Abstract
Background
Patients with a poor ovarian response (POR) represent the most difficult group of population to deal with in the clinical fertility practice. Bologna criteria are the first uniform definition of POR. Choosing a suitable controlled ovarian stimulation (COS) protocol which could give adequate oocytes to maximize the chance of obtaining at least one euploid blastocyst is crucial in the management for such patients. The delayed start antagonist protocol is a novel COS protocol designed for POR patients, however, its real efficacy is controversial compared to conventional protocols. The present study aims to summarize all available studies on this topic and perform a meta-analysis to explore the real treatment effect of this novel protocol in terms of reproductive outcomes.
Study design
PubMed, EMBASE, Google Scholar, and the Cochrane Library from database establishment to June 2019 were searched. Randomized controlled trials (RCTs), which compared delayed start antagonist protocol (Del) to conventional controlled ovarian stimulation (COS) protocols (Con) in terms of reproductive outcomes, were included. The RevMan 5.3 was used to perform statistical analysis. The primary outcomes were the cycle cancellation rate, the clinical pregnancy rate and the miscarriage rate.
Results
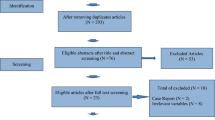
5 RCTs yielding 514 patients were eligible, of which 5, 5, 4 studies were included in analyzing the cycle cancellation rate, the clinical pregnancy rate, and the miscarriage rate respectively. Synthesized data of meta-analysis showed: delayed start antagonist protocol introduced a lower risk of cycle cancellation [risk ratio (RR) = 0.63, 95% confidence interval (CI) (0.45, 0.90), P = 0.01; 5 RCTs, 514 women (Del:Con = 256:258); I2 = 0%; with rates of 16.02% (Del) vs. 26.36% (Con)], an increased chance to get clinical pregnancy [RR = 2.30, 95% CI (1.38, 3.82), P = 0.001; 5 RCTs, 514 women (Del:Con = 256:258); I2 = 0%; with rates of 16.80% (Del) vs. 7.36% (Con)], and a comparable miscarriage rate [RR = 0.55, 95% CI (0.24, 1.23), P = 0.15; 4 RCTs, 58 women (Del:Con = 41:17) I2 = 17%; with rates of 19.51% (Del) vs. 35.29% (Con)] compared to conventional COS protocols.
Conclusions
Delayed start antagonist protocol was a potentially valuable alternation for poor ovarian responders. However, future RCTs with large sample size and more scientific design are needed to verify its validity and draw a sound conclusion.






Similar content being viewed by others
Availability of data and materials
All data generated or analysed during this study are included in this published article.
References
NS M, Stouffer Rl Fau—Giudice LC, Giudice Lc Fau— Fauser BCJM et al (2006) The science behind 25 years of ovarian stimulation for in vitro fertilization. Endocr Rev 27(2):170–207
Garcia JE, Jones GS, Acosta AA et al (1983) Human menopausal gonadotropin/human chorionic gonadotropin follicular maturation for oocyte aspiration: phase II, 1981. Fertil Steril 39(2):174–179
Polyzos NP, Devroey P (2011) A systematic review of randomized trials for the treatment of poor ovarian responders: is there any light at the end of the tunnel? Fertil Steril 96(5):1058-1061.e1057
Ferraretti AP, La Marca A, Fauser BC et al (2011) ESHRE consensus on the definition of “poor response” to ovarian stimulation for in vitro fertilization: the Bologna criteria. Hum Reprod (Oxf, Engl) 26(7):1616–1624
Alviggi C, Andersen CY, Buehler K et al (2016) A new more detailed stratification of low responders to ovarian stimulation: from a poor ovarian response to a low prognosis concept. Fertil Steril 105(6):1452–1453
Papathanasiou A (2014) Implementing the ESHRE “poor responder” criteria in research studies: methodological implications. Hum Reprod (Oxf, Engl) 29(9):1835–1838
Vaiarelli A, Cimadomo D, Ubaldi N et al (2018) What is new in the management of poor ovarian response in IVF? Curr Opin Obstet Gynecol 30(3):155–162
Patrizio P, Vaiarelli A, Levi Setti PE et al (2015) How to define, diagnose and treat poor responders? Responses from a worldwide survey of IVF clinics. Reprod Biomed Online 30(6):581–592
Polyzos NP, Nwoye M, Corona R et al (2014) Live birth rates in Bologna poor responders treated with ovarian stimulation for IVF/ICSI. Reprod Biomed Online 28(4):469–474
La Marca A, Grisendi V, Giulini S et al (2015) Live birth rates in the different combinations of the Bologna criteria poor ovarian responders: a validation study. J Assist Reprod Genet 32(6):931–937
Busnelli A, Papaleo E, Del Prato D et al (2015) A retrospective evaluation of prognosis and cost-effectiveness of IVF in poor responders according to the Bologna criteria. Hum Reprod (Oxf, Engl) 30(2):315–322
Cakmak H, Tran ND, Zamah AM et al (2014) A novel “delayed start” protocol with gonadotropin-releasing hormone antagonist improves outcomes in poor responders. Fertil Steril 101(5):1308–1314
Cozzolino M, Franasiak J, Andrisani A et al (2020) “Delayed start” gonadotropin-releasing hormone antagonist protocol in Bologna poor-responders: a systematic review and meta-analysis of randomized controlled trials. Eur J Obstet Gynecol Reprod Biol 244:154–162
Park CW, Hwang YI, Koo HS et al (2014) Early gonadotropin-releasing hormone antagonist start improves follicular synchronization and pregnancy outcome as compared to the conventional antagonist protocol. Clin Exp Reprod Med 41(4):158–164
Elassar A, Mann JS, Engmann L et al (2011) Luteal phase estradiol versus luteal phase estradiol and antagonist protocol for controlled ovarian stimulation before in vitro fertilization in poor responders. Fertil Steril 95(1):324–326
Eftekhar M, Bagheri RB, Neghab N et al (2018) Evaluation of pretreatment with Cetrotide in an antagonist protocol for patients with PCOS undergoing IVF/ICSI cycles: a randomized clinical trial. JBRA Assist Reprod 22(3):238–243
Shin JJ, Park KE, Choi YM et al (2018) Early gonadotropin-releasing hormone antagonist protocol in women with polycystic ovary syndrome: a preliminary randomized trial. Clin Exp Reprod Med 45(3):135–142
Blockeel C, Riva A, De Vos M et al (2011) Administration of a gonadotropin-releasing hormone antagonist during the 3 days before the initiation of the in vitro fertilization/intracytoplasmic sperm injection treatment cycle: impact on ovarian stimulation. A pilot study. Fertil Steril. 95(5):1714–1719
Younis JS, Soltsman S, Izhaki I et al (2010) Early and short follicular gonadotropin-releasing hormone antagonist supplementation improves the meiotic status and competence of retrieved oocytes in in vitro fertilization-embryo transfer cycles. Fertil Steril 94(4):1350–1355
Frankfurter D, Dayal M, Dubey A et al (2007) Novel follicular-phase gonadotropin-releasing hormone antagonist stimulation protocol for in vitro fertilization in the poor responder. Fertil Steril 88(5):1442–1445
Papanikolaou EG, Yarali H, Timotheou E et al (2018) A Proof-of-concept clinical trial of a single luteal use of long-acting gonadotropin-releasing hormone antagonist degarelix in controlled ovarian stimulation for in vitro fertilization: long antagonist protocol. Front Endocrinol (Lausanne) 9:25
Maged AM, Nada AM, Abohamila F et al (2015) Delayed start versus conventional gnrh antagonist protocol in poor responders pretreated with estradiol in luteal phase: a randomized controlled trial. Reprod Sci 22(12):1627–1631
Zarei A, Parsanezhad ME, Kutenaei MA et al (2018) Delayed start protocol with gonadotropin-releasing hormone antagonist in poor responders undergoing in vitro fertilization: a randomized, double-blinded, clinical trial. Oman Med J 33(6):506–511
Aflatoonian A, Hosseinisadat A, Baradaran R et al (2017) Pregnancy outcome of “delayed start” GnRH antagonist protocol versus GnRH antagonist protocol in poor responders: a clinical trial study. Int J Reprod Biomed 15(4):231–238
Ashrafi M, Arabipoor A, Yahyaei A et al (2018) Does the “delayed start” protocol with gonadotropin-releasing hormone antagonist improve the pregnancy outcome in Bologna poor responders? a randomized clinical trial. Reprod Biol Endocrinol 16(1):124
Davar R, Neghab N, Naghshineh E (2018) Pregnancy outcome in delayed start antagonist versus microdose flare GnRH agonist protocol in poor responders undergoing IVF/ICSI: an RCT. Int J Reprod Biomed 16(4):255–260
Oudendijk JF, Yarde F, Eijkemans MJ et al (2012) The poor responder in IVF: is the prognosis always poor?: a systematic review. Hum Reprod Update 18(1):1–11
Fauser BC, Van Heusden AM (1997) Manipulation of human ovarian function: physiological concepts and clinical consequences. Endocr Rev 18(1):71–106
De Sutter P, Dhont M (2003) Poor response after hormonal stimulation for in vitro fertilization is not related to ovarian aging. Fertil Steril 79(6):1294–1298
McGee EA, Hsueh AJ (2000) Initial and cyclic recruitment of ovarian follicles. Endocr Rev 21(2):200–214
Baerwald AR, Adams GP, Pierson RA (2012) Ovarian antral folliculogenesis during the human menstrual cycle: a review. Hum Reprod Update 18(1):73–91
Klein NA, Battaglia DE, Fujimoto VY et al (1996) Reproductive aging: accelerated ovarian follicular development associated with a monotropic follicle-stimulating hormone rise in normal older women. J Clin Endocrinol Metabol 81(3):1038–1045
Roseff SJ, Bangah ML, Kettel LM et al (1989) Dynamic changes in circulating inhibin levels during the luteal-follicular transition of the human menstrual cycle. J Clin Endocrinol Metabol 69(5):1033–1039
Humaidan P, Bungum L, Bungum M et al (2005) Reproductive outcome using a GnRH antagonist (cetrorelix) for luteolysis and follicular synchronization in poor responder IVF/ICSI patients treated with a flexible GnRH antagonist protocol. Reprod Biomed Online 11(6):679–684
Santos MA, Kuijk EW, Macklon NS (2010) The impact of ovarian stimulation for IVF on the developing embryo. Reproduction 139(1):23–34
Katz-Jaffe MG, Trounson AO, Cram DS (2005) Chromosome 21 mosaic human preimplantation embryos predominantly arise from diploid conceptions. Fertil Steril 84(3):634–643
Baart EB, Martini E, Eijkemans MJ et al (2007) Milder ovarian stimulation for in-vitro fertilization reduces aneuploidy in the human preimplantation embryo: a randomized controlled trial. Hum Reprod (Oxf, Engl) 22(4):980–988
Baker VL, Brown MB, Luke B et al (2015) Gonadotropin dose is negatively correlated with live birth rate: analysis of more than 650,000 assisted reproductive technology cycles. Fertil Steril. 104(5):1145–1152
Heger A, Sator M, Pietrowski D (2012) Endometrial Receptivity And Its Predictive Value for IVF/ICSI-outcome. Geburtshilfe Frauenheilkd 72(8):710–715
Fang R, Cai L, Xiong F et al (2016) The effect of endometrial thickness on the day of hCG administration on pregnancy outcome in the first fresh IVF/ICSI cycle. Gynecol Endocrinol 32(6):473–476
Zhao J, Zhang Q, Wang Y et al (2014) Endometrial pattern, thickness and growth in predicting pregnancy outcome following 3319 IVF cycle. Reprod Biomed Online 29(3):291–298
Al-Ghamdi A, Coskun S, Al-Hassan S et al (2008) The correlation between endometrial thickness and outcome of in vitro fertilization and embryo transfer (IVF-ET) outcome. Reprod Biol Endocrinol 6:37
Wu Y, Gao X, Lu X et al (2014) Endometrial thickness affects the outcome of in vitro fertilization and embryo transfer in normal responders after GnRH antagonist administration. Reprod Biol Endocrinol 12:96
Papathanasiou A, Searle BJ, King NM et al (2016) Trends in “poor responder” research: lessons learned from RCTs in assisted conception. Hum Reprod Update 22(3):306–319
Humaidan P, Alviggi C, Fischer R et al (2016) The novel POSEIDON stratification of “Low prognosis patients in Assisted Reproductive Technology” and its proposed marker of successful outcome. F1000Research 5:2911
Leijdekkers JA, Eijkemans MJC, van Tilborg TC et al (2019) Cumulative live birth rates in low-prognosis women. Hum Reprod (Oxf, Engl) 34(6):1030–1041
Li Y, Li X, Yang X et al (2019) Cumulative live birth rates in low prognosis patients according to the POSEIDON criteria: an analysis of 26,697 cycles of in vitro fertilization/intracytoplasmic sperm injection. Front Endocrinol (Lausanne) 10:642
Funding
The authors was funded by the National Natural Science Foundation of China (http://www.nsfc.gov.cn/) (Grant no. 81571441).
Author information
Authors and Affiliations
Contributions
YS contributed to the study design and acquisition of data, article drafting and revising as well as organization of the final approval of the version to be published. ZL contributed substantially to the interpretation of the data and helped with drafting and revision of the article. LNH and LYP contributed to conception and design, acquisition of data and analysis and interpretation of data. ZL and YRX contributed significantly to the acquisition, analysis and interpretation of the data. LNH and LYP helped with revision of the article. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Yang, S., Liu, N., Li, Y. et al. Efficacy of the delayed start antagonist protocol for controlled ovarian stimulation in Bologna poor ovarian responders: a systematic review and meta-analysis. Arch Gynecol Obstet 303, 347–362 (2021). https://doi.org/10.1007/s00404-020-05894-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-020-05894-8