Abstract
Background
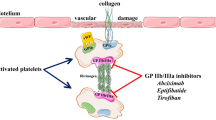
In patients with ST-elevation myocardial infarction (STEMI), direct intracoronary bolus administration of the glycoprotein (GP) IIb/IIIa receptor antagonist abciximab is associated with a reduction in infarct size, better myocardial salvage, less microvascular obstruction and improved myocardial blush grade as compared to intravenous bolus injection, presumably caused by higher local drug concentrations leading to a more pronounced inhibition of platelet aggregation. We investigated whether there are differences in the degree of GP IIb/IIIa receptor occupancy and platelet inhibition in blood drawn from the coronary sinus (CS) shortly after intracoronary versus intravenous abciximab bolus administration.
Methods
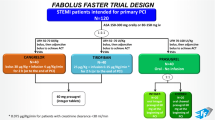
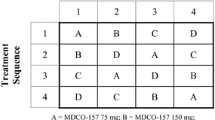
A total of 16 patients with acute STEMI undergoing primary percutaneous coronary intervention within 12 h of symptom onset underwent blood sampling from the CS before, immediately after and 30 min after abciximab bolus administration (intracoronary bolus: n = 8 patients; intravenous bolus: n = 8 patients).
Results
Immediately after bolus application, GP IIb/IIIa receptor occupancy in CS blood was significantly higher in patients who received direct intracoronary bolus injection compared to administration via a peripheral vein (intracoronary bolus: 93.5% [IQR 92.7–95.4]; intravenous bolus: 74.0% [IQR 17.6–94.0], p = 0.04). The degree of platelet inhibition was also markedly higher with intracoronary compared to intravenous dosing. At late sampling after 30 min no significant differences were found between groups for both platelet reactivity and GP IIb/IIIa receptor occupancy.
Conclusions
Acutely, direct intracoronary bolus injection resulted in a more pronounced local inhibition of platelet function and a higher degree of GP IIb/IIIa receptor occupancy as compared to standard intravenous bolus injection.



Similar content being viewed by others
Abbreviations
- STEMI:
-
ST-elevation myocardial infarction
- GP:
-
Glycoprotein
- PCI:
-
Percutaneous coronary intervention
- CS:
-
Coronary sinus
- ADP:
-
Adenosine diphosphate
- TRAP:
-
Thrombin receptor activating peptide
- AU:
-
Aggregation unit
- IQR:
-
Interquartile range
References
Kushner FG, Hand M, Smith SC Jr, King SB 3rd, Anderson JL, Antman EM, Bailey SR, Bates ER, Blankenship JC, Casey DE Jr, Green LA, Hochman JS, Jacobs AK, Krumholz HM, Morrison DA, Ornato JP, Pearle DL, Peterson ED, Sloan MA, Whitlow PL, Williams DO (2009) 2009 Focused Updates: ACC/AHA Guidelines for the Management of Patients With ST-Elevation Myocardial Infarction (updating the 2004 Guideline and 2007 Focused Update) and ACC/AHA/SCAI Guidelines on Percutaneous Coronary Intervention (updating the 2005 Guideline and 2007 Focused Update): a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. Circulation 120(22):2271–2306. doi:10.1161/CIRCULATIONAHA.109.192663
Hansen PR, Iversen A, Abdulla J (2010) Improved clinical outcomes with intracoronary compared to intravenous abciximab in patients with acute coronary syndromes undergoing percutaneous coronary intervention: a systematic review and meta-analysis. J Invasive Cardiol 22(6):278–282
Schulz S, Birkmeier KA, Ndrepepa G, Moshage W, Dotzer F, Huber K, Dirschinger J, Seyfarth M, Schomig A, Kastrati A, Mehilli J (2010) One-year clinical outcomes with abciximab in acute myocardial infarction: results of the BRAVE-3 randomized trial. Clin Res Cardiol 99(12):795–802. doi:10.1007/s00392-010-0185-z
Bellandi F, Maioli M, Gallopin M, Toso A, Dabizzi RP (2004) Increase of myocardial salvage and left ventricular function recovery with intracoronary abciximab downstream of the coronary occlusion in patients with acute myocardial infarction treated with primary coronary intervention. Catheter Cardiovasc Interv 62(2):186–192. doi:10.1002/ccd.20041
Eitel I, Friedenberger J, Fuernau G, Dumjahn A, Desch S, Schuler G, Thiele H (2011) Intracoronary versus intravenous bolus abciximab application in patients with ST-elevation myocardial infarction undergoing primary percutaneous coronary intervention: 6-month effects on infarct size and left ventricular function : The randomised Leipzig Immediate PercutaneouS Coronary Intervention Abciximab i.v. versus i.c. in ST-Elevation Myocardial Infarction Trial (LIPSIAbciximab-STEMI). Clin Res Cardiol 100(5):425–432. doi:10.1007/s00392-010-0260-5
Gu YL, Kampinga MA, Wieringa WG, Fokkema ML, Nijsten MW, Hillege HL, van den Heuvel AF, Tan ES, Pundziute G, van der Werf R, Hoseyni Guyomi S, van der Horst IC, Zijlstra F, de Smet BJ (2010) Intracoronary versus intravenous administration of abciximab in patients with ST-segment elevation myocardial infarction undergoing primary percutaneous coronary intervention with thrombus aspiration: the comparison of intracoronary versus intravenous abciximab administration during emergency reperfusion of ST-segment elevation myocardial infarction (CICERO) trial. Circulation 122(25):2709–2717. doi:10.1161/CIRCULATIONAHA.110.002741
Thiele H, Schindler K, Friedenberger J, Eitel I, Furnau G, Grebe E, Erbs S, Linke A, Mobius-Winkler S, Kivelitz D, Schuler G (2008) Intracoronary compared with intravenous bolus abciximab application in patients with ST-elevation myocardial infarction undergoing primary percutaneous coronary intervention: the randomized Leipzig immediate percutaneous coronary intervention abciximab IV versus IC in ST-elevation myocardial infarction trial. Circulation 118(1):49–57. doi:10.1161/CIRCULATIONAHA.107.747642
Thiele H, Wohrle J, Neuhaus P, Brosteanu O, Sick P, Prondzinsky R, Birkemeyer R, Wiemer M, Kerber S, Schuehlen H, Kleinertz K, Axthelm C, Zimmermann R, Rittger H, Braun-Dullaeus RC, Lauer B, Burckhardt W, Ferrari M, Bergmann MW, Hambrecht R, Schuler G (2010) Intracoronary compared with intravenous bolus abciximab application during primary percutaneous coronary intervention: design and rationale of the Abciximab Intracoronary versus intravenously Drug Application in ST-Elevation Myocardial Infarction (AIDA STEMI) trial. Am Heart J 159(4):547–554. doi:10.1016/j.ahj.2009.12.038
Sibbing D, Braun S, Jawansky S, Vogt W, Mehilli J, Schomig A, Kastrati A, von Beckerath N (2008) Assessment of ADP-induced platelet aggregation with light transmission aggregometry and multiple electrode platelet aggregometry before and after clopidogrel treatment. Thromb Haemost 99(1):121–126. doi:10.1160/TH07-07-0478
Sibbing D, Braun S, Morath T, Mehilli J, Vogt W, Schomig A, Kastrati A, von Beckerath N (2009) Platelet reactivity after clopidogrel treatment assessed with point-of-care analysis and early drug-eluting stent thrombosis. J Am Coll Cardiol 53(10):849–856. doi:10.1016/j.jacc.2008.11.030
Toth O, Calatzis A, Penz S, Losonczy H, Siess W (2006) Multiple electrode aggregometry: a new device to measure platelet aggregation in whole blood. Thromb Haemost 96(6):781–788 pii: 06120781
Seyfarth HJ, Koksch M (2004) Fibrinogen receptor antagonists induce conformational changes of the human platelet glycoprotein IIb. Cytometry B Clin Cytom 62(1):14–24. doi:10.1002/cyto.b.20026
Deibele AJ, Jennings LK, Tcheng JE, Neva C, Earhart AD, Gibson CM (2010) Intracoronary eptifibatide bolus administration during percutaneous coronary revascularization for acute coronary syndromes with evaluation of platelet glycoprotein IIb/IIIa receptor occupancy and platelet function: the Intracoronary Eptifibatide (ICE) Trial. Circulation 121(6):784–791. doi:10.1161/CIRCULATIONAHA.109.882746
Collet JP, Montalescot G, Lesty C, Soria J, Mishal Z, Thomas D, Soria C (2001) Disaggregation of in vitro preformed platelet-rich clots by abciximab increases fibrin exposure and promotes fibrinolysis. Arterioscler Thromb Vasc Biol 21(1):142–148
Marciniak SJ Jr, Mascelli MA, Furman MI, Michelson AD, Jakubowski JA, Jordan RE, Marchese PJ, Frelinger AL (2002) An additional mechanism of action of abciximab: dispersal of newly formed platelet aggregates. Thromb Haemost 87(6):1020–1025
Cox AD, Devine DV (1994) Factor XIIIa binding to activated platelets is mediated through activation of glycoprotein IIb-IIIa. Blood 83(4):1006–1016
Romagnoli E, Burzotta F, Trani C, Biondi-Zoccai GG, Giannico F, Crea F (2007) Rationale for intracoronary administration of abciximab. J Thromb Thrombolysis 23(1):57–63. doi:10.1007/s11239-006-9000-0
Mehilli J, Kastrati A, Schulz S, Frungel S, Nekolla SG, Moshage W, Dotzer F, Huber K, Pache J, Dirschinger J, Seyfarth M, Martinoff S, Schwaiger M, Schomig A (2009) Abciximab in patients with acute ST-segment-elevation myocardial infarction undergoing primary percutaneous coronary intervention after clopidogrel loading: a randomized double-blind trial. Circulation 119(14):1933–1940. doi:10.1161/CIRCULATIONAHA.108.818617
Stone GW, Witzenbichler B, Guagliumi G, Peruga JZ, Brodie BR, Dudek D, Kornowski R, Hartmann F, Gersh BJ, Pocock SJ, Dangas G, Wong SC, Kirtane AJ, Parise H, Mehran R (2008) Bivalirudin during primary PCI in acute myocardial infarction. N Engl J Med 358(21):2218–2230. doi:10.1056/NEJMoa0708191
Van’t Hof AW, Ten Berg J, Heestermans T, Dill T, Funck RC, van Werkum W, Dambrink JH, Suryapranata H, van Houwelingen G, Ottervanger JP, Stella P, Giannitsis E, Hamm C (2008) Prehospital initiation of tirofiban in patients with ST-elevation myocardial infarction undergoing primary angioplasty (On-TIME 2): a multicentre, double-blind, randomised controlled trial. Lancet 372(9638):537–546. doi:10.1016/S0140-6736(08)61235-0
Saraf S, Ong PJ, Gorog DA (2008) ClearWay RX—rapid exchange therapeutic perfusion catheter. EuroIntervention 3(5):639–642 pii: EIJV3I5A114
Prati F, Capodanno D, Pawlowski T, Ramazzotti V, Albertucci M, La Manna A, Di Salvo M, Gil RJ, Tamburino C (2010) Local delivery versus intracoronary infusion of abciximab in patients with acute coronary syndromes. JACC Cardiovasc Interv 3(9):928–934. doi:10.1016/j.jcin.2010.05.017
Gibson CM, Maehara A, Lansky AJ, Wohrle J, Stuckey T, Dave R, Cox D, Grines C, Dudek D, Steg G, Parise H, Wolff SD, Cristea E, Stone GW (2011) Rationale and design of the INFUSE-AMI study: a 2 × 2 factorial, randomized, multicenter, single-blind evaluation of intracoronary abciximab infusion and aspiration thrombectomy in patients undergoing percutaneous coronary intervention for anterior ST-segment elevation myocardial infarction. Am Heart J 161 (3):478–486 e477. doi:10.1016/j.ahj.2010.10.006
Bonello L, Tantry US, Marcucci R, Blindt R, Angiolillo DJ, Becker R, Bhatt DL, Cattaneo M, Collet JP, Cuisset T, Gachet C, Montalescot G, Jennings LK, Kereiakes D, Sibbing D, Trenk D, Van Werkum JW, Paganelli F, Price MJ, Waksman R, Gurbel PA (2010) Consensus and future directions on the definition of high on-treatment platelet reactivity to adenosine diphosphate. J Am Coll Cardiol 56(12):919–933. doi:10.1016/j.jacc.2010.04.047
National Kidney Foundation (2002) K/DOQI clinical practice guidelines for chronic kidney disease: evaluation, classification, stratification. Am J Kidney Dis 39(1):S1–S266 pii: S0272638602093563
Gibson CM, de Lemos JA, Murphy SA, Marble SJ, McCabe CH, Cannon CP, Antman EM, Braunwald E (2001) Combination therapy with abciximab reduces angiographically evident thrombus in acute myocardial infarction: a TIMI 14 substudy. Circulation 103(21):2550–2554
Acknowledgments
The AIDA-STEMI trial is supported by an unrestricted grant from Lilly Deutschland GmbH.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Desch, S., Siegemund, A., Scholz, U. et al. Platelet inhibition and GP IIb/IIIa receptor occupancy by intracoronary versus intravenous bolus administration of abciximab in patients with ST-elevation myocardial infarction. Clin Res Cardiol 101, 117–124 (2012). https://doi.org/10.1007/s00392-011-0372-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00392-011-0372-6