Abstract
Introduction
Sprint interval training (SIT), characterized by brief bouts of ‘supramaximal’ exercise interspersed with recovery periods, increases peak oxygen uptake (\({\dot{\text{V}}}{\text{O}}_{2{\text{peak}}} \)) despite a low total exercise volume. Per the Fick principle, increased \({\dot{\text{V}}}{\text{O}}_{2{\text{peak}}} \) is attributable to increased peak cardiac output (\({\dot{{Q}}}_{\text{peak}} \)) and/or peak arterio-venous oxygen difference (a-vO2diff). There are limited and equivocal data regarding the physiological basis for SIT-induced increases in \({\dot{\text{V}}}{\text{O}}_{2{\text{peak}}} \), with most studies lasting ≤ 6 weeks.
Purpose
To determine the effect of 12 weeks of SIT on \({\dot{{Q}}}_{\text{peak}} \), measured using inert gas rebreathing, and the relationship between changes in \({\dot{{Q}}}_{\text{peak}} \) and \({\dot{\text{V}}}{\text{O}}_{2{\text{peak}}} \).
Methods
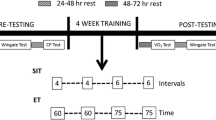
15 healthy untrained adults [6 males, 9 females; 21 ± 2 y (mean ± SD)] performed 28 ± 3 training sessions. Each session involved a 2-min warm-up at 50 W, 3 × 20-s ‘all-out’ cycling bouts (581 ± 221 W) interspersed with 2-min of recovery, and a 3-min cool-down at 50 W.
Results
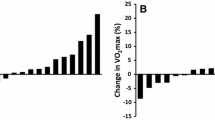
Measurements performed before and after training showed that 12 weeks of SIT increased \({\dot{{Q}}}_{\text{peak}} \) (17.0 ± 3.7 vs 18.1 ± 4.6 L/min, p = 0.01, partial η2 = 0.28) and \({\dot{\text{V}}}{\text{O}}_{2{\text{peak}}} \) (2.63 ± 0.78 vs 3.18 ± 1.1 L/min, p < 0.01, partial η2 = 0.58). The changes in these two variables were correlated (r2 = 0.46, p < 0.01). Calculated peak a-vO2diff also increased after training (154 ± 22 vs 174 ± 23 ml O2/L; p < 0.01) and was correlated with the change in \({\dot{\text{V}}}{\text{O}}_{2{\text{peak}}} \) (r2 = 0.33, p = 0.03). Exploratory analyses revealed an interaction (p < 0.01) such that \({\dot{{Q}}}_{\text{peak}} \) increased in male (+ 10%, p < 0.01) but not female participants (+ 0.6%, p = 0.96), suggesting potential sex-specific differences.
Conclusion
Twelve weeks of SIT increased \({\dot{{Q}}}_{\text{peak}} \) by 6% in previously untrained participants and the change was correlated with the larger 21% increase in \({\dot{\text{V}}}{\text{O}}_{2{\text{peak}}} \).




Similar content being viewed by others
Data availability
The datasets generated and/or analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- a-vO2diff :
-
Arterio-venous oxygen difference
- ANOVA:
-
Analysis of variance
- bpm:
-
Beats per minute
- CI:
-
Cardiac index
- CV:
-
Coefficient of variation
- h:
-
Hours
- HIIT:
-
High-intensity interval training
- HR:
-
Heart rate
- kg:
-
Kilograms
- kJ:
-
Kilojoules
- L/min:
-
Liters per minute
- MICT:
-
Moderate intensity continuous training
- min:
-
Minutes
- MET:
-
Metabolic equivalent of task
- ml O2/L blood:
-
Milliliters of oxygen per liter of blood
- partial η 2 :
-
Partial eta-squared
- \({\dot{{Q}}}_{\text{peak}} \) :
-
Peak cardiac output
- r:
-
Correlation coefficient
- RER:
-
Respiratory exchange ratio
- rpm:
-
Revolutions per minute
- s:
-
Seconds
- SD:
-
Standard deviation
- SIT:
-
Sprint interval training
- SVpeak :
-
Peak stroke volume
- TT:
-
Time trial
- W:
-
Watts
- W peak :
-
Peak power output
- \({\dot{\text{V}}}{\text{O}}_{2{\text{peak}}} \) :
-
Peak oxygen consumption
References
Agostoni P, Cattadori G, Apostolo A et al (2005) Noninvasive measurement of cardiac output during exercise by inert gas rebreathing technique: a new tool for heart failure evaluation. J Am Coll Cardiol 46:1779–1781. https://doi.org/10.1016/j.jacc.2005.08.005
Agostoni P, Vignati C, Gentile P et al (2017) Reference values for peak exercise cardiac output in healthy individuals. Chest 151:1329–1337. https://doi.org/10.1016/j.chest.2017.01.009
Ansdell P, Thomas K, Hicks KM et al (2020) Physiological sex differences affect the integrative response to exercise: Acute and chronic implications. Exp Physiol 105:2007–2021. https://doi.org/10.1113/EP088548
Astorino TA, Edmunds RM, Clark A et al (2018) Increased cardiac output and maximal oxygen uptake in response to ten sessions of high intensity interval training. J Sport Med Phys Fit 58:164–171. https://doi.org/10.23736/S0022-4707.16.06606-8
Ayotte B, Seymour J, McIlroy M (1970) A new method for measurement of cardiac output with nitrous oxide. J Appl Physiol 28:863–866. https://doi.org/10.1152/jappl.1970.28.6.863
Burgomaster KA, Hughes SC, Heigenhauser GJF et al (2005) Six sessions of sprint interval training increases muscle oxidative potential and cycle endurance capacity in humans. J Appl Physiol 98:1985–1990. https://doi.org/10.1152/japplphysiol.01095.2004
Christensen P, Clemensen P, Andersen PK, Henneberg SW (2000) Thermodilution versus inert gas rebreathing for estimation of effective pulmonary blood flow. Crit Care Med 28:51–56. https://doi.org/10.1097/00003246-200001000-00008
CSEP Get Active Questionnaire. Canadian Society for Exercise Physiology, Ottawa, ON, Canada. Available from https://www.csep.ca/CMFiles/GAQ_CSEPPATHReadinessForm_2pages.pdf; 2017
De Revere JL, Clausen RD, Astorino TA (2021) Changes in VO2max and cardiac output in response to short-term high-intensity interval training in Caucasian and Hispanic young women: a pilot study. PLoS ONE 16:1–15. https://doi.org/10.1371/journal.pone.0244850
Diaz-Canestro C, Montero D (2020) The Impact of Sex on left ventricular cardiac adaptations to endurance training: a systematic review and meta‑analysis. Sport Med. 50:1501–1513. https://doi.org/10.1007/s40279-020-01294-9
Elliott-Sale KJ, McNulty KL, Ansdell P et al (2020) The effects of oral contraceptives on exercise performance in women: a systematic review and meta-analysis. Sport Med 50:1785–1812. https://doi.org/10.1007/s40279-020-01317-5
Gifford JR, Garten RS, Nelson AD et al (2016) Symmorphosis and skeletal muscle VO2max: in vivo and in vitro measures reveal differing constraints in the exercise-trained and untrained human. J Physiol 6:1741–1751. https://doi.org/10.1113/JP271229
Gillen J, Martin B, MacInnis M et al (2016) Twelve weeks of sprint interval training improves indices of cardiometabolic health similar to traditional endurance training despite a five-fold lower exercise volume and time commitment. PLoS ONE. https://doi.org/10.1371/journal.pone.0154075
Gist NH, Fedewa MV, Dishman RK, Cureton KJ (2014) Sprint interval training effects on aerobic capacity: a systematic review and meta-analysis. Sport Med 44:269–279. https://doi.org/10.1007/s40279-013-0115-0
Gordon D, Scruton A, Barnes R et al (2018) The effects of menstrual cycle phase on the incidence of plateau at VO2max and associated cardiorespiratory dynamics. Clin Physiol Funct Imaging 38:689–698. https://doi.org/10.1111/cpf.12469
Gordon D, Swain P, Keiller D et al (2020) Quantifying the effects of four weeks of low-volume high-intensity sprint interval training on VO2max through assessment of hemodynamics. J Sport Med Phys Fit 60:53–61. https://doi.org/10.23736/s0022-4707.19.09912-2
Helgerud J, Hoydal K, Wang E et al (2007) Aerobic high-intensity intervals improve VO2max more than moderate training. Med Sci Sport Exerc 39:665–671. https://doi.org/10.1249/mss.0b013e3180304570
Howden EJ, Perhonen M, Peshock RM et al (2015) Females have a blunted cardiovascular response to one year of intensive supervised endurance training. J Appl Physiol 119:37–46. https://doi.org/10.1152/japplphysiol.00092.2015
Iannetta D, de Almeida AR, Ingram CP et al (2020) Evaluating the suitability of supra-POpeak verification trials after ramp-incremental exercise to confirm the attainment of maximum O2 uptake. Am J Physiol Regul Integr Comp Physiol 319:R315–R322. https://doi.org/10.1152/ajpregu.00126.2020
Jacobs RA, Flück D, Bonne TC et al (2013) Improvements in exercise performance with high-intensity interval training coincide with an increase in skeletal muscle mitochondrial content and function. J Appl Physiol 115:785–793. https://doi.org/10.1152/japplphysiol.00445.2013
Lakens D (2013) Calculating and reporting effect sizes to facilitate cumulative science: a practical primer for t-tests and ANOVAs. Front Psychol 4:1–12. https://doi.org/10.3389/fpsyg.2013.00863
Larsen FJ, Schiffer TA, Zinner C et al (2020) Mitochondrial oxygen affinity increases after sprint interval training and is related to the improvement in peak oxygen uptake. Acta Physiol 229:1–9. https://doi.org/10.1111/apha.13463
Lundby C, Montero D, Joyner M (2017) Biology of VO2max: looking under the physiology lamp. Acta Physiol 220:218–228. https://doi.org/10.1111/apha.12827
MacInnis MJ, Gibala MJ (2017) Physiological adaptations to interval training and the role of exercise intensity. J Physiol 9:2915–2930. https://doi.org/10.1113/JP273196
Macpherson R, Hazell T, Olver T et al (2011) Run sprint interval training improves aerobic performance but not maximal cardiac output. Med Sci Sports Exerc 43:115–122. https://doi.org/10.1249/MSS.0b013e3181e5eacd
Mattu AT, Iannetta D, MacInnis MJ et al (2020) Menstrual and oral contraceptive cycle phases do not affect submaximal and maximal exercise responses. Scand J Med Sci Sport 30:472–484. https://doi.org/10.1111/sms.13590
McKenna MJ, Heigenhauser GJ, McKelvie RS et al (1997) Sprint training enhances ionic regulation during intense exercise in men. J Physiol 501:687–702. https://doi.org/10.1111/j.1469-7793.1997.687bm.x
Metcalfe RS, Babraj JA, Fawkner SG, Vollaard NBJ (2012) Towards the minimal amount of exercise for improving metabolic health: Beneficial effects of reduced-exertion high-intensity interval training. Eur J Appl Physiol 112:2767–2775. https://doi.org/10.1007/s00421-011-2254-z
Milanović Z, Sporiš G, Weston M (2015) Effectiveness of high-intensity interval training (HIT) and continuous endurance training for VO2max improvements: a systematic review and meta-analysis of controlled trials. Sport Med 45:1469–1481. https://doi.org/10.1007/s40279-015-0365-0
Montero D, Cathomen A, Jacobs RA et al (2015a) Haematological rather than skeletal muscle adaptations contribute to the increase in peak oxygen uptake induced by moderate endurance training. J Physiol 593:4677–4688. https://doi.org/10.1113/JP270250
Montero D, Diaz-Canestro C, Lundby C (2015b) Endurance training and VO2max: role of maximal cardiac output and oxygen extraction. Med Sci Sports Exerc 47:2024–2033. https://doi.org/10.1249/MSS.0000000000000640
Mosteller RD (1987) Simplified calculation of body-surface area. N Engl J Med 317:1098. https://doi.org/10.1056/nejm198710223171717
Raleigh JP, Giles MD, Islam H et al (2018) Contribution of central and peripheral adaptations to changes in maximal oxygen uptake following four weeks of sprint interval training. Appl Physiol Nutr Metab 43:1059–1068. https://doi.org/10.1139/apnm-2017-0864
Rossiter HB, Kowalchuk JM, Whipp BJ (2006) A test to establish maximum O2 uptake despite no plateau in the O2 uptake response to ramp incremental exercise. J Appl Physiol 100:764–770. https://doi.org/10.1152/japplphysiol.00932.2005
Schaumberg MA, Jenkins DG, Janse De Jonge XAK et al (2017) Oral contraceptive use dampens physiological adaptations to sprint interval training. Med Sci Sports Exerc 49:717–727. https://doi.org/10.1249/MSS.0000000000001171
Scribbans TD, Edgett BA, Vorobej K et al (2014) Fibre-specific responses to endurance and low volume high intensity interval training: striking similarities in acute and chronic adaptation. PLoS ONE. https://doi.org/10.1371/journal.pone.0098119
Siebenmann C, Rasmussen P, Sørensen H et al (2015) Cardiac output during exercise: a comparison of four methods. Scand J Med Sci Sport 25:e20–e27. https://doi.org/10.1111/sms.12201
Skattebo Ø, Calbet J, Rud B et al (2020) Contribution of oxygen extraction fraction to maximal oxygen uptake in healthy young men. Acta Physiol. https://doi.org/10.1111/apha.13486
Spina R, Ogawa T, Kohrt W et al (1993) Differences in cardiovascular adaptations to endurance exercise training between older men and women. J Appl Physiol 75:849–855. https://doi.org/10.1152/jappl.1993.75.2.849
Warburton DER, Haykowsky MJ, Quinney HA et al (2004) Blood volume expansion and cardiorespiratory function: effects of training modality. Med Sci Sports Exerc 36:991–1000. https://doi.org/10.1249/01.MSS.0000128163.88298.CB
Weston KS, Wisløff U, Coombes JS (2014) High-intensity interval training in patients with lifestyle-induced cardiometabolic disease: A systematic review and meta-analysis. Br J Sports Med 48:1227–1234. https://doi.org/10.1136/bjsports-2013-092576
Acknowledgements
This work was supported by an operating grant from the Natural Sciences and Engineering Research Council of Canada to MJG.
Author information
Authors and Affiliations
Contributions
WB, SEV, DGM, MJM, MJM, and MJG contributed to conceptualization and methodology; WB, SEV, and DGM, data collection; WB, SEV, DGM, MJM, MJM, and MJG, data analysis and interpretation; WB. SEV, DGM, MJM, MJM, and MJG, manuscript preparation and editing; DLR, MJM, MJM, and MJG, supervision; MJG, funding acquisition. All authors read and approved the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The study procedures were approved by the Hamilton Integrated Research Ethics Board.
Consent to participate
All participants provided written informed consent prior to their participation.
Additional information
Communicated by Ellen adele dawson.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Bostad, W., Valentino, S.E., McCarthy, D.G. et al. Twelve weeks of sprint interval training increases peak cardiac output in previously untrained individuals. Eur J Appl Physiol 121, 2449–2458 (2021). https://doi.org/10.1007/s00421-021-04714-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-021-04714-4