Abstract
Purpose
Hospital factors along with various patient and surgeon factors are considered to affect the prognosis of colorectal cancer. Hospital volume is well known, but little is known regarding other hospital factors.
Methods
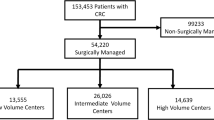
We reviewed data on 853 patients with stage IV colorectal cancer who underwent elective palliative primary tumor resection between January 2006 and December 2007. To detect the hospital factors that could influence the prognosis of incurable colorectal cancer, the relationships between patient/hospital factors and overall survival were analyzed. Among hospital factors, hospital type (Group A: university hospital or cancer center; Group B: community hospital), hospital volume, and number of colorectal surgeons were examined.
Results
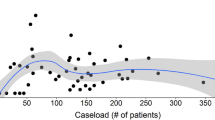
In univariate analysis, Group A hospitals showed significantly better prognosis than Group B hospitals (p = 0.034), while hospital volume and number of colorectal surgeons were not associated with overall survival. After adjustment for patient factors in multivariate analysis, hospital type was significantly associated with overall survival (hazard ratio: 1.31; 95 % confidence interval: 1.05–1.63; p = 0.016). However, there was no significant difference in short-term outcomes between hospital types.
Conclusions
Hospital type was identified as a hospital factor that possibly affects the prognosis of stage IV colorectal cancer patients.

Similar content being viewed by others
References
Gort M, Otter R, Plukker JT, Broekhuis M, Klazinga NS (2010) Actionable indicators for short and long term outcomes in rectal cancer. Eur J Cancer 46:1808–1814
Zheng Z, Hanna N, Onukwugha E, Bikov KA, Mullins CD (2014) Hospital center effect for laparoscopic colectomy among elderly stage I-III colon cancer patients. Ann Surg 259:924–929
Wibe A, Eriksen MT, Syse A, Tretli S, Myrvold HE, Soreide O (2005) Effect of hospital caseload on long-term outcome after standardization of rectal cancer surgery at a national level. Br J Surg 92:217–224
Salz T, Sandler RS (2008) The effect of hospital and surgeon volume on outcomes for rectal cancer surgery. Clin Gastroenterol Hepatol 6:1185–1193
Mathis KL, Nelson H, Pemberton JH, Haddock MG, Gunderson LL (2008) Unresectable colorectal cancer can be cured with multimodality therapy. Ann Surg 248:592–598
Ronnekleiv-Kelly SM, Kennedy GD (2011) Management of stage IV rectal cancer: palliative options. World J Gastroenterol 17:835–847
Andersen C, Rorth M, Ejlertsen B, Stage M, Moller T, Midtgaard J et al (2013) The effects of a six-week supervised multimodal exercise intervention during chemotherapy on cancer-related fatigue. Eur J Oncol Nurs 17:331–339
Cheville AL, Kollasch J, Vandenberg J, Shen T, Grothey A, Gamble G et al (2013) A home-based exercise program to improve function, fatigue, and sleep quality in patients with Stage IV lung and colorectal cancer: a randomized controlled trial. J Pain Symptom Manag 45:811–821
Hida K, Hasegawa S, Kinjo Y, Yoshimura K, Inomata M, Ito M et al (2012) Open versus laparoscopic resection of primary tumor for incurable stage IV colorectal cancer: a large multicenter consecutive patients cohort study. Ann Surg 255:929–934
Watanabe T, Itabashi M, Shimada Y, Tanaka S, Ito Y, Ajioka Y et al (2012) Japanese Society for Cancer of the Colon and Rectum (JSCCR) guidelines 2010 for the treatment of colorectal cancer. Int J Clin Oncol 17:1–29
Jan S, Slap G, Smith-Whitley K, Dai D, Keren R, Rubin DM (2013) Association of hospital and provider types on sickle cell disease outcomes. Pediatrics 132:854–861
Gort M, Broekhuis M, Otter R, Klazinga NS (2007) Improvement of best practice in early breast cancer: actionable surgeon and hospital factors. Breast Cancer Res Treat 102:219–226
van der Geest LG, van Meer S, Schrier JG, Ijzermans JN, Klumpen HJ, van Erpecum KJ, et al. (2015) Survival in relation to hospital type after resection or sorafenib treatment for hepatocellular carcinoma in The Netherlands. Clin Res Hepatol Gastroenterol [Epub ahead of print]
Hicks CW, Wick EC, Canner JK, Black JH 3rd, Arhuidese I, Qazi U et al (2015) Hospital-level factors associated with mortality after endovascular and open abdominal aortic aneurysm repair. JAMA Surg 150:632–636
Elferink MA, Wouters MW, Krijnen P, Lemmens VE, Jansen-Landheer ML, van de Velde CJ et al (2010) Disparities in quality of care for colon cancer between hospitals in the Netherlands. Eur J Surg Oncol 36:S64–S73
Selby P, Gillis C, Haward R (1996) Benefits from specialised cancer care. Lancet 348:313–318
Costi R, Di Mauro D, Giordano P, Leonardi F, Veronesi L, Sarli L et al (2010) Impact of palliative chemotherapy and surgery on management of stage IV incurable colorectal cancer. Ann Surg Oncol 17:432–440
Platell C, Ng S, O’Bichere A, Tebbutt N (2011) Changing management and survival in patients with stage IV colorectal cancer. Dis Colon Rectum 54:214–219
McLeod A (1999) Variation in the provision of chemotherapy for colorectal cancer. J Epidemiol Community Health 53:775–781
Nakano T (2004) Status of Japanese radiation oncology. Radiat Med 22:17–19
de Azambuja E, Ameye L, Paesmans M, Zielinski CC, Piccart-Gebhart M, Preusser M (2014) The landscape of medical oncology in Europe by 2020. Ann Oncol 25:525–528
van Ryn M, Phelan SM, Arora NK, Haggstrom DA, Jackson GL, Zafar SY et al (2014) Patient-reported quality of supportive care among patients with colorectal cancer in the Veterans Affairs Health Care System. J Clin Oncol 32:809–815
Hu CY, Bailey CE, You YN, Skibber JM, Rodriguez-Bigas MA, Feig BW et al (2015) Time trend analysis of primary tumor resection for stage IV colorectal cancer: less surgery, improved survival. JAMA Surg 150:245–251
Stillwell AP, Buettner PG, Ho YH (2010) Meta-analysis of survival of patients with stage IV colorectal cancer managed with surgical resection versus chemotherapy alone. World J Surg 34:797–807
Acknowledgments
The authors completed this study in collaboration with the following in data collection: Seiichiro Yamamoto (National Cancer Center Hospital), Hiroya Kuroyanagi (Cancer Institute ARIAKE Hospital), Atsushi Ikeda (Kitasato University), Koki Otsuka (Iwate Medical University), Shungo Endo (Showa University Northern Yokohama Hospital), Masaaki Ito (National Cancer Hospital East), Michitoshi Goto (Juntendo University), Shuji Saito (Shizuoka Cancer Center), Akiyoshi Kanazawa (Osaka Red Cross Hospital), Tadashi Suda (St. Marianna University), Hisanaga Horie (Jichi Medical University), Yousuke Kinjo (Kyoto University), Yoshiro Kubo (Shikoku Cancer Center), Koichi Hanai (Fujita Health University), Hiroyuki Bando (Ishikawa Prefectural Central Hospital), Yosuke Fukunaga (Bell-land General Hospital), Yasuhiro Munakata (Nagano Municipal Hospital), Toshimasa Yatsuoka (Saitama Cancer Center), Takashi Yamaguchi (Kyoto Medical Center), Hirotoshi Hasegawa (Keio University), Hitoshi Idani and Kanyu Nakano (Fukuyama Municipal Hospital), Shoichi Fujii (Yokohama City University), Ichiro Takemasa (Osaka University), Toshiaki Watanabe (Teikyo University), Yoshihisa Saida (Toho University Ohashi Medical Center), Tomohisa Furuhata (Sapporo Medical University), Kunihiko Nagakari (Juntendo University Urayasu Hospital), Ichio Suzuka (Kagawa Prefectural Central Hospital), Shigeki Yamaguchi (Saitama Medical University), Yoshiaki Kuriu (Kyoto Prefectural University), Kohei Murata (Suita Municipal Hospital), Kiyoshi Maeda (Osaka City University), Takeshi Ueki (Kyusyu University), Masafumi Inomata (Oita University), Hiroshi Hirukawa (Tachikawa General Hospital), Takao Ichihara (Nishinomiya Municipal Central Hospital), Kazuya Okamoto (Fujinomiya City General Hospital), Takao Hinoi (Hiroshima University), and Katsuichi Matsuo (Fukuoka University).
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Human and animal rights and informed consent
For this type of study formal consent is not required.
Rights and permissions
About this article
Cite this article
Hoshino, N., Hasegawa, S., Hida, K. et al. Influence of hospital type on survival in stage IV colorectal cancer. Int J Colorectal Dis 31, 1443–1449 (2016). https://doi.org/10.1007/s00384-016-2611-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-016-2611-9