Abstract
Introduction
Previous studies indicated that location and amount of detected sentinel lymph nodes (SLNs) in prostate cancer (PCa) are influenced where SLN-tracer is deposited within the prostate. To validate whether intratumoral (IT) tracer injection helps to increase identification of tumor-positive lymph nodes (LNs) better than intraprostatic (IP) tracer injection, a prospective randomized phase II trial was performed.
Methods
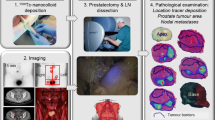
PCa patients with a > 5% risk of lymphatic involvement were randomized between ultrasound-guided transrectal injection of indocyanine green-[99mTc]Tc-nanocolloid in 2 depots of 1 mL in the tumor (n = 55, IT-group) or in 4 depots of 0.5 mL in the peripheral zone of the prostate (n = 58, IP-group). Preoperative lymphoscintigraphy and SPECT/CT were used to define the location of the SLNs. SLNs were dissected using combination of radio- and fluorescence-guidance, followed by extended pelvic LN dissection and robot-assisted radical prostatectomy. Outcome measurements were number of tumor-bearing SNs, tumor-bearing LNs, removed nodes, number of patients with nodal metastases, and metastasis-free survival (MFS) of 4–7-year follow-up data.
Results
IT-injection did not result in significant difference of removed SLNs (5.0 vs 6.0, p = 0.317) and histologically positive SLNs (28 vs 22, p = 0.571). However, in IT-group, the SLN-positive nodes were 73.7% of total positive nodes compared to 37.3% in IP-group (p = 0.015). Moreover, significantly more node-positive patients were found in IT-group (42% vs 24%, p = 0.045), which did not result in worse MFS. In two patients (3.6%) from whom the IT-tracer injection only partly covered intraprostatic tumor spread, nodal metastases in ePLND without tumor-positive SNs were yielded.
Conclusions
The percentage-positive SLNs found after IT-injection were significantly higher compared to IP-injection. Significantly more node-positive patients were found using IT-injection, which did not affect MFS. IT-injection failed to detect nodal metastases from non-index satellite lesions. Therefore, we suggest to combine IT- and IP-tracer injections in men with visible tumor on imaging.





Similar content being viewed by others
References
Mottet N, van den Bergh RCN, Briers E, Van den Broeck T, Cumberbatch MG, De Santis M, et al. EAU-EANM-ESTRO-ESUR-SIOG Guidelines on prostate cancer-2020 update. Part 1: Screening, Diagnosis, and Local Treatment with Curative Intent. Eur Urol. 2021;79(2):243–62.
Briganti A, Chun FK, Salonia A, Suardi N, Gallina A, Da Pozzo LF, et al. Complications and other surgical outcomes associated with extended pelvic lymphadenectomy in men with localized prostate cancer. Eur Urol. 2006;50(5):1006–13.
Mottet N, Bellmunt J, Bolla M, Briers E, Cumberbatch MG, De Santis M, et al. EAU-ESTRO-SIOG Guidelines on prostate cancer. Part 1: Screening, Diagnosis, and Local Treatment with Curative Intent. Eur Urol. 2017;71:618–29.
Jeschke S, Beri A, Grull M, Ziegerhofer J, Prammer P, Leeb K, et al. Laparoscopic radioisotope-guided sentinel lymph node dissection in staging of prostate cancer. Eur Urol. 2008;53(1):126–33.
KleinJan GH, van den Berg NS, de Jong J, Wit EM, Thygessen H, Vegt E, et al. Multimodal hybrid imaging agents for sentinel node mapping as a means to (re)connect nuclear medicine to advances made in robot-assisted surgery. Eur J Nucl Med Mol Imaging. 2016;43(7):1278–87.
Wit EM, Acar C, Grivas N, Yuan C, Horenblas S, Liedberg F, et al. Sentinel node procedure in prostate cancer: a systematic review to assess diagnostic accuracy. Eur Urol. 2016.
van der Poel HG, Wit EM, Acar C, van den Berg NS, van Leeuwen FWB, Valdes Olmos RA, et al. Sentinel node biopsy for prostate cancer: report from a consensus panel meeting. BJU Int. 2017;120(2):204–11.
Tanis PJ, Deurloo EE, Valdes Olmos RA, Rutgers EJ, Nieweg OE, Besnard AP, et al. Single intralesional tracer dose for radio-guided excision of clinically occult breast cancer and sentinel node. Ann Surg Oncol. 2001;8(10):850–5.
Estourgie SH, Nieweg OE, Valdes Olmos RA, Th Rutgers EJ, Kroon BB. Intratumoral versus intraparenchymal injection technique for lymphoscintigraphy in breast cancer. Clin Nucl Med. 2003;28(5):371–4.
Niebling MG, Pleijhuis RG, Bastiaannet E, Brouwers AH, van Dam GM, Hoekstra HJ. A systematic review and meta-analyses of sentinel lymph node identification in breast cancer and melanoma, a plea for tracer mapping. Eur J Surg Oncol. 2016;42(4):466–73.
Ahmed M, Purushotham AD, Horgan K, Klaase JM, Douek M. Meta-analysis of superficial versus deep injection of radioactive tracer and blue dye for lymphatic mapping and detection of sentinel lymph nodes in breast cancer. Br J Surg. 2015;102(3):169–81.
Sadeghi R, Asadi M, Treglia G, Zakavi SR, Fattahi A, Krag DN. Axillary concordance between superficial and deep sentinel node mapping material injections in breast cancer patients: systematic review and meta-analysis of the literature. Breast Cancer Res Treat. 2014;144(2):213–22.
Fowler JC, Solanki CK, Ballinger JR, Ravichandran D, Douglas-Jones A, Lawrence D, et al. Axillary lymph node drainage pathways from intradermal and intraparenchymal breast planes. J Surg Res. 2010;161(1):69–75.
Brouwer OR, Vermeeren L, van der Ploeg IM, Valdes Olmos RA, Loo CE, Pereira-Bouda LM, et al. Lymphoscintigraphy and SPECT/CT in multicentric and multifocal breast cancer: does each tumour have a separate drainage pattern? Results of a Dutch multicentre study (MULTISENT). Eur J Nucl Med Mol Imaging. 2012;39(7):1137–43.
Acar C, Kleinjan GH, van den Berg NS, Wit EM, van Leeuwen FW, van der Poel HG. Advances in sentinel node dissection in prostate cancer from a technical perspective. Int J Urol. 2015;22(10):898–909.
de Korne CM, Wit EM, de Jong J, Valdes Olmos RA, Buckle T, van Leeuwen FWB, et al. Anatomical localization of radiocolloid tracer deposition affects outcome of sentinel node procedures in prostate cancer. Eur J Nucl Med Mol Imaging. 2019;46(12):2558–68.
Buckle T, Brouwer OR, Valdes Olmos RA, van der Poel HG, van Leeuwen FW. Relationship between intraprostatic tracer deposits and sentinel lymph node mapping in prostate cancer patients. J Nuclear Med. 2012;53(7):1026–33.
Rais-Bahrami S, Turkbey B, Rastinehad AR, Walton-Diaz A, Hoang AN, Siddiqui MM, et al. Natural history of small index lesions suspicious for prostate cancer on multiparametric MRI: recommendations for interval imaging follow-up. Diagn Interv Radiol. 2014;20(4):293–8.
Briganti A, Larcher A, Abdollah F, Capitanio U, Gallina A, Suardi N, et al. Updated nomogram predicting lymph node invasion in patients with prostate cancer undergoing extended pelvic lymph node dissection: the essential importance of percentage of positive cores. Eur Urol. 2012;61(3):480–7.
van der Poel HG, Buckle T, Brouwer OR, Valdes Olmos RA, van Leeuwen FW. Intraoperative laparoscopic fluorescence guidance to the sentinel lymph node in prostate cancer patients: clinical proof of concept of an integrated functional imaging approach using a multimodal tracer. Eur Urol. 2011;60(4):826–33.
KleinJan GH, van den Berg NS, Brouwer OR, de Jong J, Acar C, Wit EM, et al. Optimisation of fluorescence guidance during robot-assisted laparoscopic sentinel node biopsy for prostate cancer. Eur Urol. 2014;66(6):991–8.
Meinhardt W, Valdes Olmos RA, Van Der Poel HG, Bex A, Horenblas S. Laparoscopic sentinel node dissection for prostate carcinoma: technical and anatomical observations. BJU Int. 2008;102(6):714–7.
van den Berg NS, Miwa M, KleinJan GH, Sato T, Maeda Y, van Akkooi AC, et al. (Near-infrared) fluorescence-guided surgery under ambient light conditions: a next step to embedment of the technology in clinical routine. Ann Surg Oncol. 2016;23(8):2586–95.
Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 2004;240(2):205–13.
Gharzai LA, Jiang R, Wallington D, Jones G, Birer S, Jairath N, et al. Intermediate clinical endpoints for surrogacy in localised prostate cancer: an aggregate meta-analysis. Lancet Oncol. 2021;22(3):402–10.
Kneppers J, Krijgsman O, Melis M, de Jong J, Peeper DS, Bekers E, et al. Frequent clonal relations between metastases and non-index prostate cancer lesions. JCI Insight. 2019;4(2).
Weckermann D, Holl G, Dorn R, Wagner T, Harzmann R. Reliability of preoperative diagnostics and location of lymph node metastases in presumed unilateral prostate cancer. BJU Int. 2007;99(5):1036–40.
Rouviere O, Puech P, Renard-Penna R, Claudon M, Roy C, Mege-Lechevallier F, et al. Use of prostate systematic and targeted biopsy on the basis of multiparametric MRI in biopsy-naive patients (MRI-FIRST): a prospective, multicentre, paired diagnostic study. Lancet Oncol. 2019;20(1):100–9.
KleinJan GH, van Werkhoven E, van den Berg NS, Karakullukcu MB, Zijlmans H, van der Hage JA, et al. The best of both worlds: a hybrid approach for optimal pre- and intraoperative identification of sentinel lymph nodes. Eur J Nucl Med Mol Imaging. 2018;45(11):1915–25.
Holl G, Dorn R, Wengenmair H, Weckermann D, Sciuk J. Validation of sentinel lymph node dissection in prostate cancer: experience in more than 2,000 patients. Eur J Nucl Med Mol Imaging. 2009;36(9):1377–82.
Siddiqui MM, Rais-Bahrami S, Turkbey B, George AK, Rothwax J, Shakir N, et al. Comparison of MR/ultrasound fusion-guided biopsy with ultrasound-guided biopsy for the diagnosis of prostate cancer. JAMA. 2015;313(4):390–7.
Funding
This work was partially supported by an ERC starting grant (2012–306890) and a NWO-TTW-VICI grant (TTW 16141).
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Oncology - Genitourinary
Rights and permissions
About this article
Cite this article
Wit, E.M.K., van Beurden, F., Kleinjan, G.H. et al. The impact of drainage pathways on the detection of nodal metastases in prostate cancer: a phase II randomized comparison of intratumoral vs intraprostatic tracer injection for sentinel node detection. Eur J Nucl Med Mol Imaging 49, 1743–1753 (2022). https://doi.org/10.1007/s00259-021-05580-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-021-05580-0