Abstract
Purpose
Evidence about the effect of maternal vitamin B12 supplementation on offspring’s vitamin B12 status is limited. The present interventional study sought to evaluate the association of antenatal vitamin B complex supplementation with neonatal vitamin B12 status.
Methods
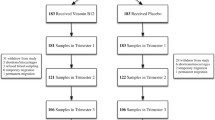
In an ongoing cluster randomized controlled trial conducted in three rural counties in northwest China, pregnant women < 20 weeks of gestation were randomized to three treatment groups: blank control, iron supplements, or vitamin B complex supplements. All women were administered folic acid supplements during the periconceptional period. In a sub-study, we collected cord blood samples of 331 participants from the control or vitamin B complex groups in the Xunyi county from January 2017 to December 2017. Plasma concentrations of folate, vitamin B12, and homocysteine were measured. Linear mixed models with a random intercept for cluster were used to compare biochemical indexes between groups after controlling for covariates.
Results
Compared with newborns whose mothers were in the control group, newborns of the vitamin B complex-supplemented women had significantly higher cord plasma vitamin B12 (P = 0.001) and lower homocysteine concentrations (P = 0.043). The association of antenatal vitamin B complex supplementation with cord blood vitamin B12 concentrations appeared to be more pronounced among newborns with high folate status than those with low folate status (Pinteraction = 0.060).
Conclusions
Maternal vitamin B complex supplementation during pregnancy was associated with better neonatal vitamin B12 status in rural northwest China.

Similar content being viewed by others
References
McGee M, Bainbridge S, Fontaine-Bisson B (2018) A crucial role for maternal dietary methyl donor intake in epigenetic programming and fetal growth outcomes. Nutr Rev 76:469–478
Stover PJ (2004) Physiology of folate and vitamin B12 in health and disease. Nutr Rev 62:S3–12
Gomes S, Lopes C, Pinto E (2016) Folate and folic acid in the periconceptional period: recommendations from official health organizations in thirty-six countries worldwide and WHO. Public Health Nutr 19:176–189
Global Progress of Industrially Milled Cereal Grain Fortification. https://www.ffinetwork.org/global_progress/. Accessed 10 Apr 2020
Sukumar N, Rafnsson SB, Kandala NB, Bhopal R, Yajnik CS, Saravanan P (2016) Prevalence of vitamin B-12 insufficiency during pregnancy and its effect on offspring birth weight: a systematic review and meta-analysis. Am J Clin Nutr 103:1232–1251
Dang S, Yan H, Zeng L, Wang Q, Li Q, Xiao S, Fan X (2014) The status of vitamin B12 and folate among Chinese women: a population-based cross-sectional study in northwest China. PLoS ONE 9:e112586
Samuel TM, Duggan C, Thomas T, Bosch R, Rajendran R, Virtanen SM, Srinivasan K, Kurpad AV (2013) Vitamin B-12 intake and status in early pregnancy among urban South Indian women. Ann Nutr Metab 62:113–122
Chandyo RK, Ulak M, Sommerfelt H, Schneede J, Ueland PM, Strand TA (2016) Nutritional intake and status of cobalamin and folate among non-pregnant women of reproductive age in Bhaktapur. Nepal Nutrients 8:375
Soofi S, Khan GN, Sadiq K, Ariff S, Habib A, Kureishy S, Hussain I, Umer M, Suhag Z, Rizvi A et al (2017) Prevalence and possible factors associated with anaemia, and vitamin B-12 and folate deficiencies in women of reproductive age in Pakistan: analysis of national-level secondary survey data. BMJ Open 7:e018007
Lindstrom E, Hossain MB, Lonnerdal B, Raqib R, EI Arifeen S, Ekstrom EC (2011) Prevalence of anemia and micronutrient deficiencies in early pregnancy in rural Bangladesh, the MINIMat trial. Acta Obstet Gynecol Scand 90:47–56
Liu D, Cheng Y, Dang S, Wang D, Zhao Y, Li C, Li S, Lei F, Qu P, Mi B et al (2019) Maternal adherence to micronutrient supplementation before and during pregnancy in Northwest China: a large-scale population-based cross-sectional survey. BMJ Open 9:e028843
Molloy AM, Kirke PN, Troendle JF, Burke H, Sutton M, Brody LC, Scott JM, Mills JL (2009) Maternal vitamin B12 status and risk of neural tube defects in a population with high neural tube defect prevalence and no folic acid fortification. Pediatrics 123:917–923
Lai JS, Mohamad Ayob MN, Cai S, Quah PL, Gluckman PD, Shek LP, Yap F, Tan KH, Chong YS, Godfrey KM et al (2019) Maternal plasma vitamin B12 concentrations during pregnancy and infant cognitive outcomes at 2 years of age. Br J Nutr 121:1303–1312
Yajnik CS, Deshpande SS, Jackson AA, Refsum H, Rao S, Fisher DJ, Bhat DS, Naik SS, Coyaji KJ, Joglekar CV et al (2008) Vitamin B12 and folate concentrations during pregnancy and insulin resistance in the offspring: the Pune Maternal Nutrition Study. Diabetologia 51:29–38
Eneroth H, El Arifeen S, Persson LA, Lonnerdal B, Hossain MB, Stephensen CB, Ekström EC (2010) Maternal multiple micronutrient supplementation has limited impact on micronutrient status of Bangladeshi infants compared with standard iron and folic acid supplementation. J Nutr 140:618–624
Duggan C, Srinivasan K, Thomas T, Samuel T, Rajendran R, Muthayya S, Finkelstein JL, Lukose A, Fawzi W, Allen LH et al (2014) Vitamin B-12 supplementation during pregnancy and early lactation increases maternal, breast milk, and infant measures of vitamin B-12 status. J Nutr 144:758–764
Siddiqua TJ, Ahmad SM, Ahsan KB, Rashid M, Roy A, Rahman SM, Shahab-Ferdows S, Hampel D, Ahmed T, Allen LH et al (2016) Vitamin B12 supplementation during pregnancy and postpartum improves B12 status of both mothers and infants but vaccine response in mothers only: a randomized clinical trial in Bangladesh. Eur J Nutr 55:281–293
Van Spall HG, Toren A, Kiss A, Fowler RA (2007) Eligibility criteria of randomized controlled trials published in high-impact general medical journals: a systematic sampling review. JAMA 297:1233–1240
Rutterford C, Copas A, Eldridge S (2015) Methods for sample size determination in cluster randomized trials. Int J Epidemiol 44:1051–1067
Project management plan on folic acid supplementation prevented neural tube defects. https://www.nhc.gov.cn/cms-search/xxgk/getManuscriptXxgk.htm?id=41532. Accessed 24 Jun 2009
Devalia V, Hamilton MS, Molloy AM (2014) Guidelines for the diagnosis and treatment of cobalamin and folate disorders. Br J Haematol 166:496–513
Huijgen HJ, Frans PW, Tegelaers FPW, Schoenmakers CHH, Pronk-Admiraal CJ, Ekema S (2004) Multicenter analytical evaluation of an enzymatic method for the measurement of plasma homocysteine and comparison with HPLC and immunochemistry. Clin Chem 50:937–941
Filmer D, Pritchett LH (2001) Estimating wealth effects without expenditure data–or tears: an application to educational enrollments in states of India. Demography 38:115–132
Villar J, Cheikh Ismail L, Victora CG, Ohuma EO, Bertino E, Altman DG, Lambert A, Papageorghiou AT, Carvalho M, Jaffer YA et al (2014) International standards for newborn weight, length, and head circumference by gestational age and sex: the Newborn Cross-Sectional Study of the INTERGROWTH-21st Project. Lancet 384:857–868
Hedeker D, Gibbons RD, Flay BR (1994) Random-effects regression models for clustered data with an example from smoking prevention research. J Consult Clin Psychol 62:757–765
Leyrat C, Morgan KE, Leurent B, Kahan BC (2018) Cluster randomized trials with a small number of clusters: which analyses should be used? Int J Epidemiol 47:321–331
Li P, Redden DT (2015) Comparing denominator degrees of freedom approximations for the generalized linear mixed model in analyzing binary outcome in small sample cluster-randomized trials. BMC Med Res Methodol 15:38
Hay G, Clausen T, Whitelaw A, Trygg K, Johnston C, Henriksen T, Refsum H (2010) Maternal folate and cobalamin status predicts vitamin status in newborns and 6-month-old infants. J Nutr 140:557–564
Mickey RM, Greenland S (1989) The impact of confounder selection criteria on effect estimation. Am J Epidemiol 129:125–137
Sedgwick P (2015) Randomized controlled trials: understanding effect sizes. BMJ 350:h1690
Dijkman B, Kooistra B, Bhandari M, Evidence-Based Surgery Working Group (2009) How to work with a subgroup analysis. Can J Surg 52:515–522
Rogne T, Tielemans MJ, Chong MF-F, Yajnik CS, Krishnaveni GV, Poston L, Jaddoe VWV, Steegers EA, Joshi S, Chong YS et al (2017) Associations of maternal vitamin b12 concentration in pregnancy with the risks of preterm birth and low birth weight: a systematic review and meta-analysis of individual participant data. Am J Epidemiol 185:212–223
Bjorke Monsen AL, Ueland PM (2003) Homocysteine and methylmalonic acid in diagnosis and risk assessment from infancy to adolescence. Am J Clin Nutr 78:7–21
Shane B (2008) Folate and vitamin B12 metabolism: overview and interaction with riboflavin, vitamin B6, and polymorphisms. Food Nutr Bull 29(2 Suppl):S5–S19
Frery N, Huel G, Leroy M, Moreau T, Savard R, Blot P, Lellouch J (1992) Vitamin B12 among parturients and their newborns and its relationship with birthweight. Eur J Obstet Gynecol Reprod Biol 45:155–163
Obeid R, Munz W, Jager M, Schmidt W, Herrmann W (2005) Biochemical indexes of the B vitamins in cord serum are predicted by maternal B vitamin status. Am J Clin Nutr 82:133–139
List of 832 poverty-stricken counties in China. https://www.cpad.gov.cn/art/2014/12/23/art_343_981.html. Accessed 23 Dec 2014
Variant: rs1801133. https://asia.ensembl.org/Homo_sapiens/Variation/Population?db=core;r=1:11795821-11796821;v=rs1801133;vdb=variation;vf=502019084. Accessed 10 Apr 2020
Yang B, Fan S, Zhi X, Xia R, Wang Y, Zheng Q, Sun G (2017) Geographical and ethnic distribution of MTHFR gene polymorphisms and their associations with diseases among Chinese population. Clin Genet 92:243–258
Zinck JW, de Groh M, MacFarlane AJ (2015) Genetic modifiers of folate, vitamin B-12, and homocysteine status in a cross-sectional study of the Canadian population. Am J Clin Nutr 101:1295–1304
Horan MK, McGowan CA, Gibney ER, Donnelly JM, McAuliffe FM (2015) The association between maternal dietary micronutrient intake and neonatal anthropometry—secondary analysis from the ROLO study. Nutr J 14:105
Bhate V, Deshpande S, Bhat D, Joshi N, Ladkat R, Watve S, Fall C, de Jager CA, Refsum H, Yajnik C (2008) Vitamin B12 status of pregnant Indian women and cognitive function in their 9-year-old children. Food Nutr Bull 29:249–254
Hrobjartsson A, Emanuelsson F, Skou Thomsen AS, Hilden J, Brorson S (2014) Bias due to lack of patient blinding in clinical trials. A systematic review of trials randomizing patients to blind and nonblind sub-studies. Int J Epidemiol 43:1272–1283
Farrell C-JL, Kirsch SH, Herrmann M (2013) Red cell or serum folate: what to do in clinical practice? Clin Chem Lab Med 51:555–569
Nexo E, Hoffmann-Lücke E (2011) Holotranscobalamin, a marker of vitamin B-12 status: analytical aspects and clinical utility. Am J Clin Nutr 94:359S–365S
Bjørke Monsen AL, Ueland PM (2003) Homocysteine and methylmalonic acid in diagnosis and risk assessment from infancy to adolescence. Am J Clin Nutr 78:7–21
Acknowledgements
The authors thank all participants and researchers who participated in this study. The authors are also grateful to the Xunyi County Hospital and the Xunyi County Maternal and Child Health Hospital for their collaboration during the implementation of this trial.
Funding
This study was sponsored by the National Key Research and Development Program of China (grant number 2017YFC0907200, grant number 2017YFC0907201), the National Natural Science Foundation of China (grant number 81230016), the Project of birth defect control and prevention in Shaanxi (grant number Sxwsjswzfcght2016-013), the China Postdoctoral Science Foundation (grant number 2015M582678) and Xi’an Jiaotong University (xjj2018146). The funders had no role in the design of the study; in the collection, analyses, and interpretation of the data; in the writing of the manuscript, and in the decision to submit the manuscript for publication.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors have no conflicts of interest related to this study to disclose.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Li, S., Mi, B., Qu, P. et al. Association of antenatal vitamin B complex supplementation with neonatal vitamin B12 status: evidence from a cluster randomized controlled trial. Eur J Nutr 60, 1031–1039 (2021). https://doi.org/10.1007/s00394-020-02309-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-020-02309-x