Abstract
Objective
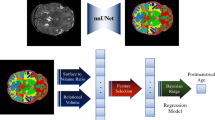
To develop a postmenstrual age (PMA) prediction model based on segmentation volume and to evaluate the brain maturation index using the proposed model.
Methods
Neonatal brain MRIs without clinical illness or structural abnormalities were collected from four datasets from the Developing Human Connectome Project, the Catholic University of Korea, Hammersmith Hospital (HS), and Dankook University Hospital (DU). T1- and T2-weighted images were used to train a brain segmentation model. Another model to predict the PMA of neonates based on segmentation data was developed. Accuracy was assessed using mean absolute error (MAE), root mean square error (RMSE), and mean error (ME). The brain maturation index was calculated as the difference between the PMA predicted by the model and the true PMA, and its correlation with postnatal age was analyzed.
Results
A total of 247 neonates (mean gestation age 37 ± 4 weeks; range 24–42 weeks) were included. Thirty-one features were extracted from each neonate and the three most contributing features for PMA prediction were the right lateral ventricle, left caudate, and corpus callosum. The predicted and true PMA were positively correlated (coefficient = 0.88, p < .001). MAE, RMSE, and ME of the external dataset of HS and DU were 1.57 and 1.33, 1.79 and 1.37, and 0.37 and 0.06 weeks, respectively. The brain maturation index negatively correlated with postnatal age (coefficient = − 0.24, p < .001).
Conclusion
A model that calculates the regional brain volume can predict the PMA of neonates, which can then be utilized to show the brain maturation degree.
Clinical relevance statement
A brain maturity index based on regional volume of neonate’s brain can be used to measure brain maturation degree, which can help identify the status of early brain development.
Key Points
• Neonatal brain MRI segmentation model could be used to assess neonatal brain maturation status.
• A postmenstrual age (PMA) prediction model was developed based on a neonatal brain MRI segmentation model.
• The brain maturation index, derived from the PMA prediction model, enabled the estimation of the neonatal brain maturation status.






Similar content being viewed by others
Abbreviations
- CU:
-
The Catholic University of Korea, Eunpyeong St. Mary’s Hospital
- dHCP:
-
Developing Human Connectome Project
- DU:
-
Dankook University Hospital
- HS:
-
Hammersmith Hospital
- MAE:
-
Mean absolute error
- ME:
-
Mean error
- PMA:
-
Postmenstrual age
- RMSE:
-
Root mean square error
- ROIs:
-
Regions of interest
- XGBoost:
-
Extreme gradient boosting
References
Gilmore JH, Knickmeyer RC, Gao W (2018) Imaging structural and functional brain development in early childhood. Nat Rev Neurosci 19:123–137
Roze E, Benders MJ, Kersbergen KJ et al (2015) Neonatal DTI early after birth predicts motor outcome in preterm infants with periventricular hemorrhagic infarction. Pediatr Res 78:298–303. https://doi.org/10.1038/pr.2015.94
Guo T, Duerden EG, Adams E et al (2017) Quantitative assessment of white matter injury in preterm neonates. Neurology 88:614–622. https://doi.org/10.1212/WNL.0000000000003606
Peterson BS, Anderson AW, Ehrenkranz R et al (2003) Regional brain volumes and their later neurodevelopmental correlates in term and preterm infants. Pediatrics 111:939–948
Gui L, Loukas S, Lazeyras F, Hüppi PS, Meskaldji DE, Borradori Tolsa C (2019) Longitudinal study of neonatal brain tissue volumes in preterm infants and their ability to predict neurodevelopmental outcome. Neuroimage 185:728–741. https://doi.org/10.1016/j.neuroimage.2018.06.034
Thompson DK, Warfield SK, Carlin JB et al (2007) Perinatal risk factors altering regional brain structure in the preterm infant. Brain 130:667–677. https://doi.org/10.1093/brain/awl277
Brouwer MJ, de Vries LS, Groenendaal F et al (2012) New reference values for the neonatal cerebral ventricles. Radiology 262:224–233
Chau V, Synnes A, Grunau RE, Poskitt KJ, Brant R, Miller SP (2013) Abnormal brain maturation in preterm neonates associated with adverse developmental outcomes. Neurology 81:2082–2089. https://doi.org/10.1212/01.wnl.0000437298.43688.b9
Zöllei L, Iglesias JE, Ou Y, Grant PE, Fischl B (2020) Infant FreeSurfer: an automated segmentation and surface extraction pipeline for T1-weighted neuroimaging data of infants 0–2 years. Neuroimage 218:116946
Mewes AUJ, Hüppi PS, Als H et al (2006) Regional brain development in serial magnetic resonance imaging of low-risk preterm infants. Pediatrics 118:23–33. https://doi.org/10.1542/peds.2005-2675
Xue H, Srinivasan L, Jiang S et al (2007) Automatic segmentation and reconstruction of the cortex from neonatal MRI. Neuroimage 38:461–477. https://doi.org/10.1016/j.neuroimage.2007.07.030
Chen JV, Chaudhari G, Hess CP et al (2022) Deep learning to predict neonatal and infant brain age from myelination on brain MRI scans. Radiology. https://doi.org/10.1148/radiol.211860
Taoudi-Benchekroun Y, Christiaens D, Grigorescu I et al (2022) Predicting age and clinical risk from the neonatal connectome. Neuroimage 257. https://doi.org/10.1016/j.neuroimage.2022.119319
Smith SM, Vidaurre D, Alfaro-Almagro F, Nichols TE, Miller KL (2019) Estimation of brain age delta from brain imaging. Neuroimage 200:528–539. https://doi.org/10.1016/j.neuroimage.2019.06.017
Liem F, Varoquaux G, Kynast J et al (2017) Predicting brain-age from multimodal imaging data captures cognitive impairment. Neuroimage 148:179–188. https://doi.org/10.1016/j.neuroimage.2016.11.005
Makropoulos A, Robinson EC, Schuh A et al (2018) The developing human connectome project: a minimal processing pipeline for neonatal cortical surface reconstruction. Neuroimage 173:88–112. https://doi.org/10.1016/j.neuroimage.2018.01.054
Gousias IS, Edwards AD, Rutherford MA et al (2012) Magnetic resonance imaging of the newborn brain: manual segmentation of labelled atlases in term-born and preterm infants. Neuroimage 62:1499–1509. https://doi.org/10.1016/j.neuroimage.2012.05.083
Hughes EJ, Winchman T, Padormo F et al (2017) A dedicated neonatal brain imaging system. Magn Reson Med 78:794–804. https://doi.org/10.1002/mrm.26462
Makropoulos A, Gousias IS, Ledig C et al (2014) Automatic whole brain MRI segmentation of the developing neonatal brain. IEEE Trans Med Imaging 33:1818–1831. https://doi.org/10.1109/TMI.2014.2322280
Zhou Z, Rahman Siddiquee MM, Tajbakhsh N, Liang J (2018) UNet++: a nested u-net architecture for medical image segmentation. In: Stoyanov D, Taylor Z, Carneiro G et al (eds) Deep learning in medical image analysis and multimodal learning for clinical decision support. Springer International Publishing, Cham, pp 3–11
Chen T, Guestrin C (2016) XGBoost: a scalable tree boosting system. In: Krishnapuram B, Shah M, Smola A, Aggarwal C, Shen D, Rastogi R (eds) Proceedings of the 22nd ACM SIGKDD international conference on knowledge discovery and data mining. ACM, New York, pp 785–794
Dosenbach NUF, Nardos B, Cohen AL et al (2010) Prediction of individual brain maturity using fMRI. Science 329:1358–1361
Brown CJ, Moriarty KP, Miller SP et al (2017) Prediction of brain network age and factors of delayed maturation in very preterm infants. In: Medical Image Computing and Computer Assisted Intervention− MICCAI 2017: 20th International Conference, Quebec City, QC, Canada, September 11–13, 2017, Proceedings, Part I 20. Springer, pp 84–91
Galdi P, Blesa M, Stoye DQ et al (2020) Neonatal morphometric similarity mapping for predicting brain age and characterizing neuroanatomic variation associated with preterm birth. Neuroimage Clin 25:102195
Zhang W, Li R, Deng H et al (2015) Deep convolutional neural networks for multi-modality isointense infant brain image segmentation. Neuroimage 108:214–224. https://doi.org/10.1016/j.neuroimage.2014.12.061
Sun Y, Gao K, Wu Z et al (2021) Multi-site infant brain segmentation algorithms: the iSeg-2019 Challenge. IEEE Trans Med Imaging 40:1363–1376
Hong J, Feng Z, Wang SH et al (2020) Brain age prediction of children using routine brain MR images via deep learning. Front Neurol 11. https://doi.org/10.3389/fneur.2020.584682
Achiron R, Achiron A (2001) Development of the human fetal corpus callosum: a high-resolution, cross-sectional sonographic study. Ultrasound Obstet Gynecol 18:343–347
Peterson BS, Vohr B, Staib LH et al (2022) Regional brain volume abnormalities and long-term cognitive outcome in preterm infants. In: Obsessive-compulsive disorder and Tourette’s syndrome. Routledge, pp 215–223
Woodward LJ, Anderson PJ, Austin NC et al (2006) Neonatal MRI to predict neurodevelopmental outcomes in preterm infants. N Engl J Med 355:685–694
Abernethy LJ, Cooke RWI, Foulder-Hughes L (2004) Caudate and hippocampal volumes, intelligence, and motor impairment in 7-year-old children who were born preterm. Pediatr Res 55:884–893. https://doi.org/10.1203/01.PDR.0000117843.21534.49
Alexander B, Kelly CE, Adamson C et al (2019) Changes in neonatal regional brain volume associated with preterm birth and perinatal factors. Neuroimage 185:654–663. https://doi.org/10.1016/j.neuroimage.2018.07.021
Funding
This study has received funding by the National Research Foundation of Korea (NRF-2021R1A2C1007831 and RS-2023-00233871).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Guarantor
The scientific guarantor of this publication is Hyun Gi Kim.
Conflict of interest
Author Donghyeon Kim has equity in Neurophet, Inc. Authors Sunghwan Park, Hyeonsik Yang, Minho Lee, and Regina E. Y. Kim are employed by Neurophet, Inc. No other author has reported a potential conflict of interest relevant to this article.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Informed consent
This retrospective study was approved by the Institutional Review Board, and the requirement for informed consent was waived.
Ethical approval
Approval from the Institutional Review Board of The Catholic University of Korea, Eunpyeong St. Mary’s Hospital, was obtained.
Study subjects or cohorts overlap
This study has used public datasets.
Some cases of the Catholic University of Korea dataset have been previously reported in “Three-dimensional magnetic resonance fingerprinting in neonates: quantifying regional difference and maturation in the brain”. Investigative Radiology. 2022 Jan 1;57(1):44–51.
However, the previous study used magnetic resonance fingerprinting of the neonates whereas this study used T1WI and T2WI.
Methodology
• retrospective
• experimental
• multicenter study
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Sunghwan Park and Hyun Gi Kim are co-first authors.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Park, S., Kim, H.G., Yang, H. et al. A regional brain volume–based age prediction model for neonates and the derived brain maturation index. Eur Radiol (2023). https://doi.org/10.1007/s00330-023-10408-6
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00330-023-10408-6