Abstract
Liver transplantation is a potentially curative treatment for patients with acute liver failure, end-stage liver disease, and primary hepatic malignancy. Despite tremendous advancements in surgical techniques and immunosuppressive management, there remains a high rate of post-transplant complications, with one of the main complications being biliary complications. In addition to anastomotic leak and stricture, numerous additional biliary complications are encountered, including ischemic cholangiopathy due to the sole arterial supply of the bile ducts, recurrence of primary biliary disease, infections, biliary obstruction from stones, cast, or hemobilia, and less commonly cystic duct remnant mucocele, vanishing duct syndrome, duct discrepancy and kinking, post-transplant lymphoproliferative disorder, retained stent, and ampullary dysfunction. This article presents an overview of biliary anatomy and surgical techniques in liver transplantation, followed by a detailed review of post-transplant biliary complications with their corresponding imaging findings on multiple modalities with emphasis on magnetic resonance imaging and MR cholangiopancreatography.
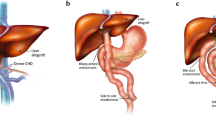
Graphical abstract
















Similar content being viewed by others
Availability of data and materials
Not applicable.
Code availability
Not applicable.
Abbreviations
- CT:
-
Computed tomography
- CHD:
-
Common hepatic duct
- CBD:
-
Common bile duct
- ERCP:
-
Endoscopic retrograde cholangiopancreatography
- FASE:
-
Fast advanced spin echo
- HASTE:
-
Half-Fourier acquisition single-shot turbo spin echo imaging
- HIDA:
-
Hepatobiliary scintigraphy
- LDLT:
-
Living donor liver transplant
- LHD:
-
Left hepatic duct
- MRI:
-
Magnetic resonance imaging
- MRCP:
-
Magnetic resonance cholangiopancreatography
- MIP:
-
Maximum intensity projection
- OLT:
-
Orthotopic liver transplant
- PTC:
-
Percutaneous transhepatic cholangiogram
- PTLD:
-
Post-transplant lymphoproliferative disorder
- PBC:
-
Primary biliary cholangitis
- PSC:
-
Primary sclerosing cholangitis
- RAHD:
-
Right anterior hepatic duct
- RPHD:
-
Right posterior hepatic duct
- RHD:
-
Right hepatic duct
- RARE:
-
Rapid acquisition with relaxation enhancement
- SSFSE:
-
Single-shot fast spin echo
References
Moy BT, Birk JW (2019). A review on the management of biliary complications after orthotopic liver transplantation. J Clin Transl Hepatol 7(1):61-71. https://doi.org/10.14218/JCTH.2018.00028
Daniel K, Said A (2017) Early biliary complications after liver transplantation. Clin Liver Dis 10(3):63-67. https://doi.org/10.1002/cld.654
Uzochukwu LN, Bluth EI, Smetherman DH, et al (2005) Early postoperative hepatic sonography as a predictor of vascular and biliary complications in adult orthotopic liver transplant patients. Am J Roentgenol 185(6):1558-1570. https://doi.org/10.2214/AJR.04.1258
Balderramo D, Bordas JM, Sendino O, et al (2011) Complications after ERCP in liver transplant recipients. Gastrointest Endosc 74(2):285-294. https://doi.org/10.1016/j.gie.2011.04.025
Kinner S, Schubert TB, Said A, Mezrich JD, Reeder SB (2017) Added value of gadoxetic acid-enhanced T1-weighted magnetic resonance cholangiography for the diagnosis of post-transplant biliary complications. Eur Radiol 27(10):4415-4425. https://doi.org/10.1007/s00330-017-4797-9
Boraschi P, Donati F, Pacciardi F, Ghinolfi D, Falaschi F (2018) Biliary complications after liver transplantation: assessment with MR cholangiopancreatography and MR imaging at 3T device. Eur J Radiol 106:46-55. https://doi.org/10.1016/j.ejrad.2018.07.009
Blumgart LH, Schwartz LH, DeMatteo RP (2017) Surgical and radiologic anatomy of the liver, biliary tract, and pancreas. In: Jarnagin WR (ed) Blumgart’s Surgery of the Liver, Biliary Tract and Pancreas, 2-Volume Set, 6th edn. Elsevier, St. Louis, pp 32–59. https://doi.org/10.1016/B978-0-323-34062-5.00002-9
Healey JE Jr, Schroy PC (1953) Anatomy of the biliary ducts within the human liver: analysis of the prevailing pattern of branchings and the major variations of the biliary ducts. AMA Arch Surg 66(5):599-616. https://doi.org/10.1001/archsurg.1953.01260030616008
Makki K, Chorasiya V, Srivastava A, Singhal A, Khan AA, Vij V (2018) Analysis of caudate lobe biliary anatomy and its implications in living donor liver transplantation—a single centre prospective study. Transpl Int 31(9):1041-1049. https://doi.org/10.1111/tri.13272
Renz JF, Kinkhabwala M (2015) Surgical anatomy of the liver. In: Busuttil RW, Klintmalm GBG (eds) Transplantation of the Liver, 3rd edn. W.B. Saunders, Philadelphia, pp 23–39. https://doi.org/10.1016/B978-1-4557-0268-8.00002-6
Skandalakis LJ, Skandalakis JE, Skandalakis PN (2009) Surgical Anatomy and Technique: A Pocket Manual. Springer New York. https://doi.org/10.1007/978-0-387-09515-8
Chaib E, Kanas AF, Galvão FHF, D’Albuquerque LAC (2014) Bile duct confluence: anatomic variations and its classification. Surg Radiol Anat 36(2):105-109. https://doi.org/10.1007/s00276-013-1157-6
Huang TL, Cheng YF, Chen CL, Chen TY, Lee TY (1996) Variants of the bile ducts: clinical application in the potential donor of living-related hepatic transplantation. Transplant Proc 28(3):1669-1670.
Cheng YF, Huang TL, Chen CL, Chen YS, Lee TY (1997) Variations of the intrahepatic bile ducts: application in living related liver transplantation and splitting liver transplantation. Clin Transplant 11(4):337-340.
Cahalane AM, Mojtahed A, Sahani DV, Elias N, Kambadakone AR (2019) Pre-hepatic and pre-pancreatic transplant donor evaluation. Cardiovasc Diagn Ther 0(0):S97-S9S115. Accessed June 19, 2022. https://cdt.amegroups.com/article/view/22240
Jhaveri KS, Guo L, Guimarães L (2017) Current state-of-the-art MRI for comprehensive evaluation of potential living liver donors. Am J Roentgenol 209(1):55-66. https://doi.org/10.2214/AJR.16.17741
Artioli D, Tagliabue M, Aseni P, Sironi S, Vanzulli A (2010) Detection of biliary and vascular anatomy in living liver donors: value of gadobenate dimeglumine enhanced MR and MDCT angiography. Eur J Radiol 76(2):e1-e5. https://doi.org/10.1016/j.ejrad.2009.07.001
Ramesh Babu CS, Sharma M. (2014) Biliary tract anatomy and its relationship with venous drainage J Clin Exp Hepatol 4:S18-S26. https://doi.org/10.1016/j.jceh.2013.05.002
Northover JMA, Terblanche J (1979) A new look at the arterial supply of the bile duct in man and its surgical implications. Br J Surg 66(6):379-384. https://doi.org/10.1002/bjs.1800660603
Seiler CA (1999) The bile duct anastomosis in liver transplantation. Dig Surg 16(2):102-106. https://doi.org/10.1159/000018700
Vij V, Makki K, Chorasiya VK, Sood G, Singhal A, Dargan P (2016) Targeting the Achilles’ heel of adult living donor liver transplant: corner-sparing sutures with mucosal eversion technique of biliary anastomosis. Liver Transpl 22(1):14-23. https://doi.org/10.1002/lt.24343
Jung DH, Ikegami T, Balci D, Bhangui P (2020) Biliary reconstruction and complications in living donor liver transplantation. Int J Surg Lond Engl 82S:138-144. https://doi.org/10.1016/j.ijsu.2020.04.069
Saad WEA, Orloff MC, Davies MG, Waldman DL, Bozorgzadeh A (2007). Postliver transplantation vascular and biliary surgical anatomy. Tech Vasc Interv Radiol 10(3):172-190. https://doi.org/10.1053/j.tvir.2007.09.013
Wojcicki M, Milkiewicz P, Silva M (2008) Biliary tract complications after liver transplantation: a review. Dig Surg 25(4):245-257. https://doi.org/10.1159/000144653
Sundaram KM, Morgan MA, Itani M, Thompson W (2022). Imaging of benign biliary pathologies. Abdom Radiol. Published online February 24, 2022. https://doi.org/10.1007/s00261-022-03440-5
Greif F, Bronsther OL, Van Thiel DH, et al (1994) The incidence, timing, and management of biliary tract complications after orthotopic liver transplantation. Ann Surg 219(1):40-45. https://doi.org/10.1097/00000658-199401000-00007
Rao HB, Prakash A, Sudhindran S, Venu RP (2018) Biliary strictures complicating living donor liver transplantation: problems, novel insights and solutions. World J Gastroenterol 24(19):2061-2072. https://doi.org/10.3748/wjg.v24.i19.2061
Zimmerman MA, Baker T, Goodrich NP, et al (2013) Development, management, and resolution of biliary complications after living and deceased donor liver transplantation: a report from the A2ALL consortium. Liver Transplant 19(3):259-267. https://doi.org/10.1002/lt.23595
Hwang S, Lee SG, Sung KB, et al (2006) Long-term incidence, risk factors, and management of biliary complications after adult living donor liver transplantation. Liver Transpl 12(5):831-838. https://doi.org/10.1002/lt.20693
Koksal AS, Eminler AT, Parlak E, Gurakar A (2017) Management of biliary anastomotic strictures after liver transplantation. Transplant Rev 31(3):207-217. https://doi.org/10.1016/j.trre.2017.03.002
Riediger C, Müller MW, Michalski CW, et al (2010) T-tube or no T-tube in the reconstruction of the biliary tract during orthotopic liver transplantation: systematic review and meta-analysis. Liver Transpl 16(6):705-717. https://doi.org/10.1002/lt.22070
Brookmeyer CE, Bhatt S, Fishman EK, Sheth S (2022). Multimodality imaging after liver transplant: top 10 Important complications. Radiographics. Published online March 4, 2022:210108. https://doi.org/10.1148/rg.210108
Zheng BW, Tan YY, Fu BS, et al (2018) Tardus parvus waveforms in Doppler ultrasonography for hepatic artery stenosis after liver transplantation: can a new cut-off value guide the next step? Abdom Radiol N Y 43(7):1634-1641. https://doi.org/10.1007/s00261-017-1358-2
Tsujino T, Isayama H, Sugawara Y, et al (2006) Endoscopic management of biliary complications after adult living donor liver transplantation. Am J Gastroenterol 101(10):2230-2236. https://doi.org/10.1111/j.1572-0241.2006.00797.x
Kırnap M, Ayvazoğlu Soy EH, Akdur A, et al (2017) Incidence and treatment of bile stones after liver transplant. Exp Clin Transplant. Published online April 14, 2017. https://doi.org/10.6002/ect.2017.0023
Girometti R, Cereser L, Como G, Zuiani C, Bazzocchi M (2008) Biliary complications after orthotopic liver transplantation: MRCP findings. Abdom Imaging 33(5):542-554. https://doi.org/10.1007/s00261-007-9316-z
Lemmers A, Pezzullo M, Hadefi A, et al (2021) Biliary cast syndrome after liver transplantation: a cholangiographic evolution study. J Gastroenterol Hepatol 36(5):1366-1377. https://doi.org/10.1111/jgh.15318
Jagannath S, Kalloo AN (2002) Biliary complications after liver transplantation. Curr Treat Options Gastroenterol 5(2):101-112. https://doi.org/10.1007/s11938-002-0057-3
Zajko AB, Bennett MJ, Campbell WL, Koneru B (1990) Mucocele of the cystic duct remnant in eight liver transplant recipients: findings at cholangiography, CT, and US. Radiology 177(3):691-693. https://doi.org/10.1148/radiology.177.3.2243970
Chatterjee S, Das D, Hudson M, et al (2011) Mucocele of the cystic duct remnant after orthotopic liver transplant: a problem revisited. Exp Clin Transplant 9(3):214-216.
Koneru B, Zajko AB, Sher L, et al (1989) Obstructing mucocele of the cystic duct after transplantation of the liver. Surg Gynecol Obstet 168(5):394–396. PMID: 2652346; PMCID: PMC 2672429.
Liu Y, Sun LY, Zhu ZJ, et al (2021) Post-transplant lymphoproliferative disorder after paediatric liver transplantation. Int J Clin Pract 75(4):e13843. https://doi.org/10.1111/ijcp.13843
Tajima T, Hata K, Haga H, et al (2021) Post-transplant Lymphoproliferative disorders after liver transplantation: a retrospective cohort study including 1954 transplants. Liver Transpl 27(8):1165-1180. https://doi.org/10.1002/lt.26034
Kamdar KY, Rooney CM, Heslop HE (2011) Post-transplant lymphoproliferative disease following liver transplantation. Curr Opin Organ Transplant 16(3):274-280. https://doi.org/10.1097/MOT.0b013e3283465715
Torres V, Martinez N, Lee G, et al (2013) How do we manage post-OLT redundant bile duct? World J Gastroenterol WJG 19(16):2501-2506. https://doi.org/10.3748/wjg.v19.i16.2501
Wan P, Xia Q, Zhang JJ, et al (2015) Bile duct kinking after adult living donor liver transplantation: case reports and literature review. J Dig Dis 16(10):610-615. https://doi.org/10.1111/1751-2980.12263
Koo PT, Medici V, Tabibian JH (2018) Anastomotic Biliary stricture development after liver transplantation in the setting of retained prophylactic intraductal pediatric feeding tube: case and review. Case Rep Hepatol 2018:e4707389. https://doi.org/10.1155/2018/4707389
Sohn SH, Park JH, Kim KH, Kim TN (2017) Complications and management of forgotten long-term biliary stents. World J Gastroenterol 23(4):622-628. https://doi.org/10.3748/wjg.v23.i4.622
Londoño MC, Balderramo D, Cárdenas A (2008) Management of biliary complications after orthotopic liver transplantation: the role of endoscopy. World J Gastroenterol 14(4):493. https://doi.org/10.3748/wjg.14.493
Eckenschwiller M, Ackermann H, Bechstein WO, Grünwald F (2016) Accuracy of hepatobiliary scintigraphy after liver transplantation and liver resection. Int J Mol Imaging 2016:7857849. https://doi.org/10.1155/2016/7857849
Reddy S, Lopes Vendrami C, Mittal P, Borhani AA, Moreno CC, Miller FH (2021) MRI evaluation of bile duct injuries and other post-cholecystectomy complications. Abdom Radiol 46(7):3086-3104. https://doi.org/10.1007/s00261-020-02947-z
Lee NK, Kim S, Lee JW, et al (2009) Biliary MR Imaging with Gd-EOB-DTPA and Its Clinical Applications. Radiographics 29(6):1707-1724. https://doi.org/10.1148/rg.296095501
Jabłońska B, Lampe P (2009) Iatrogenic bile duct injuries: Etiology, diagnosis and management. World J Gastroenterol 15(33):4097-4104. https://doi.org/10.3748/wjg.15.4097
Green MH, Duell RM, Johnson CD, Jamieson NV (2001) Haemobilia. Br J Surg 88(6):773-786. https://doi.org/10.1046/j.1365-2168.2001.01756.x
Murugesan SD, Sathyanesan J, Lakshmanan A, et al (2014) Massive hemobilia: a diagnostic and therapeutic challenge. World J Surg 38(7):1755-1762. https://doi.org/10.1007/s00268-013-2435-5
Parvinian A, Fletcher JG, Storm AC, Venkatesh SK, Fidler JL, Khandelwal AR (2021) Challenges in diagnosis and management of hemobilia. Radiographics 41(3):802-813. https://doi.org/10.1148/rg.2021200192
Reau NS, Jensen DM (2008) Vanishing bile duct syndrome. Clin Liver Dis 12(1):203-217. https://doi.org/10.1016/j.cld.2007.11.007
Inomata Y, Tanaka K (2001) Pathogenesis and treatment of bile duct loss after liver transplantation. J Hepatobiliary Pancreat Surg 8(4):316-322. https://doi.org/10.1007/s005340170003
Ludwig J, Wiesner RH, Batts KP, Perkins JD, Krom RA (1987) The acute vanishing bile duct syndrome (acute irreversible rejection) after orthotopic liver transplantation. Hepatol Baltim Md 7(3):476-483. https://doi.org/10.1002/hep.1840070311
Boraschi P, Donati F (2014) Postoperative biliary adverse events following orthotopic liver transplantation: assessment with magnetic resonance cholangiography. World J Gastroenterol WJG 20(32):11080-11094. https://doi.org/10.3748/wjg.v20.i32.11080
Silveira MG, Talwalkar JA, Lindor KD, Wiesner RH (2010) Recurrent primary biliary cirrhosis after liver transplantation. Am J Transplant 10(4):720-726. https://doi.org/10.1111/j.1600-6143.2010.03038.x
Schreibman I, Regev A (2006) Recurrent primary biliary cirrhosis after liver transplantation—the disease and its management. Medscape Gen Med May 3; 8(2):30. PMID: 16926769; PMCID: PMC1785210
Meng Y, Liang Y, Liu M (2015) The value of MRI in the diagnosis of primary biliary cirrhosis and assessment of liver fibrosis. PloS One. 2015;10(3):e0120110. https://doi.org/10.1371/journal.pone.0120110
Ruemmele P, Hofstaedter F, Gelbmann CM (2009) Secondary sclerosing cholangitis. Nat Rev Gastroenterol Hepatol 6(5):287-295. https://doi.org/10.1038/nrgastro.2009.46
Fosby B, Karlsen TH, Melum E (2012) Recurrence and rejection in liver transplantation for primary sclerosing cholangitis. World J Gastroenterol 18(1):1-15. https://doi.org/10.3748/wjg.v18.i1.1
Graziadei IW, Wiesner RH, Batts KP, et al (1999) Recurrence of primary sclerosing cholangitis following liver transplantation. Hepatol Baltim Md 29(4):1050-1056. https://doi.org/10.1002/hep.510290427
Hernandez MDP, Martin P, Simkins J (2015) Infectious complications after liver transplantation. Gastroenterol Hepatol 11(11):741–753. PMID: 27134589; PMCID: PMC4849501
Camacho JC, Coursey-Moreno C, Telleria JC, Aguirre DA, Torres WE, Mittal PK (2015) Nonvascular post–liver transplantation complications: from us screening to cross-sectional and interventional imaging. Radiographics 35(1):87-104. https://doi.org/10.1148/rg.351130023
Fishman JA, Rubin RH (1998) Infection in organ-transplant recipients N Engl J Med 338(24):1741-1751. https://doi.org/10.1056/NEJM199806113382407
Bhargava P, Vaidya S, Dick AAS, Dighe M (2011) Imaging of orthotopic liver transplantation: review. Am J Roentgenol 196(3_supplement):WS15-WS25. https://doi.org/10.2214/AJR.09.7221
Itani M, Lalwani N, Anderson MA, Arif-Tiwari H, Paspulati RM, Shetty AS (2021). Magnetic resonance cholangiopancreatography: pitfalls in interpretation. Abdom Radiol N Y. Published online October 28, 2021. https://doi.org/10.1007/s00261-021-03323-1
Funding
No funding or research support for this article.
Author information
Authors and Affiliations
Contributions
The authors made substantial contributions to the conception or design of the work; drafted the work or revised it critically for important intellectual content; approved the version to be published; and agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Ethics approval
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Khot, R., Morgan, M.A., Nair, R.T. et al. Radiologic findings of biliary complications post liver transplantation. Abdom Radiol 48, 166–185 (2023). https://doi.org/10.1007/s00261-022-03714-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-022-03714-y