Abstract
Purpose
Curcumin exerts its anti-inflammatory activity via inhibition of nuclear factor κB. Oropharyngeal epithelia and residing bacteria closely interact in inflammation and infection. This in vitro model investigated the effects of curcumin on bacterial survival, adherence to, and invasion of upper respiratory tract epithelia, and studied its anti-inflammatory effect. We aimed to establish a model, which could offer insights into the host–pathogen interaction in cancer therapy induced mucositis.
Methods
Moraxella catarrhalis (Mcat) and the oropharyngeal epithelial cell line Detroit 562 were used. Time–kill curves assessed the inhibition of bacterial growth and adherence assays and gentamicin protection assays determined the effect of curcumin-preincubated cells on bacterial adherence and invasion. Curcumin-mediated inhibition of pro-inflammatory activation by Mcat was determined via interleukin-8 concentrations in the supernatants. The synergistic role of secretory IgA (sIgA) on adherence was investigated.
Results
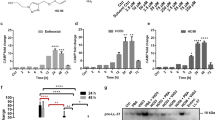
Curcumin was bactericidal at concentrations >50 µM. Preincubation of Detroit cells for 60 min demonstrated that concentrations >100 µM inhibited bacterial adherence. Together with sIgA, curcumin inhibited adherence at concentrations ≥50 µM. Both 100 and 200 µM curcumin significantly inhibited Mcat cell invasion. Finally, curcumin inhibited Mcat-induced pro-inflammatory activation by strongly suppressing IL-8 release. At a concentration of 200 µM, 10 min of curcumin exposure inhibited IL-8 release significantly, and complete suppression required a pre-exposure time of ≥45 min.
Conclusion
Curcumin, in clinically relevant concentrations for topical use, displayed strong antibacterial effect against a facultative upper respiratory tract pathogen by inhibiting bacterial growth, adherence, invasion, and pro-inflammatory activation of upper respiratory tract epithelial cells in vitro.






Similar content being viewed by others
References
Aebi C, Lafontaine ER, Cope LD, Latimer JL, Lumbley SL, McCracken GH Jr, Hansen EJ (1998) Phenotypic effect of isogenic uspA1 and uspA2 mutations on Moraxella catarrhalis 035E. Infect Immun 66:3113–3119
Aebi C, Maciver I, Latimer JL, Cope LD, Stevens MK, Thomas SE, McCracken GH Jr, Hansen EJ (1997) A protective epitope of Moraxella catarrhalis is encoded by two different genes. Infect Immun 65:4367–4377
Bartos LC, Murphy TF (1988) Comparison of the outer membrane proteins of 50 strains of Branhamella catarrhalis. J Infect Dis 158:761–765
Bender K, Gottlicher M, Whiteside S, Rahmsdorf HJ, Herrlich P (1998) Sequential DNA damage-independent and -dependent activation of NF-kappaB by UV. EMBO J 17:5170–5181
Bernhoft CH, Skaug N (1985) Oral findings in irradiated edentulous patients. Int J Oral Surg 14:416–427
Blijlevens NM, Logan RM, Netea MG (2009) The changing face of febrile neutropenia-from monotherapy to moulds to mucositis. Mucositis: from febrile neutropenia to febrile mucositis. J Antimicrob Chemother 63(Suppl 1):i36–i40
Bowen JM, Keefe DM (2008) New pathways for alimentary mucositis. J Oncol 2008:907892
Elting LS, Cooksley C, Chambers M, Cantor SB, Manzullo E, Rubenstein EB (2003) The burdens of cancer therapy. Clinical and economic outcomes of chemotherapy-induced mucositis. Cancer 98:1531–1539
Faden H, Harabuchi Y, Hong JJ (1994) Epidemiology of Moraxella catarrhalis in children during the first 2 years of life: relationship to otitis media. J Infect Dis 169:1312–1317
Fink J, Mathaba LT, Stewart GA, Graham PT, Steer JH, Joyce DA, McWilliam AS (2006) Moraxella catarrhalis stimulates the release of proinflammatory cytokines and prostaglandin E from human respiratory epithelial cells and monocyte-derived macrophages. FEMS Immunol Med Microbiol 46:198–208
Gonzalez-Barca E, Fernandez-Sevilla A, Carratala J, Granena A, Gudiol F (1996) Prospective study of 288 episodes of bacteremia in neutropenic cancer patients in a single institution. Eur J Clin Microbiol Infect Dis 15:291–296
Griffiths NJ, Bradley CJ, Heyderman RS, Virji M (2007) IFN-gamma amplifies NFkappaB-dependent Neisseria meningitidis invasion of epithelial cells via specific upregulation of CEA-related cell adhesion molecule 1. Cell Microbiol 9:2968–2983
Heiniger N, Spaniol V, Troller R, Vischer M, Aebi C (2007) A reservoir of Moraxella catarrhalis in human pharyngeal lymphoid tissue. J Infect Dis 196:1080–1087
Helminen ME, Maciver I, Paris M, Latimer JL, Lumbley SL, Cope LD, McCracken GH Jr, Hansen EJ (1993) A mutation affecting expression of a major outer membrane protein of Moraxella catarrhalis alters serum resistance and survival in vivo. J Infect Dis 168:1194–1201
Hill AT, Campbell EJ, Hill SL, Bayley DL, Stockley RA (2000) Association between airway bacterial load and markers of airway inflammation in patients with stable chronic bronchitis. Am J Med 109:288–295
Jagetia GC, Aggarwal BB (2007) “Spicing up” of the immune system by curcumin. J Clin Immunol 27:19–35
Lin YT, Wang LF, Hsu YC (2009) Curcuminoids suppress the growth of pharynx and nasopharyngeal carcinoma cells through induced apoptosis. J Agric Food Chem 57:3765–3770
Logan RM, Stringer AM, Bowen JM, Yeoh AS, Gibson RJ, Sonis ST, Keefe DM (2007) The role of pro-inflammatory cytokines in cancer treatment-induced alimentary tract mucositis: pathobiology, animal models and cytotoxic drugs. Cancer Treat Rev 33:448–460
Muenzner P, Billker O, Meyer TF, Naumann M (2002) Nuclear factor-kappa B directs carcinoembryonic antigen-related cellular adhesion molecule 1 receptor expression in Neisseria gonorrhoeae-infected epithelial cells. J Biol Chem 277:7438–7446
Murphy TF, Parameswaran GI (2009) Moraxella catarrhalis, a human respiratory tract pathogen. Clin Infect Dis 49:124–131
Palmu AA, Herva E, Savolainen H, Karma P, Makela PH, Kilpi TM (2004) Association of clinical signs and symptoms with bacterial findings in acute otitis media. Clin Infect Dis 38:234–242
Perez Vidakovics ML, Riesbeck K (2009) Virulence mechanisms of Moraxella in the pathogenesis of infection. Curr Opin Infect Dis 22:279–285
Rai D, Singh JK, Roy N, Panda D (2008) Curcumin inhibits FtsZ assembly: an attractive mechanism for its antibacterial activity. Biochem J 410:147–155
Revai K, McCormick DP, Patel J, Grady JJ, Saeed K, Chonmaitree T (2006) Effect of pneumococcal conjugate vaccine on nasopharyngeal bacterial colonization during acute otitis media. Pediatrics 117:1823–1829
Rezvani M, Ross GA (2004) Modification of radiation-induced acute oral mucositis in the rat Int. J Radiat Biol 80:177–182
Rovers MM, Schilder AG, Zielhuis GA, Rosenfeld RM (2004) Otitis media. Lancet 363:465–473
Singh S, Aggarwal BB (1995) Activation of transcription factor NF-kappa B is suppressed by curcumin (diferuloylmethane) [corrected]. J Biol Chem 270:24995–25000
Slevogt H, Maqami L, Vardarowa K, Beermann W, Hocke AC, Eitel J, Schmeck B, Weimann A, Opitz B, Hippenstiel S, Suttorp N, N'Guessan PD (2008) Differential regulation of Moraxella catarrhalis-induced interleukin-8 response by protein kinase C isoforms. Eur Respir J 31:725–735
Slevogt H, Schmeck B, Jonatat C, Zahlten J, Beermann W, van Laak V, Opitz B, Dietel S, N'Guessan PD, Hippenstiel S, Suttorp N, Seybold J (2006) Moraxella catarrhalis induces inflammatory response of bronchial epithelial cells via MAPK and NF-kappaB activation and histone deacetylase activity reduction. Am J Physiol Lung Cell Mol Physiol 290:L818–L826
Slevogt H, Seybold J, Tiwari KN, Hocke AC, Jonatat C, Dietel S, Hippenstiel S, Singer BB, Bachmann S, Suttorp N, Opitz B (2007) Moraxella catarrhalis is internalized in respiratory epithelial cells by a trigger-like mechanism and initiates a TLR2- and partly NOD1-dependent inflammatory immune response. Cell Microbiol 9:694–707
Sonis ST (1998) Mucositis as a biological process: a new hypothesis for the development of chemotherapy-induced stomatotoxicity. Oral Oncol 34:39–43
Spaniol V, Heiniger N, Troller R, Aebi C (2008) Outer membrane protein UspA1 and lipooligosaccharide are involved in invasion of human epithelial cells by Moraxella catarrhalis. Microbes Infect 10:3–11
Spaniol V, Troller R, Aebi C (2009) Physiologic cold shock increases adherence of Moraxella catarrhalis to and secretion of interleukin 8 in human upper respiratory tract epithelial cells. J Infect Dis 200:1593–1601
van't Land B, Blijlevens NM, Marteijn J, Timal S, Donnelly JP, de Witte TJ, M'Rabet L (2004) Role of curcumin and the inhibition of NF-kappaB in the onset of chemotherapy-induced mucosal barrier injury. Leukemia 18:276–284
Wessler S, Muenzner P, Meyer TF, Naumann M (2005) The anti-inflammatory compound curcumin inhibits Neisseria gonorrhoeae-induced NF-kappaB signaling, release of pro-inflammatory cytokines/chemokines and attenuates adhesion in late infection. Biol Chem 386:481–490
Acknowledgements
This work was funded in part by grant number 3100A0-116053 (to C.A.) from the Swiss National Science Foundation. Strain 035E and the monoclonal antibodies 24B5 and 10F3 are a kind gift of Dr. Eric Hansen, University of Texas Southwestern Medical Center, Dallas, TX, USA.
Conflict of interest
None declared.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lüer, S., Troller, R., Jetter, M. et al. Topical curcumin can inhibit deleterious effects of upper respiratory tract bacteria on human oropharyngeal cells in vitro: potential role for patients with cancer therapy induced mucositis?. Support Care Cancer 19, 799–806 (2011). https://doi.org/10.1007/s00520-010-0894-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-010-0894-x