Abstract
Introduction
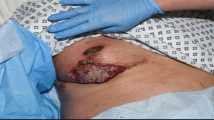
Pyoderma gangrenosum (PG) is a neutrophilic dermatosis characterised by a painful ulceration mimicking infection of the operative site. To this day, there is still no general agreement on the medical and surgical treatment of PG. This systematic review of the literature aims to summarise recent studies about post-operative PG in orthopaedic surgery to improve its medical and surgical management.
Method
In April 2017, we carried out an exhaustive review of the literature in MEDLINE, PubMed and Cochrane databases. Key words were pyoderma gangrenosum, orthopaedic surgery, and surgical wound infection. We identified 183 articles. After excluding articles reporting idiopathic PG, cases secondary to non-orthopaedic surgery, and cases about other subtypes of dermatosis, 30 studies were identified. We only included articles reporting PG after orthopaedic or trauma surgery.
Results
Thirty-one cases of PG have been reported, 58% (18) of which were in women, whose mean age was 56.5 years. Clinical signs were constant, the most frequently affected site was lower limbs [77.4% (24)] and delay of symptom onset was two to 17 days. Systemic corticosteroid therapy was systematic, polyvalent immunoglobulins were used in two cases and immunosuppressive drugs in one. Negative pressure therapy was used in seven cases and hyperbaric oxygen in three.
Discussion
Delayed diagnosis leads to one or more surgical revisions, which could have been avoided by using early and adapted medical treatment. Early onset of a painful and infected ulcer at the operating site in a patient at risk of PG is an indicator that dermatologist advice is recommended before surgical debridement. Surgical revision, outside the inflammatory phase and/or covered by a systemic corticosteroid therapy, does not lead to PG relapse.
Level of evidence
IV: Systematic revue of the literature.


Similar content being viewed by others
References
Brunsting LA (1930) Pyoderma (echtyma) gangrenosum: clinical and experimental observations in five cases occuring in adults. Arch Dermatol Syphilol 22:655. https://doi.org/10.1001/archderm.1930.01440160053009
Powell FC, Daniel Su WP, Perry HO (1996) Pyoderma gangrenosum: classification and management. J Am Acad Dermatol 34:395–409. https://doi.org/10.1016/S0190-9622(96)90428-4
Braswell SF, Kostopoulos TC, Ortega-Loayza AG (2015) Pathophysiology of pyoderma gangrenosum (PG): an updated review. J Am Acad Dermatol 73:691–698. https://doi.org/10.1016/j.jaad.2015.06.021
Bagouri E, Smith J, Geutjens G (2012) Anterior cruciate ligament reconstruction complicated by pyoderma gangrenosum. Ann R Coll Surg Engl 94:e257–e259. https://doi.org/10.1308/003588412X13373405387573
Ogon M, Sepp NT, Wimmer C, Behensky H (2000) A surgical wound infection? Lancet Lond Engl 356:1652. https://doi.org/10.1016/S0140-6736(00)03161-5
Verma SB (2009) Atypical pyoderma gangrenosum following total knee replacement surgery: first report in dermatologic literature. An Bras Dermatol 84:689–691
Yari SS, Reichel LM (2014) Case report: misdiagnosed olecranon bursitis: pyoderma gangrenosum. J Shoulder Elb Surg 23:e207–e211. https://doi.org/10.1016/j.jse.2014.06.032
Henault B, Duvernay A, Legré R, Zwetyenga N (2011) Dermo-hypodermites nécrosantes neutrophiliques postopératoires de la main. Un diagnostic à ne pas rater. Chir Main 30:288–293. https://doi.org/10.1016/j.main.2011.06.003
Long CC, Jessop J, Young M, Holt PJ (1992) Minimizing the risk of post-operative pyoderma gangrenosum. Br J Dermatol 127:45–48
Ayestaray B, Dudrap E, Chartaux E et al (2010) Necrotizing pyoderma gangrenosum: an unusual differential diagnosis of necrotizing fasciitis. J Plast Reconstr Aesthetic Surg JPRAS 63:e655–e658. https://doi.org/10.1016/j.bjps.2010.02.008
Tolkachjov SN, Fahy AS, Wetter DA et al (2015) Postoperative pyoderma gangrenosum (PG): the Mayo Clinic experience of 20 years from 1994 through 2014. J Am Acad Dermatol 73:615–622. https://doi.org/10.1016/j.jaad.2015.06.054
Wadia F, Malik MHA, Porter ML (2007) Postoperative wound breakdown caused by pyoderma Gangrenosum after bilateral simultaneous Total knee arthroplasty. J Arthroplast 22:1232–1235. https://doi.org/10.1016/j.arth.2006.09.017
Madsen JT, Skov O, Andersen KE (2009) Pyoderma gangraenosum as a complication to knee arthroscopy. Knee 16:299–300. https://doi.org/10.1016/j.knee.2008.12.006
Armstrong PM, Ilyas I, Pandey R et al (1999) Pyoderma gangrenosum A DIAGNOSIS NOT TO BE MISSED. J Bone Joint Surg Br 81-B:893–894
De Thomasson E, Caux I (2010) Pyoderma gangrenosum following an orthopedic surgical procedure. Orthop Traumatol Surg Res 96:600–602. https://doi.org/10.1016/j.otsr.2009.12.014
Hill DS, O’Neill JK, Toms A, Watts AM (2011) Pyoderma gangrenosum: a report of a rare complication after knee arthroplasty requiring muscle flap cover supplemented by negative pressure therapy and hyperbaric oxygen. J Plast Reconstr Aesthet Surg 64:1528–1532. https://doi.org/10.1016/j.bjps.2011.03.024
Attar S, Spangehl MJ, Casey WJ, Smith AA (2010) Pyoderma gangrenosum complicating bilateral total knee arthroplasty. Orthopedics 33:441. https://doi.org/10.3928/01477447-20100429-28
Fang Z, Waizy H, Berger S et al (2013) Pyoderma Gangrenosum following Orthopaedic surgery. JBJS Case Connect 3:e84. https://doi.org/10.2106/JBJS.CC.M.00031
Melo Grollmus R, Fernández de Retana P (2013) Pyoderma gangrenosum following foot and ankle surgery: a case report. Foot Ankle Int 34:745–748. https://doi.org/10.1177/1071100712471661
Wanich T, Swanson AN, Wyatt AJ, Kelly AM (2012) Pyoderma gangrenosum following patellar tendon repair: a case report and review of the literature. Am J Orthop Belle Mead NJ 41:E4–E9
Steenbrugge F, Raaijmaakers M, Caekebeke P, Van Landuyt K (2011) Pyoderma gangrenosum following trauma of the knee: a case of pathergy and review of orthopaedic cases. Injury 42:421–423. https://doi.org/10.1016/j.injury.2010.06.015
Lee HS, Choi YR, Ha SH, Jeong JJ (2013) Pyoderma Gangrenosum mimicking a diabetic foot infection: a case report. J Foot Ankle Surg 52:67–71. https://doi.org/10.1053/j.jfas.2012.09.002
Nizamoglu M (2015) Pyoderma Gangrenosum mimicking an infected wound following dynamic hip screw fixation. Case Rep Orthop 2015:571472. https://doi.org/10.1155/2015/571472
Yik JH, Bigliardi PL, Sebastin SJ et al (2015) Pyoderma gangrenosum mimicking early acute infection following total knee arthroplasty. Ann Acad Med Singap 44:150–151
Bennett CR, Brage ME, Mass DP (1999) Pyoderma Gangrenosum mimicking postoperative infection in the extremities. A report of two cases*. J Bone Jt Surg Case Connect 81:1013–1018
Wangia MW, Mitchell CL, Wesson SK et al (2013) Pyoderma gangrenosum or necrotizing fasciitis? A diagnostic conundrum Case report and literature review. J Pediatr Surg Case Rep 1:139–142. https://doi.org/10.1016/j.epsc.2013.05.005
Choe H, Sakano H, Takigami H et al (2013) Pyoderma gangrenosum with wrist joint destruction: case report. J Hand Surg 38:357–361. https://doi.org/10.1016/j.jhsa.2012.10.049
Reid AB, Stanley P, Grinsell D, Daffy JR (2014) Severe, steroid-responsive, myositis mimicking necrotizing fasciitis following orthopedic surgery: a pyoderma variant with Myonecrosis. Plast Reconstr Surg Glob Open 2:e175. https://doi.org/10.1097/GOX.0000000000000124
Nakajima N, Ikeuchi M, Izumi M et al (2011) Successful treatment of wound breakdown caused by pyoderma gangrenosum after total knee arthroplasty. Knee 18:453–455. https://doi.org/10.1016/j.knee.2010.06.005
Jain A, Nanchahal J, Bunker C (2000) Pyoderma gangrenosum occurring in a lower limb fasciocutaneous flap — a lesson to learn. Br J Plast Surg 53:437–440. https://doi.org/10.1054/bjps.2000.3351
Mandal A, Addison P, Stewart K, Neligan P (2005) Vacuum-assisted closure therapy in pyoderma gangrenosum. Eur J Plast Surg 28:529–531. https://doi.org/10.1007/s00238-005-0014-1
Suarez C, Mercier E, Piquet P et al (2011) À propos de l’article : « Pyoderma gangrenosum après chirurgie orthopédique » de E. de Thomasson et I. Caux, publié dans Rev Chir Orthop 2010;96:672–4. Rev Chir Orthopédique Traumatol 97:865–866. https://doi.org/10.1016/j.rcot.2011.10.013
Hackl S, Merkel P, Hungerer S et al (2015) Pyoderma gangraenosum nach Marknagelosteosynthese bei Tibiaschaftfraktur: Eine Differenzialdiagnose zur nekrotisierenden Fasziitis. Unfallchirurg 118:1062–1066. https://doi.org/10.1007/s00113-015-2737-1
Ruocco E, Sangiuliano S, Gravina A et al (2009) Pyoderma gangrenosum: an updated review. J Eur Acad Dermatol Venereol 23:1008–1017. https://doi.org/10.1111/j.1468-3083.2009.03199.x
Amazan E, Baubion E, Thimon S et al (2013) Incidence du Pyoderma gangrenosum en Martinique (Antilles françaises). Ann Dermatol Vénéréologie 140:S372. https://doi.org/10.1016/j.annder.2013.09.029
Zuo KJ, Fung E, Tredget EE, Lin AN (2015) A systematic review of post-surgical pyoderma gangrenosum: identification of risk factors and proposed management strategy. J Plast Reconstr Aesthet Surg 68:295–303. https://doi.org/10.1016/j.bjps.2014.12.036
Crowson AN, Mihm MC Jr, Magro C (2003) Pyoderma gangrenosum: a review. J Cutan Pathol 30:97–107. https://doi.org/10.1034/j.1600-0560.2003.00024.x
Ahronowitz I, Harp J, Shinkai DK (2012) Etiology and Management of Pyoderma Gangrenosum. Am J Clin Dermatol 13:191–211. https://doi.org/10.2165/11595240-000000000-00000
DeFilippis EM, Feldman SR, Huang WW (2015) The genetics of pyoderma gangrenosum and implications for treatment: a systematic review. Br J Dermatol 172(6):1487–1497. https://doi.org/10.1111/bjd.13493
Van de Vijver E, van den Berg TK, Kuijpers TW (2013) Leukocyte adhesion deficiencies. Hematol Oncol Clin North Am 27:101–116. https://doi.org/10.1016/j.hoc.2012.10.001
Marzano AV, Fanoni D, Antiga E et al (2014) Expression of cytokines, chemokines and other effector molecules in two prototypic autoinflammatory skin diseases, pyoderma gangrenosum and Sweet’s syndrome. Clin Exp Immunol 178:48–56. https://doi.org/10.1111/cei.12394
Wollina U (2007) Pyoderma gangrenosum – a review. Orphanet J Rare Dis 2:19. https://doi.org/10.1186/1750-1172-2-19
Wollina U (2015) Pyoderma gangrenosum—a systemic disease? Clin Dermatol 33:527–530. https://doi.org/10.1016/j.clindermatol.2015.05.003
Maejima H, Watarai A, Tanabe K, Takasu H, Katsuoka K, Sada M (2014) Osteomyelitis in association with pyoderma Gangrenosum and ulcerative colitis. Cutis 93(4):E14–E16
Wolff DA (1884) Zur Aetiologie der Psoriasis. Vierteljahresschr Für Dermatol Syph 11:337–340. https://doi.org/10.1007/BF01843434
Su WPD, Davis MDP, Weenig RH et al (2004) Pyoderma gangrenosum: clinicopathologic correlation and proposed diagnostic criteria. Int J Dermatol 43:790–800. https://doi.org/10.1111/j.1365-4632.2004.02128.x
Waterworth AS, Horgan K (2004) Pyoderma gangrenosum—an unusual differential diagnosis for acute infection. Breast 13:250–253. https://doi.org/10.1016/j.breast.2003.10.012
Lê Huu S, Spertini F, Roggero P et al (2009) Le pyoderma gangrenosum : pathologie rare ou diagnostic omis ? Ann Chir Plast Esthét 54:82–87. https://doi.org/10.1016/j.anplas.2008.05.006
Barr KL, Chhatwal HK, Wesson SK et al (2009) Pyoderma gangrenosum masquerading as necrotizing fasciitis. Am J Otolaryngol 30:273–276. https://doi.org/10.1016/j.amjoto.2008.05.005
Villarreal-Villarreal CD, Ocampo-Candiani J, Villarreal-Martínez A (2016) Sweet syndrome: a review and update. Actas Dermosifiliogr 107(5):369–378. https://doi.org/10.1016/j.ad.2015.12.001
Gibson LE, Daoud MS, Muller SA, Perry HO (1997) Malignant pyodermas revisited. Mayo Clin Proc 72:734–736. https://doi.org/10.1016/S0025-6196(11)63593-3
Reichrath J, Bens G, Bonowitz A, Tilgen W (2005) Treatment recommendations for pyoderma gangrenosum: an evidence-based review of the literature based on more than 350 patients. J Am Acad Dermatol 53:273–283. https://doi.org/10.1016/j.jaad.2004.10.006
Chow RKP, Ho VC (1996) Treatment of pyoderma gangrenosum. J Am Acad Dermatol 34:1047–1060. https://doi.org/10.1016/S0190-9622(96)90285-6
Ormerod AD, Thomas KS, Craig FE et al (2015) Comparison of the two most commonly used treatments for pyoderma gangrenosum: results of the STOP GAP randomised controlled trial. BMJ 350:h2958. https://doi.org/10.1136/bmj.h2958
Dobson CM, Parslew RA, Evans S (2003) Superficial granulomatous pyoderma treated with intravenous immunoglobulin. J Am Acad Dermatol 48:456–460. https://doi.org/10.1067/mjd.2003.172
Novo-Torres A, Céspedes-Guirao FJ, Restituyo NG, Lorda-Barraguer E (2015) Management of pyoderma gangrenosum with combination of systemic treatment, vacuum-assisted closure and synthetic dermal substitute. Eur J Plast Surg 39:297–302. https://doi.org/10.1007/s00238-015-1147-5
Ghersi MM, Ricotti C, Nousari CH, Newman MI (2007) NEgative pressure dressing in the management of pyoderma gangrenosum ulcer. Arch Dermatol 143:1249–1251. https://doi.org/10.1001/archderm.143.10.1249
Geller SM, Longton JA (2005) Ulceration of pyoderma Gangrenosum treated with negative pressure wound therapy. J Am Podiatr Med Assoc 95:171–174. https://doi.org/10.7547/0950171
Fraccalvieri M, Fierro MT, Salomone M et al (2014) Gauze-based negative pressure wound therapy: a valid method to manage pyoderma gangrenosum. Int Wound J 11:164–168. https://doi.org/10.1111/j.1742-481X.2012.01058.x
Pichler M, Larcher L, Holzer M et al (2016) Surgical treatment of pyoderma gangrenosum with negative pressure wound therapy and split thickness skin grafting under adequate immunosuppression is a valuable treatment option: case series of 15 patients. J Am Acad Dermatol 74:760–765. https://doi.org/10.1016/j.jaad.2015.09.009
Cabalag MS, Wasiak J, Lim SW, Raiola FB (2015) Inpatient management of pyoderma gangrenosum: treatments, outcomes, and clinical implications. Ann Plast Surg 74:354–360. https://doi.org/10.1097/SAP.0b013e31829565f3
Mazokopakis EE, Kofteridis DP, Pateromihelaki AT et al (2011) Improvement of ulcerative pyoderma gangrenosum with hyperbaric oxygen therapy. Dermatol Ther 24:134–136. https://doi.org/10.1111/j.1529-8019.2010.01387.x
Vieira WA, Barbosa LR, Martin LMM (2011) Hyperbaric oxygen therapy as an adjuvant treatment for pyoderma gangrenosum. An Bras Dermatol 86:1193–1196. https://doi.org/10.1590/S0365-05962011000600022
Wasserteil V, Bruce S, Sessoms SL, Guntupalli KK (1992) Pyoderma Gangrenosum treated with hyperbaric oxygen therapy. Int J Dermatol 31:594–596. https://doi.org/10.1111/j.1365-4362.1992.tb02728.x
Chiang IH, Liao YS, Dai NT, Chou CY, Chen SG, Chen TM, Chang SC (2016) Hyperbaric oxygen therapy for the adjunctive treatment of pyoderma Gangrenosum: a case report. Ostomy Wound Manage 62(2):32–36
Niezgoda JA, Cabigas EB, Allen HK et al (2006) Managing pyoderma Gangrenosum: a synergistic approach combining surgical D??Bridement, vacuum-assisted closure, and hyperbaric oxygen therapy. Plast Reconstr Surg 117:24e–28e. https://doi.org/10.1097/01.prs.0000200776.13868.02
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Rights and permissions
About this article
Cite this article
Ebrad, S., Severyns, M., Benzakour, A. et al. Pyoderma gangrenosum after orthopaedic or traumatologic surgery: a systematic revue of the literature. International Orthopaedics (SICOT) 42, 239–245 (2018). https://doi.org/10.1007/s00264-017-3672-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-017-3672-2