Abstract
Purpose
Lower plasma level of folate has been associated with an increased risk of age-related cognitive impairment. However, studies that examined this relation have yielded mixed results. We aimed to examine the prospective association of plasma folate level with risk of cognitive impairment in a community-based prospective cohort of older adults in China.
Methods
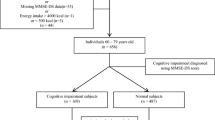
This study included 615 participants (mean age: 76.3 years) without baseline cognitive impairment from the Rugao Longevity and Ageing Study (RuLAS). We used logistic regression to examine the prospective association between baseline plasma folate and risk of cognitive impairment in the next two years. Fasting blood samples were collected and assayed for plasma folate level at baseline. Cognitive impairment was defined as Hasegawa Dementia Scale (HDS) score ≤ 21.5 points.
Results
During two years’ follow-up, 20.7% of the participants developed cognitive impairment. After controlled for age, gender, and plasma homocysteine, a higher level of plasma folate was associated with lower odds of cognitive impairment. The corresponding odds ratio (OR) with 95% confidence interval was 0.41 (0.19–0.89) comparing participants at extreme quintiles of plasma folate (median level 17.2 vs. 6.3 nmol/L). The associations were similar after further adjustment for major demographic and lifestyle factors (OR = 0.42, 0.18–0.98). Moreover, the inverse association was particularly stronger among males (OR = 0.12, 0.03–0.52) but was non-significant among females.
Conclusion
Our findings support a potential beneficial role of higher plasma folate levels in cognitive function in older Chinese adults, particularly among males. Future studies with larger sample size and longer follow-up are warranted to confirm these findings and to identify the optimal plasma folate level for cognitive function.


Similar content being viewed by others
Availability of data and material
The datasets used and analyzed for the current study are available from the corresponding author on reasonable request.
Code availability
Analysis codes used in this analysis are available from the corresponding author upon reasonable request.
References
Wortmann M (2012) Dementia: a global health priority-highlights from an ADI and World Health Organization report. Alzheimer’s Res Ther 4(5):40. https://doi.org/10.1186/alzrt143
Wimo A, Jönsson L, Bond J, Prince M, Winblad B, International AD (2013) The worldwide economic impact of dementia 2010. Alzheimer’s Dement 9(1):1–11. https://doi.org/10.1016/j.jalz.2012.11.006
Alzheimer’s association (2016) 2016 Alzheimer’s disease facts and figures. Alzheimer’s Dement 12(4):459–509. https://doi.org/10.1016/j.jalz.2016.03.001
Morris MC (2016) Nutrition and risk of dementia: overview and methodological issues. Ann N Y Acad Sci 1367(1):31. https://doi.org/10.1111/nyas.13047
Smith P, Blumenthal J (2016) Dietary factors and cognitive decline. Journal Prev Alzheimer’s Dis 3(1):53. https://doi.org/10.14283/jpad.2015.71
Tucker KL (2016) Nutrient intake, nutritional status, and cognitive function with aging. Ann N Y Acad Sci 1367(1):38–49. https://doi.org/10.1111/nyas.13062
Morris MC, Evans DA, Bienias JL, Tangney CC, Hebert LE, Scherr PA, Schneider JA (2005) Dietary folate and vitamin B12 intake and cognitive decline among community-dwelling older persons. Arch Neurol 62(4):641–645. https://doi.org/10.1001/archneur.62.4.641
Kado DM, Karlamangla AS, Huang M-H, Troen A, Rowe JW, Selhub J, Seeman TE (2005) Homocysteine versus the vitamins folate, B6, and B12 as predictors of cognitive function and decline in older high-functioning adults: MacArthur studies of successful aging. Am J Med 118(2):161–167
Koike T, Kuzuya M, Kanda S, Okada K, Izawa S, Enoki H, Iguchi A (2008) Raised homocysteine and low folate and vitamin B-12 concentrations predict cognitive decline in community-dwelling older Japanese adults. Clin Nutr 27(6):865–871. https://doi.org/10.1016/j.clnu.2008.08.006
Delchier N, Herbig AL, Rychlik M, Renard CM (2016) Folates in fruits and vegetables: contents, processing, and stability. Compr Rev Food Sci Food Safety 15(3):506–528. https://doi.org/10.1111/1541-4337.12193
Mikkelsen K, Stojanovska L, Tangalakis K, Bosevski M, Apostolopoulos V (2016) Cognitive decline: A vitamin B perspective. Maturitas 93:108–113. https://doi.org/10.1016/j.maturitas.2016.08.001
Iskandar BJ, Nelson A, Resnick D, Pate Skene J, Gao P, Johnson C, Cook TD, Hariharan N (2004) Folic acid supplementation enhances repair of the adult central nervous system. Ann Neurol 56(2):221–227. https://doi.org/10.1002/ana.20174
Lefèvre-Arbogast S, Féart C, Dartigues J-F, Helmer C, Letenneur L, Samieri C (2016) Dietary B vitamins and a 10-year risk of dementia in older persons. Nutrients 8(12):761. https://doi.org/10.3390/nu8120761
Agnew-Blais JC, Wassertheil-Smoller S, Kang JH, Hogan PE, Coker LH, Snetselaar LG, Smoller JW (2015) Folate, vitamin B-6, and vitamin B-12 intake and mild cognitive impairment and probable dementia in the women’s health initiative memory study. J Acad Nutr Diet 115(2):231–241. https://doi.org/10.1016/j.jand.2014.07.006
Luchsinger JA, Tang M-X, Miller J, Green R, Mayeux R (2007) Relation of higher folate intake to lower risk of alzheimer disease in the elderly. Arch Neurol 64(1):86–92. https://doi.org/10.1001/archneur.64.1.86
Mei X, Zhang Y, Zhu H, Zou Y, Zhang Z, Guo H, Liu Y, Cheng X, Wang J, Qian Z, Ling Y, Liu M, Huang W, Yi Z, Lu H (2020) Observations about symptomatic and asymptomatic infections of 494 patients with COVID-19 in Shanghai. China Am J Infect Control 48(9):1045–1050. https://doi.org/10.1016/j.ajic.2020.06.221
Vogel T, Dali-Youcef N, Kaltenbach G, Andres E (2009) Homocysteine, vitamin B12, folate and cognitive functions: a systematic and critical review of the literature. Int J Clin Pract 63(7):1061–1067. https://doi.org/10.1111/j.1742-1241.2009.02026.x
Wang B, Sahyoun NR, Shao K, Dutta E, Clarke J (2020) Assessment of the dose-response relationship between folate exposure and cognitive impairment: synthesizing data from documented studies. Risk Anal 40(2):276–293. https://doi.org/10.1111/risa.13404
Barnes JL, Tian M, Edens NK, Morris MC (2014) Consideration of nutrient levels in studies of cognitive decline. Nutr Rev 72(11):707–719
Liu Z, Wang Y, Zhang Y, Chu X, Wang Z, Qian D, Chen F, Xu J, Li S, Jin L (2016) Cohort profile: the Rugao longevity and ageing study (RuLAS). Int J Epidemiol 45(4):1064–1073
Kashiwase H, Watanabe M, Suda E, Tachibana S, Kinuya M, Ohtakeno S, Watanabe H, Hotori A, Tatsunuma T, Nagashima K (1991) Affective and cognitive symptoms in the Aged in a Japanese nursing home. Dement Geriatr Cogn Disord 2(2):112–115
Ma T, Lu D, Zhu YS, Chu XF, Wang Y, Shi GP, Wang ZD, Yu L, Jiang XY, Wang XF (2018) ACTN3 genotype and physical function and frailty in an elderly Chinese population: the Rugao longevity and ageing study. Age Ageing 47(3):416–422
Husain MA, Laurent B, Plourde M (2021) APOE and Alzheimer’s disease: from lipid transport to physiopathology and therapeutics. Front Neurosci 15:85
Montagne A, Nation DA, Sagare AP, Barisano G, Sweeney MD, Chakhoyan A, Pachicano M, Joe E, Nelson AR, D’Orazio LM (2020) APOE4 leads to blood–brain barrier dysfunction predicting cognitive decline. Nature 581(7806):71–76. https://doi.org/10.1038/s41586-020-2247-3
Liu Y, Zhang H, Chen G, Wu W, Hu J, Wan W, Ma C (2008) Therapeutic effects of scalp-acupuncture in patients with vascular dementia induced by cerebral infarction: a randomized controlled trial. J Chin Integr Medicine 6(8):806–809
Ninomiya T (2018) Japanese legacy cohort studies: the Hisayama Study. J Epidemiol 28(11):444–451
Cricco M, Simonsick EM, Foley DJ (2001) The impact of insomnia on cognitive functioning in older adults. J Am Geriatr Soc 49(9):1185–1189. https://doi.org/10.1046/j.1532-5415.2001.49235.x
Mortimer JA, Ebbitt B, Jun S-P, Finch MD (1992) Predictors of cognitive and functional progression in patients with probable Alzheimer’s disease. Neurology 42(9):1689–1689. https://doi.org/10.1212/WNL.42.9.1689
Maxwell CJ, Hogan DB, Ebly EM (2002) Serum folate levels and subsequent adverse cerebrovascular outcomes in elderly persons. Dement Geriatr Cogn Disord 13(4):225–234. https://doi.org/10.1159/000057701
Durga J, van Boxtel MP, Schouten EG, Kok FJ, Jolles J, Katan MB, Verhoef P (2007) Effect of 3-year folic acid supplementation on cognitive function in older adults in the FACIT trial: a randomised, double blind, controlled trial. The Lancet 369(9557):208–216. https://doi.org/10.1016/S0140-6736(07)60109-3
Meng H, Li Y, Zhang W, Zhao Y, Niu X, Guo J (2019) The relationship between cognitive impairment and homocysteine in a B12 and folate deficient population in China: a cross-sectional study. Medicine. https://doi.org/10.1097/MD.0000000000017970
Ma F, Wu T, Zhao J, Ji L, Song A, Zhang M, Huang G (2017) Plasma homocysteine and serum folate and vitamin B12 levels in mild cognitive impairment and alzheimer’s disease: a case-control study. Nutrients 9(7):725. https://doi.org/10.3390/nu9070725
Li M, Li W, Gao Y, Chen Y, Bai D, Weng J, Du Y, Ma F, Wang X, Liu H (2020) Effect of folic acid combined with docosahexaenoic acid intervention on mild cognitive impairment in elderly: a randomized double-blind, placebo-controlled trial. Eur J Nutr. https://doi.org/10.1007/s00394-020-02373-3
Scott JM, Weir DG (1998) Folic acid, homocysteine and one-carbon metabolism: a review of the essential biochemistry. J Cardiovasc Risk 5(4):223–227. https://doi.org/10.1177/174182679800500403
Selhub J, Miller JW (1992) The pathogenesis of homocysteinemia: interruption of the coordinate regulation by S-adenosylmethionine of the remethylation and transsulfuration of homocysteine. Am J Clin Nutr 55(1):131–138. https://doi.org/10.1093/ajcn/55.1.131
Morris MS, Jacques PF, Rosenberg IH, Selhub J (2001) Hyperhomocysteinemia associated with poor recall in the third National health and nutrition examination survey. Am J Clin Nutr 73(5):927–933. https://doi.org/10.1093/ajcn/73.5.927
Troen AM, Chao W-H, Crivello NA, D’Anci KE, Shukitt-Hale B, Smith DE, Selhub J, Rosenberg IH (2008) Cognitive impairment in folate-deficient rats corresponds to depleted brain phosphatidylcholine and is prevented by dietary methionine without lowering plasma homocysteine. J Nutr 138(12):2502–2509. https://doi.org/10.3945/jn.108.093641
Kruman II, Kumaravel T, Lohani A, Pedersen WA, Cutler RG, Kruman Y, Haughey N, Lee J, Evans M, Mattson MP (2002) Folic acid deficiency and homocysteine impair DNA repair in hippocampal neurons and sensitize them to amyloid toxicity in experimental models of alzheimer’s disease. J Neurosci 22(5):1752–1762. https://doi.org/10.1523/JNEUROSCI.22-05-01752.2002
Dolatabadi HRD, Reisi P, Alaei H, Malekabadi HA, Pilehvarian AA (2012) Folic acid and coenzyme Q10 ameliorate cognitive dysfunction in the rats with intracerebroventricular injection of streptozotocin. Iran J Basic Med Sci 15(2):719
Liu R, Liu IY, Bi X, Thompson RF, Doctrow SR, Malfroy B, Baudry M (2003) Reversal of age-related learning deficits and brain oxidative stress in mice with superoxide dismutase/catalase mimetics. Proc Natl Acad Sci 100(14):8526–8531. https://doi.org/10.1073/pnas.1332809100
Joshi R, Adhikari S, Patro B, Chattopadhyay S, Mukherjee T (2001) Free radical scavenging behavior of folic acid: evidence for possible antioxidant activity. Free Radical Biol Med 30(12):1390–1399. https://doi.org/10.1016/S0891-5849(01)00543-3
Shane B, Stokstad ER (1985) Vitamin B12-folate interrelationships. Annu Rev Nutr 5(1):115–141
Levitt AJ, Joffe RT (1989) Folate, B12, and life course of depressive illness. Biol Psychiat 25(7):867–872. https://doi.org/10.1016/0006-3223(89)90266-7
Das UN (2008) Folic acid and polyunsaturated fatty acids improve cognitive function and prevent depression, dementia, and Alzheimer’s disease–but how and why? Prostaglandins Leukot Essent Fatty Acids 78(1):11–19. https://doi.org/10.1016/j.plefa.2007.10.006
Ma F, Wu T, Zhao J, Song A, Liu H, Xu W, Huang G (2016) Folic acid supplementation improves cognitive function by reducing the levels of peripheral inflammatory cytokines in elderly Chinese subjects with MCI. Sci Rep 6:37486. https://doi.org/10.1038/srep37486
Tsai N, Gao Z-X (1989) Validity of Hasegawa’s dementia scale for screening dementia among aged Chinese. Int Psychogeriatr 1(2):145–152. https://doi.org/10.1017/S1041610289000153
Höller U, Bakker SJ, Düsterloh A, Frei B, Köhrle J, Konz T, Lietz G, McCann A, Michels AJ, Molloy AM (2018) Micronutrient status assessment in humans: current methods of analysis and future trends. TrAC Trends Anal Chem 102:110–122
Bailey LB, Stover PJ, McNulty H, Fenech MF, Gregory JF III, Mills JL, Pfeiffer CM, Fazili Z, Zhang M, Ueland PM (2015) Biomarkers of nutrition for development—folate review. J Nutr 145(7):1636S-1680S
Acknowledgements
The authors acknowledge the support from the Key Laboratory of Intelligent Preventive Medicine of Zhejiang Province (2020E10004).
Funding
This work was supported by the National Key R&D Program of China (2018YFC2000400/2018YFC2000400-3), the Shanghai Municipal Science and Technology Major Project (Grant No. 2017SHZDZX01).
Author information
Authors and Affiliations
Contributions
XW and CY designed the analysis; XC and JY performed the statistical analyses; CY, XC, JY, and HZ interpreted the data and drafted and revised the manuscript; CY supervised the data analysis and interpretation; CY, XW had the primary responsibility for the study final content; all authors critically reviewed the manuscript and approved the final draft.
Corresponding authors
Ethics declarations
Conflict of interest
None.
Ethics approval
This study was approved by the Human Ethics Committee of the School of Life Sciences of Fudan University, Shanghai, China (Ethical Approval No. BE1815).
Consent to participate
Informed consent was obtained from all participants before participation.
Consent for publication
All the authors have approved the submitted version.
Supplementary Information
Below is the link to the electronic supplementary material.
394_2022_2825_MOESM1_ESM.docx
Supplementary Table 1 Multivariable-adjusted ORs (95% CIs) for cognitive impairment comparing top to bottom quintile of plasma folate levels across subgroups
Rights and permissions
About this article
Cite this article
Chen, X., Yang, J., Zhang, H. et al. Plasma folate levels in relation to cognitive impairment: a community-based cohort of older adults in China. Eur J Nutr 61, 2837–2845 (2022). https://doi.org/10.1007/s00394-022-02825-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-022-02825-y