Abstract
Goals of work
The purpose of this study was to better understand various variables related to food intake and eating problems in children with cancer during their chemotherapy.
Patients and methods
Twenty-two consecutively admitted children, diagnosed with cancer and undergoing chemotherapy, participated in this study. Twenty-one of them, their parents and attending nurses participated in semi-structured interviews. Ten of the children underwent a taste acuity test, and recognition thresholds for the four basic tastes were determined.
Main results
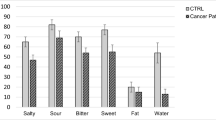
The shared view of both children and parents was that altered taste was the predominant cause of the eating problems. In contrast, the nurses perceived that nausea was the most important cause of the children’s eating problems. In addition, psychological aspects such as learned food aversions and negative attitudes towards hospital food were regarded as important by children, parents and nurses. The taste test showed that the patients had higher thresholds for bitter taste and made more taste recognition errors compared to controls.
Conclusions
Changes seem to exist both in the primary gustatory sense as well as in food perception in paediatric cancer patients undergoing chemotherapy. Single solutions, such as efforts to serve “tasty food”, do not suffice alone. A more effective solution may be to combine different strategies and combinations of oral, enteral and parenteral nutrition should be considered to prevent malnutrition.
Similar content being viewed by others
References
Albertsson Wikland K, Luo ZC, Niklasson A, Karlberg J (2002) Swedish population-based longitudinal reference values from birth to 18 years of age for height, weight and head circumference. Acta Paediatr 91:739–754
Barale K, Aker SN, Martinsen CS (1982) Primary taste thresholds in children with leukemia undergoing marrow transplantation. J Parenter Enteral Nutr 6:287–290
Berde CB, Billett AL, Collins JJ (2002) Symptom management in supportive care. In: Pizzo PA, Poplack DG (eds) Principles and practice of pediatric oncology. Lippincott Williams & Wilkins, Philadelphia, pp 1302–1332
Bernstein IL (1978) Learned taste aversions in children receiving chemotherapy. Science 200:1302–1303
Bernstein IL (1999) Taste aversion learning: a contemporary perspective. Nutrition 15:229–234
Berteretche MV, Dalix AM, dÓrnano AM, Bellisle F, Khayat D, Faurion A (2004) Decreased taste sensitivity in cancer patients under chemotherapy. Support Care Cancer 12:571–576
Birch LL (1999) Development of food preferences. Annu Rev Nutr 19:41–62
Boman KK, Viksten J, Kogner P, Samuelsson U (2004) Serious illness in childhood: the different threats of cancer and diabetes from a parent perspective. J Pediatr 145:373–379
Comeau TB, Epstein JB, Migas C (2001) Taste and smell dysfunction in patients receiving chemotherapy: a review of current knowledge. Support Care Cancer 9:575–580
Cornsweet TN (1962) The staircase-method in psychophysics. Am J Psychol 75:485–591
Davies CM, Noll RB, Davies WH, Bukowski WM (1993) Mealtime interactions and family relationships of families with children who have cancer in long-term remission and controls. J Am Diet Assoc 93:773–776
Delbecque-Boussard L, Gottrand F, Ategbo S, Nelken B, Mazingue F, Vic P, Farriaux JP, Turck D (1997) Nutritional status of children with acute lymphoblastic leukemia: a longitudinal study. Am J Clin Nutr 65:95–100
Drewnowski A (1997) Taste preferences and food intake. Annu Rev Nutr 17:237–253
Fallon AE, Rozin P, Pliner P (1984) The child’s conception of food: the development of food rejections with special reference to disgust and contamination sensitivity. Child Dev 55:566–575
Fischler C (1988) Food, self and identity. Soc Sci Inform 27:275–293
Hawkes CH (2002) Smell and taste complaints. Butterworth Heinemann, Amsterdam, pp 123–179
Hockenberry M (2004) Symptom management research in children with cancer. J Pediatr Oncol Nurs 21:132–136
Holm L, Smidt S (1997) Uncovering social structures and status differences in health systems. Eur J Public Health 7:373–378
Holm L, Smidt S, Michaelsen KF (1996) Socio-psychological significance of hospital meals—the impact of the introduction of a new catering system in a children’s cancer ward. Scand J Nutr 40:6–10
Kennedy DD, Tucker KL, Ladas ED, Rheingold SR, Blumberg J, Kelly KM (2004) Low antioxidant vitamin intakes are associated with increases in adverse effects of chemotherapy in children with acute lymphoblastic leukaemia. Am J Clin Nutr 79:1029–1036
Krippendorf K (1980) Content analysis. An introduction to its methodology. Sage Publications, Beverly Hills
Kvist SB, Rajantie J, Kvist M, Siimes MA (1991) Perceptions of problematic events and quality of care among patients and parents after successful therapy of the child’s malignant disease. Soc Sci Med 33:249–256
Lee K (1989) Food neophobia: major causes and treatments. Food Technol 43:62–73
Murry DJ, Riva L, Poplack DG (1998) Impact of nutrition on pharmacokinetics of anti-neoplastic agents. Int J Cancer 11:48–51
Nilsson H, Holm AK (1983) Taste thresholds, taste preferences and dental caries in 15-year-olds. J Dent Res 62:1069–1072
Nordic Society of Pediatric Haematology and Oncology (NOPHO) (2004) Childhood cancer in the Nordic countries. Report on epidemiologic and therapeutic results from registries and working groups. NOPHO Annual Meeting, Odense
Pelchat ML, Rozin P (1982) The special role of nausea in the acquisition of food dislikes by humans. Appetite 3:341–351
Reilly JJ, Brougham M, Montgomery C, Richardson F, Kelly A, Gibson BE (2001) Effect of glucocorticoid treatment on energy intake in children treated for acute lymphoblastic leukemia. J Clin Endocrinol Metab 86:3742–3745
Sala A, Pencharz P, Barr RD (2004) Children, cancer and nutrition—a dynamic triangle in review. Cancer 100:677–687
Schiffman SS (1997) Taste and smell losses in normal aging and disease. JAMA 278:1357–1362
Schnell FM (2003) Chemotherapy-induced nausea and vomiting: the importance of acute antiemetic control. Oncologist 8:187–198
Scrimshaw NS (2003) Historical concepts of interactions, synergism and antagonisms between nutrition and infection. J Nutr 133:316–321
Skolin I, Axelsson K, Ghannad P, Hernell O, Wahlin YB (1997) Nutrient intake and weight development in children during chemotherapy for malignant disease. Oral Oncol 33:364–368
Skolin I, Hernell O, Wahlin YB (2001) Energy and nutrient intake and nutritional status of children with malignant disease during chemotherapy after the introduction of new mealtime routines. Scand J Caring Sci 15:82–91
Skolin I, Hursti UK, Wahlin YB (2001) Parents’ perception of their child’s food intake after the start of chemotherapy. J Pediatr Oncol Nurs 18:124–136
Wall DT, Gabriel LA (1983) Alteration of taste in children with leukemia. Cancer Nurs 6:447–452
Williams R, Virtue K, Adkins A (1998) Room service improves patient food intake and satisfaction with hospital food. J Pediatr Oncol Nurs 15:183–189
Acknowledgements
This study was financed by the Children’s Cancer Foundation in Sweden and by the Gunnar Nilsson Cancer Foundation. The authors wish to thank the patients, parents and staff at the Paediatric Haematology and Oncology Unit at Umeå University Hospital. Special thanks to Siv Inger Eliasson for the medical records’ review, Margareta Holmgren for carrying out the taste acuity tests and Lena Carling for providing the software program for the anthropometry analysis. We are indebted to Dr. Gregory Neely and Gareth Morgan for valuable comments on the manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Skolin, I., Wahlin, Y.B., Broman, D.A. et al. Altered food intake and taste perception in children with cancer after start of chemotherapy: perspectives of children, parents and nurses. Support Care Cancer 14, 369–378 (2006). https://doi.org/10.1007/s00520-005-0904-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-005-0904-6