Abstract
Purpose
Effective symptom discussion is an essential step to enhance symptom management in patients with advanced pancreatic cancer (APC). However, little is known about how these patients communicate their symptoms during health encounters. The purpose of this study was to develop a typology to describe patterns of interactions between patients with APC, their caregivers, and healthcare providers as regards to symptoms and symptom management.
Methods
Thematic analysis was used to analyze 37 transcripts of audio-recorded, naturally occurring encounters among APC patients, caregivers, and healthcare providers. Transcripts were drawn from the Values and Options in Cancer Care study, a larger randomized controlled communication and decision-making intervention trial, which recruited advanced cancer patients and caregivers across the USA. All transcripts from APC patients that were pre-intervention were analyzed.
Results
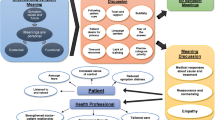
Eight unique types of interaction patterns among patients, caregivers, and healthcare providers were identified as follows: collaborative interactions, explanatory interactions, agentic interactions, checklist interactions, cross-purpose interactions, empathic interactions, admonishing interactions, and diverging interactions.
Conclusions
Our findings provide a systematic description of a variety of types of interaction patterns regarding symptom discussion among APC patients, caregivers, and healthcare providers. These typologies can be used to facilitate effective communication and symptom management.
Similar content being viewed by others
References
Tang C, Von Ah D, Fulton J (2018) The symptom experience of patients with advanced pancreatic cancer: an integrative review. Cancer Nurs 41(1):33–44
Gooden H, White K (2013) Pancreatic cancer and supportive care—pancreatic exocrine insufficiency negatively impacts on quality of life. Support Care Cancer 21(7):1835–1841
Labori KJ, Hjermstad MJ, Wester T, Buanes T, Loge JH (2006) Symptom profiles and palliative care in advanced pancreatic cancer: a prospective study. Support Care Cancer 14(11):1126–1133
Muller-Nordhorn J, Roll S, Bohmig M et al (2006) Health-related quality of life in patients with pancreatic cancer. Digestion 74(2):118–125
Tang C, Shields CG, Von Ah D (2016, Sep) How did advanced pancreatic cancer patients and caregivers communicate their needs: a pilot study. Paper presented to the Sigma Theta Tau International Leadership Connection, Indianapolis
Grant MS, Wiegand DL (2013) Conversations with strangers: the needs of those accessing a palliative care nurse practitioner on a pancreatic cancer web site. J Hospice Palliat Nurs 15(5):278–285
Epstein RM, Street RL (2007) Patient-centered communication in cancer care: promoting healing and reducing suffering. National Cancer Institute, US Department of Health and Human Services, National Institutes of Health, Bethesda
Scheunemann LP, McDevitt M, Carson SS, Randomized HLC (2011) Controlled trials of interventions to improve communication in intensive care: a systematic review. CHEST Journal 139(3):543–554
Thorne SE, Bultz BD, Baile WF (2005) Is there a cost to poor communication in cancer care?: a critical review of the literature. Psycho-Oncology 14(10):875–884
Wright KB, Sparks L, O'hair HD (2012) Health Communication in the 21st Century. Wiley, Hoboken
Bodie GD, MacGeorge EL (2014) Supportive communication theories: dual-process theory of supportive message outcomes and advice response theory. In: Baxter LA, Braithwaite DO (eds) Engaging theories in interpersonal communication: multiple perspectives. Sage, Los Angeles
Donovan HS, Hartenbach EM, Method MW (2005) Patient–provider communication and perceived control for women experiencing multiple symptoms associated with ovarian cancer. Gynecol Oncol 99(2):404–411
Sakai EY, Carpenter BD (2011) Linguistic features of power dynamics in triadic dementia diagnostic conversations. Patient Educ Couns 85(2):295–298
Laws MB, Beach MC, Lee Y, Rogers WH, Saha S, Korthuis PT, Sharp V, Wilson IB (2013) Provider-patient adherence dialogue in HIV care: results of a multisite study. AIDS Behav 17(1):148–159
Mast MS, Hall JA, Roter DL (2008) Caring and dominance affect participants’ perceptions and behaviors during a virtual medical visit. J Gen Intern Med 23(5):523–527
Berry DL, Wilkie DJ, Thomas M Jr, Charles R, Fortner P (2003) Clinicians communicating with patients experiencing cancer pain: ORIGINAL ARTICLE. Cancer Investig 21(3):374–381
Coward DD, Wilkie DJ (2000) Metastatic bone pain: meanings associated with self-report and self-management decision making. Cancer Nurs 23(2):101–108
Kimberlin C, Brushwood D, Allen W, Radson E, Wilson D (2004) Cancer patient and caregiver experiences: communication and pain management issues. J Pain Symptom Manag 28(6):566–578
Passik SD, Kirsh KL, Donaghy K, Holtsclaw E, Theobald D, Cella D, Breitbart W, Fatigue Coalition (2002) Patient-related barriers to fatigue communication: initial validation of the fatigue management barriers questionnaire. J Pain Symptom Manag 24(5):481–493
Hoerger M, Epstein RM, Winters PC, Fiscella K, Duberstein PR, Gramling R, Butow PN, Mohile SG, Kaesberg PR, Tang W, Plumb S, Walczak A, Back AL, Tancredi D, Venuti A, Cipri C, Escalera G, Ferro C, Gaudion D, Hoh B, Leatherwood B, Lewis L, Robinson M, Sullivan P, Kravitz RL (2013) Values and options in cancer care (VOICE): study design and rationale for a patient-centered communication and decision-making intervention for physicians, patients with advanced cancer, and their caregivers. BMC Cancer 13(1):188
B raun V, Clarke V (2006) Using thematic analysis in psychology. Qual Res Psychol 3(2):77–101
D’Agostino TA, Atkinson TM, Latella LE, Rogers M, Morrissey D, DeRosa AP, Parker PA (2017) Promoting patient participation in healthcare interactions through communication skills training: a systematic review. Patient Educ Couns 100:1247–1257
Rao JK, Anderson LA, Sukumar B, Beauchesne DA, Stein T, Frankel RM (2010) Engaging communication experts in a Delphi process to identify patient behaviors that could enhance communication in medical encounters. BMC Health Serv Res 10(1):97
Alegría M, Sribney W, Perez D, Laderman M, Keefe K (2009) The role of patient activation on patient–provider communication and quality of care for US and foreign born Latino patients. J Gen Intern Med 24(3):534–541
Burleson BR, Daly J, Wiemann J (1994) Comforting messages: features, functions, and outcomes. In: Daly JA, Wiemann JM (eds) Strategic Interpersonal Communication. Routledge, Hillsdale, p 135–161
Beck RS, Daughtridge R, Sloane PD (2002) Physician-patient communication in the primary care office: a systematic review. J Am Board Fam Pract 15(1):25–38
Zachariae R, Pedersen CG, Jensen AB, Ehrnrooth E, Rossen PB, von der Maase H (2003) Association of perceived physician communication style with patient satisfaction, distress, cancer-related self-efficacy, and perceived control over the disease. Br J Cancer 88(5):658–665
Flickinger TE, Saha S, Roter D, Korthuis PT, Sharp V, Cohn J, Eggly S, Moore RD, Beach MC (2016) Clinician empathy is associated with differences in patient–clinician communication behaviors and higher medication self-efficacy in HIV care. Patient Educ Couns 99(2):220–226
Del Piccolo L, Mazzi M, Saltini A, Zimmermann C (2002) Inter and intra individual variations in physicians’ verbal behaviour during primary care consultations. Soc Sci Med 55(10):1871–1885
Wooffitt R (2005) Conversation analysis and discourse analysis: a comparative and critical introduction. Sage, London
Funding
Chia-Chun Tang was supported by the Behavioral Cooperative Oncology Group (BCOG) Center for Symptom Management and Walther Cancer Foundation (2014–2016 Graduate Student Fellowship Award). The authors have full control of all primary data and agree to allow the journal to review data if requested.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Tang, CC., Draucker, C., Tejani, M.A. et al. Patterns of interactions among patients with advanced pancreatic cancer, their caregivers, and healthcare providers during symptom discussions. Support Care Cancer 26, 3497–3506 (2018). https://doi.org/10.1007/s00520-018-4202-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-018-4202-5