Abstract
Background
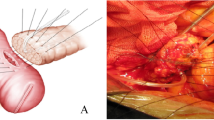
While the best technique for pancreatic anastomosis during Whipple’s procedure remains controversial, laparoscopic pancreaticoduodenectomy (LPD) has been rapidly increasing in popularity. Because of their feasibility and reliability, new pancreatic anastomosis techniques may have vital roles when adapted for LPD. Here, we describe a new pancreaticojejunostomy (PJ) technique using three sutures (termed the “three sutures” PJ technique), which facilitates pancreatic anastomosis during total LPD.
Methods
A total of 149 patients who underwent LPD using the “three sutures” PJ technique at three hospitals were included in this study (81 patients at Guangdong Provincial People’s Hospital [GDPH], 60 patients at Sun Yat-Sen Memorial Hospital [SMH], and 8 patients at Affiliated Hospital of Guangdong Medical University [AHGMU]). Data on the demographic characteristics, operative outcomes, and postoperative results (pancreatic fistula rate, mortality rate, and length of hospital stay) of these patients were collected and analyzed.
Results
A surgical video showing the details of the “three sutures” PJ method was included. The mean operation times at GDPH, SMH, and AHGMU were 4.08 ± 0.99 h, 4.65 ± 1.53 h, and 4.67 ± 0.64 h, respectively, and the average PJ times were 17.96 ± 3.49 min, 18.19 ± 2.63 min, and 22.5 ± 3.96 min, respectively. The numbers of grade B pancreatic fistulas were 9 (11.11%), 2 (3.33%), and 1 (12.50%), respectively, and two patients had grade C fistulas, one each at GDPH and SMH. The numbers of clinically relevant postoperative pancreatic fistula (CR-POPF) were 10 (12.35%), 3 (5.00%), and 1 (12.50%) in each center, respectively. The overall rate of CR-POPF was 9.40% (14/149) among patients of all three centers. The perioperative mortality rate was 0%.
Conclusions
The “three sutures” PJ technique for total LPD is a safe and reliable method, with a low risk of pancreatic fistula, short anastomosis time, and steep learning curve.

Similar content being viewed by others
References
Chen K, Zhou Y, Jin W et al (2020) Laparoscopic pancreaticoduodenectomy versus open pancreaticoduodenectomy for pancreatic ductal adenocarcinoma: oncologic outcomes and long-term survival. Surg Endosc 34(5):1948–1958
Wang M, Peng B, Liu J et al (2021) Practice patterns and perioperative outcomes of laparoscopic pancreaticoduodenectomy in China: a retrospective multicenter analysis of 1029 patients. Ann Surg 273(1):145–153
de Rooij T, Klompmaker S, Abu Hilal M, Kendrick ML, Busch OR, Besselink MG (2016) Laparoscopic pancreatic surgery for benign and malignant disease. Nat Rev Gastroenterol Hepatol 13(4):227–238
Shrikhande SV, Sivasanker M, Vollmer CM et al (2017) Pancreatic anastomosis after pancreatoduodenectomy: a position statement by the International Study Group of Pancreatic Surgery (ISGPS). Surgery 161(5):1221–1234
Ecker BL, McMillan MT, Asbun HJ et al (2018) Characterization and optimal management of high-risk pancreatic anastomoses during pancreatoduodenectomy. Ann Surg 267(4):608–616
Xiang Y, Wu J, Lin C et al (2019) Pancreatic reconstruction techniques after pancreaticoduodenectomy: a review of the literature. Expert Rev Gastroenterol Hepatol 13(8):797–806
Wang W, Zhang Z, Gu C et al (2018) The optimal choice for pancreatic anastomosis after pancreaticoduodenectomy: a network meta-analysis of randomized control trials. Int J Surg 57:111–116
Ratnayake CBB, Wells CI, Kamarajah SK et al (2020) Critical appraisal of the techniques of pancreatic anastomosis following pancreaticoduodenectomy: a network meta-analysis. Int J Surg 73:72–77
Kendrick ML, Cusati D (2010) Total laparoscopic pancreaticoduodenectomy: feasibility and outcome in an early experience. Arch Surg 145(1):19–23
Cai Y, Luo H, Li Y, Gao P, Peng B (2019) A novel technique of pancreaticojejunostomy for laparoscopic pancreaticoduodenectomy. Surg Endosc 33(5):1572–1577
Poves I, Morató O, Burdío F, Grande L (2017) Laparoscopic-adapted Blumgart pancreaticojejunostomy in laparoscopic pancreaticoduodenectomy. Surg Endosc 31(7):2837–2845
Wang M, Xu S, Zhang H, Peng S, Zhu F, Qin R (2017) Imbedding pancreaticojejunostomy used in pure laparoscopic pancreaticoduodenectomy for nondilated pancreatic duct. Surg Endosc 31(4):1986–1992
Bassi C, Marchegiani G, Dervenis C et al (2017) The 2016 update of the International Study Group (ISGPS) definition and grading of postoperative pancreatic fistula: 11 years after. Surgery 161(3):584–591
Gagner M, Palermo M (2009) Laparoscopic Whipple procedure: review of the literature. J Hepatobiliary Pancreat Surg 16(6):726–730
Wu J, Zhang G, Yao X et al (2020) Achilles’ heel of laparoscopic pancreatectomy: reconstruction of the remnant pancreas. Expert Rev Gastroenterol Hepatol 14(7):527–537
Chen JS, Liu G, Li TR et al (2019) Pancreatic fistula after pancreaticoduodenectomy: risk factors and preventive strategies. J Cancer Res Ther 15(4):857–863
Yildirim OY, Özer N (2020) Effect of anastomosis technique on pancreatic fistula formation in proximal pancreaticoduodenectomy. J Coll Physicians Surg Pak 30(5):480–484
Xu J, Ji SR, Zhang B, Ni QX, Yu XJ (2018) Strategies for pancreatic anastomosis after pancreaticoduodenectomy: what really matters? Hepatobiliary Pancreat Dis Int 17(1):22–26
Tanaka K, Yamada S, Sonohara F et al (2021) Pancreatic fat and body composition measurements by computed tomography are associated with pancreatic fistula after pancreatectomy. Ann Surg Oncol 28(1):530–538
Xingjun G, Feng Z, Meiwen Y et al (2019) A score model based on pancreatic steatosis and fibrosis and pancreatic duct diameter to predict postoperative pancreatic fistula after pancreatoduodenectomy. BMC Surg 19(1):75
Ke ZX, Xiong JX, Hu J, Chen HY, Li Q, Li YQ (2019) Risk factors and management of postoperative pancreatic fistula following pancreaticoduodenectomy: single-center experience. Curr Med Sci 39(6):1009–1018
Fiorentini G, Tamburrino D, Belfiori G, Crippa S, Partelli S, Falconi M (2019) Which is the best pancreatic anastomosis? Minerva Chir 74(3):241–252
Peng SY, Wang JW, Li JT, Mou YP, Liu YB, Cai XJ (2004) Binding pancreaticojejunostomy–a safe and reliable anastomosis procedure. HPB (Oxford) 6(3):154–160
di Mola FF, Grottola T, Panaccio P et al (2020) End-to-side duct-to-mucosa pancreaticojejunostomy after pancreaticoduodenectomy a comparison trial of small versus larger jejunal incision. A single center experience. Ann Ital Chir. 91:469–477
Ohwada S, Iwazaki S, Nakamura S et al (1997) Pancreaticojejunostomy-securing technique: duct-to-mucosa anastomosis by continuous running suture and parachuting using monofilament absorbable thread. J Am Coll Surg 185(2):190–194
Murakami Y, Uemura K, Hayashidani Y et al (2008) No mortality after 150 consecutive pancreatoduodenctomies with duct-to-mucosa pancreaticogastrostomy. J Surg Oncol 97(3):205–209
El Nakeeb A, El Hemaly M, Askr W et al (2015) Comparative study between duct to mucosa and invagination pancreaticojejunostomy after pancreaticoduodenectomy: a prospective randomized study. Int J Surg 16(Pt A):1–6
Olakowski M, Grudzińska E, Mrowiec S (2020) Pancreaticojejunostomy-a review of modern techniques. Langenbecks Arch Surg 405(1):13–22
Oda T, Hashimoto S, Shimomura O et al (2015) Inter-anastomosis drainage tube between the pancreas and jejunum: a novel technique for preventing pancreatic fistula after pancreaticoduodenectomy. J Am Coll Surg 221(3):e55-60
Wen XD, Liu DQ, Zhang BY, Xiao L, Yan HT, Liu WH (2020) The bridge stenting-based internal drainage in pancreatic trauma patients with main pancreatic duct injury. Updates Surg 72(3):717–726
Funding
This study was funded by grants from the National Natural Science Foundation of China (grant number: 82072639).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Compliance with ethical standards
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhou, Y., Yang, J., Wei, L. et al. A novel anastomosis technique facilitates pancreaticojejunostomy in total laparoscopic pancreaticoduodenectomy (with video). Langenbecks Arch Surg 406, 2891–2897 (2021). https://doi.org/10.1007/s00423-021-02347-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-021-02347-x