Abstract
Background
As the cost of health care increases in the US, focus has been placed upon efficiency, cost reduction, and containment of spending. Operating room costs play a significant role in this spending. We investigated whether surgeon education and universal preference cards can have an impact on reducing the disposable supply costs for common laparoscopic general surgery procedures.
Methods
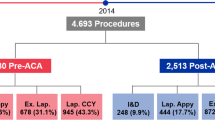
General surgeons at two institutions participated in an educational session about the costs of the operative supplies used to perform laparoscopic appendectomies and cholecystectomies. All the surgeons at one institution agreed upon a universal preference card, with other supplies opened only by request. At the other, no universal preference cards were created, and surgeons were free to modify their own existing preference cards. Case cost data for these procedures were collected for each institution pre- (July 2014-December 2014) and post-intervention (February 2015–November 2017).
Results
At the institution with an education only program, there was no statistically significant change in supply costs after the intervention. At the institution that intervened with the combined education and universal preference card program, there was a statistically significant supply cost decrease for these common laparoscopic procedures combined. This significant cost decrease persisted for each appendectomies and cholecystectomies when analyzed independently as well (p = 0.001 and p < 0.001 respectively).
Conclusions
In this study, surgeon education alone was not effective in reducing operating room disposable supply costs. Surgeon education, combined with the implementation of universal preference cards, significantly maintains reductions in operating room supply costs. As health care costs continue to increase in the US and internationally, universal preference cards can be an effective tool to contain cost for common laparoscopic general surgery procedures.
Similar content being viewed by others
References
Chu T, Chandhoke RA, Smith PC, Schwaitzberg SD (2011) The Impact of surgeon choice on the cost of performing laparoscopic appendectomy. Surg Endosc 25:1187–1191
Wehrman WE, Tangren CM, Inge TH (2007) Cost analysis of ligature versus stapling techniques of laparoscopic appendectomy in children. J Laparoendosc Adv Surg Tech A 3:371–374
Parikh PP, Tashiro J, Wagenaar AE, Curbelo M, Perez EA, Neville HL, Hogan AR, Sola JE (2018) Looped suture versus stapler device in pediatric laparoscopic appendectomy: a comparative outcomes and intraoperative cost analysis. J Pediatr Surg 53:616–619
Al-Temimi MH, Berglin MA, Kim EG, Tessier DJ, Johna SD (2017) Endostapler versus Hem-O-Lok Clip to secure the appendiceal stump and mesoappendix during laparoscopic appendectomy. Am J Surg 214:1149–1150
Mehdorn M, Schürmann O, Mehdorn HM, Gockel I (2017) Intended cost reduction in laparoscopic appendectomy by introducing the endoloop: a single center experience. BMC Surg 17:80
Kim S, Weireter L (2018) Cost effectiveness of different methods of appendiceal stump closure during laparoscopic appendectomy. Am Surg 84:1329–1332
Brauer DG, Hawkins WG, Strasberg SM, Brunt LM, Jaques DP, Mercurio NR, Hall BL, Fields RC (2015) Cost variation in a laparoscopic cholecystectomy and the association with outcomes across a single health system: implications for standardization and improved resource utilization. HPB (Oxford) 17:1113–1118
Guzman MJ, Gitelis ME, Linn JG, Ujiki MB, Waskerwitz M, Umanskiy K, Muldoon JP (2015) A Model of cost reduction and standardization: improved cost savings while maintaining the quality of care. Dis Colon Rectum 58:1104–1107
Robinson JR, Carter NH, Gibson C, Brinkman AS, Van Arendonk K, Speck KE, Danko ME, Jackson GP, Lovvorn HN 3rd, Blakely ML (2018) Improving the value of care for appendectomy through an individual surgeon-specific approach. J Pediatr Surg 53:1181–1186
Gitelis M, Vigneswaran Y, Ujiki MB, Denham W, Talamonti M, Muldoon JP, Linn JG (2015) Educating surgeons on intraoperative disposable supply costs during laparoscopic cholecystectomy: a regional health system’s experience. Am J Surg 209:488–492
Simon KL, Frelich MJ, Gould JC (2018) Picking apart surgical pick lists—reducing variation to decrease surgical costs. Am J Surg 215:19–22
Skarda DE, Rollins M, Andrews S, McFadden M, Barnhart D, Meyers R, Scaife E (2015) One hospital, one appendectomy: the cost effectiveness of a standardized doctor’s preference card. J Pediatr Surg 50:919–922
Avansino JR, Goldin AB, Risley R, Waldhausen JH, Sawin RS (2013) Standardization of operative equipment reduces cost. J Pediatr Surg 48:1843–1849
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs. Embick, Yang, and Koehler, and Michael Bieri have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Embick, E., Bieri, M., Koehler, T.J. et al. Cost containment: an experience with surgeon education and universal preference cards at two institutions. Surg Endosc 34, 5148–5152 (2020). https://doi.org/10.1007/s00464-019-07305-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-019-07305-9