Abstract
Background
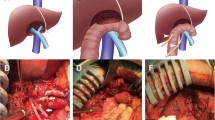
Hepaticojejunostomy (HJ) is the gold standard procedure for the reconstruction of the bile duct in many benign and malignant situations. One of the major situation is the bile duct injury (BDI) after cholecystectomy, either for early or late repair. This procedure presents some specificities associated to a debated management of BDI.
Purpose
This article provides a state-of-the-art of the hepaticojejunostomy procedure focusing on bile duct injury including its indications and outcomes
Conclusion
Performed at the right moment and respecting the technical rules, HJ provides a restoration of the biliary patency in the long term of 80 to 90%. It is the main surgical technique to repair BDI. Complications and failure of this procedure can be difficult to manage. That is why the primary repair requires an appropriate multidisciplinary approach associated with an expert high quality surgical technique.
Similar content being viewed by others
Abbreviations
- BDI:
-
Bile duct injury
- OC:
-
Open cholecystectomy
- LC:
-
Laparoscopic cholecystectomy
- HPB:
-
Hepato-pancreato-biliary
References
Braasch JW (1994) Historical perspectives of biliary tract injuries. Surg Clin N Am 74:731–740. https://doi.org/10.1016/s0039-6109(16)46403-0
HEPP J, COUINAUD C (1956) [Approach to and use of the left hepatic duct in reparation of the common bile duct]. La Press Médicale 64:947–948
Bismuth H, Franco D, Corlette MB, Hepp J (1978) Long term results of Roux-en-Y hepaticojejunostomy. Surg Gynecol Obstetrics 146:161–167
Barbier L, Souche R, Slim K, Ah-Soune P (2014) Long-term consequences of bile duct injury after cholecystectomy. J Visc Surg 151:269–279. https://doi.org/10.1016/j.jviscsurg.2014.05.006
Jabłońska B, Lampe P (2009) Iatrogenic bile duct injuries: etiology, diagnosis and management. World J Gastroentero 15:4097–4104. https://doi.org/10.3748/wjg.15.4097
Hepp J (1985) Hepaticojejunostomy using the left biliary trunk for iatrogenic biliary lesions: the French connection. World J Surg 9:507–511. https://doi.org/10.1007/bf01655291
De’angelis N, Catena F, Memeo R et al (2021) 2020 WSES guidelines for the detection and management of bile duct injury during cholecystectomy. World J Emerg Surg 16:30. https://doi.org/10.1186/s13017-021-00369-w
Bray F, Balcaen T, Baro E et al (2019) Increased incidence of cholecystectomy related to gallbladder disease in France: analysis of 807,307 cholecystectomy procedures over a period of seven years. J Visc Surg 156:209–215. https://doi.org/10.1016/j.jviscsurg.2018.12.003
Mangieri CW, Hendren BP, Strode MA et al (2019) Bile duct injuries (BDI) in the advanced laparoscopic cholecystectomy era. Surg Endosc 33:724–730. https://doi.org/10.1007/s00464-018-6333-7
Barrett M, Asbun HJ, Chien H-L et al (2018) Bile duct injury and morbidity following cholecystectomy: a need for improvement. Surg Endosc 32:1683–1688. https://doi.org/10.1007/s00464-017-5847-8
De RP, Rauws EA, Bruno MJ et al (2007) Survival in bile duct injury patients after laparoscopic cholecystectomy: a multidisciplinary approach of gastroenterologists, radiologists, and surgeons. Surgery 142:1–9. https://doi.org/10.1016/j.surg.2007.03.004
Nuzzo G, Giuliante F, Giovannini I et al (2008) Advantages of multidisciplinary management of bile duct injuries occurring during cholecystectomy. Am J Surg 195:763–769. https://doi.org/10.1016/j.amjsurg.2007.05.046
Haidar H, Manasa E, Yassin K et al (2021) Endoscopic treatment of post-cholecystectomy bile leaks: a tertiary center experience. Surg Endosc 35:1088–1092. https://doi.org/10.1007/s00464-020-07472-0
Booij KAC, De RP, Van DS et al (2018) Long-term impact of bile duct injury on morbidity, mortality, quality of life, and work related limitations. Ann Surg 268:143–150. https://doi.org/10.1097/sla.0000000000002258
Strasberg SM, Hertl M, Soper NJ (1995) An analysis of the problem of biliary injury during laparoscopic cholecystectomy. J Am Coll Surgeons 180:101–125
Mercado MA, Domínguez I (2011) Classification and management of bile duct injuries. World J Gastrointest Surg 3:43. https://doi.org/10.4240/wjgs.v3.i4.43
Aduna M, Larena JA, Martín D et al (2005) Bile duct leaks after laparoscopic cholecystectomy: value of contrast-enhanced MRCP. Abdom Imaging 30:480–487. https://doi.org/10.1007/s00261-004-0276-2
Sarno G, Al-Sarira AA, Ghaneh P et al (2012) Cholecystectomy-related bile duct and vasculobiliary injuries. Brit J Surg 99:1129–1136. https://doi.org/10.1002/bjs.8806
Alves A, Farges O, Nicolet J et al (2003) Incidence and consequence of an hepatic artery injury in patients with postcholecystectomy bile duct strictures. Ann Surg 238:93–96. https://doi.org/10.1097/01.sla.0000074983.39297.c5
Strasberg SM, Helton WS (2011) An analytical review of vasculobiliary injury in laparoscopic and open cholecystectomy. Hpb 13:1–14. https://doi.org/10.1111/j.1477-2574.2010.00225.x
Schreuder AM, Vas BCN, Booij KAC et al (2020) Optimal timing for surgical reconstruction of bile duct injury: meta-analysis. Bjs Open 4:776–786. https://doi.org/10.1002/bjs5.50321
Goykhman Y, Kory I, Small R et al (2008) Long-term outcome and risk factors of failure after bile duct injury repair. J Gastrointest Surg 12:1412–1417. https://doi.org/10.1007/s11605-008-0538-3
Krige JE, Bornman PC, Kahn D (2010) Bile leaks and sepsis: drain now, fix later: comment on “bile duct injuries associated with laparoscopic cholecystectomy”. Arch Surg-chicago 145:763–763. https://doi.org/10.1001/archsurg.2010.154
Wang X, Yu W-L, Fu X-H et al (2020) Early versus delayed surgical repair and referral for patients with bile duct injury: a systematic review and meta-analysis. Ann Surg 271:449–459. https://doi.org/10.1097/sla.0000000000003448
Sulpice L, Garnier S, Rayar M et al (2014) Biliary cirrhosis and sepsis are two risk factors of failure after surgical repair of major bile duct injury post-laparoscopic cholecystectomy. Langenbeck’s Archives Surg 399:601–608. https://doi.org/10.1007/s00423-014-1205-7
Schreuder A, Booij K, De RP et al (2018) Percutaneous-endoscopic rendezvous procedure for the management of bile duct injuries after cholecystectomy: short- and long-term outcomes. Endoscopy 50:577–587. https://doi.org/10.1055/s-0043-123935
Mercado MÁ, Chan C, Orozco H et al (2006) Long-term evaluation of biliary reconstruction after partial resection of segments IV and V in iatrogenic injuries. J Gastrointest Surg 10:77–82. https://doi.org/10.1016/j.gassur.2005.07.003
Dandekar U, Dandekar K, Chavan S (2015) Right hepatic artery: a cadaver investigation and its clinical significance. Anat Res Int 2015:412595. https://doi.org/10.1155/2015/412595
Truant S, Boleslawski E, Lebuffe G et al (2010) Hepatic resection for post-cholecystectomy bile duct injuries: a literature review. Hpb 12:334–341. https://doi.org/10.1111/j.1477-2574.2010.00172.x
Schreuder AM, Busch OR, Besselink MG et al (2020) Long-term impact of iatrogenic bile duct injury. Digest Surg 37:10–21. https://doi.org/10.1159/000496432
Chiche L, Guieu M, Bachellier P et al (2022) Liver transplantation for iatrogenic bile duct injury during cholecystectomy: a French retrospective multicenter study. Hpb 24:94–100. https://doi.org/10.1016/j.hpb.2021.08.817
Perera MTPR, Silva MA, Shah AJ et al (2010) Risk factors for litigation following major transectional bile duct injury sustained at laparoscopic cholecystectomy. World J Surg 34:2635–2641. https://doi.org/10.1007/s00268-010-0725-8
Bansal VK, Krishna A, Misra MC et al (2015) Factors affecting short-term and long-term outcomes after bilioenteric reconstruction for post-cholecystectomy bile duct injury: experience at a tertiary care centre. Indian J Surg 77:472–479. https://doi.org/10.1007/s12262-013-0880-x
Walsh RM, Henderson JM, Vogt DP, Brown N (2007) Long-term outcome of biliary reconstruction for bile duct injuries from laparoscopic cholecystectomies. Surgery 142:450–457. https://doi.org/10.1016/j.surg.2007.07.008
Halle-Smith JM, Hall LA, Mirza DF, Roberts KJ (2021) Risk factors for anastomotic stricture after hepaticojejunostomy for bile duct injury–a systematic review and meta-analysis. Surgery. https://doi.org/10.1016/j.surg.2021.05.015
Huang Q, Yao HH, Shao F et al (2014) Analysis of risk factors for postoperative complication of repair of bile duct injury after laparoscopic cholecystectomy. Digest Dis Sci 59:3085–3091. https://doi.org/10.1007/s10620-014-3255-7
Benkabbou A, Castaing D, Salloum C et al (2013) Treatment of failed Roux-en-Y hepaticojejunostomy after post-cholecystectomy bile ducts injuries. Surgery 153:95–102. https://doi.org/10.1016/j.surg.2012.06.028
Saad N, Darcy M (2008) Iatrogenic bile duct injury during laparoscopic cholecystectomy. Techniques Vasc Interventional Radiology 11:102–110. https://doi.org/10.1053/j.tvir.2008.07.004
Fidelman N (2015) Benign biliary strictures: diagnostic evaluation and approaches to percutaneous treatment. Techniques Vasc Interventional Radiology 18:210–217. https://doi.org/10.1053/j.tvir.2015.07.004
Janssen JJ, Van DO, Van LK et al (2014) Percutaneous balloon dilatation and long-term drainage as treatment of anastomotic and nonanastomotic benign biliary strictures. Cardiovasc Inter Rad 37:1559–1567. https://doi.org/10.1007/s00270-014-0836-y
Thompson CM, Saad NE, Quazi RR et al (2013) Management of iatrogenic bile duct injuries: role of the interventional radiologist. Radiographics 33:117–134. https://doi.org/10.1148/rg.331125044
Chaudhary A, Chandra A, Negi SS, Sachdev A (2002) Reoperative surgery for postcholecystectomy bile duct injuries. Digest Surg 19:22–27. https://doi.org/10.1159/000052001
Sikora SS, Pottakkat B, Srikanth G et al (2007) Postcholecystectomy benign biliary strictures – long-term results. Digest Surg 23:304–312. https://doi.org/10.1159/000097894
Booij KAC, Coelen RJ, De RP et al (2018) Long-term follow-up and risk factors for strictures after hepaticojejunostomy for bile duct injury: an analysis of surgical and percutaneous treatment in a tertiary center. Surgery 163:1121–1127. https://doi.org/10.1016/j.surg.2018.01.003
De RP, Busch ORC, Rauws EA et al (2007) Long-term results of a primary end-to-end anastomosis in peroperative detected bile duct injury. J Gastrointest Surg 11:296–302. https://doi.org/10.1007/s11605-007-0087-1
Jabłońska B, Lampe P, Olakowski M et al (2009) Hepaticojejunostomy vs. end-to-end biliary reconstructions in the treatment of iatrogenic bile duct injuries. J Gastrointest Surg 13:1084–1093. https://doi.org/10.1007/s11605-009-0841-7
Dhote A, Lupinacci RM, Peschaud F (2021) Side-to-side choledochoduodenostomy for common bile duct stones. J Visc Surg 159:59–64. https://doi.org/10.1016/j.jviscsurg.2021.04.007
Schmitz V, Neumann UP, Puhl G et al (2006) Surgical complications and long-term outcome of different biliary reconstructions in liver transplantation for primary sclerosing cholangitis—choledochoduodenostomy versus choledochojejunostomy. Am J Transplant 6:379–385. https://doi.org/10.1111/j.1600-6143.2005.01173.x
Schreuder AM, Franken LC, Van DS et al (2020) Choledochoduodenostomy versus hepaticojejunostomy – a matched case–control analysis. Hpb. 23:560–565. https://doi.org/10.1016/j.hpb.2020.08.014
Tocchi A, Mazzoni G, Liotta G et al (2001) Late development of bile duct cancer in patients who had biliary-enteric drainage for benign disease: a follow-up study of more than 1,000 patients. Ann Surg 234:210–214. https://doi.org/10.1097/00000658-200108000-00011
Cuendis-Velázquez A, Bada-Yllán O, Trejo-Ávila M et al (2018) Robotic-assisted Roux-en-Y hepaticojejunostomy after bile duct injury. Langenbeck’s Archives Surg 403:53–59. https://doi.org/10.1007/s00423-018-1651-8
Rueda-De-Leon A, Domínguez-Rosado I, Mercado MA (2021) Comment on “early versus delayed surgical repair and referral for patients with bile duct injury: a systematic review and meta-analysis”. Ann Surg 274:e756. https://doi.org/10.1097/sla.0000000000003954
De RP, Rauws EA, Vermeulen M et al (2007) Endoscopic treatment of post-surgical bile duct injuries: long term outcome and predictors of success. Gut 56:1599. https://doi.org/10.1136/gut.2007.123596
Dumonceau J-M, Tringali A, Papanikolaou I et al (2018) Endoscopic biliary stenting: indications, choice of stents, and results: European Society of Gastrointestinal Endoscopy (ESGE) Clinical Guideline ? Updated October 2017. Endoscopy 50:910–930. https://doi.org/10.1055/a-0659-9864
Desai A, Twohig P, Trujillo S et al (2021) Clinical efficacy, timing, and outcomes of ERCP for management of bile duct leaks: a nationwide cohort study. Endosc Int Open 09:E247–E252. https://doi.org/10.1055/a-1322-2425
Parlak E, Dişibeyaz S, Ödemiş B et al (2015) Endoscopic treatment of patients with bile duct stricture after cholecystectomy: factors predicting recurrence in the long term. Digest Dis Sci 60:1778–1786. https://doi.org/10.1007/s10620-014-3515-6
Canena J, Horta D, Coimbra J et al (2015) Outcomes of endoscopic management of primary and refractory postcholecystectomy biliary leaks in a multicentre review of 178 patients. Bmc Gastroenterol 15:105. https://doi.org/10.1186/s12876-015-0334-y
Holte K, Bardram L, Wettergren A, Rasmussen A (2010) Reconstruction of major bile duct injuries after laparoscopic cholecystectomy. Dan Med Bull 57:A4135
Pottakkat B, Vijayahari R, Prakash A et al (2010) Factors predicting failure following high bilio-enteric anastomosis for post-cholecystectomy benign biliary strictures. J Gastrointest Surg 14:1389–1394. https://doi.org/10.1007/s11605-010-1241-8
Perera MTPR, Silva MA, Hegab B et al (2011) Specialist early and immediate repair of post-laparoscopic cholecystectomy bile duct injuries is associated with an improved long-term outcome. Ann Surg 253:553–560. https://doi.org/10.1097/sla.0b013e318208fad3
Lubikowski J, Post M, Białek A et al (2011) Surgical management and outcome of bile duct injuries following cholecystectomy: a single-center experience. Langenbeck’s Archives Surg 396:699–707. https://doi.org/10.1007/s00423-011-0745-3
Iannelli A, Paineau J, Hamy A et al (2013) Primary versus delayed repair for bile duct injuries sustained during cholecystectomy: results of a survey of the Association Francaise de Chirurgie. Hpb 15:611–616. https://doi.org/10.1111/hpb.12024
Hajjar NA, Tomuş C, Mocan L et al (1990) (2014) Management of bile duct injuries following laparoscopic cholecystectomy: long-term outcome and risk factors influencing biliary reconstruction. Chir Buchar Romania 109:493–499
Felekouras E, Petrou A, Neofytou K et al (2015) Early or delayed intervention for bile duct injuries following laparoscopic cholecystectomy? A dilemma looking for an answer. Gastroent Res Pract 2015:1–10. https://doi.org/10.1155/2015/104235
Cho JY, Jaeger AR, Sanford DE et al (2015) Proposal for standardized tabular reporting of observational surgical studies illustrated in a study on primary repair of bile duct injuries. J Am Coll Surgeons 221:678–688. https://doi.org/10.1016/j.jamcollsurg.2015.06.004
Gomes RM, Doctor NH (2015) Predictors of outcome after reconstructive hepaticojejunostomy for post cholecystectomy bile duct injuries. Tropical Gastroenterology 36:229–235. https://doi.org/10.7869/tg.296
Rystedt J, Lindell G, Montgomery A (2016) Bile duct injuries associated with 55,134 cholecystectomies: treatment and outcome from a national perspective. World J Surg 40:73–80. https://doi.org/10.1007/s00268-015-3281-4
Stilling NM, Fristrup C, Wettergren A et al (2015) Long-term outcome after early repair of iatrogenic bile duct injury. A national Danish multicentre study. Hpb 17:394–400. https://doi.org/10.1111/hpb.12374
Dominguez-Rosado I, Sanford DE, Liu J et al (2016) Timing of surgical repair after bile duct injury impacts postoperative complications but not anastomotic patency. Ann Surg 264:544–553. https://doi.org/10.1097/sla.0000000000001868
Khadra H, Johnson H, Crowther J et al (2019) Bile duct injury repairs: progressive outcomes in a tertiary referral center. Surgery 166:698–702. https://doi.org/10.1016/j.surg.2019.06.032
Ray S, Sanyal S, Das S et al (2020) Outcomes of surgery for post-cholecystectomy bile duct injuries: an audit from a tertiary referral center. J Visc Surg 157:3–11. https://doi.org/10.1016/j.jviscsurg.2019.08.005
Lindemann J, Krige JEJ, Kotze U, Jonas E (2020) Factors leading to loss of patency after biliary reconstruction of major laparoscopic cholecystectomy bile duct injuries: an observational study with long-term outcomes. Hpb 22:1613–1621. https://doi.org/10.1016/j.hpb.2020.02.010
Anand U, Kumar R, Priyadarshi RN et al (2021) Analysis of outcomes of biliary reconstruction after post-cholecystectomy bile duct injuries. Anz J Surg 91:1542–1548. https://doi.org/10.1111/ans.17047
Diaz-Martinez J, Chapa-Azuela O, Roldan-Garcia JA, Flores-Rangel GA (2020) Bile duct injuries after cholecystectomy, analysis of constant risk. Ann Hepato-biliary-pancreatic Surg 24:150–155. https://doi.org/10.14701/ahbps.2020.24.2.150
Jajja MR, Laboe A, Hashmi S et al (2021) Standardizing diagnostic and surgical approach to management of bile duct injuries after cholecystectomy: long-term outcomes of patients treated at a high-volume HPB center. J Gastrointest Surg 25:2796–2805. https://doi.org/10.1007/s11605-021-04916-3
Giulianotti PC, Quadri P, Durgam S, Bianco FM (2018) Reconstruction/Repair of Iatrogenic Biliary Injuries. Ann Surg 267:e7–e9. https://doi.org/10.1097/sla.0000000000002343
Marino MV, Mirabella A, Guarrasi D et al (2019) Robotic-assisted repair of iatrogenic common bile duct injury after laparoscopic cholecystectomy: surgical technique and outcomes. Int J Medical Robotics Comput Assisted Surg 15:e1992. https://doi.org/10.1002/rcs.1992
Cuendis-Velázquez A, Trejo-Ávila M, Bada-Yllán O et al (2019) A new era of bile duct repair: robotic-assisted versus laparoscopic hepaticojejunostomy. J Gastrointest Surg 23:451–459. https://doi.org/10.1007/s11605-018-4018-0
Javed A, Shashikiran BD, Aravinda PS, Agarwal AK (2021) Laparoscopic versus open surgery for the management of post-cholecystectomy benign biliary strictures. Surg Endosc 35:1254–1263. https://doi.org/10.1007/s00464-020-07496-6
Gómez D, Cabrera LF, Pedraza-Ciro M et al (2020) Reconstrucción laparoscópica con hepatoyeyunostomía en Y de Roux después de una lesión del conducto biliar iatrogénico: serie de casos. Cirugía Y Cirujanos 88:608–616. https://doi.org/10.24875/ciru.20001541
Acknowledgements
The authors would like to thank Ms. E. Faherty, English native speaker, for the English checking of this manuscript.
Author information
Authors and Affiliations
Contributions
Study conception and design: AM, LC. Acquisition of data: AM, LC. Analysis and interpretation of data: AM, LC. Drafting of manuscript: AM, LC, JPA, CL. Critical revision of manuscript: AM, LC, JPA, CL
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Marichez, A., Adam, JP., Laurent, C. et al. Hepaticojejunostomy for bile duct injury: state of the art. Langenbecks Arch Surg 408, 107 (2023). https://doi.org/10.1007/s00423-023-02818-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00423-023-02818-3