Abstract
Introduction
In hip osteoarthritis, hip flexion contracture can severely alter the patient’s alignment, and, therefore, affect the patient’s quality of life (QOL). Hip contracture is not well-studied, partly because of the difficulties of its diagnosis. The aim of this study was to propose a quantitative definition of hip flexion contracture, and to analyse sagittal alignment in these patients compared to non-contracture ones, before and 12 months after total hip arthroplasty (THA).
Materials and methods
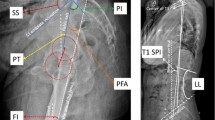
Consecutive patients with hip arthrosis and an indication for THA were included (N = 123). Sagittal full-body radiographs were acquired in free standing position and in extension. QOL questionnaires were administered before and after surgery. Spinopelvic parameters were measured, including the pelvic–femur angle (PFA). Patients with low pelvic incidence (< 45°) were included in the hip contracture group if PFA > 5°, or PFA > -5° when pelvic incidence ≥ 45°.
Results
29% of patients were in the hip flexion contracture group, and they showed lower pelvic tilt than the no-contracture group (p < 0.001), larger lumbar lordosis (LL) and smaller PI-LL (p < 0.001), as well as a forward position of the head. 16% of patients still had hip contracture 12-months postop. Contracture patients showed higher QOL scores after surgery.
Conclusions
The proposed method to diagnose hip contracture group allowed to define a group of patients who showed a specific pattern of sagittal spinopelvic alignment. These patients improved their alignment and quality of life postoperatively, but their hip mobility was not always restored. Diagnosing these patients is a first step toward the development of more specific surgical approaches, aiming to improve their surgical outcome.






Similar content being viewed by others
Availability of data and materials
Data are available on an as-requested basis.
References
Buckland AJ, Steinmetz L, Zhou P et al (2019) Spinopelvic compensatory mechanisms for reduced hip motion (ROM) in the setting of hip osteoarthritis. Spine Deform 7:923–928. https://doi.org/10.1016/j.jspd.2019.03.007
Weng W-J, Wang W-J, Wu M-D et al (2015) Characteristics of sagittal spine–pelvis–leg alignment in patients with severe hip osteoarthritis. Eur Spine J 24:1228–1236. https://doi.org/10.1007/s00586-014-3700-5
Kim Y, Pour AE, Lazennec JY (2020) How do global sagittal alignment and posture change after total hip arthroplasty? Int Orthop 44:267–273. https://doi.org/10.1007/s00264-019-04363-5
Steultjens MPM, Dekker J, Van Baar ME et al (2000) Range of joint motion and disability in patients with osteoarthritis of the knee or hip. Rheumatology 39:955–961. https://doi.org/10.1093/rheumatology/39.9.955
Tateuchi H, Akiyama H, Goto K et al (2018) Sagittal alignment and mobility of the thoracolumbar spine are associated with radiographic progression of secondary hip osteoarthritis. Osteoarthr Cartil 26:397–404. https://doi.org/10.1016/j.joca.2017.12.005
Gautam D, Malhotra R (2019) Total hip arthroplasty in ankylosing spondylitis with extension contracture of hips. J Arthroplasty 34:71–76. https://doi.org/10.1016/j.arth.2018.08.025
Dwosh IL, Resnick D, Becker MA (1976) Hip involvement in ankylosing spondylitis. Arthritis Rheum 19:683–692. https://doi.org/10.1002/1529-0131(197607/08)19:4%3c683::AID-ART1780190405%3e3.0.CO;2-8
Lee K, Chung C, Kwon D et al (2011) Reliability of physical examination in the measurement of hip flexion contracture and correlation with gait parameters in cerebral palsy. J Bone Jt Surg Am 93:150–215. https://doi.org/10.2106/JBJSJ.00252
Lamartina C, Berjano P (2014) Classification of sagittal imbalance based on spinal alignment and compensatory mechanisms. Eur Spine J 23:1177–1189. https://doi.org/10.1007/s00586-014-3227-9
Peeler J, Anderson JE (2007) Reliability of the Thomas test for assessing range of motion about the hip. Phys Ther Sport 8:14–21. https://doi.org/10.1016/j.ptsp.2006.09.023
Lazennec JY, Brusson A, Rousseau MA (2013) Lumbar-pelvic-femoral balance on sitting and standing lateral radiographs. Orthop Traumatol Surg Res 99:S87–S103. https://doi.org/10.1016/j.otsr.2012.12.003
Kim G-M, Ha S-M (2015) Reliability of the modified Thomas test using a lumbo-plevic stabilization. J Phys Ther Sci 27:447–449. https://doi.org/10.1589/jpts.27.447
Protopsaltis T, Schwab F, Bronsard N et al (2014) The T1 pelvic angle, a novel radiographic measure of global sagittal deformity, accounts for both spinal inclination and pelvic tilt and correlates with health-related quality of life. JBJS 96:1631–1640
Amabile C, Pillet H, Lafage V et al (2016) A new quasi-invariant parameter characterizing the postural alignment of young asymptomatic adults. Eur Spine J 25:3666–3674. https://doi.org/10.1007/s00586-016-4552-y
Matsumoto T, Kaneuji A, Hiejima Y et al (2012) Japanese Orthopaedic Association Hip Disease Evaluation Questionnaire (JHEQ): a patient-based evaluation tool for hip-joint disease. The subcommittee on hip disease evaluation of the clinical outcome committee of the Japanese Orthopaedic Association. J Orthop Sci 17:25–38. https://doi.org/10.1007/s00776-011-0166-8
Erdfelder E, Faul F, Buchner A (1996) GPOWER: a general power analysis program. Behav Res Methods Instrum Comput 28:1–11. https://doi.org/10.3758/BF03203630
Vialle R, Levassor N, Rillardon L et al (2005) Radiographic analysis of the sagittal alignment and balance of the spine in asymptomatic subjects. J Bone Jt Surg 87:260–267. https://doi.org/10.2106/JBJS.D.02043
Watanabe N, Murakami S, Uchida S et al (2020) Validity of the Japanese orthopaedic association hip disease evaluation questionnaire (JHEQ) for Japanese patients with labral tear. J Hip Preserv Surg 7:466–473. https://doi.org/10.1093/jhps/hnaa038
Seki T, Ishiguro N, Hasegawa Y et al (2013) Reliability and validity of the Japanese Orthopaedic Association hip disease evaluation questionnaire (JHEQ) for patients with hip disease. J Orthop Sci 18:782–787. https://doi.org/10.1007/s00776-013-0436-8
Ochi H, Homma Y, Baba T et al (2017) Sagittal spinopelvic alignment predicts hip function after total hip arthroplasty. Gait Posture 52:293–300. https://doi.org/10.1016/j.gaitpost.2016.12.010
Eftekhary N, Shimmin A, Lazennec JY et al (2019) A systematic approach to the hip-spine relationship and its applications to total hip arthroplasty. Bone Joint J-B 101:808–816. https://doi.org/10.1302/0301-620X.101B7.BJJ-2018-1188.R1
Amabile C, Le Huec J-C, Skalli W (2018) Invariance of head-pelvis alignment and compensatory mechanisms for asymptomatic adults older than 49 years. Eur Spine J 27:458–466. https://doi.org/10.1007/s00586-016-4830-8
Bassani T, Galbusera F, Luca A et al (2019) Physiological variations in the sagittal spine alignment in an asymptomatic elderly population. Spine J 19:1840–1849. https://doi.org/10.1016/j.spinee.2019.07.016
McKnight BM, Trasolini NA, Dorr LD (2019) Spinopelvic motion and impingement in total hip arthroplasty. J Arthroplasty 34:S53–S56. https://doi.org/10.1016/j.arth.2019.01.033
Philippot R, Wegrzyn J, Farizon F, Fessy MH (2009) Pelvic balance in sagittal and Lewinnek reference planes in the standing, supine and sitting positions. Orthop Traumatol Surg Res 95:70–76. https://doi.org/10.1016/j.otsr.2008.01.001
Kim Y, Vergari C, Girinon F et al (2019) Stand-to-sit kinematics of the pelvis is not always as expected: hip and spine pathologies can have an impact. J Arthroplasty. https://doi.org/10.1016/j.arth.2019.04.059
Lazennec J-Y, Charlot N, Gorin M et al (2004) Hip-spine relationship: a radio-anatomical study for optimization in acetabular cup positioning. Surg Radiol Anat 26:136–144. https://doi.org/10.1007/s00276-003-0195-x
Stefl M, Lundergan W, Heckmann N et al (2017) Hip arthroplasty: Avoiding and managing problems spinopelvic mobility and acetabular component position for total hip arthroplasty. Bone Joint J 99B:37–45
Acknowledgements
The authors are grateful to the Japan Society for the Promotion of Science for funding, and to Ms. Yasuda Hisayo for her technical support.
Funding
The study was funded by the Japan Society for the Promotion of Science trough an invitational fellowship grant (S21026). The study sponsor had no role in study design, collection, analysis and interpretation of data; in the writing of the manuscript; or in the decision to submit the manuscript for publication.
Author information
Authors and Affiliations
Contributions
CV: concept and design, obtaining of funding, analysis and interpretation of the data, drafting of the article, and final approval of the article. CV was the main investigator of this study, and performed all of the measurements. YK: provision of study patients, obtaining of funding, collection, analysis and interpretation of data, participation in the reproducibility study, critical revision of the article for important intellectual content and final approval of the article. MT: concept and design, analysis and interpretation of data, critical revision of the article for important intellectual content, and final approval of the article. YS: provision of study patients, analysis and interpretation of data, critical revision of the article for important intellectual content, and final approval of the article. CT: provision of study patients, analysis and interpretation of data, critical revision of the article for important intellectual content, and final approval of the article. SF: provision of study patients, analysis and interpretation of data, critical revision of the article for important intellectual content, and final approval of the article. SF: provision of study patients, analysis and interpretation of data, critical revision of the article for important intellectual content, and final approval of the article. SM: concept and design, obtaining of funding, analysis and interpretation of data, critical revision of the article for important intellectual content, and final approval of the article.
Corresponding author
Ethics declarations
Conflict of interest
There are no conflicts of interest to declare.
Research involving Human Participants
Institutional review board approved the data collection (authorization N. 621).
Informed consent
Patients informed consent was collected.
Consent to publish
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Vergari, C., Kim, Y., Takemoto, M. et al. Sagittal alignment in patients with flexion contracture of the hip before and after total hip arthroplasty. Arch Orthop Trauma Surg 143, 3587–3596 (2023). https://doi.org/10.1007/s00402-022-04606-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-022-04606-y