Abstract
Aim
The aim of this study is to compare surgical, functional, physiologic outcomes and QOL after low anterior resection (LAR) with andside-to-end or straight colorectal anastomosis.
Method
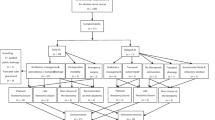
Between 2012 and 2015, 86 patients with mid and low rectal tumors were enrolled into randomized trial. Wexner score, number of defecations, use of antidiarrheal medicine or laxatives, enemas, pads, episodes of nocturnal incontinence, and urgency were recorded. The Fecal Incontinence Quality of Life (FIQL) scale was used for assessment of QOL. Anal manometry and volumetric examination were performed.
Results
Six patients were excluded from the study. There was no mortality. The morbidity rate was 6 (14.6 %) for side-to-end vs. 8 (20.0 %) for straight anastomosis (p = 0.57). The median Wexner score was 5 vs. 6 (p = 0.033), 4 vs. 5 (p = 0.006), and 2 vs. 3 (p = 0.1) at 1, 3, and 6 months after stoma reversal, respectively. Side-to-end anastomosis resulted in a fewer mean numbers of bowel movements per day at the same check points of follow-up: 5.8 ± 0.14 vs. 6.4 ± 0.15 (p = 0.006), 3.7 ± 0.1 vs. 4.2 ± 0.1 (p = 0.003), and 2.5 ± 0.1 vs. 3.0 ± 0.10 (p = 0.0002), correspondingly. Maximal tolerated volume was higher for side-to-end anastomosis at 3 and 6 months of follow-up: 152.0 vs. 137.8 cm3 (p = 0.002) and 180.5 vs. 167.0 cm3 (p = 0.006), respectively. Better FIQL score was found at 1 and 3 months in the side-to-end group.
Conclusion
Better functional outcomes and QOL were observed in a short period after stoma closure, but at 6 months of follow-up, the only benefit of side-to-end anastomosis was a lower number of bowel movements.





Similar content being viewed by others
References
Hida J, Yasutomi M, Maruyama T et al (1998) Indications for colonic J-pouch reconstruction after anterior resection for rectal cancer: determining the optimum level of anastomosis. Dis Colon Rectum 41(5):558–563
Bryant CL, Lunniss PJ, Knowles CH et al (2012) Anterior resection syndrome. Lancet Oncol 13(9):e403–e408
Emmertsen KJ, Laurberg S (2012) Low anterior resection syndrome score: development and validation of a symptom-based scoring system for bowel dysfunction after low anterior resection for rectal cancer. Ann Surg 255(5):922–928
Juul T, Ahlberg M, Biondo S, Espin E et al (2014) Low anterior resection syndrome and quality of life: an international multicenter study. Dis Colon Rectum 57(5):585–591
Lazorthes F, Fages P, Chiotasso P, Lemozy J, Bloom E (1986) Resection of the rectum with construction of a colonic reservoir and colo-anal anastomosis for carcinoma of the rectum. Br J Surg 73(2):136–138
Fazio VW, Mantyh CR, Hull TL (2000) Colonic “coloplasty”: novel technique to enhance low colorectal or coloanal nastomosis. Dis Colon Rectum 43(10):1448–1450
Huber FT, Herter B, Siewert JR (1999) Colonic pouch vs. side-to-end anastomosis in low anterior resection. Dis Colon Rectum 42(7):896–902
Brown CJ, Fenech DS, McLeod RS (2008) Reconstructive techniques after rectal resection for rectal cancer. Cochrane Database Syst Rev 16(2):CD006040
Rockwood TH, Church JM, Fleshman JW, Kane RL et al (1999) Patient and surgeon ranking of the severity of symptoms associated with fecal incontinence: the fecal incontinence severity index. Dis Colon Rectum 42(12):1525–1532
Rockwood TH, Church JM, Fleshman JW, Kane RL et al (2000) Fecal Incontinence Quality of Life Scale: quality of life instrument for patients with fecal incontinence. Dis Colon Rectum 43:9–16
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240(2):205–213
Rahbari NN, Weitz J, Hohenberger W, Heald RJ et al (2010) Definition and grading of anastomotic leakage following anterior resection of the rectum: a proposal by the International Study Group of Rectal Cancer. Surgery 147(3):339–351
Konanz J, Herrle F, Weiss C, Post S, Kienle P (2013) Quality of life of patients after low anterior, intersphincteric, and abdominoperineal resection for rectal cancer--a matched-pair analysis. Int J Colorectal Dis 28(5):679–688
Digennaro R, Tondo M, Cuccia F, Giannini I et al (2013) Coloanal anastomosis or abdominoperineal resection for very low rectal cancer: what will benefit, the surgeon’s pride or the patient’s quality of life? Int J Colorectal Dis 28(7):949–957
Doeksen A, Bakx R, Vincent A, van Tets WF et al (2012) J-pouch versus side-to-end coloanal anastomosis after preoperative radiotherapy and total mesorectal excision for rectal cancer: a multicentre randomized trial. Colorectal Dis 14(6):705–713
Huttner FJ, Tenckhoff S, Jensen K, Uhlmann L et al (2015) Meta-analysis of reconstruction techniques after low anterior resection for rectal cancer. Br J Surg 102(7):735–745
Bregendahl S, Emmertsen KJ, Lous J, Lauberg S (2013) Bowel dysfunction after anterior resection with and without neoadjuvant therapy for rectal cancer: a population-based cross-sectional study. Colorectal Dis 15(9):1130–1139
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
It was institutional trial with no external funding. The State Scientific Center of Coloproctology registration number of the trial is #012/2012. All authors contributed to the design of the study, acquisition of data, analysis of results, and revised intellectual content of the manuscript.
Conflict of interest
The authors of the article have no financial or other conflicts of interest to disclose.
Ethical approval
All procedures performed in studies involving human participants were done in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Rights and permissions
About this article
Cite this article
Rybakov, E.G., Pikunov, D.Y., Fomenko, O.Y. et al. Side-to-end vs. straight stapled colorectal anastomosis after low anterior resection: results of randomized clinical trial. Int J Colorectal Dis 31, 1419–1426 (2016). https://doi.org/10.1007/s00384-016-2608-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-016-2608-4