Abstract
Objectives
We examined racial/ethnic differences in the association between influenza vaccine recommendations from healthcare providers and maternal vaccination uptake.
Methods
This cross-sectional study examined data from the Pregnancy Risk Assessment Monitoring System. We categorized respondents as non-Hispanic (NH) Whites, NH-Blacks, NH-Asians, American Indians/Alaska Natives, NH Other non-Whites, and Hispanics. We conducted multivariable logistical regression models to evaluate adjusted odds ratios (AOR) and 95% confidence intervals (CI). Covariates included maternal age, marital status, education, insurance status before pregnancy, the number of previous live births, the number of prenatal care visits, and smoking status during pregnancy.
Results
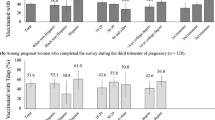
The prevalences of receiving influenza vaccine recommendations from healthcare providers and maternal vaccine were 80.01% and 50.42%, respectively. NH-Blacks are less likely to receive provider recommendations (AOR = 0.82; 95%CI 0.77–0.87) and be vaccinated (AOR = 0.76; 95%CI 0.72−0.80) than NH-Whites. Receiving provider recommendations was significantly associated with increased maternal influenza vaccine uptake (AOR = 15.50; 95% CI 14.51–16.55). The associations were significant for all racial/ethnic groups, with the highest among NH-Asians (AOR = 22.04; 95% CI 17.88−27.16) and the lowest among NH Other non-Whites (AOR = 11.07; 95% CI 8.25−14.86). Within NH-Asians, effectiveness among Chinese was highest (AOR = 29.39; 95% CI 18.10−47.71).
Conclusions
Racial/ethnic disparities in maternal influenza vaccine uptake and receiving vaccine recommendations from healthcare providers persisted. Further studies on the racial/ethnic disparities in maternal vaccination were warranted and tailored strategies are required to reduce this health disparity.



Similar content being viewed by others
Data availability
The PRAMS dataset analyzed in the current study is available from the CDC PRAMS website on request/application.
References
Sebghati M, Khalil A (2021) Uptake of vaccination in pregnancy. Best Pract Res Clin Obstet Gynaecol 76:53–65. https://doi.org/10.1016/j.bpobgyn.2021.03.007
Grohskopf LA (2016) Prevention and control of seasonal influenza with vaccines. MMWR Recomm Rep. https://doi.org/10.15585/mmwr.rr6505a1
Callahan AG, Coleman-Cowger VH, Schulkin J, Power ML (2021) Racial disparities in influenza immunization during pregnancy in the United States: A narrative review of the evidence for disparities and potential interventions. Vaccine 39:4938–4948. https://doi.org/10.1016/j.vaccine.2021.07.028
Razzaghi H, Kahn KE, Black CL et al (2020) Influenza and Tdap vaccination coverage among pregnant women—United States, April 2020. MMWR Morb Mortal Wkly Rep 69:1391–1397. https://doi.org/10.15585/mmwr.mm6939a2
Ahluwalia IB, Ding H, Harrison L et al (2014) Disparities in influenza vaccination coverage among women with live-born infants: prams surveillance during the 2009–2010 influenza season. Public Health Rep 129:408–416
Ding H, Black CL, Ball S et al (2017) Influenza vaccination coverage among pregnant women—United States, 2016–17 influenza season. MMWR Morb Mortal Wkly Rep. https://doi.org/10.15585/mmwr.mm6638a2
Lu P, Hung M-C, O’Halloran AC et al (2019) Seasonal influenza vaccination coverage trends among adult populations, U.S., 2010–2016. Am J Prev Med 57:458–469. https://doi.org/10.1016/j.amepre.2019.04.007
Barrett T, McEntee E, Drew R et al (2018) Influenza vaccination in pregnancy: vaccine uptake, maternal and healthcare providers’ knowledge and attitudes. A quantitative study. BJGP Open 2:bjgpopen18X101599. https://doi.org/10.3399/bjgpopen18X101599
Ellingson MK, Dudley MZ, Limaye RJ et al (2019) Enhancing uptake of influenza maternal vaccine. Expert Rev Vaccines 18:191–204. https://doi.org/10.1080/14760584.2019.1562907
Maher L, Hope K, Torvaldsen S et al (2013) Influenza vaccination during pregnancy: coverage rates and influencing factors in two urban districts in Sydney. Vaccine 31:5557–5564. https://doi.org/10.1016/j.vaccine.2013.08.081
Moniz MH, Hasley S, Meyn LA, Beigi RH (2013) Improving influenza vaccination rates in pregnancy through text messaging: a randomized controlled trial. Obstet Gynecol 121:734–740. https://doi.org/10.1097/AOG.0b013e31828642b1
Skirrow H, Holder B, Meinel A et al (2021) Evaluation of a midwife-led, hospital based vaccination service for pregnant women. Hum Vaccin Immunother 17:237–246. https://doi.org/10.1080/21645515.2020.1770515
Yeung MPS, Lam FLY, Coker R (2016) Factors associated with the uptake of seasonal influenza vaccination in adults: a systematic review. J Public Health. https://doi.org/10.1093/pubmed/fdv194
Frew PM, Saint-Victor DS, Owens LE, Omer SB (2014) Socioecological and message framing factors influencing maternal influenza immunization among minority women. Vaccine 32:1736–1744. https://doi.org/10.1016/j.vaccine.2014.01.030
Meharry PM, Cusson RM, Stiller R, Vázquez M (2014) Maternal influenza vaccination: evaluation of a patient-centered pamphlet designed to increase uptake in pregnancy. Matern Child Health J 18:1205–1214. https://doi.org/10.1007/s10995-013-1352-4
Ahluwalia IB, Jamieson DJ, Rasmussen SA et al (2010) Correlates of seasonal influenza vaccine coverage among pregnant women in Georgia and Rhode Island. Obstet Gynecol 116:949–955. https://doi.org/10.1097/AOG.0b013e3181f1039f
Black CL, Yue X, Ball SW et al (2015) Influenza vaccination coverage among health care personnel—United States, 2014–15 influenza season. Morb Mortal Wkly Rep 64:44. https://doi.org/10.15585/mmwr.mm6436a1
Arnold LD, Luong L, Rebmann T, Chang JJ (2019) Racial disparities in U.S. maternal influenza vaccine uptake: results from analysis of Pregnancy Risk Assessment Monitoring System (PRAMS) data, 2012–2015. Vaccine 37:2520–2526. https://doi.org/10.1016/j.vaccine.2019.02.014
Landis K, Bednarczyk RA, Gaydos LM (2018) Correlates of HPV vaccine initiation and provider recommendation among male adolescents, 2014 NIS-Teen. Vaccine 36:3498–3504. https://doi.org/10.1016/j.vaccine.2018.04.075
Ylitalo KR, Lee H, Mehta NK (2013) Health care provider recommendation, human papillomavirus vaccination, and race/ethnicity in the US national immunization survey. Am J Public Health 103:164–169. https://doi.org/10.2105/AJPH.2011.300600
Shulman HB, D’Angelo DV, Harrison L et al (2018) The pregnancy risk assessment monitoring system (PRAMS): overview of design and methodology. Am J Public Health 108:1305–1313. https://doi.org/10.2105/AJPH.2018.304563
(2023) Are PRAMS data available to researchers? | CDC. https://www.cdc.gov/prams/prams-data/researchers.htm. Accessed 13 Dec 2023
Xie S, Monteiro K, Gjelsvik A (2022) The association between adverse birth outcomes and smoking cessation during pregnancy across the United States—43 States and New York City, 2012–2017. Arch Gynecol Obstet. https://doi.org/10.1007/s00404-022-06792-x
Xie S, Monteiro K, Gjelsvik A (2023) The association between maternal influenza vaccination during pregnancy and adverse birth outcomes in the United States: pregnancy risk assessment monitoring system (PRAMS). Vaccine 41:2300–2306. https://doi.org/10.1016/j.vaccine.2023.02.074
Coleman MA, Dongarwar D, Ramirez J et al (2022) Factors impacting vaccine uptake during pregnancy: a retrospective analysis. Int J Matern Child Health AIDS (IJMA). https://doi.org/10.21106/ijma.554
Callahan AG, Strassberg ER, Rhoades CP et al (2022) Pregnant women’s opinions and acceptance of influenza and Tdap vaccines. J Women’s Health 31:656–664. https://doi.org/10.1089/jwh.2021.0365
Toth JM, Nsiah I, Nair S, Ramachandran S (2022) Association between a usual source of care and influenza vaccination rates among pregnant women. Pharmacoepidemiol Drug Saf 31:361–369. https://doi.org/10.1002/pds.5394
Healthy People 2020 (2016) IID-12.14 Data Details |. https://www.healthypeople.gov/node/6362/data_details. Accessed 27 Jul 2020
Almario CV, May FP, Maxwell AE et al (2016) Persistent racial and ethnic disparities in flu vaccination coverage: results from a population-based study. Am J Infect Control 44:1004–1009. https://doi.org/10.1016/j.ajic.2016.03.064
Brixner A, Brandstetter S, Böhmer MM et al (2021) Prevalence of and factors associated with receipt of provider recommendation for influenza vaccination and uptake of influenza vaccination during pregnancy: cross-sectional study. BMC Pregnancy Childbirth 21:723. https://doi.org/10.1186/s12884-021-04182-w
Mak TK, Mangtani P, Leese J et al (2008) Influenza vaccination in pregnancy: current evidence and selected national policies. Lancet Infect Dis 8:44–52. https://doi.org/10.1016/S1473-3099(07)70311-0
Offeddu V, Tam CC, Yong TT et al (2019) Coverage and determinants of influenza vaccine among pregnant women: a cross-sectional study. BMC Public Health 19:890. https://doi.org/10.1186/s12889-019-7172-8
Regan AK, Mak DB, Hauck YL et al (2016) Trends in seasonal influenza vaccine uptake during pregnancy in Western Australia: implications for midwives. Women Birth 29:423–429. https://doi.org/10.1016/j.wombi.2016.01.009
Strassberg ER, Power M, Schulkin J et al (2018) Patient attitudes toward influenza and tetanus, diphtheria and acellular pertussis vaccination in pregnancy. Vaccine 36:4548–4554. https://doi.org/10.1016/j.vaccine.2018.05.121
Wiley KE, Massey PD, Cooper SC et al (2013) Uptake of influenza vaccine by pregnant women: a cross-sectional survey. Med J Aust 198:373–375. https://doi.org/10.5694/mja12.11849
DiTosto JD, Weiss RE, Yee LM, Badreldin N (2021) Association of Tdap vaccine guidelines with vaccine uptake during pregnancy. PLoS ONE 16:e0254863. https://doi.org/10.1371/journal.pone.0254863
Freimuth VS, Jamison AM, An J et al (2017) Determinants of trust in the flu vaccine for African Americans and Whites. Soc Sci Med 193:70–79. https://doi.org/10.1016/j.socscimed.2017.10.001
Peters RM, Benkert R, Templin TN, Cassidy-Bushrow AE (2014) Measuring African American women’s trust in provider during pregnancy. Res Nurs Health 37:144–154. https://doi.org/10.1002/nur.21581
Henning-Smith C, Ramirez MR, Hernandez A, Hardeman R, Kozhimannil K (2019) Differences in preventive care among rural residents by race and ethnicity. Policy Brief; University of Minnesota Rural Health Research Center: Minneapolis, MN, USA. https://www.ohioruralhealth.org/upload/policy_brief_differences_in_preventive_care_among_rural_resident_by_race_and_ethnicity_original_1612471091_9651.pdf
Chan H-J, Chang J-Y, Erickson SR, Wang C-C (2019) Influenza vaccination among pregnant women in the United States: findings from the 2012–2016 national health interview survey. J Women’s Health 28:965–975. https://doi.org/10.1089/jwh.2018.7139
Chalise U, McDonald JA, Amatya A, Morales M (2020) Seasonal influenza vaccination patterns among pregnant women in New Mexico. Hisp Health Care Int 18:214–223. https://doi.org/10.1177/1540415319896254
Wang Z, Jamal A, Wang R et al (2022) Disparities and trends in routine adult vaccination rates among disaggregated Asian American subgroups, NHIS 2006–2018. AJPM Focus 2:100044. https://doi.org/10.1016/j.focus.2022.100044
Srivastav A, O’Halloran A, Lu P-J, Williams WW (2018) Influenza vaccination coverage among English-speaking Asian Americans. Am J Prev Med 55:e123–e137. https://doi.org/10.1016/j.amepre.2018.06.018
Lu AB, Halim AA, Dendle C et al (2012) Influenza vaccination uptake amongst pregnant women and maternal care providers is suboptimal. Vaccine 30:4055–4059. https://doi.org/10.1016/j.vaccine.2012.04.012
SteelFisher GK, Caporello HL, Broussard CS et al (2021) Seasonal influenza vaccine in pregnant women: views and experiences of obstetrician-gynecologists. J Women’s Health 30:1086–1094. https://doi.org/10.1089/jwh.2020.8700
Dudley MZ, Limaye RJ, Salmon DA et al (2021) Racial/Ethnic disparities in maternal vaccine knowledge, attitudes, and intentions. Public Health Rep 136:699–709. https://doi.org/10.1177/0033354920974660
Daley MF, Reifler LM, Shoup JA et al (2022) Influenza vaccination among pregnant women: self-report compared with vaccination data from electronic health records, 2018–2020 influenza seasons. Public Health Rep. https://doi.org/10.1177/00333549221099932
Acknowledgements
We thank the PRAMS Working Group (Alabama—Danita Crear, DrPH; Alaska—Kathy Perham-Hester, MS, MPH; Arkansas— Mary McGehee, PhD; Colorado—Alyson Shupe, PhD; Connecticut—Jennifer Morin, MPH; Delaware— George Yocher, MS; District of Columbia—Pamela Oandasan; Florida— Jerri Foreman, MPH; Georgia— Jenna Self, MPH; Hawaii— Emily Roberson, MPH; Illinois—Theresa Sandidge, MA; Indiana—Jenny Durica, MPH; Iowa —Sarah Mauch, MPH; Louisiana— Jane Herwehe, MPH; Maine—Tom Patenaude, MPH; Maryland—Diana Cheng, MD; Massachusetts— Emily Lu, MPH; Michigan— Cristin Larder, MS; Minnesota—Judy Punyko, PhD, MPH; Mississippi— Brenda Hughes, MPPA; Missouri—Venkata Garikapaty, MSc, MS, PhD, MPH; Montana—JoAnn Dotson; Nebraska—Brenda Coufal; New Hampshire—Paulette Valliere, MPH; New Jersey—Lakota Kruse, MD; New Mexico—Eirian Coronado, MPH; New York State—Anne Radigan-Garcia; New York City—Candace Mulready-Ward, MPH; North Carolina— Kathleen Jones-Vessey, MS; North Dakota—Sandra Anseth; Ohio—Connie Geidenberger, PhD; Oklahoma—Alicia Lincoln, MSW, MSPH; Oregon—Kenneth Rosenberg, MD, MPH; Pennsylvania—Tony Norwood; Rhode Island—Sam Viner-Brown, PhD; South Carolina—Mike Smith, MSPH; Tennessee—Angela Miller, PhD, MSPH; Texas— Rochelle Kingsley, MPH; Utah—Lynsey Gammon, MPH; Vermont—Peggy Brozicevic; Virginia—Marilyn Wenner; Washington—Linda Lohdefinck; West Virginia—Melissa Baker, MA; Wisconsin—Mireille Perzan, MPH; Wyoming—Amy Spieker, MPH; CDC PRAMS Team, Applied Sciences Branch, Division of Reproductive Health).
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
SX: project development, manuscript writing, and data analysis. AG: project development, manuscript editing, and review. KM: manuscript review.
Corresponding author
Ethics declarations
Conflicts of interest
The authors have no relevant financial or non-financial interests to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Xie, S., Monteiro, K. & Gjelsvik, A. Influenza vaccine during pregnancy, recommendations from healthcare providers, and race/ethnicity in the United States. Arch Gynecol Obstet (2024). https://doi.org/10.1007/s00404-023-07366-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00404-023-07366-1