Abstract
This study aimed to assess the associated-risk determinants for cutaneous leishmaniasis (CL) in patients with diabetes mellitus (DM) compared to patients without DM. This case–control study was performed between 2017 and 2019 in southeastern Iran. Overall, 206 participants were selected from patients with DM without CL (11.2%), patients with CL without DM (6.2%), and DM patients concomitance with CL (27.6%) as case groups and healthy individuals as a control group 64 (76%). These cases were compared for parasitological, immunological, biochemical, and hematological parameters. The findings demonstrated that parasitological factors regarding the number, duration, and size of the lesion in CL patients showed a significant difference among patients with and without DM (p < 0.05). Data analysis showed that six major risk factors, including female (odds ratio (OR) = 3.47, confidence interval (CI) = 1.84–6.53, p < 0.001), total protein in CL group (OR = 4.9, CI = 2.3–10.44, p < 0.001), alanine aminotransferase (ALT) concentration in CL group (OR = 0.87, CI = 0.81–0.93, p < 0.001) and DM co-infected with CL group (OR = 0.8, CI = 0.72–0.88, p < 0.001) than healthy group, aspartate aminotransferase (AST) concentration in DM group (OR = 0.86, CI = 0.76–0.98, p = 0.02), transforming growth factor beta)TGF-β( level in the CL group (OR = 1.03, CI = 1.003–1.05, p = 0.02), and presence of diabetes disease (OR = 2.07, CI = 1.16–3.7, p < 0.05), were significantly linked with the induction of CL lesion. The findings demonstrated a significant relationship between DM and CL in distinct risk determinants. Also, the study revealed that DM enhanced the severity of active CL.

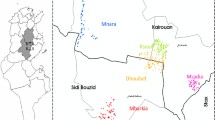
taken from diabetics (A–D) and non-diabetic patients (E–H) in endemic areas with CL in southeastern Iran
Similar content being viewed by others
Data availability
The datasets used and analyzed during the current study are available from the corresponding author on reasonable request.
Code availability
Not applicable.
Abbreviations
- L:
-
Leishmania
- DM:
-
Diabetes mellitus
- CL:
-
Cutaneous leishmaniasis
- OR:
-
Odds ratio
- CI:
-
Confidence interval
- AST:
-
Aspartate aminotransferase
- ALT:
-
Alanine aminotransferase
- ALP:
-
Alkaline phosphatase
- WBC:
-
White blood cell
- RBC:
-
Red blood cell
- TGF-β:
-
Transforming growth factor-beta
- IL:
-
Interleukin
- INF:
-
Interferon
References
Abdoli A, Maspi N, Ghaffarifar F (2017) Wound healing in cutaneous leishmaniasis: a double edged sword of IL-10 and TGF-β. Comp Immunol Microbiol Infect Dis 51:15–26
Aflatoonian MR, Sharifi I, Hakimi Parizi M et al (2014) A prospective cohort study of cutaneous leishmaniasis risk and opium addiction in south eastern Iran. PLoS ONE 9:e89043. https://doi.org/10.1371/journal.pone.0089043
Akash MSH, Rehman K, Fiayyaz F et al (2020) Diabetes-associated infections: development of antimicrobial resistance and possible treatment strategies. Arch Microbiol 202:953–965
Akbarzadeh A, Salehi A, Vardanjani HM et al (2019) Epidemiology of adult diabetes mellitus and its correlates in pars cohort study in southern Iran. Arch Iran Med 22:633–639
Al-Safar H, Kamal W, Hassoun A et al (2015) Combined association analysis of interleukin 1-receptor antagonist (IL-1RN) variable number of tandem repeat (VNTR) and Haptoglobin 1/2 polymorphisms with type 2 diabetes mellitus risk. J Diabetes Metab Disord 15:1–8
Alemayehu B, Alemayehu M (2017) Leishmaniasis: a review on parasite, vector and reservoir host. Heal Sci J 11:1
Bailey F, Mondragon-Shem K, Hotez P et al (2017) A new perspective on cutaneous leishmaniasis—implications for global prevalence and burden of disease estimates. PLoS Negl Trop Dis 11:e0005739. https://doi.org/10.1371/journal.pntd.0005739
Baker MA, Harries AD, Jeon CY et al (2011) The impact of diabetes on tuberculosis treatment outcomes: a systematic review. BMC Med 9:1–15
Bamorovat M, Sharifi I, Aflatoonian MR, et al (2019) Host’s immune response in unresponsive and responsive patients with anthroponotic cutaneous leishmaniasis treated by meglumine antimoniate: a case-control study of Th1 and Th2 pathways. Int Immunopharmacol 69:321-327
Bamorovat M, Sharifi I, Aflatoonian MR et al (2018) Risk factors for anthroponotic cutaneous leishmaniasis in unresponsive and responsive patients in a major focus, southeast of Iran. PLoS ONE 13:e0192236. https://doi.org/10.1371/journal.pone.0192236
Bamorovat M, Sharifi I, Dabiri S et al (2021) Major risk factors and histopathological profile of treatment failure, relapse and chronic patients with anthroponotic cutaneous leishmaniasis: a prospective case-control study on treatment outcome and their medical importance. PLoS Negl Trop Dis 15:e0009089
Bonyek-Silva I, Nunes S, Santos RL et al (2020) Unbalanced production of LTB4/PGE2 driven by diabetes increases susceptibility to cutaneous leishmaniasis. Emerg Microbes Infect 9:1275–1286
Burza S, Croft SL, Boelaert M (2018) Leishmaniasis. Lancet (london, England) 392:951–970. https://doi.org/10.1016/S0140-6736(18)31204-2
Casqueiro J, Casqueiro J, Alves C (2012) Infections in patients with diabetes mellitus: a review of pathogenesis. Indian J Endocrinol Metab 16:S27
Cox FE (2001) Concomitant infections, parasites and immune responses. Parasitology 122(Suppl):S23-38
da Silva DAM, Santana FR, Katz S et al (2020) Protective cellular immune response induction for cutaneous leishmaniasis by a new immunochemotherapy schedule. Front Immunol 11:1–12. https://doi.org/10.3389/fimmu.2020.00345
Dubie T (2020) Review article review on the role of host immune response in protection and immunopathogenesis during cutaneous leishmaniasis infection 2020:2496713
Gautam S, Shrestha N, Mahato S et al (2021) Diabetes among tuberculosis patients and its impact on tuberculosis treatment in South Asia: a systematic review and meta-analysis. Sci Rep 11:1–12
Geerlings SE, Hoepelman AI (1999) Immune dysfunction in patients with diabetes mellitus (DM). FEMS Immunol Med Microbiol 26:259–265
Haj S, Chodick G, Goren S et al (2021) Differences in glycated hemoglobin levels and cholesterol levels in individuals with diabetes according to Helicobacter pylori infection. Sci Rep 11:1–9
Harries AD, Kumar AMV, Satyanarayana S et al (2016) Addressing diabetes mellitus as part of the strategy for ending TB. Trans R Soc Trop Med Hyg 110:173–179
Jeon CY, Murray MB (2008) Diabetes mellitus increases the risk of active tuberculosis: a systematic review of 13 observational studies. PLoS Med | www 5:1091. https://doi.org/10.1371/journal.pmed.0050152
Karimi A, Hanafi-Bojd AA, Yaghoobi-Ershadi MR et al (2014) Spatial and temporal distributions of phlebotomine sand flies (Diptera: Psychodidae), vectors of leishmaniasis, in Iran. Acta Trop 132:131–139. https://doi.org/10.1016/j.actatropica.2014.01.004
Khaledi S, Moridi G, Gharibi F (2011) Survey of eight dimensions quality of life for patients with diabetes type II, referred to Sanandaj diabetes center in 2009. J Fasa Univ Med Sci 1:29–37
Lago AS, Lima FR, Carvalho AM, et al (2020) Diabetes modifies the clinic presentation of cutaneous leishmaniasis. In: open forum infectious diseases. Oxford University Press US 7(12):ofaa491
Mahmoudi A (2006) Effects of self care planning on reduction of A1C hemoglobin in adults with diabetes mellitus. Med Sci J Islam Azad Univesity - Tehran Med Branch 16:171–176
Matima R, Murphy K, Levitt NS et al (2018) A qualitative study on the experiences and perspectives of public sector patients in Cape town in managing the workload of demands of HIV and type 2 diabetes multimorbidity. PLoS ONE 13:e0194191. https://doi.org/10.1371/journal.pone.0194191
Mave V, Gaikwad S, Barthwal M, et al (2021) Diabetes mellitus and tuberculosis treatment outcomes in Pune, India. Open forum infectious diseases 8(4):ofab097
Nieva CAB, Cid AG, Romero AI et al (2021) An appraisal of the scientific current situation and new perspectives in the treatment of cutaneous leishmaniasis. Acta Trop 221:105988
Nosratabadi R, Arababadi MK, Hassanshahi G et al (2009) Evaluation of IFN-gamma serum level in nephropatic type 2 diabetic patients. Pakistan J Biol Sci PJBS 12:746–749
Rider V, GubbelsBupp MR, Bupp GM et al (2018) The confluence of sex hormones and aging on immunity. Immunity Front Immunol 9:1269. https://doi.org/10.3389/fimmu.2018.01269
Ridzuan N, John CM, Sandrasaigaran P et al (2016) Preliminary study on overproduction of reactive oxygen species by neutrophils in diabetes mellitus. World J Diabetes 7:271
Rushton DH, Dover R, Sainsbury AW et al (2001) Why should women have lower reference limits for haemoglobin and ferritin concentrations than men? Br Med J 322:1355–1357
Saghafipour A, Rassi Y, Abai M, Oshaghi M (2013) Outbreak of zoonotic cutaneous leishmaniasis: a report. Arch Hyg Sci 2(2):48–54
Seuring T, Archangelidi O, Suhrcke M (2015) The economic costs of type 2 diabetes: a global systematic review. Pharmacoeconomics 33:811–831. https://doi.org/10.1007/s40273-015-0268-9
Sharifi I, Aflatoonian MR, Fekri AR et al (2015) A comprehensive review of cutaneous leishmaniasis in kerman province, southeastern iran-narrative review article. Iran J Public Health 44:299–307
Sharifi I, Fekri AR, Aflatonian M-R et al (1998) Randomised vaccine trial of single dose of killed Leishmania major plus BCG against anthroponotic cutaneous leishmaniasis in Bam. Iran Lancet 351:1540–1543. https://doi.org/10.1016/S0140-6736(98)09552-X
Sison JP, Kemper CA, Loveless M et al (1995) Disseminated acanthamoeba infection in patients with AIDS: case reports and review. Clin Infect Dis 20:1207–1216
Skopiński P, Rogala E, Duda-Król B et al (2005) Increased interleukin-18 content and angiogenic activity of sera from diabetic (type 2) patients with background retinopathy. J Diabetes Complications 19 (6):335–338
Sokal JE (1975) Measurement of delayed skin-test responses.N Engl J Med 293:501-502
Stalenhoef JE, Alisjahbana B, Nelwan EJ et al (2008) The role of interferon-gamma in the increased tuberculosis risk in type 2 diabetes mellitus. Eur J Clin Microbiol Infect Dis 27 (2):97–103
Torres-Guerrero E, Quintanilla-Cedillo MR, Ruiz-Esmenjaud J, Arenas R (2017) Leishmaniasis: a review. F1000Research 6:750
Unnikrishnan R, Pradeepa R, Joshi SR, Mohan V (2017) Type 2 diabetes: demystifying the global epidemic. Diabetes 66:1432–1442
World Health Organization (WHO) (2019) Classification of diabetes mellitus. International Diabetes Federation 6–10
World Health Organization (2014) Manual for case management of cutaneous leishmaniasis in the WHO Eastern Mediterranean Region. WHO Regional Publications, Eastern Mediterranean Series 1–50
Zimmet P (2000) Globalization, coca-colonization and the chronic disease epidemic: can the Doomsday scenario be averted? J Intern Med 247:301–310
Acknowledgements
We would like to express our heartfelt thanks to the health personnel of the Bam Health Center. Special thanks to Dr. Dabiri and Mr.Karimi and Kerman University of Medical Sciences that helped carry out this study.
Funding
This work was financially supported by grant No. 95/230 from Kerman University of Medical Sciences.
Author information
Authors and Affiliations
Contributions
ISh administered and supervised the work. GhA, ISh, and MM conceived and designed the experiments. SK and MM performed the experiments. NN, MM, and MRA analyzed and interpreted the patient data. MM and SK wrote the first draft of the paper. ISh, MB, and RTO reviewed and corrected the paper. All authors reviewed and approved the manuscript.
Corresponding author
Ethics declarations
Ethics approval
The survey protocol was reviewed and approved by the joint Ethics Committees of the Leishmaniasis Research Center and Vice-Chancellor for Research, Kerman University of Medical Sciences, under protocol number 95/230.
Consent to participate
The participants signed a consent sheet. Informed consent was obtained from a parent or guardian for participants under 16 years old.
Consent for publication
Not applicable.
Conflict of interest
The authors declare no competing interests.
Disclaimer
The funders had no role in study design, data collection and analysis, decision to publish, or manuscript preparation.
Additional information
Section Editor: Sarah Hendrickx
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Mostafavi, M., Sharifi, I., Asadikaram, G. et al. The impact of diabetes on cutaneous leishmaniasis: a case–control field assessment. Parasitol Res 120, 3865–3874 (2021). https://doi.org/10.1007/s00436-021-07255-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00436-021-07255-z