Abstract
Purpose
The effects of sleep surgery on the lipid profile of adults diagnosed as having obstructive sleep apnea (OSA) remain unclear. This meta-analysis aimed to clarify whether sleep surgeries improve patients’ lipid profile.
Methods
The study protocol was registered on PROSPERO (CRD42020154425). Two authors independently searched the PubMed, MEDLINE, EMBASE, and Cochrane review databases up to September 2020 using keywords such as sleep apnea, OSA, sleep apnea syndromes, lipids, and surgery. The effects of sleep surgery on the apnea–hypopnea index (AHI) and lipid profile parameters were evaluated using a random-effects model.
Results
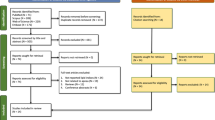
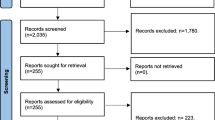
Thirteen studies were included, with a total of 710 patients (mean age: 42.0 years; 85% men; mean sample size: 54.6 patients). The summary estimate of AHI change was − 20.6 events/h (95% CI − 25.9 to − 15.3) and the Epworth Sleepiness Scale score was − 4.2 (95% CI − 5.9 to − 2.5). Sleep surgery lowered total cholesterol (mean − 7.7 mg/dL; 95% CI − 12.2 to − 3.2), low-density lipoprotein (mean − 7.2 mg/dL; 95% CI − 11.0 to − 3.3), and triglyceride (mean − 14.0 mg/dL; 95% CI − 22.2 to − 5.8) levels but did not affect high-density lipoprotein (mean 1.5 mg/dL; 95% CI − 0.6 to 3.7) levels. Subgroup analysis revealed that the lipid profile changes were not associated with the surgical procedure but with the degree of OSA improvement. Meta-regression analyses demonstrated that the improvement in the lipid profile was positively correlated with AHI reduction.
Conclusion
Surgeries for OSA may improve the lipid profile, which is positively correlated with the degree of OSA improvement.




Similar content being viewed by others
References
Gottlieb DJ, Punjabi NM (2020) Diagnosis and management of obstructive sleep apnea: a review. JAMA 323(14):1389–1400. https://doi.org/10.1001/jama.2020.3514
Heinzer R, Vat S, Marques-Vidal P, Marti-Soler H et al (2015) Prevalence of sleep-disordered breathing in the general population: the HypnoLaus study. Lancet Respir Med 3(4):310–318. https://doi.org/10.1016/S2213-2600(15)00043-0
Schwartz AR, Patil SP, Laffan AM, Polotsky V, Schneider H, Smith PL (2008) Obesity and obstructive sleep apnea: pathogenic mechanisms and therapeutic approaches. Proc Am Thorac Soc 5(2):185–192. https://doi.org/10.1513/pats.200708-137MG
Xu S, Wan Y, Xu M et al (2015) The association between obstructive sleep apnea and metabolic syndrome: a systematic review and meta-analysis. BMC Pulm Med 15:105. https://doi.org/10.1186/s12890-015-0102-3
Nadeem R, Singh M, Nida M et al (2014) Effect of obstructive sleep apnea hypopnea syndrome on lipid profile: a meta-regression analysis. J Clin Sleep Med 10(5):475–489. https://doi.org/10.5664/jcsm.3690
McPherson R, Frohlich J, Fodor G, Genest J (2006) Canadian Cardiovascular Society. Canadian Cardiovascular Society position statement—recommendations for the diagnosis and treatment of dyslipidemia and prevention of cardiovascular disease. Can J Cardiol 22(11):913–927. https://doi.org/10.1016/s0828-282x(06)70310-5
McDaid C, Griffin S, Weatherly H et al (2009) Continuous positive airway pressure devices for the treatment of obstructive sleep apnoea-hypopnoea syndrome: a systematic review and economic analysis. Health Technol Assess 13(4):143–274. https://doi.org/10.3310/hta13040 (iii–iv, xi–xiv, 1–119)
Xu H, Yi H, Guan J, Yin S (2014) Effect of continuous positive airway pressure on lipid profile in patients with obstructive sleep apnea syndrome: a meta-analysis of randomized controlled trials. Atherosclerosis 234(2):446–453. https://doi.org/10.1016/j.atherosclerosis.2014.03.034
Nadeem R, Singh M, Nida M et al (2014) Effect of CPAP treatment for obstructive sleep apnea hypopnea syndrome on lipid profile: a meta-regression analysis. J Clin Sleep Med 10(12):1295–1302. https://doi.org/10.5664/jcsm.4282
Lin MT, Lin HH, Lee PL et al (2015) Beneficial effect of continuous positive airway pressure on lipid profiles in obstructive sleep apnea: a meta-analysis. Sleep Breath 19(3):809–817. https://doi.org/10.1007/s11325-014-1082-x
Eveloff SE (2002) Treatment of obstructive sleep apnea: no longer just a lot of hot air. Chest 121(3):674–677. https://doi.org/10.1378/chest.121.3.674
Caples SM, Rowley JA, Prinsell JR et al (2010) Surgical modifications of the upper airway for obstructive sleep apnea in adults: a systematic review and meta-analysis. Sleep 33(10):1396–1407. https://doi.org/10.1093/sleep/33.10.1396
Kotecha BT, Hall AC (2014) Role of surgery in adult obstructive sleep apnoea. Sleep Med Rev 18(5):405–413. https://doi.org/10.1016/j.smrv.2014.02.003
Camacho M, Certal V, Brietzke SE, Holty JE, Guilleminault C, Capasso R (2014) Tracheostomy as treatment for adult obstructive sleep apnea: a systematic review and meta-analysis. Laryngoscope 124(3):803–811. https://doi.org/10.1002/lary.24433
Fujita S, Conway W, Zorick F, Roth T (1981) Surgical correction of anatomic azbnormalities in obstructive sleep apnea syndrome: uvulopalatopharyngoplasty. Otolaryngol Head Neck Surg 89(6):923–934. https://doi.org/10.1177/019459988108900609
Choi JH, Cho SH, Kim SN, Suh JD, Cho JH (2016) Predicting outcomes after uvulopalatopharyngoplasty for adult obstructive sleep apnea: a meta-analysis. Otolaryngol Head Neck Surg 155(6):904–913. https://doi.org/10.1177/0194599816661481
He M, Yin G, Zhan S et al (2019) Long-term efficacy of uvulopalatopharyngoplasty among adult patients with obstructive sleep apnea: a systematic review and meta-analysis. Otolaryngol Head Neck Surg 161(3):401–411. https://doi.org/10.1177/0194599819840356
Camacho M, Nesbitt NB, Lambert E et al (2017) Laser-assisted uvulopalatoplasty for obstructive sleep apnea: a systematic review and meta-analysis. Sleep. https://doi.org/10.1093/sleep/zsx004
Lin HC, Friedman M, Chang HW, Gurpinar B (2008) The efficacy of multilevel surgery of the upper airway in adults with obstructive sleep apnea/hypopnea syndrome. Laryngoscope 118(5):902–908. https://doi.org/10.1097/MLG.0b013e31816422ea
Holty JE, Guilleminault C (2010) Maxillomandibular advancement for the treatment of obstructive sleep apnea: a systematic review and meta-analysis. Sleep Med Rev 14(5):287–297. https://doi.org/10.1016/j.smrv.2009.11.003
Meccariello G, Cammaroto G, Montevecchi F et al (2017) Transoral robotic surgery for the management of obstructive sleep apnea: a systematic review and meta-analysis. Eur Arch Otorhinolaryngol 274(2):647–653. https://doi.org/10.1007/s00405-016-4113-3
Certal VF, Zaghi S, Riaz M et al (2015) Hypoglossal nerve stimulation in the treatment of obstructive sleep apnea: a systematic review and meta-analysis. Laryngoscope 125(5):1254–1264. https://doi.org/10.1002/lary.25032
Halle TR, Oh MS, Collop NA, Quyyumi AA, Bliwise DL, Dedhia RC (2017) Surgical treatment of OSA on cardiovascular outcomes: a systematic review. Chest 152(6):1214–1229. https://doi.org/10.1016/j.chest.2017.09.004
Kang KT, Yeh TH, Hsu YS et al (2021) Effect of sleep surgery on C-reactive protein levels in adults with obstructive sleep apnea: a meta-analysis. Laryngoscope 131(5):1180–1187. https://doi.org/10.1002/lary.29212
PROSPERO International Prospective Register of Systematic Reviews, Lee C-H, Kang K-T (2020) Effects of surgeries on cardiovascular markers in patients with obstructive sleep apnea. PROSPERO CRD42020154425. https://www.crd.york.ac.uk/prospero/display_record.php?ID=CRD42020154425
Page MJ, McKenzie JE, Bossuyt PM et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 372:n71. https://doi.org/10.1136/bmj.n71
Wells GA, Shea B, O’Connell D et al. The Newcastle–Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analysis. [WWW document]. http://www.ohri.ca/programs/clinical_epidemiology/oxford.htm
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327:557–560. https://doi.org/10.1136/bmj.327.7414.557
Kinoshita H, Shibano A, Sakoda T et al (2006) Uvulopalatopharyngoplasty decreases levels of C-reactive protein in patients with obstructive sleep apnea syndrome. Am Heart J 152(4):692.e1–5. https://doi.org/10.1016/j.ahj.2006.07.004
Lee MY, Lin CC, Lee KS et al (2009) Effect of uvulopalatopharyngoplasty on endothelial function in obstructive sleep apnea. Otolaryngol Head Neck Surg 140(3):369–374. https://doi.org/10.1016/j.otohns.2008.11.032
Lin CC, Wang YP, Lee KS, Liaw SF, Chiu CH (2014) Effect of uvulopalatopharyngoplasty on leptin and endothelial function in sleep apnea. Ann Otol Rhinol Laryngol 123(1):40–46. https://doi.org/10.1177/0003489414521385
Li L, Zhan X, Wang N et al (2014) Does airway surgery lower serum lipid levels in obstructive sleep apnea patients? A retrospective case review. Med Sci Monit 20:2651–2657. https://doi.org/10.12659/MSM.892230
Lu CH, Lin HC, Huang CC et al (2015) Increased circulating endothelial progenitor cells and anti-oxidant capacity in obstructive sleep apnea after surgical treatment. Clin Chim Acta 448:1–7. https://doi.org/10.1016/j.cca.2015.05.023
Zheng YL, Wan YF, Xie CL et al (2016) Influence of uvulopalatopharyngoplasty on serum uric acid level in obstructive sleep apnea patients. Lab Med 40(3):207–214. https://doi.org/10.1515/labmed-2015-0110
Lin WC, Huang CC, Chen HL et al (2016) Longitudinal brain structural alterations and systemic inflammation in obstructive sleep apnea before and after surgical treatment. J Transl Med 14(1):139. https://doi.org/10.1186/s12967-016-0887-8
Peng Y, Zhang L, Hu D, Dai Y, Wang S, Liao H, Xiong Y (2016) Reduction of internal carotid artery intima-media thickness in patients with moderate-to-severe obstructive sleep apnea syndrome after nasal surgery and uvulopalatopharyngoplasty. Acta Otolaryngol 136(5):514–521. https://doi.org/10.3109/00016489.2015.1130856
Chin CH, Lin PW, Lin HC, Friedman M, Lin MC (2019) Effects of OSA surgery on leptin and metabolic profiles. Otolaryngol Head Neck Surg 161(6):1048–1055. https://doi.org/10.1177/0194599819877647
Wang F, Liu Y, Xu H et al (2019) Association between upper-airway surgery and ameliorative risk markers of endothelial function in obstructive sleep apnea. Sci Rep 9(1):20157. https://doi.org/10.1038/s41598-019-56601-w
Li X, Huang H, Xu H et al (2019) Excessive daytime sleepiness, metabolic syndrome, and obstructive sleep apnea: two independent large cross-sectional studies and one interventional study. Respir Res 20(1):276. https://doi.org/10.1186/s12931-019-1248-y
Alterki A, Joseph S, Thanaraj TA et al (2020) Targeted metabolomics analysis on obstructive sleep apnea patients after multilevel sleep surgery. Metabolites 10(9):358. https://doi.org/10.3390/metabo10090358
Qian Y, Zou J, Xu H et al (2020) Association of upper airway surgery and improved cardiovascular biomarkers and risk in OSA. Laryngoscope 130(3):818–824. https://doi.org/10.1002/lary.28012
Elshaug AG, Moss JR, Southcott AM, Hiller JE (2007) Redefining success in airway surgery for obstructive sleep apnea: a meta analysis and synthesis of the evidence. Sleep 30(4):461–467. https://doi.org/10.1093/sleep/30.4.461
Ishii L, Roxbury C, Godoy A, Ishman S, Ishii M (2015) Does nasal surgery improve OSA in patients with nasal obstruction and OSA? A meta-analysis. Otolaryngol Head Neck Surg 153(3):326–333. https://doi.org/10.1177/0194599815594374
Tell GS, Crouse JR, Furberg CD (1988) Relation between blood lipids, lipoproteins, and cerebrovascular atherosclerosis. A review. Stroke 19(4):423–430. https://doi.org/10.1161/01.str.19.4.423 (PMID: 3284015)
Wilson PW, D’Agostino RB, Levy D, Belanger AM, Silbershatz H, Kannel WB (1998) Prediction of coronary heart disease using risk factor categories. Circulation 97(18):1837–1847. https://doi.org/10.1161/01.cir.97.18.1837
Ingelsson E, Schaefer EJ, Contois JH et al (2007) Clinical utility of different lipid measures for prediction of coronary heart disease in men and women. JAMA 298(7):776–785. https://doi.org/10.1001/jama.298.7.776
Jellinger PS, Smith DA, Mehta AE et al (2012) AACE task force for management of dyslipidemia and prevention of atherosclerosis. American Association of Clinical Endocrinologists’ Guidelines for management of dyslipidemia and prevention of atherosclerosis. Endocr Pract 18(Suppl 1):1–78. https://doi.org/10.4158/ep.18.s1
Gündüz C, Basoglu OK, Hedner J et al (2018) Obstructive sleep apnoea independently predicts lipid levels: data from the European Sleep Apnea Database. Respirology 23(12):1180–1189. https://doi.org/10.1111/resp.13372
Chen SY, Cherng YG, Lee FP et al (2015) Risk of cerebrovascular diseases after uvulopalatopharyngoplasty in patients with obstructive sleep apnea: a nationwide cohort study. Medicine 94(41):e1791. https://doi.org/10.1097/MD.0000000000001791
Lin MT, Lai CL, Lee PL et al (2018) Timely diagnosis and treatment of sleep apnea reduce cardiovascular sequelae in patients with myocardial infarction. PLoS ONE 13(7):e0201493. https://doi.org/10.1371/journal.pone.0201493
Funding
This study was supported by grant from Taipei Hospital, Ministry of Health and Welfare (202010 and 202011).
Author information
Authors and Affiliations
Contributions
Kang KT and Lin MT both equally participated in this study’s design and coordination and are acknowledged as co-corresponding authors. All authors read and approved the final manuscript. The authors would like to thank the editor and the anonymous reviewers for their comments.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
405_2022_7382_MOESM2_ESM.tif
Supplement figure 1 Meta-regression analyses of correlations between change in AHI and change in total cholesterol (TIF 1439 kb)
405_2022_7382_MOESM3_ESM.tif
Supplement figure 2 Meta-regression analyses of associations between change in AHI and change in low-density lipoprotein (TIF 2029 kb)
405_2022_7382_MOESM4_ESM.tif
Supplement figure 3 Meta-regression analyses of associations between change in AHI and change in high-density lipoprotein (TIF 2196 kb)
405_2022_7382_MOESM5_ESM.tif
Supplement figure 4 Meta-regression analyses of associations between change in AHI and change in triglyceride (TIF 2097 kb)
405_2022_7382_MOESM10_ESM.tif
Supplement figure 9 Forest plot showing the mean AHI change after sleep surgery (exclude isolated nasal surgery) (TIF 1226 kb)
405_2022_7382_MOESM11_ESM.tif
Supplement figure 10 Forest plot showing changes in (A) total cholesterol and (B) low-density lipoprotein (C) high-density lipoprotein (D) triglyceride after sleep surgery (exclude isolated nasal surgery) (TIF 2559 kb)
405_2022_7382_MOESM12_ESM.tif
Supplement figure 11 Forest plot comparing changes in lipid profiles in patients with mean AHI reduction < 20 vs. > 20 events/hour after surgery (exclude isolated nasal surgery) (TIF 1209 kb)
405_2022_7382_MOESM13_ESM.tif
Supplement figure 12 Meta-regression analyses of correlations between change in AHI and change in total cholesterol (exclude isolated nasal surgery) (TIF 978 kb)
405_2022_7382_MOESM14_ESM.tif
Supplement figure 13 Meta-regression analyses of associations between change in AHI and change in low-density lipoprotein (exclude isolated nasal surgery) (TIF 977 kb)
405_2022_7382_MOESM15_ESM.tif
Supplement figure 14 Meta-regression analyses of associations between change in AHI and change in high-density lipoprotein (exclude isolated nasal surgery) (TIF 1006 kb)
405_2022_7382_MOESM16_ESM.tif
Supplement figure 15 Meta-regression analyses of associations between change in AHI and change in triglyceride (exclude isolated nasal surgery) (TIF 920 kb)
Rights and permissions
About this article
Cite this article
Lee, CH., Hsu, WC., Yeh, TH. et al. Effect of sleep surgery on lipid profiles in adults with obstructive sleep apnea: a meta-analysis. Eur Arch Otorhinolaryngol 279, 3811–3820 (2022). https://doi.org/10.1007/s00405-022-07382-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-022-07382-y