Abstract
Objectives
This study uses a practical positional MRI protocol to evaluate tibiofemoral translation and rotation in normal and injured knees.
Methods
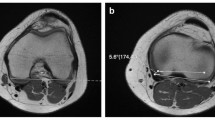
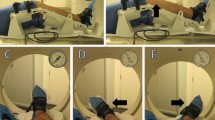
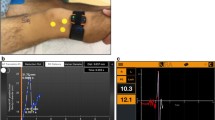
Following ethics approval, positional knee MRI of both knees was performed at 35° flexion, extension, and hyperextension in 34 normal subjects (mean age 31.1 ± 10 years) and 51 knee injury patients (mean age 36.4 ± 11.5 years, ACL tear n = 23, non-ACL injury n = 28). At each position, tibiofemoral translation and rotation were measured.
Results
Normal knees showed 8.1 ± 3.3° external tibial rotation (i.e., compatible with physiological screw home mechanism) in hyperextension. The unaffected knee of ACL tear patients showed increased tibial anterior translation laterally (p = 0.005) and decreased external rotation (p = 0.002) in hyperextension compared to normal knees. ACL-tear knees had increased tibial anterior translation laterally (p < 0.001) and decreased external rotation (p < 0.001) compared to normal knees. Applying normal thresholds, fifteen (65%) of 23 ACL knees had excessive tibial anterior translation laterally while 17 (74%) had limited external rotation. None (0%) of 28 non-ACL-injured knees had excessive tibial anterior translation laterally while 13 (46%) had limited external rotation. Multidirectional malalignment was much more common in ACL-tear knees.
Conclusions
Positional MRI shows (a) physiological tibiofemoral movement in normal knees, (b) aberrant tibiofemoral alignment in the unaffected knee of ACL tear patients, and (c) a high frequency of abnormal tibiofemoral malalignment in injured knees which was more frequent, more pronounced, more multidirectional, and of a different pattern in ACL-tear knees than non-ACL-injured knees.
Key Points
• Positional MRI shows physiological tibiofemoral translation and rotation in normal knees.
• Positional MRI shows a different pattern of tibiofemoral alignment in the unaffected knee of ACL tear patients compared to normal control knees.
• Positional MRI shows a high prevalence of abnormal tibiofemoral alignment in injured knees, which is more frequent and pronounced in ACL-tear knees than in ACL-intact injured knees.






Similar content being viewed by others
Abbreviations
- 3D:
-
Three-dimensional
- ACL:
-
Anterior cruciate ligament
- ANOVA:
-
Analysis of variance
- FOV:
-
Field of view
- ICC:
-
Intraclass correlation coefficient
- MRI:
-
Magnetic resonance imaging
- NSA:
-
Number of signal averages
- ROC:
-
Receiver operating characteristic
- SPSS:
-
Statistical Product and Service Solutions
- TE:
-
Time to echo
- TR:
-
Repetition time
- VISTA:
-
Volume isotropic turbo-spin echo acquisition
References
Mouton C, Seil R, Meyer T, Agostinis H, Theisen D (2015) Combined anterior and rotational laxity measurements allow characterizing personal knee laxity profiles in healthy individuals. Knee Surg Sports Traumatol Arthrosc 23:3571–3577
Snyder-Mackler L, Fitzgerald GK, Bartolozzi AR 3rd, Ciccotti MG (1997) The relationship between passive joint laxity and functional outcome after anterior cruciate ligament injury. Am J Sports Med 25:191–195
Musahl V, Kopf S, Rabuck S et al (2012) Rotatory knee laxity tests and the pivot shift as tools for ACL treatment algorithm. Knee Surg Sports Traumatol Arthrosc 20:793–800
Macchiarola L, Jacquet C, Dor J, Zaffagnini S, Mouton C, Seil R (2022) Side-to-side anterior tibial translation on monopodal weightbearing radiographs as a sign of knee decompensation in ACL-deficient knees. Knee Surg Sports Traumatol Arthrosc 30:1691–1699
Andreassen TE, Hamilton LD, Hume D et al (2021) Apparatus for in vivo knee laxity assessment using high-speed stereo radiography. J Med Device 15:041004
Logan MC, Williams A, Lavelle J, Gedroyc W, Freeman M (2004) What really happens during the Lachman test? A dynamic MRI analysis of tibiofemoral motion. Am J Sports Med 32:369–375
Mishima S, Takahashi S, Kondo S, Ishiguro N (2005) Anterior tibial subluxation in anterior cruciate ligament-deficient knees: quantification using magnetic resonance imaging. Arthroscopy 21:1193–1196
Okazaki K, Miura H, Matsuda S et al (2007) Assessment of anterolateral rotatory instability in the anterior cruciate ligament-deficient knee using an open magnetic resonance imaging system. Am J Sports Med 35:1091–1097
Tardy N, Marchand P, Kouyoumdjian P, Blin D, Demattei C, Asencio G (2014) A preliminary in vivo assessment of anterior cruciate ligament-deficient knee kinematics with the KneeM device: a new method to assess rotatory laxity using open MRI. Orthop J Sports Med 2:2325967114525583
Johal P, Williams A, Wragg P, Hunt D, Gedroyc W (2005) Tibio-femoral movement in the living knee. A study of weight bearing and non-weight bearing knee kinematics using ‘interventional’ MRI. J Biomech 38:269–276
Espregueira-Mendes J, Pereira H, Sevivas N et al (2012) Assessment of rotatory laxity in anterior cruciate ligament-deficient knees using magnetic resonance imaging with Porto-knee testing device. Knee Surg Sports Traumatol Arthrosc 20:671–678
Ishii Y, Terajima K, Terashima S, Koga Y (1997) Three-dimensional kinematics of the human knee with intracortical pin fixation. Clin Orthop Relat Res 343:144–150
Chen HN, Yang K, Dong QR, Wang Y (2014) Assessment of tibial rotation and meniscal movement using kinematic magnetic resonance imaging. J Orthop Surg Res 9:65
Zhang LK, Wang XM, Niu YZ, Liu HX, Wang F (2016) Relationship between patellar tracking and the “screw-home” mechanism of tibiofemoral joint. Orthop Surg 8:490–495
van Melick N, Meddeler BM, Hoogeboom TJ, Nijhuis-van der Sanden MWG, van Cingel REH (2017) How to determine leg dominance: the agreement between self-reported and observed performance in healthy adults. PLoS One 12:e0189876
Griffith JF, Ng AWH (2019) Top-ten tips for imaging the ACL. Semin Musculoskelet Radiol 23:444–452
Nacey NC, Geeslin MG, Miller GW, Pierce JL (2017) Magnetic resonance imaging of the knee: an overview and update of conventional and state of the art imaging. J Magn Reson Imaging 45:1257–1275
Ahn JH, Chang MJ, Lee YS, Koh KH, Park YS, Eun SS (2010) Non-operative treatment of ACL rupture with mild instability. Arch Orthop Trauma Surg 130:1001–1006
Tigerstrand Grevnerts H, Grävare Silbernagel K, Sonesson S et al (2017) Translation and testing of measurement properties of the Swedish version of the IKDC subjective knee form. Scand J Med Sci Sports 27:554–562
Kircher J (2019) Editorial commentary: The measurement of knee laxity: instrumented measurement and stress radiography for anterior cruciate ligament injuries. Arthroscopy 35:1733–1735
Eberhart HD, Inman VT (1951) An evaluation of experimental procedures used in a fundamental study of human locomotion. Ann N Y Acad Sci 51:1213–1228
Branch TP, Browne JE, Campbell JD et al (2010) Rotational laxity greater in patients with contralateral anterior cruciate ligament injury than healthy volunteers. Knee Surg Sports Traumatol Arthrosc 18:1379–1384
Mouton C, Theisen D, Meyer T et al (2015) Noninjured knees of patients with noncontact ACL injuries display higher average anterior and internal rotational knee laxity compared with healthy knees of a noninjured population. Am J Sports Med 43:1918–1923
Benoit DL, Ramsey DK, Lamontagne M, Xu L, Wretenberg P, Renström P (2006) Effect of skin movement artifact on knee kinematics during gait and cutting motions measured in vivo. Gait Posture 24:152–164
Barrance PJ, Williams GN, Novotny JE, Buchanan TS (2005) A method for measurement of joint kinematics in vivo by registration of 3-D geometric models with cine phase contrast magnetic resonance imaging data. J Biomech Eng 127:829–837
Shultz SJ, Shimokochi Y, Nguyen AD, Schmitz RJ, Beynnon BD, Perrin DH (2007) Measurement of varus-valgus and internal-external rotational knee laxities in vivo, part II: relationship with anterior-posterior and general joint laxity in males and females. J Orthop Res 25:989–996
Lin HC, Lai WH, Shih YF, Chang CM, Lo CY, Hsu HC (2009) Physiological anterior laxity in healthy young females: the effect of knee hyperextension and dominance. Knee Surg Sports Traumatol Arthrosc 17:1083–1088
Ng AW, Griffith JF, Hung EH, Law KY, Ho EP, Yung PS (2013) Can MRI predict the clinical instability and loss of the screw home phenomenon following ACL tear? Clin Imaging 37:116–123
Sernert N, Kartus JT, Ejerhed L, Karlsson J (2004) Right and left knee laxity measurements: a prospective study of patients with anterior cruciate ligament injuries and normal control subjects. Arthroscopy 20:564–571
Frobell RB, Roos HP, Roos EM, Roemer FW, Ranstam J, Lohmander LS (2013) Treatment for acute anterior cruciate ligament tear: five year outcome of randomised trial. BMJ 346:f232
Harris K, Driban JB, Sitler MR, Cattano NM, Hootman JM (2015) Five-year clinical outcomes of a randomized trial of anterior cruciate ligament treatment strategies: an evidence-based practice paper. J Athl Train 50:110–112
Mehier C, Ract I, Metten MA, Najihi N, Guillin R (2022) Primary anterior cruciate ligament repair: magnetic resonance imaging characterisation of reparable lesions and correlation with arthroscopy. Eur Radiol 32:582–592
Cahill SV, Sharkey MS, Carter CW (2021) Clinical assessment of generalized ligamentous laxity using a single test: is thumb-to-forearm apposition enough? J Pediatr Orthop B 30:296–300
Funding
The authors state that this work has not received any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Prof James F Griffith
Conflict of interest
The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and biometry
One of the authors has significant statistical expertise.
Informed consent
Written informed consent was obtained from all subjects (patients) in this study.
Ethical approval
Institutional Review Board approval was obtained.
Methodology
• prospective
• case-control study
• performed at one institution
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
ESM 1
(TIFF 320 KB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Griffith, J.F., Leung, C.T.P., Lee, J.C.H. et al. Positional MR imaging of normal and injured knees. Eur Radiol 33, 1553–1564 (2023). https://doi.org/10.1007/s00330-022-09198-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-022-09198-0