Abstract
Objectives
To develop and validate a risk scoring system based on clinical and imaging findings to predict lymph node metastasis from HPV-related oropharyngeal squamous cell carcinomas.
Methods
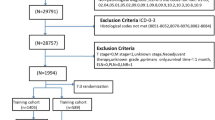
This study population who had undergone neck dissections or lymph node biopsies in patients with HPV+ OPSCC was obtained from a historical cohort from two tertiary referral hospitals. The training set from one hospital included 455 lymph nodes from 82 patients, and the test set from the other hospital included 150 lymph nodes from 42 patients. The baseline clinical and imaging findings on pretreatment CT or MR were investigated and the reference standards were the histopathologic results. A risk scoring system was constructed based on logistic regression and validated both internally and externally.
Results
A 7-point risk scoring system was developed based on the following variables: central necrosis, infiltration of adjacent planes, lymph node level, and the maximal axial diameter of the lymph node. This risk scoring system showed good discriminative ability for metastasis in the training set (C-statistic 0.952; 95% CI, 0.931–0.972) and test set (C-statistic 0.968, 95% CI, 0.936–0.999) and good calibration ability in the training set (p = 0.723) and test set (p = 0.253).
Conclusions
We developed and validated a reliable risk scoring system that predicts lymph node metastasis from HPV+ OPSCCs based on the clinical data and pretreatment imaging findings. We expect this risk scoring system to be a useful guide for better decision-making in practice.
Key Points
• It is important to diagnose lymph node metastasis from HPV+ OPSCC for treatment planning; however, there has been little research on that.
• We developed and externally validated a new scoring system for stratifying the risk of lymph node metastasis from HPV+ OPSCC based on clinical and imaging data.
• A predictive model combining both clinical and imaging data showed high diagnostic accuracy and efficiency for lymph node metastasis from HPV+ OPSCC.



Similar content being viewed by others
Abbreviations
- CT:
-
Computed tomography
- HPV+ OPSCC(s):
-
HPV-related oropharyngeal squamous cell carcinoma(s)
- MR:
-
Magnetic resonance imaging
References
Ang KK, Harris J, Wheeler R et al (2010) Human papillomavirus and survival of patients with oropharyngeal cancer. N Engl J Med 363:24–35
Chaturvedi AK, Engels EA, Pfeiffer RM et al (2011) Human papillomavirus and rising oropharyngeal cancer incidence in the United States. J Clin Oncol 29:4294–4301
O’Sullivan B, Huang SH, Su J et al (2016) Development and validation of a staging system for HPV-related oropharyngeal cancer by the International Collaboration on Oropharyngeal cancer Network for Staging (ICON-S): a multicentre cohort study. Lancet Oncol 17:440–451
Chaturvedi AK, Anderson WF, Lortet-Tieulent J et al (2013) Worldwide trends in incidence rates for oral cavity and oropharyngeal cancers. J Clin Oncol 31:4550–4559
Amin MB, Greene FL, Edge SB et al (2017) The Eighth Edition AJCC Cancer Staging Manual: continuing to build a bridge from a population-based to a more “personalized” approach to cancer staging. CA Cancer J Clin 67:93–99
Gillison ML, Broutian T, Pickard RK et al (2012) Prevalence of oral HPV infection in the United States, 2009-2010. JAMA 307:693–703
Taberna M, Mena M, Pavon MA, Alemany L, Gillison ML, Mesia R (2017) Human papillomavirus-related oropharyngeal cancer. Ann Oncol 28:2386–2398
Oosthuizen JC, Doody J (2019) De-intensified treatment in human papillomavirus-positive oropharyngeal cancer. Lancet 393:5–7
Masterson L, Moualed D, Liu ZW et al (2014) De-escalation treatment protocols for human papillomavirus-associated oropharyngeal squamous cell carcinoma: a systematic review and meta-analysis of current clinical trials. Eur J Cancer 50:2636–2648
Cantrell SC, Peck BW, Li G, Wei Q, Sturgis EM, Ginsberg LE (2013) Differences in imaging characteristics of HPV-positive and HPV-Negative oropharyngeal cancers: a blinded matched-pair analysis. AJNR Am J Neuroradiol 34:2005–2009
Collins GS, Reitsma JB, Altman DG, Moons KG (2015) Transparent Reporting of a multivariable prediction model for Individual Prognosis or Diagnosis (TRIPOD): the TRIPOD statement. Ann Intern Med 162:55–63
von Elm E, Altman DG, Egger M et al (2007) Strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. BMJ 335:806–808
Han K, Song K, Choi BW (2016) How to develop, validate, and compare clinical prediction models involving radiological parameters: study design and statistical methods. Korean J Radiol 17:339–350
Steinkamp HJ, Cornehl M, Hosten N, Pegios W, Vogl T, Felix R (1995) Cervical lymphadenopathy: ratio of long- to short-axis diameter as a predictor of malignancy. Br J Radiol 68:266–270
Yousem DM, Som PM, Hackney DB, Schwaibold F, Hendrix RA (1992) Central nodal necrosis and extracapsular neoplastic spread in cervical lymph nodes: MR imaging versus CT. Radiology 182:753–759
Som PM (1987) Lymph nodes of the neck. Radiology 165:593–600
Kaji AV, Mohuchy T, Swartz JD (1997) Imaging of cervical lymphadenopathy. Semin Ultrasound CT MR 18:220–249
Som PM (1992) Detection of metastasis in cervical lymph nodes: CT and MR criteria and differential diagnosis. AJR Am J Roentgenol 158:961–969
Goldenberg D, Begum S, Westra WH et al (2008) Cystic lymph node metastasis in patients with head and neck cancer: an HPV-associated phenomenon. Head Neck 30:898–903
Kalnins IK, Leonard AG, Sako K, Razack MS, Shedd DP (1977) Correlation between prognosis and degree of lymph node involvement in carcinoma of the oral cavity. Am J Surg 134:450–454
Mancuso AA, Harnsberger HR, Muraki AS, Stevens MH (1983) Computed tomography of cervical and retropharyngeal lymph nodes: normal anatomy, variants of normal, and applications in staging head and neck cancer. Part II: pathology. Radiology 148:715–723
Snow GB, Annyas AA, van Slooten EA, Bartelink H, Hart AA (1982) Prognostic factors of neck node metastasis. Clin Otolaryngol Allied Sci 7:185–192
Sullivan LM, Massaro JM, D’Agostino RB Sr (2004) Presentation of multivariate data for clinical use: the Framingham Study risk score functions. Stat Med 23:1631–1660
Murali R, Desilva C, Thompson JF, Scolyer RA (2010) Non-Sentinel Node Risk Score (N-SNORE): a scoring system for accurately stratifying risk of non-sentinel node positivity in patients with cutaneous melanoma with positive sentinel lymph nodes. J Clin Oncol 28:4441–4449
Liu W, Cheng R, Ma Y et al (2018) Establishment and validation of the scoring system for preoperative prediction of central lymph node metastasis in papillary thyroid carcinoma. Sci Rep 8:6962
Jeong JJ, Lee YS, Lee SC et al (2011) A scoring system for prediction of lateral neck node metastasis from papillary thyroid cancer. J Korean Med Sci 26:996–1000
He N, Xie C, Wei W et al (2012) A new, preoperative, MRI-based scoring system for diagnosing malignant axillary lymph nodes in women evaluated for breast cancer. Eur J Radiol 81:2602–2612
Lee L, Ronellenfitsch U, Hofstetter WL et al (2013) Predicting lymph node metastases in early esophageal adenocarcinoma using a simple scoring system. J Am Coll Surg 217:191–199
Tran TB, Worhunsky DJ, Squires MH et al (2018) Clinicopathologic score predicting lymph node metastasis in T1 gastric cancer. Surgery 163:889–893
Imai K, Kato H, Katayama K et al (2016) A preoperative risk-scoring system to predict lymph node metastasis in endometrial cancer and stratify patients for lymphadenectomy. Gynecol Oncol 142:273–277
Chung MS, Choi YJ, Kim SO et al (2019) A scoring system for prediction of cervical lymph node metastasis in patients with head and neck squamous cell carcinoma. AJNR Am J Neuroradiol 40:1049–1054
King AD, Tse GM, Ahuja AT et al (2004) Necrosis in metastatic neck nodes: diagnostic accuracy of CT, MR imaging, and US. Radiology 230:720–726
Som PM, Brandwein-Gensler MS (2011) Lymph nodes of the neck. In: Som PM, Curtin HD (eds) Head and neck imaging, 5th edn. Mosby Elsevier, St. Louis, pp 2287–2384
Ballantyne AJ (1964) Significance of retropharyngeal nodes in cancer of the head and neck. Am J Surg 108:500–504
Schwartz DL, Ford E, Rajendran J et al (2005) FDG-PET/CT imaging for preradiotherapy staging of head-and-neck squamous cell carcinoma. Int J Radiat Oncol Biol Phys 61:129–136
Park JT, Roh JL, Kim JS et al (2016) (18)F FDG PET/CT versus CT/MR imaging and the prognostic value of contralateral neck metastases in patients with head and neck squamous cell carcinoma. Radiology 279:481–491
Wong WL, Hussain K, Chevretton E et al (1996) Validation and clinical application of computer-combined computed tomography and positron emission tomography with 2-[18F]fluoro-2-deoxy-D-glucose head and neck images. Am J Surg 172:628–632
Ha PK, Hdeib A, Goldenberg D et al (2006) The role of positron emission tomography and computed tomography fusion in the management of early-stage and advanced-stage primary head and neck squamous cell carcinoma. Arch Otolaryngol Head Neck Surg 132:12–16
Zanation AM, Sutton DK, Couch ME, Weissler MC, Shockley WW, Shores CG (2005) Use, accuracy, and implications for patient management of [18F]-2-fluorodeoxyglucose-positron emission/computerized tomography for head and neck tumors. Laryngoscope 115:1186–1190
Funding
The authors state that this work has not received any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Young Jun Choi.
Conflict of interest
The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and biometry
One of the authors (Seon-Ok Kim) kindly provided statistical advice for this manuscript.
Informed consent
Written informed consent was waived by the Institutional Review Board.
Ethical approval
Institutional Review Board approval was obtained.
Methodology
• retrospective
• diagnostic or prognostic study
• multicenter study
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 17 kb)
Rights and permissions
About this article
Cite this article
Joo, L., Bae, Y.J., Choi, Y.J. et al. Prediction model for cervical lymph node metastasis in human papillomavirus-related oropharyngeal squamous cell carcinomas. Eur Radiol 31, 7429–7439 (2021). https://doi.org/10.1007/s00330-021-07766-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-021-07766-4