Abstract
Background
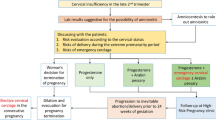
Cervical cerclage is a treatment for an incompetent cervix, the latter being a contributor to spontaneous preterm birth. There is significant difficulty with a transvaginal cerclage insertion for the absent vaginal or ecto-cervix in the mid-2nd trimester period resulting in a higher risk of late miscarriages, extremely preterm labour with increased neonatal morbidity and mortality.
Methods
A retrospective review of 5 consecutive cases managed by a surgical technique—modified high vaginal cerclage insertion at 18-20 weeks—and adjunct protocols which included vaginal progesterone use, serial infection screening and lifestyle advice, over a 12-month period ending in August 2021, is presented. Inclusion criteria included minimal or absent ecto-cervix, singleton pregnancies with an incompetent cervix attending for a vaginal cerclage whilst exclusion criteria were the usual contraindications to a cerclage insertion. Primary outcome was delivery after 34 weeks whilst seconday outcomes included maternal hemorrhage, bowel/bladder injury, chorioamnionitis and neonatal admission.
Results
A increased gestational latency of 13 gestational weeks (range 12–18). Mean gestational age at delivery was 36 weeks +1 (253 days) with a range of 241–264 days. Delivery after 34 weeks gestational age was 100% with no maternal surgical complications and corresponding neonatal outcomes.
Conclusion
There is a potential therapeutic benefit of this technique and adjunct management, in managing an incompetent mid-2nd trimester absent ecto-cervix.
Similar content being viewed by others
Data availability
No.
References
Alfirevic Z, Stampalija T, Medley N (2017) Cervical stitch (cerclage) for preventing preterm birth in singleton pregnancy. Cochrane Database Syst Rev 6:CD008991. https://doi.org/10.1002/14651858.CD008991.pub3
Owen J, Hankins G, Iams JD et al (2009) Multicenter randomized trial of cerclage for preterm birth prevention in high-risk women with shortened midtrimester cervical length. Am J Obstet Gynecol 201(4):375.e1-375.e8
Shennan A, Story L, Jacobsson B, Grobman WA, The FIGO Working Group for Preterm Birth (2021) FIGO good practice recommendations on cervical cerclage for prevention of preterm birth. Int J Gynecol Obstet 155:19–22. https://doi.org/10.1002/ijgo.13835
Namouz S, Porat S, Okun N, Windrim R, Farine D (2013) Emergency cerclage: literature review. Obstet Gynecol Surv 68(5):379–388. https://doi.org/10.1097/OGX.0b013e31828737c7
Wierzchowska-Opoka M, Kimber-Trojnar Ż, Leszczyńska-Gorzelak B (2021) Emergency cervical cerclage. J Clin Med 10(6):1270. https://doi.org/10.3390/jcm10061270
Hezelgrave NL, Watson HA, Ridout A, Diab F, Seed PT, Chin-Smith E, Tribe RM, Shennan AH (2016) Rationale and design of SuPPoRT: a multicentre randomised controlled trial to compare three treatments: cervical cerclage, cervical pessary and vaginal progesterone, for the prevention of preterm birth in women who develop a short cervix. BMC Pregnancy Childbirth 16(1):358. https://doi.org/10.1186/s12884-016-1148-9
National Institute for Health and Care Excellence (2018) IP overview: laparoscopic cerclage for cervical incompetence to prevent late miscarriage or preterm birth (NICE IP 379/2). Accessed Date 27th Dec 2021, https://www.nice.org.uk/guidance/ipg639/documents/overview-2.
Moawad GN, Tyan P, Bracke T et al (2018) Systematic review of transabdominal cerclage placed via laparoscopy for the prevention of preterm birth. J Minim Invasive Gynecol 25:277–286
Israfi-Bayli F, Toozs-Hobson P, Ismail K (2014) Cerclage outcome by the type of suture material (COTS): study protocol for a pilot and feasibility randomised controlled trial. Trials 15:415 https://doi.org/10.1186/1745-6215-15-415
Cook JR, Chatfield S, Chandiramani M et al (2017) Cerclage position, cervical length and preterm delivery in women undergoing ultrasound indicated cervical cerclage: A retrospective cohort study. PLoS ONE 12(6):e0178072
Rastogi S et al (2020) Tolerance of chlorhexidine gluconate vaginal cleansing solution: a randomized controlled trial. J Gyneco Surg 36(1):13–19
Lakhi NA, Tricorico G, Osipova Y, Moretti ML (2019) Vaginal cleansing with chlorhexidine gluconate or povidone-iodine prior to cesarean delivery: a randomized comparator-controlled trial. Am J Obstet Gynecol MFM 1(1):2–9. https://doi.org/10.1016/j.ajogmf.2019.03.004
Baumer A, Gimovsky A, Gallagher M, Leftwich MC (2019) A synthetic cervix model and the impact of softness on cerclage integrity. Interface Focus 9(5):20190009. https://doi.org/10.1098/rsfs.2019.0009
Nicolaides KH, Syngelaki A, Poon LC et al (2016) A randomized trial of a cervical pessary to prevent preterm singleton birth. N Engl J Med 374:1044–1052
Dugoff L, Berghella V, Sehdev H, Mackeen AD, Goetzl L, Ludmir J (2018) Prevention of preterm birth with pessary in singletons (PoPPS): randomized controlled trial. Ultrasound Obstet Gynecol 51:573–579. https://doi.org/10.1002/uog.18908
Norman JE, Marlow N, Messow CM, OPPTIMUM study group et al (2016) Vaginal progesterone prophylaxis for preterm birth (the OPPTIMUM study): a multicentre, randomised, double-blind trial. Lancet 387:2106–2116
Jarde A, Lutsiv O, Beyene J, McDonald SD (2018) Vaginal progesterone, oral progesterone, 17-OHPC, cerclage, and pessary for preventing preterm birth in at-risk singleton pregnancies: an updated systematic review and network meta-analysis. BJOG. https://doi.org/10.1111/1471-0528.15566
EPPPIC Group (2021) Evaluating Progestogens for Preventing Preterm birth International Collaborative (EPPPIC): meta-analysis of individual participant data from randomised controlled trials. Lancet 397:1183–1194. https://doi.org/10.1016/S0140-6736(21)00217-8
Enakpene CA, DiGiovanni L, Jones TN, Marshalla M, Mastrogiannis D, Della TM (2018) Cervical cerclage for singleton pregnant patients on vaginal progesterone with progressive cervical shortening. Am J Obstet Gynecol 219(4):397.e1-397.e10. https://doi.org/10.1016/j.ajog.2018.06.020 (Epub 2018 Jul 11 PMID: 30017683)
Lavie M, Shamir-Kaholi N, Lavie I et al (2020) Outcomes of ultrasound and physical-exam based cerclage: assessment of risk factors and the role of adjunctive progesterone in preventing preterm birth—a retrospective cohort study. Arch Gynecol Obstet 301:981–986. https://doi.org/10.1007/s00404-020-05482-w
Sosa CG, Althabe F, Belizán JM, Bergel E (2015) Bed rest in singleton pregnancies for preventing preterm birth. Cochrane Database Syst Rev 3:CD003581. https://doi.org/10.1002/14651858.CD003581.pub3 (PMID: 25821121; PMCID: PMC7144825)
Critchfield AS, Yao G, Jaishankar A, Friedlander RS, Lieleg O et al (2013) Cervical mucus properties stratify risk for preterm birth. PLoS ONE 8(8):e69528. https://doi.org/10.1371/journal.pone.0069528
Son M, Miller ES (2017) Predicting preterm birth: cervical length and fetal fibronectin. Semin Perinatol 41(8):445–451. https://doi.org/10.1053/j.semperi.2017.08.002
Goldenburg RL, Mercer BM, Meis PJ, Copper RL, Das A, McNellis D (1996) The preterm prediction study: fetal fibronectin testing and spontaneous preterm birth. NICHD Maternal Fetal Medicine Units Network. Obstet Gynecol 87(5 Pt 1):643–648
Krispin E, Danieli-Gruber S, Hadar E et al (2019) Primary, secondary, and tertiary preventions of preterm birth with cervical cerclage. Arch Gynecol Obstet 300:305–312. https://doi.org/10.1007/s00404-019-05184-y
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
TOA—Study design, Data collection and Manuscript writing. AAA—manuscript writing. UOC—manuscript writing.
Corresponding author
Ethics declarations
Conflict of interest
There are no financial interests to declare.
Ethics approval
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Adedipe, T.O., Akintunde, A.A. & Chukwujama, U.O. Management of an incompetent mid-second (mid-2nd) trimester absent ecto-cervix: a case series. Cervical amplification pre-cerclage insertion. Arch Gynecol Obstet 306, 969–975 (2022). https://doi.org/10.1007/s00404-022-06694-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-022-06694-y