brink MRM (2020) Microbiota as predictor of mortality in allogeneic hematopoietic-cell transplantation. N Engl J Med 382(9):822–834. https://doi.org/10.1056/NEJMoa1900623
Monnet E, Choy EH, McInnes I, Kobakhidze T, de Graaf K, Jacqmin P, Lapeyre G, de Min C (2020) Efficacy and safety of NI-0101, an anti-toll-like receptor 4 monoclonal antibody, in patients with rheumatoid arthritis after inadequate response to methotrexate: a phase II study. Ann Rheum Dis 79(3):316–323. https://doi.org/10.1136/annrheumdis-2019-216487
Mougeot FB, Beckman M, Osipoff A, Dodd B, Butler C, Noll J, Morton DS, Avalos B, Copelan E, Brennan M, Mougeot JL (2020) Oral microbiome profiles of haematopoietic stem cell transplant patients who develop graft-versus-host disease [abstract]. Support Care Cancer [publication deferred due to COVID]
Yoshimura A, Kaneko T, Kato Y, Golenbock DT, Hara Y (2002) Lipopolysaccharides from periodontopathic bacteria Porphyromonas gingivalis and Capnocytophaga ochracea are antagonists for human toll-like receptor 4. Infect Immun 70(1):218–225. https://doi.org/10.1128/iai.70.1.218-225.2002
Spindelboeck W, Schulz E, Uhl B, Kashofer K, Aigelsreiter A, Zinke-Cerwenka W, Mulabecirovic A, Kump PK, Halwachs B, Gorkiewicz G, Sill H, Greinix H, Hogenauer C, Neumeister P (2017) Repeated fecal microbiota transplantations attenuate diarrhea and lead to sustained changes in the fecal microbiota in acute, refractory gastrointestinal graft-versus-host-disease. Haematologica 102(5):e210–e213. https://doi.org/10.3324/haematol.2016.154351
Funding
This study was supported by Atrium Health Research fund.
Author information
Authors and Affiliations
Contributions
Dr. Farah Bahrani Mougeot and Dr. Jean-Luc Mougeot conceived the study. Darla Morton conducted the conventional literature search and compiling of summaries. Micaela Beckman conducted verifications of the conventional literature search and complemented the study with the bioinformatics approach. All authors had significant contributions in writing and revisions of main manuscript, tables, and figures.
Corresponding authors
Ethics declarations
Conflict of interest
None to disclose.
Consent for publication
All authors have approved the final version of this manuscript.
Ethics approval
N/A
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(PDF 89 kb)
Supplementary Table S1
(DOCX 23 kb)
Supplementary Table S2
(DOCX 16 kb)
Supplementary Table S3
(DOCX 14 kb)
Rights and permissions
About this article
Cite this article
Beckman, M., Morton, D.S., Bahrani Mougeot, F. et al. Allogenic stem cell transplant-associated acute graft versus host disease: a computational drug discovery text mining approach using oral and gut microbiome signatures. Support Care Cancer 29, 1765–1779 (2021). https://doi.org/10.1007/s00520-020-05821-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-020-05821-2