Abstract
Background
Many neuroscience and neurology studies have forced a reconsideration of the traditional motor-related scope of cerebellar function, which has now expanded to include various cognitive functions. Spinocerebellar ataxia type 3 (SCA3; the most common hereditary ataxia) is neuropathologically characterized by cerebellar atrophy and frequently presents with cognitive impairment.
Objective
To characterize cognitive impairment in SCA3 and investigate the cerebellum–cognition associations.
Methods
This prospective, cross-sectional cohort study recruited 126 SCA3 patients and 41 healthy control individuals (HCs). Participants underwent a brain 3D T1-weighted images as well as neuropsychological tests. Voxel-based morphometry (VBM) and region of interest (ROI) approaches were performed on the 3D T1-weighted images. CERES was used to automatically segment cerebellums. Patients were grouped into cognitively impaired (CI) and cognitively preserved (CP), and clinical and MRI parameters were compared. Multivariable regression models were fitted to examine associations between cerebellar microstructural alterations and cognitive domain impairments.
Results
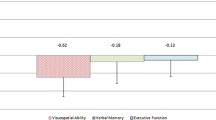
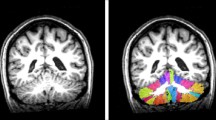
Compared to HCs, SCA3 patients showed cognitive domain impairments in information processing speed, verbal memory, executive function, and visuospatial perception. Between CI and CP subgroups, the CI subgroup was older and had lower education, as well as higher severity scores. VBM and ROI analyses revealed volume loss in cerebellar bilateral lobule VI, right lobule Crus I, and right lobule IV of the CI subgroup, and all these cerebellar lobules were associated with the above cognitive domain impairments.
Conclusions
Our findings demonstrate the multiple cognitive domain impairments in SCA3 patients and indicate the responsible cerebellar lobules for the impaired cognitive domain(s).


Similar content being viewed by others
Data Availability
The data sets used or analyzed during the current study are available from the corresponding author on reasonable request.
References
Sereno MI, Diedrichsen J, Tachrount M, Testa-Silva G, d’Arceuil H, De Zeeuw C (2020) The human cerebellum has almost 80% of the surface area of the neocortex. Proc Natl Acad Sci U S A 117:19538–19543
Buckner RL (2013) The cerebellum and cognitive function: 25 years of insight from anatomy and neuroimaging. Neuron 80:807–815
Schmahmann JD, Guell X, Stoodley CJ, Halko MA (2019) The theory and neuroscience of cerebellar cognition. Annu Rev Neurosci 42:337–364
Stoodley CJ (2012) The cerebellum and cognition: evidence from functional imaging studies. Cerebellum 11:352–365
Olivito G, Serra L, Marra C, Di Domenico C, Caltagirone C, Toniolo S, Cercignani M, Leggio M, Bozzali M (2020) Cerebellar dentate nucleus functional connectivity with cerebral cortex in Alzheimer’s disease and memory: a seed-based approach. Neurobiol Aging 89:32–40
Yao Q, Tang F, Wang Y, Yan Y, Dong L, Wang T, Zhu D, Tian M, Lin X, Shi J (2022) Effect of cerebellum stimulation on cognitive recovery in patients with Alzheimer disease: a randomized clinical trial. Brain Stimul 15:910–920
Kawabata K, Watanabe H, Bagarinao E, Ohdake R, Hara K, Ogura A, Masuda M, Kato T, Tsuboi T, Maesawa S, Katsuno M, Sobue G (2020) Cerebello-basal ganglia connectivity fingerprints related to motor/cognitive performance in Parkinson’s disease. Parkinsonism Relat Disord 80:21–27
Pasqua G, Tommasin S, Bharti K, Ruggieri S, Petsas N, Piervincenzi C, Pozzilli C, Pantano P (2021) Resting-state functional connectivity of anterior and posterior cerebellar lobes is altered in multiple sclerosis. Mult Scler 27:539–548
Jacobs HIL, Hopkins DA, Mayrhofer HC, Bruner E, van Leeuwen FW, Raaijmakers W, Schmahmann JD (2018) The cerebellum in Alzheimer’s disease: evaluating its role in cognitive decline. Brain 141:37–47
Schmahmann JD, Caplan D (2006) Cognition, emotion and the cerebellum. Brain: J Neurol 129:290–292
Ruet A, Hamel D, Deloire MS, Charre-Morin J, Saubusse A, Brochet B (2014) Information processing speed impairment and cerebellar dysfunction in relapsing-remitting multiple sclerosis. J Neurol Sci 347:246–250
Tabatabaei-Jafari H, Walsh E, Shaw ME, Cherbuin N, Alzheimer’s Disease Neuroimaging I (2017) The cerebellum shrinks faster than normal ageing in Alzheimer’s disease but not in mild cognitive impairment. Hum Brain Mapp 38:3141–3150
Klockgether T, Mariotti C, Paulson HL (2019) Spinocerebellar ataxia. Nat Rev Dis Primers 5:24
Dürr A, Stevanin G, Cancel G, Duyckaerts C, Abbas N, Didierjean O, Chneiweiss H, Benomar A, Lyon-Caen O, Julien J, Serdaru M, Penet C, Agid Y, Brice A (1996) Spinocerebellar ataxia 3 and Machado-Joseph disease: clinical, molecular, and neuropathological features. Ann Neurol 39:490–499
Guimaraes RP, D’Abreu A, Yasuda CL, Franca MC Jr, Silva BH, Cappabianco FA, Bergo FP, Lopes-Cendes IT, Cendes F (2013) A multimodal evaluation of microstructural white matter damage in spinocerebellar ataxia type 3. Mov Disord 28:1125–1132
de Rezende TJ, D’Abreu A, Guimaraes RP, Lopes TM, Lopes-Cendes I, Cendes F, Castellano G, Franca MC Jr (2015) Cerebral cortex involvement in Machado-Joseph disease. Eur J Neurol 22(277–283):e223-274
Rezende TJR, de Paiva JLR, Martinez ARM, Lopes-Cendes I, Pedroso JL, Barsottini OGP, Cendes F, Franca MC Jr (2018) Structural signature of SCA3: from presymptomatic to late disease stages. Ann Neurol 84:401–408
Hengel H, Martus P, Faber J, Giunit P, Garcia-Moreno H, Solanky N, Klockgether T, Reetz K, van de Warrenburg BP, Santana MM, Silva P, Cunha I, de Almeida LP, Timmann D, Infante J, de Vries J, Lima M, Pires P, Bushara K, Jacobi H, Onyike C, Schmahmann JD, Hübener-Schmid J, Synofzik M, Schöls L (2023) The frequency of non-motor symptoms in SCA3 and their association with disease severity and lifestyle factors. J Neurol 270:944–952
Yap KH, Kessels RPC, Azmin S, van de Warrenburg B, Mohamed Ibrahim N (2022) Neurocognitive changes in spinocerebellar Ataxia type 3: a systematic review with a Narrative design. Cerebellum 21:314–327
Ackermann H (2008) Cerebellar contributions to speech production and speech perception: psycholinguistic and neurobiological perspectives. Trends Neurosci 31:265–272
Lopes TM, D’Abreu A, França MC Jr, Yasuda CL, Betting LE, Samara AB, Castellano G, Somazz JC, Balthazar ML, Lopes-Cendes I, Cendes F (2013) Widespread neuronal damage and cognitive dysfunction in spinocerebellar ataxia type 3. J Neurol 260:2370–2379
Silva UC, Marques W Jr, Lourenco CM, Hallak JE, Osorio FL (2015) Psychiatric disorders, spinocerebellar ataxia type 3 and CAG expansion. J Neurol 262:1777–1779
Stefanescu MR, Dohnalek M, Maderwald S, Thürling M, Minnerop M, Beck A, Schlamann M, Diedrichsen J, Ladd ME, Timmann D (2015) Structural and functional MRI abnormalities of cerebellar cortex and nuclei in SCA3, SCA6 and Friedreich’s ataxia. Brain: J Neurol 138:1182–1197
Romero JE, Coupe P, Giraud R, Ta VT, Fonov V, Park MTM, Chakravarty MM, Voineskos AN, Manjon JV (2017) CERES: a new cerebellum lobule segmentation method. Neuroimage 147:916–924
Zeng Y, Feng Q, Hesketh T, Christensen K, Vaupel JW (2017) Survival, disabilities in activities of daily living, and physical and cognitive functioning among the oldest-old in China: a cohort study. Lancet 389:1619–1629
Nie K, Zhang Y, Wang L, Zhao J, Huang Z, Gan R, Li S, Wang L (2012) A pilot study of psychometric properties of the Beijing version of montreal cognitive assessment in patients with idiopathic Parkinson’s disease in China. J Clin Neurosci 19:1497–1500
Zhang N, Li YJ, Fu Y, Shao JH, Luo LL, Yang L, Shi FD, Liu Y (2015) Cognitive impairment in Chinese neuromyelitis optica. Mult Scler 21:1839–1846
Dong X, Xu G, Wang J, Yin N, Meng N (2022) Clinical and MRI predictors of cognitive decline in patients with relapsing-remitting multiple sclerosis: a 2-year longitudinal study. Mult Scler Relat Disord 65:103838
Benedict RH, Zivadinov R (2007) Reliability and validity of neuropsychological screening and assessment strategies in MS. J Neurol 254(Suppl 2):II22–II25
Maas R, Killaars S, van de Warrenburg BPC, Schutter D (2021) The cerebellar cognitive affective syndrome scale reveals early neuropsychological deficits in SCA3 patients. J Neurol 268:3456–3466
Thieme A, Faber J, Sulzer P, Reetz K, Dogan I, Barkhoff M, Krahe J, Jacobi H, Aktories JE, Minnerop M, Elben S, van der Veen R, Müller J, Batsikadze G, Konczak J, Synofzik M, Roeske S, Timmann D (2022) The CCAS-scale in hereditary ataxias: helpful on the group level, particularly in SCA3, but limited in individual patients. J Neurol 269:4363–4374
Zheng YP, Zhao JP, Phillips M, Liu JB, Cai MF, Sun SQ, Huang MF (1988) Validity and reliability of the Chinese Hamilton depression rating scale. Br J Psychiatry 152:660–664
Hamilton M (1959) The assessment of anxiety states by rating. Br J Med Psychol 32:50–55
Dusankova JB, Kalincik T, Havrdova E, Benedict RH (2012) Cross cultural validation of the minimal assessment of cognitive function in multiple sclerosis (MACFIMS) and the brief international cognitive assessment for multiple sclerosis (BICAMS). Clin Neuropsychol 26:1186–1200
Schmitz-Hubsch T, du Montcel ST, Baliko L, Berciano J, Boesch S, Depondt C, Giunti P, Globas C, Infante J, Kang JS, Kremer B, Mariotti C, Melegh B, Pandolfo M, Rakowicz M, Ribai P, Rola R, Schols L, Szymanski S, van de Warrenburg BP, Durr A, Klockgether T, Fancellu R (2006) Scale for the assessment and rating of ataxia: development of a new clinical scale. Neurology 66:1717–1720
Trouillas P, Takayanagi T, Hallett M, Currier R, Subramony S, Wessel K, Bryer A, Diener H, Massaquoi S, Gomez C, Coutinho P, Ben Hamida M, Campanella G, Filla A, Schut L, Timann D, Honnorat J, Nighoghossian N, Manyam B (1997) International cooperative Ataxia rating scale for pharmacological assessment of the cerebellar syndrome. The Ataxia neuropharmacology committee of the world federation of neurology. J Neurol Sci 145:205–211
Maas RP, van Gaalen J, Klockgether T, van de Warrenburg BP (2015) The preclinical stage of spinocerebellar ataxias. Neurology 85:96–103
Feng L, Chen DB, Hou L, Huang LH, Lu SY, Liang XL, Li XH (2014) Cognitive impairment in native Chinese with spinocerebellar ataxia type 3. Eur Neurol 71:262–270
Lin Q, Liu Y, Ye Z, Hu J, Cai W, Weng Q, Chen W, Wang N, Cao D, Lin Y, Fu Y (2021) Potential markers for sample size estimations in hereditary spastic paraplegia type 5. Orphanet J Rare Dis 16:391
Li M, Chen X, Xu H, Huang Z, Chen N, Tu Y, Gan S, Hu J (2021) Brain structural abnormalities in the preclinical stage of Machado-Joseph disease/spinocerebellar ataxia type 3 (MJD/SCA3): evaluation by MRI morphometry, diffusion tensor imaging and neurite orientation dispersion and density imaging. J Neurol 269:2989–2998
Braga-Neto P, Pedroso JL, Alessi H, Dutra LA, Felicio AC, Minett T, Weisman P, Santos-Galduroz RF, Bertolucci PH, Gabbai AA, Barsottini OG (2012) Cerebellar cognitive affective syndrome in Machado Joseph disease: core clinical features. Cerebellum 11:549–556
Ma J, Wu C, Lei J, Zhang X (2014) Cognitive impairments in patients with spinocerebellar ataxia types 1, 2 and 3 are positively correlated to the clinical severity of ataxia symptoms. Int J Clin Exp Med 7:5765–5771
Hoche F, Guell X, Vangel MG, Sherman JC, Schmahmann JD (2018) The cerebellar cognitive affective/Schmahmann syndrome scale. Brain 141:248–270
Stoodley CJ, Schmahmann JD (2009) Functional topography in the human cerebellum: a meta-analysis of neuroimaging studies. Neuroimage 44:489–501
Bushara KO, Wheat JM, Khan A, Mock BJ, Turski PA, Sorenson J, Brooks BR (2001) Multiple tactile maps in the human cerebellum. NeuroReport 12:2483–2486
Bando K, Honda T, Ishikawa K, Takahashi Y, Mizusawa H, Hanakawa T (2019) Impaired adaptive motor learning is correlated with cerebellar hemispheric gray matter atrophy in spinocerebellar ataxia patients: a voxel-based morphometry study. Front Neurol 10:1183
Olivito G, Lupo M, Iacobacci C, Clausi S, Romano S, Masciullo M, Molinari M, Cercignani M, Bozzali M, Leggio M (2018) Structural cerebellar correlates of cognitive functions in spinocerebellar ataxia type 2. J Neurol 265:597–606
D’Agata F, Caroppo P, Boghi A, Coriasco M, Caglio M, Baudino B, Sacco K, Cauda F, Geda E, Bergui M, Geminiani G, Bradac GB, Orsi L, Mortara P (2011) Linking coordinative and executive dysfunctions to atrophy in spinocerebellar ataxia 2 patients. Brain Struct Funct 216:275–288
Dogan I, Tinnemann E, Romanzetti S, Mirzazade S, Costa AS, Werner CJ, Heim S, Fedosov K, Schulz S, Timmann D, Giordano IA, Klockgether T, Schulz JB, Reetz K (2016) Cognition in Friedreich’s ataxia: a behavioral and multimodal imaging study. Ann Clin Transl Neurol 3:572–587
Yang H, Wang N, Luo X, Lv H, Liu H, Li Y, Fan G (2019) Cerebellar atrophy and its contribution to motor and cognitive performance in multiple system atrophy. Neuroimage Clin 23:101891
Toniolo S, Serra L, Olivito G, Marra C, Bozzali M, Cercignani M (2018) Patterns of cerebellar gray matter atrophy across Alzheimer’s disease progression. Front Cell Neurosci 12:430
Moroso A, Ruet A, Lamargue-Hamel D, Munsch F, Deloire M, Coupé P, Ouallet JC, Planche V, Moscufo N, Meier DS, Tourdias T, Guttmann CR, Dousset V, Brochet B (2017) Posterior lobules of the cerebellum and information processing speed at various stages of multiple sclerosis. J Neurol Neurosurg Psychiatry 88:146–151
Fritz NE, Edwards EM, Ye C, Prince J, Yang Z, Gressett T, Keller J, Myers E, Calabresi PA, Zackowski KM (2022) Cerebellar contributions to motor and cognitive control in multiple sclerosis(✰✰✰). Arch Phys Med Rehabil 103:1592–1599
Morelli N (2022) Patients with Parkinson’s disease and a history of falls have decreased cerebellar grey matter volumes in the cognitive cerebellum. Rev Neurol (Paris) 178:924–931
Chen Y, Landin-Romero R, Kumfor F, Irish M, Dobson-Stone C, Kwok JB, Halliday GM, Hodges JR, Piguet O (2022) Cerebellar integrity and contributions to cognition in C9orf72-mediated frontotemporal dementia. Cortex 149:73–84
Benussi A, Cantoni V, Manes M, Libri I, Dell’Era V, Datta A, Thomas C, Ferrari C, Di Fonzo A, Fancellu R, Grassi M, Brusco A, Alberici A, Borroni B (2021) Motor and cognitive outcomes of cerebello-spinal stimulation in neurodegenerative ataxia. Brain 144:2310–2321
Chen XY, Lian YH, Liu XH, Sikandar A, Li MC, Xu HL, Hu JP, Chen QL, Gan SR (2022) Effects of repetitive transcranial magnetic stimulation on cerebellar metabolism in patients with spinocerebellar ataxia type 3. Front Aging Neurosci 14:827993
Maas R, Teerenstra S, Toni I, Klockgether T, Schutter D, van de Warrenburg BPC (2022) Cerebellar transcranial direct current stimulation in spinocerebellar ataxia type 3: a randomized, double-blind, sham-controlled trial. Neurotherapeutics 19:1259–1272
D’Mello AM, Turkeltaub PE, Stoodley CJ (2017) Cerebellar tDCS modulates neural circuits during semantic prediction: a combined tDCS-fMRI study. J Neurosci 37:1604–1613
Maas R, Faber J, van de Warrenburg BPC, Schutter D (2023) Interindividual differences in posterior fossa morphometry affect cerebellar tDCS-induced electric field strength. Clin Neurophysiol 153:152–165
Yacoubi B, Casamento-Moran A, Burciu RG, Subramony SH, Vaillancourt DE, Christou EA (2020) Temporal invariance in SCA6 is related to smaller cerebellar lobule VI and greater disease severity. J Neurosci 40:1722–1731
Suenaga M, Kawai Y, Watanabe H, Atsuta N, Ito M, Tanaka F, Katsuno M, Fukatsu H, Naganawa S, Sobue G (2008) Cognitive impairment in spinocerebellar ataxia type 6. J Neurol Neurosurg Psychiatry 79:496–499
Grady C (2012) The cognitive neuroscience of ageing. Nat Rev Neurosci 13:491–505
Kumar M, Hiremath C, Khokhar SK, Bansal E, Sagar KJV, Padmanabha H, Girimaji AS, Narayan S, Kishore MT, Yamini BK, JacFredo AR, Saini J, Bharath RD (2023) Altered cerebellar lobular volumes correlate with clinical deficits in siblings and children with ASD: evidence from toddlers. J Transl Med 21:246
Torres K (2023) Comparison of core and process scores on the California verbal learning test-3 for Parkinson’s disease and essential tremor patients. J Clin Exp Neuropsychol 28:1–15
Li Y, Liu H, Yu H, Yang H, Guo M, Cao C, Pang H, Liu Y, Cao K, Fan G (2023) Alterations of voxel-wise spontaneous activity and corresponding brain functional networks in multiple system atrophy patients with mild cognitive impairment. Hum Brain Mapp 44:403–417
Monchi O, Petrides M, Strafella AP, Worsley KJ, Doyon J (2006) Functional role of the basal ganglia in the planning and execution of actions. Ann Neurol 59:257–264
Anderkova L, Barton M, Rektorova I (2017) Striato-cortical connections in Parkinson’s and Alzheimer’s diseases: relation to cognition. Mov Disord 32:917–922
Acknowledgements
The authors would like to thank the kind patients and families who participated in this research.
Funding
This work has been supported by the grants 82230039 (N.W.), 81870902 (N.W.), U21A20360 (Y.F.), 81971082 (S.R.G.) from the National Natural Science Foundation of China.
Author information
Authors and Affiliations
Consortia
Contributions
YF, NW, and SRG formulated and designed the study concept. ZXY, JB, LLQ, XYC, XYC, YSQ, RYY, XTY, CYH, WL, and WJC enrolled the patients and conducted clinical assessments and neuropsychological tests. ZXY, MCL, and JPH conducted imaging data collection. XYC, XTY, BC, and WL performed laboratory determination. ZXY, JB, LLQ, NW, YF, and SRG analyzed the data, and interpreted the results. All authors were involved in drafting/revising the manuscript.
Corresponding authors
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ye, ZX., Bi, J., Qiu, LL. et al. Cognitive impairment associated with cerebellar volume loss in spinocerebellar ataxia type 3. J Neurol 271, 918–928 (2024). https://doi.org/10.1007/s00415-023-12042-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-023-12042-0