Summary
Background
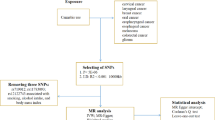
Cannabis use is increasing annually but the relationship between cannabis use and cancer incidence is not uniform because of confounding factors. We aimed to assess the effect of cannabis use on cancer risk using a two-sample Mendelian randomization (MR) approach.
Methods
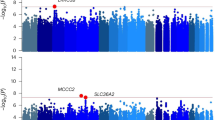
Secondary data analyses were performed on pooled data based on Genome-Wide Association Study (GWAS), selecting data from the ICC and UK-Biobank and 23andMeInc lifetime cannabis use and cannabis use disorder related to the substance use disorders working group from the Psychiatric Genomics Consortium, then selecting highly correlated SNPs as instrumental variables. The substance use disorders working group, iPSYCH, and deCODE GWAS data, and then highly correlated SNPs were selected as instrumental variables for two-sample Mendelian randomization analyses using inverse variance weighting, MR-Egger regression, and weighted median, respectively, to evaluate the relationship between lifetime cannabis use and nine tumors, and subsequently analyzed these results in the same way using cannabis use disorders.
Results
The risk of all cancers except breast cancer was not associated with lifetime cannabis use. Our inverse variance weighting method found that lifetime marijuana use reduced the breast cancer risk (P = 0.016, odds ratio [OR] = 0.981), and we subsequently conducted analyses of cannabis use disorders and cancer risk, which showed that cannabis use disorders elevated the risk of breast cancer (P = 0.007, OR = 1.007) as well as the risk of lung cancer (P = 0.014, OR = 1.122).
Conclusion
Large MR analyses suggest that lifetime cannabis use may reduce breast cancer risk, but cannabis use disorder exacerbates the risk of breast and lung cancer. The mechanisms responsible for this outcome remain to be investigated.



Similar content being viewed by others
References
Hall W. What has research over the past two decades revealed about the adverse health effects of recreational cannabis use? Addiction. 2015;110:19–35.
Lowe DJE, Sasiadek JD, Coles AS, George TP. Cannabis and mental illness: a review. Eur Arch Psychiatry Clin Neurosci. 2019;269:107–20.
Volkow ND, Baler RD, Compton WM, Weiss SRB. Adverse health effects of marijuana use. N Engl J Med. 2014;370:2219–27.
Hall W, Lynskey M. Evaluating the public health impacts of legalizing recreational cannabis use in the United States. Addiction. 2016;111:1764–73.
Hall W, Weier M. Assessing the public health impacts of legalizing recreational cannabis use in the USA. Clin Pharmacol Ther. 2015;97:607–15.
Nigatu YT, Elton-Marshall T, Rueda S, Imtiaz S, Hamilton HA. Age, period and cohort effects on time trends in monthly cannabis use in adult population: 1996–2019. Drug Alcohol Rev. 2023; https://doi.org/10.1111/dar.13658.
Siegel RL, Miller KD, Wagle NS, Jemal A. Cancer statistics. CA A Cancer J Clinicians. 2023;73:17–48.
Ghasemiesfe M, Barrow B, Leonard S, Keyhani S, Korenstein D. Association between Marijuana use and risk of cancer: a systematic review and meta-analysis. JAMA Netw Open. 2019;2:e1916318.
Erzurumlu Y, Catakli D, Sezer S. Cannabidiol negatively regulates androgenic signal in prostate cancer cells and fine-tunes the tumorigenesis by modulating endoplasmic reticulum-associated degradation, unfolded protein response, and autophagy. Rev Bras Farmacogn. 2023;33:316–25.
Motadi LR, Jantjies ZE, Moleya B. Cannabidiol and Cannabis Sativa as a potential treatment in vitro prostate cancer cells silenced with RBBp6 and PC3 xenograft. Mol Biol Rep. 2023; https://doi.org/10.1007/s11033-022-08197-0.
Whynot EG, Tomko AM, Dupré DJ. Anticancer properties of cannabidiol and ∆9-tetrahydrocannabinol and synergistic effects with gemcitabine and cisplatin in bladder cancer cell lines. J Cannabis Res. 2023;5:7.
Zhong N, Li D, Wang B, Kovalchuk O, Kovalchuk I. Cannabinol inhibits cell growth and triggers cell cycle arrest and apoptosis in cancer cells. Biocatal Agric Biotechnol. 2023;48:102627.
AminiLari M, Wang L, Neumark S, Adli T, Couban RJ, Giangregorio A, et al. Medical cannabis and cannabinoids for impaired sleep: a systematic review and meta-analysis of randomized clinical trials. Sleep. 2022;45:zsab234.
Croker JA, Bobitt J, Arora K, Kaskie B. Cannabis and palliative care utilization among non-terminal cancer patients in the illinois medical cannabis program. Psychoactives. 2023;2:52–65.
Jafri S, Hansen E, Fuenmayor R, Case AA. Medical Cannabis for insomnia in a patient with advanced breast cancer. J Pain Symptom Manage. 2023;65:e497–e502.
Wang L, Hong PJ, May C, Rehman Y, Oparin Y, Hong CJ, et al. Medical cannabis or cannabinoids for chronic non-cancer and cancer related pain: a systematic review and meta-analysis of randomised clinical trials. BMJ. 2021; https://doi.org/10.1136/bmj.n1034.
Smith DG, Ebrahim S. ‘Mendelian randomization’: can genetic epidemiology contribute to understanding environmental determinants of disease? Int J Epidemiol. 2003;32:1–22.
Hemani G, Zheng J, Elsworth B, Wade KH, Haberland V, Baird D, et al. The MR-Base platform supports systematic causal inference across the human phenome. Elife. 2018;7:e34408.
Voirin N, Berthiller J, Benhaïm-Luzon V, Boniol M, Straif K, Ayoub WB, et al. Risk of lung cancer and past use of cannabis in Tunisia. J Thorac Oncol. 2006;1:577–9.
Bouti K, Borki R, Fenane H, Harrak L. Cannabis smoking and risk of lung cancer—a systematic review and meta-analysis. IJMS. 2014;1:31–7.
Takeda S, Yamamoto I, Watanabe K. Modulation of Delta9-tetrahydrocannabinol-induced MCF‑7 breast cancer cell growth by cyclooxygenase and aromatase. Toxicology. 2009;259:25–32.
Ligresti A, Moriello AS, Starowicz K, Matias I, Pisanti S, De Petrocellis L, et al. Antitumor activity of plant cannabinoids with emphasis on the effect of cannabidiol on human breast carcinoma. J Pharmacol Exp Ther. 2006;318:1375–87.
Acknowledgements
The authors would like to thank all the researchers for their contributions to the establishment and management of the MRC IEU open GWAS project.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Data availability statement
The data that support the findings of this study are openly available in the OpenGWAS database (https://gwas.mrcieu.ac.uk/datasets/).
Supplementary Information
Rights and permissions
About this article
Cite this article
Niu, D., Li, C., Qu, H. et al. Does cannabis elevate cancer risk?. Wien Klin Wochenschr (2023). https://doi.org/10.1007/s00508-023-02303-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00508-023-02303-3