Abstract
Background
Postoperative mortality after resection of colorectal cancer is an important issue. The aim of this study was to assess early postoperative mortality in a well-defined French population.
Methods
Data on 30- and 90-day postoperative mortality after resection for colorectal cancer were extracted from the digestive cancer registry of Burgundy. Time trends of postoperative mortality between 1989 and 2013 were described for the large population. Case-control studies (death within 30 or 90 days = cases, alive at 90 days = controls) focused on the association between postoperative mortality and surgical approach, obesity and other comorbidities over the last [2010–2013] period, using conditional logistic regressions.
Results
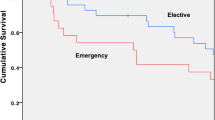
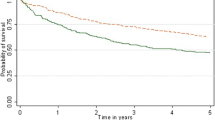
Among the 11,448 concerned patients, 30- and 90-day postoperative mortalities were 4.9 and 7.2%. Thirty-day operative mortality decreased from 7.2% (1989–1993) to 4.4% (2010–2013; p < 0.001) for colon cancer and from 4.2 to 3.3% for rectal cancer (NS). Diagnosis before 1997, male gender, advanced age, emergency surgery and palliative resection were associated with a significantly higher 30- and 90-day mortality rate. The univariate risk of mortality was two to three times higher for conventional open laparotomy and conversion than for laparoscopy-assisted surgery. The surgical approach was no longer significant in multivariate analysis. Emergency surgery and comorbidities were associated with higher 30- and 90-day postoperative mortality, whereas obesity was not specific.
Conclusion
Postoperative mortality after colorectal resection decreased over time. Surgical approach had no influence on early mortality. Improvement in the management of the elderly and patients with comorbidities is a challenge to reduce postoperative mortality in the future.
Similar content being viewed by others
References
Binder-Foucard F, Bossard N, Delafosse P, Belot A, Woronoff AS, Remontet L (2014) Cancer incidence and mortality in France over the 1980-2012 period: solid tumors. Rev Epidemiol Sante Publique 62:95–108
Buunen M, Veldkamp R, Hop WC, Kuhry E, Jeekel J, Haglind E, Pahlman L, Cuesta MA, Msika S, Morino M, Lacy A, Bonjer HJ (2009) Survival after laparoscopic surgery versus open surgery for colon cancer: long-term outcome of a randomised clinical trial. Lancet Oncol 10:44–52
Lacy AM, Garcia-Valdecasas JC, Delgado S, Castells A, Taura P, Pique JM, Visa J (2002) Laparoscopy-assisted colectomy versus open colectomy for treatment of non-metastatic colon cancer: a randomised trial. Lancet 359:2224–2229
Veldkamp R, Kuhry E, Hop WC, Jeekel J, Kazemier G, Bonjer HJ, Haglind E, Pahlman L, Cuesta MA, Msika S, Morino M, Lacy AM (2005) Laparoscopic surgery versus open surgery for colon cancer: short-term outcomes of a randomised trial. Lancet Oncol 6:477–484
Tyczynski J, Demaret E, Parkin M (2003) The ENCR recommendations. Standards and guidelines for cancer registration in Europe. IARC Technical Publication n°40, Lyon
Fritz A, Percy C, Jack A, Shanmugaratnam K, Sobin L, Parkin DM, Whelan S , editors (2000) International Classification of Diseases for Oncology, 3rd edn. World Health Organization, Geneva
Charlson ME, Pompei P, Ales KL, MacKenzie CRA (1987) New method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383
Iversen LH, Ingeholm P, Gogenur I, Laurberg S (2014) Major reduction in 30-day mortality after elective colorectal cancer surgery: a nationwide population-based study in Denmark 2001-2011. Ann Surg Oncol 21:2267–2273
Morris EJ, Taylor EF, Thomas JD, Quirke P, Finan PJ, Coleman MP, Rachet B, Forman D (2011) Thirty-day postoperative mortality after colorectal cancer surgery in England. Gut 60:806–813
Aquina CT, Mohile SG, Tejani MA, Becerra AZ, Xu Z, Hensley BJ, Arsalani-Zadeh R, Boscoe FP, Schymura MJ, Noyes K, Monson JR, Fleming FJ (2017) The impact of age on complications, survival, and cause of death following colon cancer surgery. Br J Cancer 116:389–397
Partridge JS, Harari D, Martin FC, Dhesi JK (2014) The impact of pre-operative comprehensive geriatric assessment on postoperative outcomes in older patients undergoing scheduled surgery: a systematic review. Anaesthesia 69(Suppl 1):8–16
Panis Y, Maggiori L, Caranhac G, Bretagnol F, Vicaut E (2011) Mortality after colorectal cancer surgery: a French survey of more than 84,000 patients. Ann Surg 254:738–743 discussion 43-4
Damhuis RA, Wijnhoven BP, Plaisier PW, Kirkels WJ, Kranse R, van Lanschot JJ (2012) Comparison of 30-day, 90-day and in-hospital postoperative mortality for eight different cancer types. Br J Surg 99:1149–1154
Desgrippes R, Bouvier V, Delafosse P, Robaszkiewicz M, Molinie F, Tretarre B, Lepage C, Faivre J, Jooste V, Bouvier AM (2014) Management of rectal cancer in France in a well-defined population. Eur J Gastroenterol Hepatol 26:743–747
Guren MG, Korner H, Pfeffer F, Myklebust TA, Eriksen MT, Edna TH, Larsen SG, Knudsen KO, Nesbakken A, Wasmuth HH, Vonen B, Hofsli E, Faerden AE, Braendengen M, Dahl O, Steigen SE, Johansen MJ, Lindsetmo RO, Drolsum A, Tollali G, Dorum LM, Moller B, Wibe A (2015) Nationwide improvement of rectal cancer treatment outcomes in Norway, 1993-2010. Acta Oncol 54:1714–1722
Matthiessen P, Hallbook O, Rutegard J, Sjodahl R (2006) Population-based study of risk factors for postoperative death after anterior resection of the rectum. Br J Surg 93:498–503
Mamidanna R, Burns EM, Bottle A, Aylin P, Stonell C, Hanna GB, Faiz O (2012) Reduced risk of medical morbidity and mortality in patients selected for laparoscopic colorectal resection in England: a population-based study. Arch Surg 147:219–227
Acknowledgments
The authors thank all the private and public physicians, specialists and pathologists for their collaboration and the French Public Health Institute (SpF) and the National Cancer Institute (INCa) for supporting the Registry.
Funding
The Registry is supported by the French Public Health Institute (SpF) and the National Cancer Institute (INCa).
Author information
Authors and Affiliations
Contributions
SM was responsible for study coordination, acquisition of data, interpretation of data and manuscript writing. VJ was responsible for the statistical analysis and involved in the interpretation of data and drafting of the manuscript. CG was involved in the interpretation of data and manuscript writing. JF was involved in the interpretation of data and manuscript writing. AD was involved in the interpretation of data and critical revision of the manuscript. AMB was responsible for the acquisition of data and involved in study design and manuscript writing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Rights and permissions
About this article
Cite this article
Manfredi, S., Jooste, V., Gay, C. et al. Time trends in colorectal cancer early postoperative mortality. A French 25-year population-based study. Int J Colorectal Dis 32, 1725–1731 (2017). https://doi.org/10.1007/s00384-017-2918-1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-017-2918-1