Abstract
Purpose
In the Danish national guidelines from 2006 on the treatment of acute cholecystitis, early laparoscopic operation within 5 days after the debut of symptoms was recommended. The aim of this study was to analyze the outcome in patients with acute cholecystitis subjected to cholecystectomy in Denmark in the five-year period hereafter.
Methods
All patients undergoing cholecystectomy in the period 2006–2010 were registered in the Danish Cholecystectomy Database, from which outcome data were collected. The effect of potential risk factors such as age, gender, BMI, American Society of Anesthesiologists (ASA) score, previous pancreatitis, previous abdominal surgery, year of operation, surgical approach, and surgeon experience was analyzed.
Results
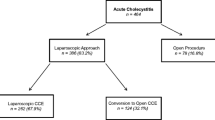
Of 33,853 patients registered with a cholecystectomy, 4667 (14%) were operated for acute cholecystitis. In 95% of the patients, laparoscopic cholecystectomy was intended and in 5% primary open access was chosen. The frequency of conversion from laparoscopic to open surgery was 18%. High age and ASA score, operation in the early years of the period, and open or converted procedure all increased the risk of hospital stay to > 3 days or readmission. High age and ASA score, converted or open operation, and previous pancreatitis increased the risk of additional procedures. Postoperative mortality was 1.2%, and significant risk factors for postoperative death were age, low BMI, high ASA score, early year of operation, and open procedures.
Conclusions
Acute cholecystectomy was safely managed laparoscopically in most patients after the introduction of national guidelines, with an increasing rate of laparoscopically completed procedures during the study period.


Similar content being viewed by others
References
Gurusamy KS, Davidson C, Gluud C, Davidson BR (2013) Early versus delayed laparoscopic cholecystectomy for people with acute cholecystitis. Cochrane Database Syst Rev 6:CD005440. https://doi.org/10.1002/14651858.CD005440.pub3
Aerts R, Penninckx F (2003) The burden of gallstone disease in Europe. Aliment Pharmacol Ther 18:49–53. https://doi.org/10.1046/j.0953-0673.2003.01721.x
Jørgensen T (1987) Prevalence of gallstones in a Danish population. Am J Epidemiol 126:912–921
Halldestam I, Enell E-L, Kullman E, Borch K (2004) Development of symptoms and complications in individuals with asymptomatic gallstones. Br J Surg 91:734–738. https://doi.org/10.1002/bjs.4547
Abou-Saif A, Al-Kawas FH (2002) Complications of gallstone disease: Mirizzi syndrome, cholecystocholedochal fistula, and gallstone ileus. Am J Gastroenterol 97:249–254
Harboe KM, Bardram L (2011) Nationwide quality improvement of cholecystectomy: results from a national database. Int J Qual Health Care 23:565–573. https://doi.org/10.1093/intqhc/mzr041
Connor S, Garden OJ (2006) Bile duct injury in the era of laparoscopic cholecystectomy. Br J Surg 93:158–168
Gomes CA, Junior CS, Di Saveiro S, Sartelli M, Kelly MD, Gomes CC, Gomes FC, Correa LD, Alves CB, Guimarães S de F (2017) Acute calculous cholecystitis: review of current best practices. World J Gastrointest Surg 9:118. https://doi.org/10.4240/wjgs.v9.i5.118
Ansaloni L, Pisano M, Coccolini F, Peitzmann AB, Fingerhut A, Catena F, Agresta F, Allegri A, Bailey I, Balogh ZJ, Bendinelli C, Biffl W, Bonavina L, Borzellino G, Brunetti F, Burlew CC, Camapanelli G, Campanile FC, Ceresoli M, Chiara O, Civil I, Coimbra R, De Moya M, Di Saverio S, Fraga GP, Gupta S, Kashuk J, Kelly MD, Khokha V, Jeekel H, Latifi R, Leppaniemi A, Maier RV, Marzi I, Moore F, Piazzalunga D, Sakakushev B, Sartelli M, Scalea T, Stahel PF, Taviloglu K, Tugnoli G, Uraneus S, Velmahos GC, Wani I, Weber DG, Viale P, Sugrue M, Ivatury R, Kluger Y, Gurusamy KS, Moore EE (2016) 2016 WSES guidelines on acute calculous cholecystitis. World J Emerg Surg 11:25. https://doi.org/10.1186/s13017-016-0082-5
The Danish National Board of Health (2006) Guidelines for the treatment of patients with gallstone disease. [Online]. Available from: https://www.sst.dk/-/media/Udgivelser/2006/Publ2006/PLAN/SfR/Galdesten/Galdestenssygdomme,-d-,pdf.ashx. Accessed 5 July 2019.
Bardram L, Rosenberg J, Kristiansen VB (2005) The Danish Cholecystectomy Database--DCD. Ugeskr Laeger 167:2618–2620
Harboe KM, Anthonsen K, Bardram L (2009) Validation of data and indicators in the Danish Cholecystectomy Database. Int J Qual Health Care 21:160–168. https://doi.org/10.1093/intqhc/mzp009
Brodsky A, Matter I, Sabo E, Cohen A, Abrahamson J, Eldar S (2000) Laparoscopic cholecystectomy for acute cholecystitis: can the need for conversion and the probability of complications be predicted? A prospective study. Surg Endosc 14:755–760
Terho PM, Leppäniemi AK, Mentula PJ (2016) Laparoscopic cholecystectomy for acute calculous cholecystitis: a retrospective study assessing risk factors for conversion and complications. World J Emerg Surg 11:54. https://doi.org/10.1186/s13017-016-0111-4
Halpin V, Gupta A (2011) Acute cholecystitis. BMJ Clin Evid. 0411.
Loozen CS, Van Ramshorst B, Van Santvoort HC, Boerma D (2017) Early cholecystectomy for acute cholecystitis in the elderly population: a systematic review and meta-analysis. Dig Surg 34:371–379
Paul Wright G, Stilwell K, Johnson J, Hefty MT, Chung MH (2015) Predicting length of stay and conversion to open cholecystectomy for acute cholecystitis using the 2013 Tokyo Guidelines in a US population. J Hepatobiliary Pancreat Sci 22:795–801. https://doi.org/10.1002/jhbp.284
Coccolini F, Catena F, Pisano M, Gheza F, Fagiuoli S, Di Saverio S, Leandro G, Montori G, Ceresoli M, Corbella D, Sartelli M, Sugrue M, Ansaloni L (2015) Open versus laparoscopic cholecystectomy in acute cholecystitis. Systematic review and meta-analysis. Int J Surg 18:196–204. https://doi.org/10.1016/j.ijsu.2015.04.083
González-Muñoz JI, Franch-Arcas G, Angoso-Clavijo M, Sánchez-Hernández M, García-Plaza A, Caraballo-Angeli M, Muñoz-Bellvís L (2017) Risk-adjusted treatment selection and outcome of patients with acute cholecystitis. Langenbeck’s Arch Surg 402:607–614. https://doi.org/10.1007/s00423-016-1508-y
Grau-Talens EJ, Motos-Micó JJ, Giraldo-Rubio R, Aparicio-Gallego JM, Salgado JF, Ibáñez CD, Mangione-Castro PG, Arribas-Jurado M, Jordán-Chaves C, Arias-Díaz J (2018) Small-incision cholecystectomy (through a cylinder retractor) under local anaesthesia and sedation: a prospective observational study of five hundred consecutive cases. Langenbeck’s Arch Surg 403:733–740. https://doi.org/10.1007/s00423-018-1707-9
Gutt CN, Encke J, Köninger J, Harnoss J-C, Weigand K, Kipfmüller K, Schunter O, Götze T, Golling MT, Menges M, Klar E, Feilhauer K, Zoller WG, Ridwelski K, Ackmann S, Baron A, Schön MR, Seitz HK, Daniel D, Stremmel W, Büchler MW (2013) Acute cholecystitis: early versus delayed cholecystectomy, a multicenter randomized trial (ACDC study, NCT00447304). Ann Surg 258:385–393. https://doi.org/10.1097/SLA.0b013e3182a1599b
Saber A, Hokkam EN (2014) Operative outcome and patient satisfaction in early and delayed laparoscopic cholecystectomy for acute cholecystitis. Minim Invasive Surg 2014:162643. https://doi.org/10.1155/2014/162643
Macafee DAL, Humes DJ, Bouliotis G, Beckingham IJ, Whynes DK, Lobo DN (2009) Prospective randomized trial using cost-utility analysis of early versus delayed laparoscopic cholecystectomy for acute gallbladder disease. Br J Surg 96:1031–1040. https://doi.org/10.1002/bjs.6685
Lyu Y, Cheng Y, Wang B, Zhao S, Chen L (2018) Early versus delayed laparoscopic cholecystectomy for acute cholecystitis: an up-to-date meta-analysis of randomized controlled trials. Surg Endosc 32:4728–4741. https://doi.org/10.1007/s00464-018-6400-0
Author information
Authors and Affiliations
Contributions
J: analysis and interpretation of data, drafting of manuscript, critical revision of manuscript. R: analysis and interpretation of data, drafting of manuscript, critical revision of manuscript. K: analysis and interpretation of data, drafting of manuscript, critical revision of manuscript. B: study conception and design, acquisition of data, analysis and interpretation of data, drafting of manuscript, critical revision of manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
Based on national Danish law, informed consent was not needed from participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This paper is not based on a previous communication to a society or meeting.
Rights and permissions
About this article
Cite this article
Jensen, K.K., Roth, N.O., Krarup, PM. et al. Surgical management of acute cholecystitis in a nationwide Danish cohort. Langenbecks Arch Surg 404, 589–597 (2019). https://doi.org/10.1007/s00423-019-01802-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-019-01802-0