Abstract
Purpose
To analyze the effect of implant position measured in terms of offset on patient reported outcomes (PRO) following hip arthroplasty (THA).
Methods
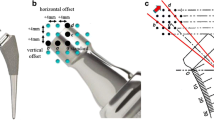
A total of 243 patients of the total hip replacement who had a one year follow-up were included in the study. Standard both hips radiograph was used to asses post-surgery implant position in terms of horizontal offset and vertical offset, and correlated with functional outcome which was evaluated as change in PRO. i.e., Harris hip score (HHS) post-op. With center of hip rotation as reference, horizontal offset was calculated as sum of distance, of centre, from proximal femoral shaft axis and a vertical line through ipsilateral teardrop, and vertical offset as limb length discrepancy. Post-op patients were classified into three groups depending on the measurement of horizontal offset of the operated hip. The patients having operated hip horizontal offset within 5 mm of the normal hip were grouped as restored offset (RO); those having shorter or higher offset by more than 5 mm compared to normal hip were labeled as decreased (DO) or increased offset (IO) group respectively. The groups were further subdivided into suboptimal and optimal function groups based on HHS, and among these groups, limb length discrepancy was evaluated.
Results
Post follow-up mean HHS (78.23 ± 9.96) improved significantly in all three groups (p < 0.0001). The difference in post-operative HHS among DO, RO, and IO groups was significant, with their averages being 72.5 ± 4.7, 82.1 ± 6.5, and 75.2 ± 4.8 respectively (p = .01). Limb length discrepancy was significantly more common in patients with suboptimal functional scores in all three groups.
Conclusion
This study concluded that both horizontal offset and vertical offset should be reconstructed in patients operated with unilateral THR due to hip pathology, since both factor demonstrated a comparable additive effect on clinical outcome.
Similar content being viewed by others
Data availability
The data that support the findings of this study are available from institutional records but restrictions apply to the availability of these data, which were used under license for the current study and so are not publicly available. Data are however available from the authors upon reasonable request and with permission of IEC.
References
Harkess JW, Crockarell JR Jr (2021) Arthroplasty of the hip. In: Azar FM, Beaty JH (eds) Campbell’s operative orthopaedics, 14th edn. Elsevier, Canada, pp 178–333
Singh JA, Lewallen D (2010) Predictors of pain and use of pain medications following primary total hip arthroplasty (THA): 5,707 THAs at 2-years and 3,289 THAs at 5-years. BMC MusculoskeletDisord 13(11):90. https://doi.org/10.1186/1471-2474-11-90
Singh JA, Lewallen DG (2010) Predictors of activity limitation and dependence on walking aids after primary total hip arthroplasty. J Am GeriatrSoc 58:2387–2393. https://doi.org/10.1111/j.1532-5415.2010.03182.x
Vissers MM, Bussmann JB, Verhaar JA, Arends LR, Furlan AD, Reijman M (2011) Recovery of physical functioning after total hip arthroplasty: systematic review and meta-analysis of the literature. PhysTher 91(5):615–629. https://doi.org/10.2522/ptj.20100201
Williams O, Fitzpatrick R, Hajat S et al (2002) Mortality, morbidity, and 1-year outcomes of primary elective total hip arthroplasty. J Arthroplasty 17:165–171. https://doi.org/10.1054/arth.2002.29389
MacWilliam CH, Yood MU, Verner JJ et al (1996) Patient-related risk factors that predict poor outcome after total hip replacement. Health Serv Res 31:623–638
Hesseling B, Mathijssen NMC, van Steenbergen LN, Melles M, Vehmeijer SBW, Porsius JT (2019) Fast starters, slow starters, and late dippers: trajectories of patient-reported outcomes after total hip arthroplasty: results from a Dutch Nationwide Database. J Bone Joint Surg Am 101(24):2175–2186. https://doi.org/10.2106/JBJS.19.00234
Lübbeke A, Zimmermann-Sloutskis D, Stern R, Roussos C, Bonvin A, Perneger T, Peter R, Hoffmeyer P (2014) Physical activity before and after primary total hip arthroplasty: a registry-based study. Arthritis Care Res (Hoboken) 66(2):277–284. https://doi.org/10.1002/acr.22101
Slaven EJ (2012) Prediction of functional outcome at six months following total hip arthroplasty. PhysTher 92(11):1386–94. https://doi.org/10.2522/ptj.20110484
Nankaku M, Tsuboyama T, Akiyama H, Kakinoki R, Fujita Y, Nishimura J, Yoshioka Y, Kawai H, Matsuda S (2013) Preoperative prediction of ambulatory status at 6 months after total hip arthroplasty. PhysTher 93(1):88–93. https://doi.org/10.2522/ptj.20120016
Quintana JM, Escobar A, Aguirre U, Lafuente I, Arenaza JC (2009) Predictors of health-related quality-of-life change after total hip arthroplasty. ClinOrthopRelat Res 467(11):2886–94. https://doi.org/10.1007/s11999-009-0868-9
Buirs LD, Van Beers LWAH, Scholtes VAB et al (2016) Predictors of physical functioning after total hip arthroplasty: a systematic review. BMJ Open 6:e010725. https://doi.org/10.1136/bmjopen-2015-010725
Anakwe RE, Jenkins PJ, Moran M (2011) Predicting dissatisfaction after total hip arthroplasty: a study of 850 patients. J Arthroplasty 26:209–213. https://doi.org/10.1016/j.arth.2010.03.013
Beswick AD, Wylde V, Gooberman-Hill R, Blom A, Dieppe P (2012) What proportion of patients report long-term pain after total hip or knee replacement for osteoarthritis? A systematic review of prospective studies in unselected patients. BMJ Open 2:e000435. https://doi.org/10.1136/bmjopen-2011-000435
Rojanasopondist P, Galea VP, Connelly JW et al (2019) What preoperative factors are associated with not achieving a minimum clinically important difference after THA? Findings from an International Multicenter Study. ClinOrthopRelat Res 477(6):1301–1312. https://doi.org/10.1097/CORR.0000000000000667
Bhaskar D, Rajpura A, Board T (2017) Current concepts in acetabular positioning in total hip arthroplasty. Indian J Orthop 51(4):386–396. https://doi.org/10.4103/ortho.IJOrtho_144_17
Harris WH (1969) Traumatic arthritis of the hip after dislocation and acetabular fractures: treatment by mold arthroplasty. An end-result study using a new method of result evaluation. JBJS 51A:737
Longo UG, Ciuffreda M, Candela V, Berton A, Maffulli N, Denaro V (2019) Hip scores: a current concept review. Br Med Bull 131(1). https://doi.org/10.1093/bmb/ldz026
Grammatopoulos G, Falsetto A, Sanders E, Weishorn J, Gill HS, Beaulé PE, Innmann MM, Merle C (2021) Integrating the combined sagittal index reduces the risk of dislocation following total hip replacement. JBJS 10–2106. https://doi.org/10.2106/JBJS.21.0043219
Asayama I, Naito M, Fujisawa M, Kambe T (2002) Relationship between radiographic measurements of reconstructed hip joint position and the Trendelenburg sign. J Arthroplasty 17:747–751. https://doi.org/10.1054/arth.2002.33552
Bourne RB, Rorabeck CH (2002) Soft tissue balancing: the hip. J Arthroplasty 17:17–22. https://doi.org/10.1054/arth.2002.33263
Confalonieri N, Manzotti A, Cerveri P, DeMomi E (2009) Bi-unicompartmental versus total knee arthroplasty: a matched paired study with early clinical results. Arch Orthop Trauma Surg 129:1157–1163. https://doi.org/10.1007/s00402-008-0713-8
Fackler CD, Poss R (1980) Dislocation in total hip arthroplasties. ClinOrthop 151:169–178
Davey JR, O’connor DO, Burke DW, Harris WH (1993) Femoral component offset. Its effect on strain in bone-cement. J Arthroplasty 8:23–6
Mcgrory BJ, Morrey BF, Cahalan TD et al (1995) Effect of femoral offset on range of motion and abductor muscle strength after total hip arthroplasty. J Bone Joint Surg Br 77:865–869
Spalding TJ (1996) Effect of femoral offset on motion and abductor muscle strength after total hip arthroplasty. J Bone Joint Surg Br 78:997–998
Cassidy KA, Noticewala MS, Macaulay W, Lee JH, Geller JA (2012) Effect of femoral offset on pain and function after total hip arthroplasty. J Arthroplasty 27:1863–1869. https://doi.org/10.1016/j.arth.2012.05.001
Incavo SJ, Havener T, Benson E et al (2004) Efforts to improve cementless femoral stems in THR: 2- to 5-year follow-up of a high-offset femoral stem with distal stem modification (Secur-Fit Plus). J Arthroplasty 19:61–67. https://doi.org/10.1016/j.arth.2003.09.006
McGrory, Morrey BF, Cahalan TD, An KN, Cabanela ME (1995) Effect of femoral offset on range of motion and abductor muscle strength after total hip arthroplasty. J Bone Joint Surg [Br] 77-B:865–869
Erivan R, Aubret S, Villatte G, Mulliez A, Descamps S, Boisgard S (2017) Does using a polyethylene RM press-fit cup modify the preparation of the acetabulum and acetabular offset in primary hip arthroplasty? Orthop Traumatol Surg Res 103(5):669–74. https://doi.org/10.1016/j.otsr.2017.03.026
Shapira J, Chen SL, Rosinsky PJ, Maldonado DR, Meghpara M, Lall AC, Domb BG (2020) The effect of postoperative femoral offset on outcomes after hip arthroplasty: a systematic review. J Orthop 1(22):5–11. https://doi.org/10.1016/j.jor.2020.03.034
Konyves A, Bannister G (2005) The importance of leg length discrepancy after total hip arthroplasty. J Bone Joint Surg Br 87(2):155–157. https://doi.org/10.1302/0301-620x.87b2.14878
McGrory B, Morrey B, Cahalan T, An K, Cabanela M (1995) Effect of femoral offset on range of motion and abductor muscle strength after total hip arthroplasty. J Bone Joint Surg Br 77(6):865–869
Gore DR, Murray MP, Gardner GM, Sepic SB (1977) Roentgenographic measurements after müller total hip replacement. Correlations among roentgenographic measurements and hip strength and mobility. J Bone Joint Surg Am 59(7):948–53
Sayed-Noor AS, Hugo A, Sjödén GO, Wretenberg P (2009) Leg length discrepancy in total hip arthroplasty: comparison of two methods of measurement. IntOrthop 33(5):1189–1193. https://doi.org/10.1007/s00264-008-0633-9
Sayed-Noor AS, Sjoden GO (2006) Greater trochanteric pain after total hip arthroplasty: the incidence, clinical outcome and associated factors. Hip Int 16(3):202–206. https://doi.org/10.5301/hip.2008.4186
Rösler J, Perka C (2000) The effect of anatomical positional relationships on kinetic parameters after total hip replacement. Int Orthop 24(1):23–7. https://doi.org/10.1007/s002640050006
Mancuso CA, Jout J, Salvati EA, Sculco TP (2009) Fulfillment of patients’ expectations for total hip arthroplasty. J Bone Joint Surg Am 91:2073–2078. https://doi.org/10.2106/JBJS.H.01802
Zhang Y, He W, Cheng T et al (2015) Total hip arthroplasty: leg length discrepancy affects functional outcomes and patient’s gait. Cell BiochemBiophys 72(1):215–219. https://doi.org/10.1007/s12013-014-0440-4
Plaass C, Clauss M, Ochsner PE, Ilchmann T (2011) Influence of leg length discrepancy on clinical results after total hip arthroplasty-a prospective clinical trial. Hip Int 21(4):441–449. https://doi.org/10.5301/HIP.2011.8575
Erivan R, Muller AS, Villatte G, Millerioux S, Mulliez A, Boisgard S, Descamps S (2020) Short stems reproduce femoral offset better than standard stems in total hip arthroplasty: a case-control study. Int Orthop 44(1):45–51. https://doi.org/10.1007/s00264-019-04355-5
Luger M, Feldler S, Klasan A, Gotterbarm T, Schopper C (2021) The morphology of the proximal femur in cementless short-stem total hip arthroplasty: no negative effect on offset reconstruction, leg length difference and implant positioning. J Orthop Surg Res 16(1):1–9. https://doi.org/10.1186/s13018-021-02876-7
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by KS, MA, and AV. The first draft of the manuscript was written by KS and all authors commented on previous versions of the manuscript. NK, RA, and HKR helped in statistical analysis and manuscript review. All authors read and approved the final manuscript. RC supervised all the things.
Corresponding author
Ethics declarations
Ethics approval
Approval was obtained from the ethics committee of DR. S. N. Medical College and associated group of hospitals, Jodhpur (Date-27/04/2018, No.F.1 Acad/MC/Ju/18/6909).
Consent to participate
Informed consent was obtained from all study participants.
Consent for publication
Patients signed informed consent regarding publishing their data and photographs.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Vaishy, A., Arif, M., Aanand, R. et al. Implant positioning in total hip arthroplasty: influence of horizontal and vertical offset on functionality of prosthetic hip joint. International Orthopaedics (SICOT) 46, 1501–1506 (2022). https://doi.org/10.1007/s00264-022-05364-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-022-05364-7