Abstract
Introduction
The present study aims to investigate the association of the femoral trochlear morphology with the risk of ACL injury and whether this can be considered an additional risk factor in this clinical table.
Materials and methods
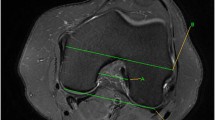
This is a retrospective case–control study with 93 patients, 41 patients with ACL total rupture (ACL-TR), and 52 patients without ACL injury who underwent knee magnetic resonance imaging (MRI) between January 2013 and January 2016. The femoral trochlear morphology was evaluated at the proximal and distal levels from the axial knee MRI. The morphological features of the trochlea using sulcus angle, sulcus depth, condylar heights, trochlear sulcus height, percentage of condyles and trochlear sulcus height to transepicondylar width, and lateral and medial trochlear inclination were evaluated. The notch width index was measured on the coronal MR images for notch stenos.
Results
ACL-TR group had a significantly higher sulcus angle (p = 0.00–0.001) and lower sulcus depth (p = 0.00–0.002) than the control group at both levels. Femoral trochlea had morphometric differences between genders. NWI was lower in the ACL-TR group than the control group (control 0.273; ACL-TR 0.247), and there was a statistically significant difference (p = 0.00).
Conclusion
This study was shown that the difference in morphology between the trochlear sulcus of patients with normal and ACL injuries should be taken into account in order to increase awareness of ACL injuries. We observed that mild trochlear dysplasia may cause intercondylar notch stenosis rather than changing the localization of the patella. Studies are needed regarding the effect of trochlear dysplasia on ACL.


Similar content being viewed by others
References
Boden BP, Dean GS, Feagin JA Jr, Garrett WE Jr. Mechanisms of anterior cruciate ligament injury. Orthopedics. 2000;23(6):573–8. https://doi.org/10.3928/0147-7447-20000601-15.
Yu B, Garrett WE. Mechanisms of non-contact ACL injuries. Br J Sports Med. 2007;41(Suppl 1):i47–51. bjsm.2007.03719/bjsm.2007.037192.
Griffin LY, Agel J, Albohm MJ, et al. Noncontact anterior cruciate ligament injuries: risk factors and prevention strategies. J Am Acad Orthop Surg. 2000;8(3):141–50. https://doi.org/10.5435/00124635-200005000-00001.
Escamilla RF, Macleod TD, Wilk KE, Paulos L, Andrews JR. Anterior cruciate ligament strain and tensile forces for weightbearing and non-weight-bearing exercises: a guide to exercise selection. J Orthop Sports Phys Ther. 2012;42(3):208–20. https://doi.org/10.2519/jospt.2012.3768.
Li H, Zeng C, Wang Y, et al. Association between magnetic resonance imaging-measured intercondylar notch dimensions and anterior cruciate ligament injury: a meta-analysis. Arthroscopy. 2018;34(3):889–900. https://doi.org/10.1016/j.arthro.2017.08.299.
Zeng C, Yang T, Wu S, et al. Is posterior tibial slope associated with noncontact anterior cruciate ligament injury? Knee Surg Sports Traumatol Arthrosc. 2016;24(3):830–7. https://doi.org/10.1007/s00167-014-3382-x.
Botchu R, Obaid H, Rennie WJ. Correlation between trochlear dysplasia and anterior cruciate ligament injury. J Orthop Surg. 2013;21(2):185–8. https://doi.org/10.1177/230949901302100214.
Chen M, Qin L, Li M, Shen J. Correlation analysis between femoral trochlear dysplasia and anterior cruciate ligament injury based on CT measurement. Quant Imaging Med Surg. 2020;10(4):847–52. https://doi.org/10.21037/qims.2020.03.15.
Ntagiopoulos PG, Bonin N, Sonnery-Cottet B, Badet R, Dejour D. The incidence of trochlear dysplasia in anterior cruciate ligament tears. Int Orthop. 2014;38(6):1269–75. https://doi.org/10.1007/s00264-014-2291-4.
Dejour H, Walch G, Nove-Josserand L, Guier C. Factors of patellar instability: an anatomic radiographic study. Knee Surg Sports Traumatol Arthrosc. 1994;2(1):19–26. https://doi.org/10.1007/bf01552649.
Feller JA, Amis AA, Andrish JT, Arendt EA, Erasmus PJ, Powers CM. Surgical biomechanics of the patellofemoral joint. Arthroscopy. 2007;23(5):542–53. https://doi.org/10.1016/j.arthro.2007.03.006.
Botchu R, Obaid H, Rennie WJ. Correlation between trochlear dysplasia and the notch index. J Orthop Surg (Hong Kong). 2013;21(3):290–3. https://doi.org/10.1177/230949901302100305.
Fleming BC, Ohlen G, Renstrom PA, Peura GD, Beynnon BD, Badger GJ. The effects of compressive load and knee joint torque on peak anterior cruciate ligament strains. Am J Sports Med. 2003;31(5):701–7. https://doi.org/10.1177/03635465030310051101.
Ha TP, Li KC, Beaulieu CF, et al. Anterior cruciate ligament injury: fast spin-echo MR imaging with arthroscopic correlation in 217 examinations. AJR Am J Roentgenol. 1998;170:1215–9. https://doi.org/10.2214/ajr.170.5.9574587.
Diederichs G, Issever AS, Scheffler S. MR imaging of patellar instability: injury patterns and assessment of risk factors. RadioGraphics. 2010;30:961–81. https://doi.org/10.1148/rg.304095755.
Charles MD, Haloman S, Chen L, Ward SR, Fithian D, Afra R. Magnetic resonance imaging-based topographical differences between control and recurrent patellofemoral instability patients. Am J Sports Med. 2013;41(2):374–84. https://doi.org/10.1177/0363546512472441.
Duran S, Cavusoglu M, Kocadal O, Sakman B. Association between trochlear morphology and chondromalacia patella: an MRI study. Clin Imaging. 2017;41:7–10. https://doi.org/10.1016/j.clinimag.2016.09.008.
Pfirrmann CW, Zanetti M, Romero J, Hodler J. Femoral trochlear dysplasia: MR findings. Radiology. 2000;216(3):858–64. https://doi.org/10.1148/radiology.216.3.r00se38858.
Tsavalas N, Katonis P, Karantanas AH. Knee joint anterior malalignment and patellofemoral osteoarthritis: an MRI study. Eur Radiol. 2012;22(2):418–28. https://doi.org/10.1007/s00330-011-2275-3.
Tuna BK, Semiz-Oysu A, Pekar B, Bukte Y, Hayirlioglu A. The association of patellofemoral joint morphology with chondromalacia patella: a quantitative MRI analysis. Clin Imaging. 2014;38(4):495–8. https://doi.org/10.1016/j.clinimag.2014.01.012.
Bisson LJ, Gurske-DePerio J. Axial and sagittal knee geometry as a risk factor for noncontact anterior cruciate ligament tear: a case-control study. Arthroscopy. 2010;26(7):901–6. https://doi.org/10.1016/j.arthro.2009.12.012.
Nelitz M, Lippacher S, Reichel H, Dornacher D. Evaluation of trochlear dysplasia using MRI: correlation between the classification system of Dejour and objective parameters of trochlear dysplasia. Knee Surg Sports Traumatol Arthrosc. 2014;22(1):120–7. https://doi.org/10.1007/s00167-012-2321-y.
Biedert RM, Bachmann M. Anterior-posterior trochlear measurements of normal and dysplastic trochlea by axial magnetic resonance imaging. Knee Surg Sports Traumatol Arthrosc. 2009;17(10):1225–30. https://doi.org/10.1007/s00167-009-0824-y.
Carrillon Y, Abidi H, Dejour D, Fantino O, Moyen B, Tran-Minh VA. Patellar instability: assessment on MR images by measuring the lateral trochlear inclination-initial experience. Radiology. 2000;216(2):582–5. https://doi.org/10.1148/radiology.216.2.r00au07582.
Stein V, Li L, Guermazi A, et al. The relation of femoral notch stenosis to ACL tears in persons with knee osteoarthritis. Osteoarthr Cartil. 2010;18:192–9. https://doi.org/10.1016/j.joca.2009.09.006.
Hoteya K, Kato Y, Motojima S, et al. Association between intercondylar notch narrowing and bilateral anterior cruciate ligament injuries in athletes. Arch Orthop Trauma Surg. 2011;131:371–6. https://doi.org/10.1007/s00402-010-1254-5.
Souryal TO, Freeman TR. Intercondylar notch size and anterior cruciate ligament injuries in athletes. A prospective study. Am J Sports Med. 1993;21:535–9. https://doi.org/10.1177/036354659302100410.
Amis AA, Oguz C, Bull AM, Senavongse W, Dejour D. The effect of trochleoplasty on patellar stability and kinematics: a biomechanical study in vitro. J Bone Joint Surg (Br). 2008;90(7):864–9. https://doi.org/10.1302/0301-620X.90B7.20447.
Van Haver A, De Roo K, De Beule M, et al. The effect of trochlear dysplasia on patellofemoral biomechanics: a cadaveric study with simulated trochlear deformities. Am J Sports Med. 2015;43(6):1354–61. https://doi.org/10.1177/0363546515572143.
Dejour D, Le Coultre B. Osteotomies in patello-femoral instabilities. Sports Med Arthrosc. 2007;15(1):39–46. https://doi.org/10.1097/JSA.0b013e31803035ae.
Carter JC, Sturnick DR, Vacek PM, et al. Relationship between geometry of the extensor mechanism of the knee and risk of anterior cruciate ligament injury. J Orthop Res. 2017;35(5):965–73. https://doi.org/10.1002/jor.23366.
Salzmann GM, Weber TS, Spang JT, Imhoff AB, Schöttle PB. Comparison of native axial radiographs with axial MR imaging for determination of the trochlear morphology in patients with trochlear dysplasia. Arch Orthop Trauma Surg. 2010;130(3):335–40. https://doi.org/10.1007/s00402-009-0912-y.
Bollier M, Fulkerson JP. The role of trochlear dysplasia in patellofemoral instability. J Am Acad Orthop Surg. 2011;19(1):8–16. https://doi.org/10.5435/00124635-201101000-00002.
Wright SJ, Boymans TA, Grimm B, Miles AW, Kessler O. Strong correlation between the morphology of the proximal femur and the geometry of the distal femoral trochlea. Knee Surg Sports Traumatol Arthrosc. 2014;22(12):2900–10. https://doi.org/10.1007/s00167-014-3343-4.
Chhabra A, Subhawong TK, Carrino JA. A systematized MRI approach to evaluating the patellofemoral joint. Skelet Radiol. 2011;40(4):375–87. https://doi.org/10.1007/s00256-010-0909-1.
Hewett TE, Myer GD, Ford KR, et al. Biomechanical measures of neuromuscular control and valgus loading of the knee predict anterior cruciate ligament injury risk in female athletes: a prospective study. Am J Sports Med. 2005;33(4):492–501. https://doi.org/10.1177/0363546504269591.
Van Haver A, De RK, De BM, et al. Semi-automated landmark-based 3D analysis reveals new morphometric characteristics in the trochlear dysplastic femur. Knee Surg Sports Traumatol Arthrosc. 2014;22:2698–708. https://doi.org/10.1007/s00167-013-2573-1.
Acknowledgements
We would like to our gratitude to Neslihan Onder Ozdemir (PhD in the University of Sheffield, UK) for doing the article’s “spell check” and “grammar check.”
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
This study was approved by the Ethics Committee of Clinical Investigations of the Bursa Uludag University Faculty of Medicine (2015-17/19, 29.09.2015). All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
As this study was retrospective, radiological images were used with the approval of the ethics committee without obtaining an informed consent form.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Isıklar, S., Ozdemir, S.T. & Gokalp, G. An association between femoral trochlear morphology and non-contact anterior cruciate ligament total rupture: a retrospective MRI study. Skeletal Radiol 50, 1441–1454 (2021). https://doi.org/10.1007/s00256-020-03706-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-020-03706-3