Abstract
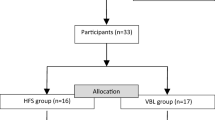
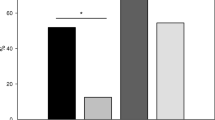
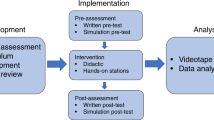
Compliance by residents in pediatrics to pediatric resuscitation guidelines is low. In many French faculties, a 1-h traditional lecture is still used to educate medical students about pediatric cardiopulmonary arrest (CPA). We developed an innovative pedagogic course combining a 23-min video and 3-h simulation exercises to improve knowledge and skills of medical students. A prospective controlled study was conducted. Medical student knowledge was tested before, just after, and 6–12 months after the innovative course and compared to that of a cohort who attended the traditional lecture. A high-fidelity mannequin simulator simulating cardiopulmonary arrest was used to assess and compare the skills of the study and control groups. Costs of the courses were evaluated; 809 of 860 (94 %) medical students were assessed for knowledge. Six to 12 months after the courses, the median score was significantly higher for the innovative group than that for the traditional lecture group (p < 0.001). In terms of skills, student in the innovative group scored higher on the performance score than the control group (p < 0.01). The innovative course was 24 times more expensive.
Conclusion: Combination of video and simulation allows better retention of knowledge than a traditional lecture and leads to better compliance to resuscitation guidelines.
What is known: • Compliance by residents to pediatric resuscitation guidelines is low. • We developed an innovative pedagogic course combining an educational video and simulation. |
What is new: • Knowledge retention after the innovative course was better than after a traditional lecture. • Sixty-six students tested on their skills demonstrated better compliance to resuscitation guidelines. |


Similar content being viewed by others
Abbreviations
- AHA:
-
American Heart Association
- BLS:
-
basic life support
- CPA:
-
cardiopulmonary arrest
- CPR:
-
cardiopulmonary resuscitation
References
Berg RA, Hilwig RW, Kern KB, Ewy GA (2000) Bystander “chest compressions and assisted ventilation independently improve outcome from piglet asphyxial pulseless” cardiac arrest. Circulation 101(14):1743–1748
Bhanji F, Gottesman R, de Grave W, Steinert Y, Winer L (2011) Paediatric resuscitation training—do medical students believe it should be a mandatory component of the curriculum? Resuscitation 82(5):584–587
Cheng A, Brown LL, Duff JP, Davidson J, Overly F, Tofil NM et al (2015) Improving cardiopulmonary resuscitation with a CPR feedback device and refresher simulations (CPR CARES Study): a randomized clinical trial. JAMA Pediatr 169(2):137–144
Cheng A, Lang TR, Starr SR, Pusic M, Cook DA (2014) Technology-enhanced simulation and pediatric education: a meta-analysis. Pediatrics 133(5):e1313–23
Donoghue A, Nishisaki A, Sutton R, Hales R, Boulet J (2010) Reliability and validity of a scoring instrument for clinical performance during Pediatric Advanced Life Support simulation scenarios. Resuscitation 81(3):331–336
Duncan HP, Frew E (2009) Short-term health system costs of paediatric in-hospital acute life-threatening events including cardiac arrest. Resuscitation 80(5):529–534
Gaies MG, Morris SA, Hafler JP, Graham DA, Capraro AJ, Zhou J et al (2009) Reforming procedural skills training for pediatric residents: a randomized, interventional trial. Pediatrics 124(2):610–619
Girotra S, Spertus JA, Li Y, Berg RA, Nadkarni VM, Chan PS et al (2013) Survival trends in pediatric in-hospital cardiac arrests: an analysis from Get With the Guidelines-Resuscitation. Circ Cardiovasc Qual Outcomes 6(1):42–49
Gupta P, Tang X, Gall CM, Lauer C, Rice TB, Wetzel RC (2014) Epidemiology and outcomes of in-hospital cardiac arrest in critically ill children across hospitals of varied center volume: a multi-center analysis. Resuscitation 85(11):1473–9
Handley JA, Handley AJ (1998) Four-step CPR—improving skill retention. Resuscitation 36(1):3–8
Hunt EA, Duval-Arnould JM, Nelson-McMillan KL, Bradshaw JH, Diener-West M, Perretta JS et al (2014) Pediatric resident resuscitation skills improve after “rapid cycle deliberate practice” training. Resuscitation 85(7):945–951
Hunt EA, Vera K, Diener-West M, Haggerty JA, Nelson KL, Shaffner DH et al (2009) Delays and errors in cardiopulmonary resuscitation and defibrillation by pediatric residents during simulated cardiopulmonary arrests. Resuscitation 80(7):819–825
Iglesias-Vázquez JA, Rodríguez-Núñez A, Penas-Penas M, Sánchez-Santos L, Cegarra-García M, Barreiro-Díaz MV (2007) Cost-efficiency assessment of Advanced Life Support (ALS) courses based on the comparison of advanced simulators with conventional manikins. BMC Emerg Med 7:18
Ilgen JS, Sherbino J, Cook DA (2013) Technology-enhanced simulation in emergency medicine: a systematic review and meta-analysis. Acad Emerg Med Off J Soc Acad Emerg Med 20(2):117–127
Kirkpatrick DL (1998) Evaluating training programs: the four levels. Berrett-Koehler Publishers, San Francisco
Kitamura T, Iwami T, Kawamura T, Nagao K, Tanaka H, Nadkarni VM et al (2010) Conventional and chest-compression-only cardiopulmonary resuscitation by bystanders for children who have out-of-hospital cardiac arrests: a prospective, nationwide, population-based cohort study. Lancet 375(9723):1347–1354
Lapkin S, Levett-Jones T (2011) A cost-utility analysis of medium vs. high-fidelity human patient simulation manikins in nursing education. J Clin Nurs 20(23–24):3543–3552
Lo BM, Devine AS, Evans DP, Byars DV, Lamm OY, Lee RJ et al (2011) Comparison of traditional versus high-fidelity simulation in the retention of ACLS knowledge. Resuscitation 82(11):1440–1443
Mosley C, Dewhurst C, Molloy S, Shaw BN (2012) What is the impact of structured resuscitation training on healthcare practitioners, their clients and the wider service? A BEME systematic review: BEME Guide No. 20. Med Teach 34(6):e349–385
Mundell WC, Kennedy CC, Szostek JH, Cook DA (2013) Simulation technology for resuscitation training: a systematic review and meta-analysis. Resuscitation 84(9):1174–1183
Nolan JP, Soar J, Zideman DA, Biarent D, Bossaert LL, Deakin C et al (2010) European resuscitation council guidelines for resuscitation 2010 section 1. Executive summary. Resuscitation 81(10):1219–1276
O’Leary FM, Janson P (2010) Can e-learning improve medical students’ knowledge and competence in paediatric cardiopulmonary resuscitation? A prospective before and after study. Emerg Med Australas 22(4):324–329
Ornato JP, Peberdy MA, Reid RD, Feeser VR, Dhindsa HS, NRCPR Investigators (2012) Impact of resuscitation system errors on survival from in-hospital cardiac arrest. Resuscitation 83(1):63–69
Roediger HL, Karpicke JD (2006) The power of testing memory: basic research and implications for educational practice. Perspect Psychol Sci J Assoc Psychol Sci 1(3):181–210
Tallentire VR, Smith SE, Skinner J, Cameron HS (2011) Understanding the behaviour of newly qualified doctors in acute care contexts. Med Educ 45(10):995–1005
Thomson NM, Campbell DE, O’Leary FM (2011) Teaching medical students to resuscitate children: an innovative two-part programme. Emerg Med Australas 23(6):741–747
Vadeboncoeur T, Stolz U, Panchal A, Silver A, Venuti M, Tobin J et al (2014) Chest compression depth and survival in out-of-hospital cardiac arrest. Resuscitation 85(2):182–188
Wayne DB, Didwania A, Feinglass J, Fudala MJ, Barsuk JH, McGaghie WC (2008) Simulation-based education improves quality of care during cardiac arrest team responses at an academic teaching hospital: a case-control study. Chest 133(1):56–61
Widdowson M-A, Meltzer MI, Zhang X, Bresee JS, Parashar UD, Glass RI (2007) Cost-effectiveness and potential impact of rotavirus vaccination in the United States. Pediatrics 119(4):684–697
Zendejas B, Wang AT, Brydges R, Hamstra SJ, Cook DA (2013) Cost: the missing outcome in simulation-based medical education research: a systematic review. Surgery 153(2):160–176
Acknowledgments
The authors would like to thank Marie-Christine Renaud and Alexandre Leccas for their help in implementing the innovative course, all the teachers involved in this education program, and the students who participated in the study.
Author’s contribution
DD and AP designed the study and were responsible for data gathering and analysis and drafting the report. CA, GT, RG, and NdS helped in data gathering and analysis and revised the manuscript critically. EG and AD revised the manuscript critically. All authors have read and approved the final report.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This study received no funding.
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
This study was part of our faculty’s educational activity. Primary data analysis was at the group level and deemed to be exempt from ethical review by the Pierre and Marie Curie medical faculty institutional review board.
Informed consent
Informed oral consent was obtained from all individual participants included in the study.
Additional information
Communicated by Patrick Van Reempts
Rights and permissions
About this article
Cite this article
Drummond, D., Arnaud, C., Thouvenin, G. et al. An innovative pedagogic course combining video and simulation to teach medical students about pediatric cardiopulmonary arrest: a prospective controlled study. Eur J Pediatr 175, 767–774 (2016). https://doi.org/10.1007/s00431-016-2702-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-016-2702-1