Abstract
Background
Atrioventricular (AV) interval optimization is often deemed too time-consuming in dual-chamber pacemaker patients with maintained LV function. Thus the majority of patients are left at their default AV interval.
Objective
To quantify the magnitude of hemodynamic improvement following AV interval optimization in chronically paced dual chamber pacemaker patients.
Patients and methods
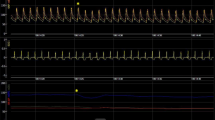
A pressure volume catheter was placed in the left ventricle of 19 patients with chronic dual chamber pacing and an ejection fraction >45 % undergoing elective coronary angiography. AV interval was varied in 10 ms steps from 80 to 300 ms, and pressure volume loops were recorded during breath hold.
Results
The average optimal AV interval was 152 ± 39 ms compared to 155 ± 8 ms for the average default AV interval (range 100–240 ms). The average improvement in stroke work following AV interval optimization was 935 ± 760 mmHg/ml (range 0–2,908; p < 0.001), which translates into an average improvement of 14 ± 9 % (range 0–28). A 10 ms variation of the AV interval changes the average stroke work by 207 ± 162 mmHg/ml. AV interval optimization also leads to improved systolic dyssynchrony indices (17.7 ± 7.0 vs. 19.4 ± 7.1 %; p = 0.01).
Conclusion
The overall hemodynamic effect of AV interval optimization in patients with maintained LV function is in the same range as for patients undergoing cardiac resynchronization therapy for several parameters. The positive effect of AV interval optimization also applies to patients who have been chronically paced for years.




Similar content being viewed by others
Abbreviations
- AV:
-
Atrioventricular
- +dp/dt max :
-
First derivative of LV pressure rise
- −dp/dt max :
-
First derivative of LV pressure decline
- CRT:
-
Cardiac resynchronization therapy
- LV:
-
Left ventricular
References
Auricchio A, Stellbrink C, Block M, Sack S, Vogt J, Bakker P, Klein H, Kramer A, Ding J, Salo R, Tockman B, Pochet T, Spinelli J (1999) Effect of pacing chamber and atrioventricular delay on acute systolic function of paced patients with congestive heart failure. The Pacing Therapies for Congestive Heart Failure Study Group. The Guidant Congestive Heart Failure Research Group. Circulation 99:2993–3001
Jansen AH, Bracke FA, van Dantzig JM, Meijer A, van der Voort PH, Aarnoudse W, van Gelder BM, Peels KH (2006) Correlation of echo-Doppler optimization of atrioventricular delay in cardiac resynchronization therapy with invasive hemodynamics in patients with heart failure secondary to ischemic or idiopathic dilated cardiomyopathy. Am J Cardiol 97:552–557
Kerlan JE, Sawhney NS, Waggoner AD, Chawla MK, Garhwal S, Osborn JL, Faddis MN (2006) Prospective comparison of echocardiographic atrioventricular delay optimization methods for cardiac resynchronization therapy. Heart Rhythm 3:148–154
Vardas PE, Auricchio A, Blanc JJ, Daubert JC, Drexler H, Ector H, Gasparini M, Linde C, Morgado FB, Oto A, Sutton R, Trusz-Gluza M (2007) Guidelines for cardiac pacing and cardiac resynchronization therapy: the task force for cardiac pacing and cardiac resynchronization therapy of the European Society of Cardiology. Developed in collaboration with the European Heart Rhythm Association. Eur Heart J 28:2256–2295
Gorcsan J 3rd, Abraham T, Agler DA, Bax JJ, Derumeaux G, Grimm RA, Martin R, Steinberg JS, Sutton MS, Yu CM (2008) Echocardiography for cardiac resynchronization therapy: recommendations for performance and reporting—a report from the American Society of Echocardiography Dyssynchrony Writing Group endorsed by the Heart Rhythm Society. J Am Soc Echocardiogr 21:191–213
Baker JH 2nd, McKenzie J 3rd, Beau S, Greer GS, Porterfield J, Fedor M, Greenberg S, Daoud EG, Corbisiero R, Bailey JR, Porterfield L (2007) Acute evaluation of programmer-guided AV/PV and VV delay optimization comparing an IEGM method and echocardiogram for cardiac resynchronization therapy in heart failure patients and dual-chamber ICD implants. J Cardiovasc Electrophysiol 18:185–191
Barold SS, Ilercil A, Herweg B (2008) Echocardiographic optimization of the atrioventricular and interventricular intervals during cardiac resynchronization. Europace 10(Suppl 3):iii88–iii95
Dupuis JM, Kobeissi A, Vitali L, Gaggini G, Merheb M, Rouleau F, Leftheriotis G, Ritter P, Victor J (2003) Programming optimal atrioventricular delay in dual chamber pacing using peak endocardial acceleration: comparison with a standard echocardiographic procedure. Pacing Clin Electrophysiol 26:210–213
Naqvi TZ, Rafique AM (2008) Echocardiography-guided pacemaker optimization and radial artery tonometry. J Card Fail 14:583–589
Zhang Q, Fung JW, Chan YS, Chan HC, Lin H, Chan S, Yu CM (2008) The role of repeating optimization of atrioventricular interval during interim and long-term follow-up after cardiac resynchronization therapy. Int J Cardiol 124:211–217
Steendijk P, Tulner SA, Bax JJ, Oemrawsingh PV, Bleeker GB, van Erven L, Putter H, Verwey HF, van der Wall EE, Schalij MJ (2006) Hemodynamic effects of long-term cardiac resynchronization therapy: analysis by pressure-volume loops. Circulation 113:1295–1304
Steendijk P, Staal E, Jukema JW, Baan J (2001) Hypertonic saline method accurately determines parallel conductance for dual-field conductance catheter. Am J Physiol Heart Circ Physiol 281:H755–H763
Steendijk P, Tulner SA, Schreuder JJ, Bax JJ, van Erven L, van der Wall EE, Dion RA, Schalij MJ, Baan J (2004) Quantification of left ventricular mechanical dyssynchrony by conductance catheter in heart failure patients. Am J Physiol Heart Circ Physiol 286:H723–H730
Hanke T, Misfeld M, Heringlake M, Schreuder JJ, Wiegand UK, Eberhardt F (2009) The effect of biventricular pacing on cardiac function after weaning from cardiopulmonary bypass in patients with reduced left ventricular function: a pressure-volume loop analysis. J Thorac Cardiovasc Surg 138:148–156
Kass DA, Chen CH, Curry C, Talbot M, Berger R, Fetics B, Nevo E (1999) Improved left ventricular mechanics from acute VDD pacing in patients with dilated cardiomyopathy and ventricular conduction delay. Circulation 99:1567–1573
Paulus WJ, Tschope C, Sanderson JE, Rusconi C, Flachskampf FA, Rademakers FE, Marino P, Smiseth OA, De Keulenaer G, Leite-Moreira AF, Borbely A, Edes I, Handoko ML, Heymans S, Pezzali N, Pieske B, Dickstein K, Fraser AG, Brutsaert DL (2007) How to diagnose diastolic heart failure: a consensus statement on the diagnosis of heart failure with normal left ventricular ejection fraction by the Heart Failure and Echocardiography Associations of the European Society of Cardiology. Eur Heart J 28:2539–2550
Delnoy PP, Ottervanger JP, Luttikhuis HO, Vos DH, Elvan A, Ramdat Misier AR, Beukema WP, Steendijk P, van Hemel NM (2009) Pressure-volume loop analysis during implantation of biventricular pacemaker/cardiac resynchronization therapy device to optimize right and left ventricular pacing sites. Eur Heart J 30:797–804
Dekker AL, Phelps B, Dijkman B, van der Nagel T, van der Veen FH, Geskes GG, Maessen JG (2004) Epicardial left ventricular lead placement for cardiac resynchronization therapy: optimal pace site selection with pressure-volume loops. J Thorac Cardiovasc Surg 127:1641–1647
Simantirakis EN, Kochiadakis GE, Vardakis KE, Igoumenidis NE, Chrysostomakis SI, Vardas PE (2003) Left ventricular mechanics and myocardial blood flow following restoration of normal activation sequence in paced patients with long-term right ventricular apical stimulation. Chest 124:233–241
Wilkoff BL, Cook JR, Epstein AE, Greene HL, Hallstrom AP, Hsia H, Kutalek SP, Sharma A (2002) Dual-chamber pacing or ventricular backup pacing in patients with an implantable defibrillator: the Dual Chamber and VVI Implantable Defibrillator (DAVID) Trial. JAMA 288:3115–3123
Tse HF, Yu C, Wong KK, Tsang V, Leung YL, Ho WY, Lau CP (2002) Functional abnormalities in patients with permanent right ventricular pacing: the effect of sites of electrical stimulation. J Am Coll Cardiol 40:1451–1458
Nitardy A, Langreck H, Dietz R, Stockburger M (2009) Reduction of right ventricular pacing in patients with sinus node dysfunction through programming a long atrioventricular delay along with the DDIR mode. Clin Res Cardiol 98:25–32
Whinnett ZI, Davies JE, Nott G, Willson K, Manisty CH, Peters NS, Kanagaratnam P, Davies DW, Hughes AD, Mayet J, Francis DP (2008) Efficiency, reproducibility and agreement of five different hemodynamic measures for optimization of cardiac resynchronization therapy. Int J Cardiol 129:216–226
Mokrani B, Lafitte S, Deplagne A, Ploux S, Laborderie J, Reant P, Dos Santos P, Roudaut R, Jais P, Haissaguerre M, Clementy J, Bordachar P (2009) Echocardiographic study of the optimal atrioventricular delay at rest and during exercise in recipients of cardiac resynchronization therapy systems. Heart Rhythm 6:972–977
Strauss M, Becker T, Kleemann T, Dyck N, Birkenhauer F, Seidl K Impact of moderate exercise workload on predicted optimal AV and VV delays determined by an intracardiac electrogram-based method for optimizing cardiac resynchronization therapy. Clin Res Cardiol 99:735–741
Voss F, Becker R, Hauck M, Katus HA, Bauer A (2009) The basic pacing rate in CRT patients: the higher the better? Clin Res Cardiol 98:219–223
Styliadis IH, Gouzoumas NI, Karvounis HI, Papadopoulos CE, Efthimiadis GK, Karamouzis M, Parharidis GE, Louridas GE (2005) Effects of variation of atrioventricular interval on left ventricular diastolic filling dynamics and atrial natriuretic peptide levels in patients with DDD pacing for complete heart block. Europace 7:576–583
Toda N, Ishikawa T, Nozawa N, Kobayashi I, Ochiai H, Miyamoto K, Sumita S, Kimura K, Umemura S (2001) Doppler index and plasma level of atrial natriuretic hormone are improved by optimizing atrioventricular delay in atrioventricular block patients with implanted DDD pacemakers. Pacing Clin Electrophysiol 24:1660–1663
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Eberhardt, F., Hanke, T., Fitschen, J. et al. AV interval optimization using pressure volume loops in dual chamber pacemaker patients with maintained systolic left ventricular function. Clin Res Cardiol 101, 647–653 (2012). https://doi.org/10.1007/s00392-012-0439-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00392-012-0439-z