Abstract
Background
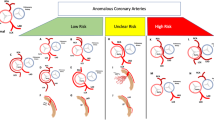
Morphological features including interarterial course, intramural course, high ostial location and slit-like ostium are presumed risk factors for sudden cardiac death in children with anomalous aortic origin of the coronary artery (AAOCA). To facilitate clinical risk stratification, the diagnostic accuracy of CT angiography for individual risk factors in the setting of AAOCA must be established.
Objective
We assessed diagnostic accuracy of standardized CT angiography interpretation for morphological characteristics that might determine risk in children with AAOCA by comparing them to surgical findings.
Materials and methods
We created a standardized protocol for CT angiography of AAOCA and retrospectively evaluated diagnostic performance in 25 consecutive surgical patients. Relevant morphological variables in AAOCA were assessed by three independent blinded readers, with surgery as the reference standard. We used Cohen kappa coefficients and accuracies to assess agreement between readers and surgical findings, and we calculated intraclass correlation coefficients to compare length of the intramural course.
Results
CT angiography correctly identified AAOCA in all patients. For the three readers, accuracies for detecting ostial stenosis were 84%, 94% and 96%; for high ostial origin, accuracies were 76%, 78% 82%; for intramurality using the peri-coronary fat sign, accuracies were 98%, 96% and 92%; and for intramurality using oval shape of coronary artery, accuracies were 98%, 94% and 92%. The intraclass correlation coefficients (ICCs) for predicting intramural length among the three readers were 0.67, 0.75 and 0.81 using peri-coronary fat, and 0.69, 0.50 and 0.81 using oval shape, respectively.
Conclusion
CT angiography reliably identified AAOCA in all children and detected the presence of intramurality with high accuracy.








Similar content being viewed by others
References
Maron BJ, Doerer JJ, Haas TS et al (2009) Sudden deaths in young competitive athletes: analysis of 1,866 deaths in the United States, 1980-2006. Circulation 119:1085–1092
Basso C, Maron BJ, Corrado D, Thiene G (2000) Clinical profile of congenital coronary artery anomalies with origin from the wrong aortic sinus leading to sudden death in young competitive athletes. J Am Coll Cardiol 35:1493–1501
Angelini P (2014) Novel imaging of coronary artery anomalies to assess their prevalence, the causes of clinical symptoms, and the risk of sudden cardiac death. Circ Cardiovasc Imaging 7:747–754
Taylor AJ, Byers JP, Cheitlin MD, Virmani R (1997) Anomalous right or left coronary artery from the contralateral coronary sinus: “high-risk” abnormalities in the initial coronary artery course and heterogeneous clinical outcomes. Am Heart J 133:428–435
Jegatheeswaran A, Devlin PJ, McCrindle BW et al (2019) Features associated with myocardial ischemia in anomalous aortic origin of a coronary artery: a Congenital Heart Surgeons' Society study. J Thorac Cardiovasc Surg 158:822–834.e3
Frescura C, Basso C, Thiene G et al (1998) Anomalous origin of coronary arteries and risk of sudden death: a study based on an autopsy population of congenital heart disease. Hum Pathol 29:689–695
Eckart RE, Scoville SL, Campbell CL et al (2004) Sudden death in young adults: a 25-year review of autopsies in military recruits. Ann Intern Med 141:829–834
Warnes CA, Williams RG, Bashore TM et al (2008) ACC/AHA 2008 guidelines for the management of adults with congenital heart disease: a report of the American College of Cardiology/American Heart Association task force on practice guidelines (writing committee to develop guidelines on the management of adults with congenital heart disease). Developed in collaboration with the American Society of Echocardiography, Heart Rhythm Society, International Society for Adult Congenital Heart Disease, Society for Cardiovascular Angiography and Interventions, and Society of Thoracic Surgeons. J Am Coll Cardiol 52:e143–e263
Mery CM, Lawrence SM, Krishnamurthy R et al (2014) Anomalous aortic origin of a coronary artery: toward a standardized approach. Semin Thoracic Surg 26:110–122
Balasubramanya S, Mongé MC, Eltayeb OM et al (2017) Anomalous aortic origin of a coronary artery: symptoms do not correlate with intramural length or ostial diameter. World J Pediatr Congenit Heart Surg 8:445–452
Lederlin M, Thambo J-B, Latrabe V et al (2011) Coronary imaging techniques with emphasis on CT and MRI. Pediatr Radiol 41:1516–1525
Shriki JE, Shinbane JS, Rashid MA et al (2012) Identifying, characterizing, and classifying congenital anomalies of the coronary arteries. Radiographics 32:453–468
Mery CM, De Leon LE, Molossi S et al (2018) Outcomes of surgical intervention for anomalous aortic origin of a coronary artery: a large contemporary prospective cohort study. J Thorac Cardiovasc Surg 155:305–319
Sun Z, Dimpudus FJ, Nugroho J, Adipranoto JD (2010) CT virtual intravascular endoscopy assessment of coronary artery plaques: a preliminary study. Eur J Radiol 75:e112–e119
Cicchetti DV, Sparrow SA (1981) Developing criteria for establishing interrater reliability of specific items: applications to assessment of adaptive behavior. Am J Ment Defic 86:127–137
Girzadas M, Varga P, Dajani K (2009) A single-center experience of detecting coronary anomalies on 64-slice computed tomography. J Cardiovasc Med 10:842–847
Miller JA, Anavekar NS, Yaman El MM et al (2012) Computed tomographic angiography identification of intramural segments in anomalous coronary arteries with interarterial course. Int J Cardiovasc Imaging 28:1525–1532
Jadhav SP, Golriz F, Atweh LA et al (2015) CT angiography of neonates and infants: comparison of radiation dose and image quality of target mode prospectively ECG-gated 320-MDCT and ungated helical 64-MDCT. AJR Am J Roentgenol 204:W184–W191
Sun Z, Ng K-H (2012) Prospective versus retrospective ECG-gated multislice CT coronary angiography: a systematic review of radiation dose and diagnostic accuracy. Eur J Radiol 81:e94–e100
Clemente A, Del Borrello M, Greco P et al (2010) Anomalous origin of the coronary arteries in children: diagnostic role of three-dimensional coronary MR angiography. Clin Imaging 34:337–343
Beerbaum P, Sarikouch S, Laser K-T et al (2009) Coronary anomalies assessed by whole-heart isotropic 3D magnetic resonance imaging for cardiac morphology in congenital heart disease. J Magn Reson Imaging 29:320–327
Biko DM, Chung C, Hitt DM et al (2015) High-resolution coronary MR angiography for evaluation of patients with anomalous coronary arteries: visualization of the intramural segment. Pediatr Radiol 45:1146–1152
Han F, Rapacchi S, Khan S et al (2015) Four-dimensional, multiphase, steady-state imaging with contrast enhancement (MUSIC) in the heart: a feasibility study in children. Magn Reson Med 74:1042–1049
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Online Supplementary Material 1
Uniform clinical algorithm to evaluate and manage children with anomalous aortic origin of a coronary artery (AAOCA). CHSS Congenital Heart Surgeon’s Society, ECG electrocardiogram, TCH Texas Children’s Hospital. Copyright 2014 Texas Children’s Hospital (reprinted with permission) (PNG 36 kb)
Online Supplementary Material 2
Bland–Altman plots for the three independent blinded readers for measuring length of intramural course using the peri-coronary fat sign (top row, a–c), and oval cross-sectional shape of the coronary artery (bottom row, d–f). IM intramural (PNG 17 kb)
Rights and permissions
About this article
Cite this article
Krishnamurthy, R., Masand, P.M., Jadhav, S.P. et al. Accuracy of computed tomography angiography and structured reporting of high-risk morphology in anomalous aortic origin of coronary artery: comparison with surgery. Pediatr Radiol 51, 1299–1310 (2021). https://doi.org/10.1007/s00247-021-05011-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-021-05011-0