Abstract
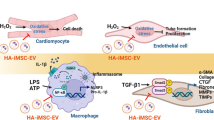
Self-assembling heart-derived stem cell clusters named cardiospheres (CSps) improve function and attenuate remodeling in rodent models of acute myocardial infarction. The effects of CSps in chronically remodeled myocardium post-MI, and the underlying mechanisms, remain unknown. One month after permanent coronary ligation, rats were randomly assigned to injection of vehicle (controls) or CSps in the peri-infarct area. One month post-injection, CSps increased left ventricular function, reduced scar mass and collagen density, and enhanced vascularity within the infarct zone compared to controls. Immunoblots revealed Tgfβ-1/smad cascade downregulation and an increase in soluble endoglin post-CSp injection. Six months post-transplantation, left ventricular function further improved and cardiomyocyte hypertrophy was attenuated in the CSp-treated group. In vitro, co-culture of CSps with fibroblasts recapitulated the suppression of the Tgf-β1/smad pathway changes, responses which were blunted by neutralizing antibody against endoglin. Thus, cardiosphere transplantation enhances angiogenesis and reduces fibrosis in chronically infarcted myocardium, leading to partial reversal of cardiac dysfunction. The underlying mechanism involves inhibition of Tgf-β1/smad signaling by CSp-secreted soluble endoglin.







Similar content being viewed by others
References
Behfar A, Crespo-Diaz R, Terzic A, Gersh BJ (2014) Cell therapy for cardiac repair—lessons from clinical trials. Nat Rev Cardiol 11:232–246. doi:10.1038/nrcardio.2014.9
Chimenti I, Smith RR, Li TS, Gerstenblith G, Messina E, Giacomello A, Marbán E (2010) Relative roles of direct regeneration versus paracrine effects of human cardiosphere-derived cells transplanted into infarcted mice. Circ Res 106:971–980. doi:10.1161/CIRCRESAHA.109.210682
Derynck R, Zhang YE (2003) Smad-dependent and Smad-independent pathways in TGF-beta family signalling. Nature 425:577–584. doi:10.1038/nature02006
Frangogiannis NG (2012) Regulation of the inflammatory response in cardiac repair. Circ Res 110:159–173. doi:10.1161/CIRCRESAHA.111.243162
Frey N, Olson EN (2003) Cardiac hypertrophy: the good, the bad, and the ugly. Annu Rev Physiol 65:45–79. doi:10.1146/annurev.physiol.65.092101.142243
Fujiu K, Nagai R (2013) Contributions of cardiomyocyte-cardiac fibroblast-immune cell interactions in heart failure development. Basic Res Cardiol 108:357. doi:10.1007/s00395-013-0357
Hein S, Arnon E, Kostin S, Schönburg M, Elsässer A, Polyakova V, Bauer EP, Klövekorn WP, Schaper J (2003) Progression from compensated hypertrophy to failure in the pressure-overloaded human heart: structural deterioration and compensatory mechanisms. Circulation 107:984–991. doi:10.1161/01.CIR.0000051865.66123.B7
Heusch G, Libby P, Gersh B, Yellon D, Bohm M, Lopaschuk G, Opie L (2014) Cardiovascular remodelling in coronary artery disease and heart failure. Lancet 383:1933–1943. doi:10.1016/S0140-6736(14)60107-0
Jeevanantham V, Butler M, Saad A, Abdel-Latif A, Zuba-Surma EK, Dawn B (2012) Adult bone marrow cell therapy improves survival and induces long-term improvement in cardiac parameters: a systematic review and meta-analysis. Circulation 126:551–568. doi:10.1161/CIRCULATIONAHA.111.086074
Johnston PV, Sasano T, Mills K, Evers R, Lee ST, Smith RR, Lardo AC, Lai S, Steenbergen C, Gerstenblith G, Lange R, Marbán E (2009) Engraftment, differentiation, and functional benefits of autologous cardiosphere-derived cells in porcine ischemic cardiomyopathy. Circulation 120:075–083. doi:10.1161/CIRCULATIONAHA.108.816058
Kakkar R, Lee RT (2010) Intramyocardial fibroblast myocyte communication. Circ Res 106:47–57. doi:10.1161/CIRCRESAHA.109.207456
Kapur NK, Wilson S, Yunis AA, Qiao X, Mackey E, Paruchuri V, Baker C, Aronovitz MJ, Karumanchi SA, Letarte M, Kass DA, Mendelsohn ME, Karas RH (2012) Reduced endoglin activity limits cardiac fibrosis and improves survival in heart failure. Circulation 125:2728–2738. doi:10.1161/CIRCULATIONAHA.111.080002
Koitabashi N, Danner T, Zaiman AL, Pinto YM, Rowell J, Mankowski J, Zhang D, Nakamura T, Takimoto E, Kass DA (2011) Pivotal role of cardiomyocyte TGF-β signaling in the murine pathological response to sustained pressure overload. J Clin Invest 121:2301–2312. doi:10.1172/JCI44824
Laflamme MA, Murry CE (2011) Heart regeneration. Nature 473:326–335. doi:10.1038/nature10147
Leask A (2010) Potential therapeutic targets for cardiac fibrosis: TGF beta, angiotensin, endothelin, CCN2, and PDGF, partners in fibroblast activation. Circ Res 106:1675–1680. doi:10.1161/CIRCRESAHA.110.217737
Li DY, Sorensen LK, Brooke BS, Urness LD, Davis EC, Taylor DG, Boak BB, Wendel DP (1999) Defective angiogenesis in mice lacking endoglin. Science 284:1534–1537. doi:10.1126/science.284.5419.1534
Li TS, Cheng K, Lee ST, Matsushita S, Davis D, Malliaras K, Zhang Y, Matsushita N, Smith RR, Marbán E (2010) Cardiospheres recapitulate a niche-like microenvironment rich in stemness and cell-matrix interactions, rationalizing their enhanced functional potency for myocardial repair. Stem Cells 28:2088–2098. doi:10.1002/stem.532
Makkar RR, Smith RR, Cheng K, Malliaras K, Thomson LE, Berman D, Czer LS, Marbán L, Mendizabal A, Johnston PV, Russell SD, Schuleri KH, Lardo AC, Gerstenblith G, Marbán E (2012) Intracoronary cardiosphere-derived cells for heart regeneration after myocardial infarction (CADUCEUS): a prospective, randomised phase 1 trial. Lancet 379:895–904. doi:10.1016/S0140-6736(12)60195-0
Malliaras K, Smith RR, Kanazawa H, Yee K, Seinfeld J, Tseliou E, Dawkins JF, Kreke M, Cheng K, Luthringer D, Ho CS, Blusztajn A, Valle I, Chowdhury S, Makkar RR, Dharmakumar R, Li D, Marbán L, Marbán E (2013) Validation of contrast-enhanced MRI to monitor regenerative efficacy after cell therapy in a porcine model of convalescent myocardial infarction. Circulation 128:2764–2775. doi:10.1161/CIRCULATIONAHA.113.002863
McAllister KA, Grogg KM, Johnson DW, Gallione CJ, Baldwin MA, Jackson CE, Helmbold EA, Markel DS, McKinnon WC, Murrell J (1994) Endoglin, a TGF-beta binding protein of endothelial cells, is the gene for hereditary haemorrhagic telangiectasia type 1. Nat Genet 8:345–351. doi:10.1038/ng1294-345
Messina E, De Angelis L, Frati G, Morrone S, Chimenti S, Fiordaliso F, Salio M, Battaglia M, Latronico MV, Coletta M, Vivarelli E, Frati L, Cossu G, Giacomello A (2004) Isolation and expansion of adult cardiac stem cells from human and murine heart. Circ Res 95:911–921. doi:10.1161/01.RES.0000147315.71699.51
Mudd JO, Kass DA (2008) Tackling heart failure in the twenty-first century. Nature 451:919–928. doi:10.1038/nature06798
Nam YJ, Song K, Luo X, Daniel E, Lambeth K, West K, Hill JA, DiMaio JM, Baker LA, Bassel-Duby R, Olson EN (2013) Reprogramming of human fibroblasts toward a cardiac fate. Proc Natl Acad Sci USA 110:5588–5593. doi:10.1073/pnas.1301019110
Nurzynska D, Di Meglio F, Romano V, Miraglia R, Sacco AM, Latino F, Bancone C, Della Corte A, Maiello C, Amarelli C, Montagnani S, Castaldo C (2013) Cardiac primitive cells become committed to a cardiac fate in adult human heart with chronic ischemic disease but fail to acquire mature phenotype: genetic and phenotypic study. Basic Res Cardiol 108:320. doi:10.1007/s00395-012-0320-2
Opie LH, Commerford PJ, Gersh BJ, Pfeffer MA (2006) Controversies in ventricular remodelling. Lancet 367:356–367. doi:10.1016/S0140-6736(06)68074-4
Papait R, Greco C, Kunderfranco P, Latronico MV, Condorelli G (2013) Epigenetics: a new mechanism of regulation of heart failure? Basic Res Cardiol 108:361. doi:10.1007/s00395-013-0361-1
Rosenkranz S, Flesch M, Amann K, Haeuseler C, Kilter H, Seeland U, Schlüter KD, Böhm M (2002) Alterations of beta-adrenergic signaling and cardiac hypertrophy in transgenic mice overexpressing TGF-beta(1). Am J Physiol Heart Circ Physiol 283:1253–1262. doi:10.1152/ajpheart.00578.2001
Sano M, Minamino T, Toko H, Miyauchi H, Orimo M, Qin Y, Akazawa H, Tateno K, Kayama Y, Harada M, Shimizu I, Asahara T, Hamada H, Tomita S, Molkentin JD, Zou Y, Komuro I (2007) p53-induced inhibition of Hif-1 causes cardiac dysfunction during pressure overload. Nature 446:444–448. doi:10.1038/nature05602
Shinde AV, Frangogiannis NG (2014) Fibroblasts in myocardial infarction: a role in inflammation and repair. J Mol Cell Cardiol 70:74–82. doi:10.1016/j.yjmcc.2013.11.015
Smith RR, Barile L, Cho HC, Leppo MK, Hare JM, Messina E, Giacomello A, Abraham MR, Marbán E (2007) Regenerative potential of cardiosphere-derived cells expanded from percutaneous endomyocardial biopsy specimens. Circulation 115:896–908. doi:10.1161/CIRCULATIONAHA.106.655209
Tseliou E, Pollan S, Malliaras K, Terrovitis J, Sun B, Galang G, Marbán L, Luthringer D, Marbán E (2013) Allogeneic cardiospheres boost cardiac function and attenuate adverse remodeling without eliciting immune reactions post-myocardial infarction in immunologically-mismatched rat strains. J Am Coll Cardiol 61:1108–1119. doi:10.1016/j.jacc.2012.10.052
Tseliou E, De Couto G, Terrovitis J, Sun B, Liu W, Marbán L, Marbán E (2014) Angiogenesis, cardiomyocyte proliferation and anti-fibrotic effects underlie structural preservation post-infarction by intramyocardially-injected cardiospheres. PLoS ONE 9:e88590. doi:10.1371/journal.pone.0088590
Wang ZF, Wang NP, Harmouche S, Philip T, Pang XF, Bai F, Zhao ZQ (2013) Postconditioning promotes the cardiac repair through balancing collagen degradation and synthesis after myocardial infarction in rats. Basic Res Cardiol 108:318. doi:10.1007/s00395-012-0318-9
Whittaker P, Kloner RA, Boughner DR, Pickering JG (1994) Quantitative assessment of myocardial collagen with picrosirius red staining and circularly polarized light. Basic Res Cardiol 89:397–410. doi:10.1007/BF00788278
Zeisberg EM, Tarnavski O, Zeisberg M, Dorfman AL, McMullen JR, Gustafsson E, Chandraker A, Yuan X, Pu WT, Roberts AB, Neilson EG, Sayegh MH, Izumo S, Kalluri R (2007) Endothelial-to-mesenchymal transition contributes to cardiac fibrosis. Nat Med. 13:952–961. doi:10.1038/nm1613
Acknowledgments
This work was supported by the California Institute for Regenerative Medicine (CIRM; RB4-06215) and the Cedars-Sinai Board of Governors Heart Stem Cell Center.
Conflict of interest
Eduardo Marbán is founder of, unpaid advisor to, and owns equity in Capricor. The other authors report no conflicts. Capricor provided no support for the present study.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Tseliou, E., Reich, H., de Couto, G. et al. Cardiospheres reverse adverse remodeling in chronic rat myocardial infarction: roles of soluble endoglin and Tgf-β signaling. Basic Res Cardiol 109, 443 (2014). https://doi.org/10.1007/s00395-014-0443-8
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00395-014-0443-8