Abstract
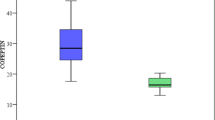
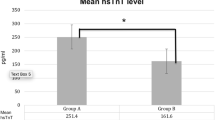
To analyze the role of sensitive cardiac troponin I (scTnI) and high-sensitive troponin T (hscTnT) in the determination of myocardial injury caused by volume and pressure load due to pulmonary hypertension (PH) and to investigate if these markers may be useful in the management of PH in childhood. Twenty-eight patients with congenital heart disease (CHD) with left to right shunt and PH, 29 patients with CHD with left to right shunt but without PH, and 18 healthy children, in total 75 individuals, were included in the study. All cases were aged between 4 and 36 months. Echocardiographic evaluation was performed in all cases, and invasive hemodynamic investigation was performed in 33 cases. Blood samples were obtained from all cases, for the measurement of brain natriuretic peptide (BNP), pro-brain natriuretic peptide (pro-BNP), sensitive cardiac troponin I (scTnI), and high-sensitive troponin T (hscTnT) levels. The mean BNP, pro-BNP, scTnI, and hsTnT levels were statistically significantly higher in patients with PH than in the patients without PH (p < 0.001). A statistically significant positive correlation was determined between pulmonary artery systolic pressure and scTnI and hscTnT levels (r = 0.34 p = 0.01, r = 0.46 p < 0.001, respectively) levels. Pulmonary hypertension determined in congenital heart diseases triggers myocardial damage independently of increased volume or pressure load and resistance, occurring by disrupting the perfusion via increasing ventricular wall tension and the myocardial oxygen requirement. Serum scTnI and hscTnT levels may be helpful markers to determine the damage associated with PH in childhood.

Similar content being viewed by others
References
Olguntürk R (2010) Pediatric pulmonary hypertension and pulmonary arterial hypertension secondary to congenital heart diseases. Anadol Kardiyol Derg 10:50–56
Lammers AE, Apitz C, Zartner P, Hager A, Dubowy KO, Hansmann G (2016) Diagnostics, monitoring and outpatient care in children with suspected pulmonary hypertension/paediatric pulmonary hypertensive vascular disease. Expert consensus statement on the diagnosis and treatment of paediatric pulmonary hypertension. The European Paediatric Pulmonary Vascular Disease Network, endorsed by ISHLT and DGPK. Heart 102:1–13
Haworth SG (2006) The management of children with congenital heart disease. Pulmonary Arterial Hypertension Related to Congenital Heart Disease 1st ed. London
Joshi R, Kalra R, Kumar N, Aggarwal N (2016) Critical decision of operability in congenital heart disease patient with severe pulmonary hypertension. Ann Card Anaesth 19:744
Apitz C, Hansmann G, Schranz D (2016) Hemodynamic assessment and acute pulmonary vasoreactivity testing in the evaluation of children with pulmonary vascular disease. Expert consensus statement on the diagnosis and treatment of paediatric pulmonary hypertension. The European Paediatric Pulmonary Vascular Disease Network, endorsed by ISHLT and DGPK. Heart 102:23–29
Hoeper MM, Lee SH, Voswinckel R, Palazzini M, Jais X, Marinelli A (2006) Complications of right heart catheterization procedures in patients with pulmonary hypertension in experienced centers. J Am Coll Cardiol 48:2546–2552
Pattathu J, Gorenflo M, Hilgendorff A, Koskenvuo JW, Apitz C, Hansmann G, Alastalo TP (2016) Genetic testing and blood biomarkers in paediatric pulmonary hypertension. Expert consensus statement on the diagnosis and treatment of paediatric pulmonary hypertension. The European Paediatric Pulmonary Vascular Disease Network, endorsed by ISHLT and DGPK. Heart 102:36–41
Pezzuto B, Badagliacca R, Poscia R, Ghio S, D’Alto M, Vitulo P, Mulè M, Albera C, Volterrani M, Fedele F, Vizza CD (2015 Mar) Circulating biomarkers in pulmonary arterial hypertension: update and future direction. J Heart Lung Transplant 34:282–305
Yilmaz MB, Zorlu A, Dogan OT, Karahan O, Tandogan I, Akkurt I (2011) Role of CA-125 in identification of right ventricular failure in chronic obstructive pulmonary disease. Clin Cardiol 34:244–248
Oguz MM, Oguz AD, Sanli C, Cevik A (2014) Serum levels of soluble ICAM-1 in children with pulmonary artery hypertension. Tex Heart Inst J 4:159–164
Yıldırım A, Güzelmeriç F, Öner CN, Karaağaç AT, Şaşmazel A, Erdem H, Özdemir O, Baysal A (2014) Prognostic significance of sICAM-1 and sVCAM-1 molecules for cardiac surgery in pediatric patients with pulmonary hypertension. Anadolu Kardiyol Derg 14:274–279
Garg P, Morris P, Fazlanie AL, Vijayan S, Dancso B, Dastidar AG, Plein S, Mueller C, Haaf P (2017) Cardiac biomarkers of acute coronary syndrome: from history to high-sensitivity cardiac troponin. Intern Emerg Med 12:147–155
Hafez MO, Morsy SM, Mahfoz RA, Ali AR (2015) Myocardial injury in children with unoperated congenital heart diseases. Cardiol Res Pract. https://doi.org/10.1155/2015/104818
Torbicki A, Kurzyna M, Kuca P, Fijałkowska A, Sikora J, Florczyk M et al (2003) Detectable serum cardiac troponin T as a marker of poor prognosis among patients with chronic precapillary pulmonary hypertension. Circulation 108:844–848
Antman EM (2002) Decision making with cardiac troponin tests. N Engl J Med 346:2079–2082
Mair J (2014) High-sensitivity cardiac troponins in everyday clinical practice. World J Cardiol 6:175–182
Kunii Y, Kamada M, Ohtsuki S, Araki T, Kataoka K, Kageyama M et al (2003) Plasma brain natriuretic peptide and the evaluation of volume overload in infants and children with congenital heart disease. Acta Med Okayama 57(4):191–197
Bader D, Kugelman A, Lanir A, Tamir A, Mula E, Riskin A (2006) Cardiac troponin I serum concentrations in newborns: a study and review of literature. Clin Chin Acta 371(1–2):61–65
Bossone E, D’Andrea A, D’Alto M, Citro R, Argiento P, Ferrara F et al (2013) Echocardiography in pulmonary arterial hypertension: from diagnosis to prognosis. J Am Soc Echocardiogr 26:1–14
Apple FS, Wu AHB, Jaffe AS (2002) European Society of Cardiology and American College of Cardiology guidelines for redefinition of myocardial infarction: how to use existing assays clinically and for clinical trials. Am Heart J 144:981–986
Apple FS, Wu AHB (2001) Myocardial infarction redefined: role of cardiac troponin testing. Clin Chem 47:377–379
Antman EM, Tanasijevic MJ, Thompson B et al (1996) Cardiac-specific troponin I levels to predict the risk of mortality in patients with acute coronary syndromes. N Eng J Med 335:1342–1349
Venge P, Langerquist B, Diderholm E et al (2002) On behalf of the FRISC II Study Group. Clinical Performance of three cardiac troponin assays in patients with unstable coronary artery disease (FRISC II substudy). Am J Cardiol 89:1035–1041
Özhan H, Albayrak S, Uzun H,et al (2007) Correlation of plasma B Type natriuretic peptide with shunt severity in patients with atrial or ventricular septal defect. Pediatr Cardiol 28:272–275
Holmström H, Hall C, Thaulow E (2001) Plasma levels of natriuretic peptides and hemodynamic assessment of patent ductus arteriosus in preterm infants. Acta Paediatr 90:184–191
Leuchte HH, Holzapfel M, Baumgartner RA et al (2005) Characterization of brain natriuretic peptide in long-term follow-up of pulmonary arterial hypertension. Chest 128:2368–2374
Fijalkowska A, Kurzyna M, Torbicki A et al (2006) Serum N-terminal brain natriuretic peptide as a prognostic parameter in patients with pulmonary hypertension. Chest 129:1313–1321
Conen D, Pfisterer M, Martina B (2006) Substantial intraindividual variability of BNP concentrations in patients with hypertension. J Hum Hypertens 20:387–391
Takatsuki S, Wagner BD, Ivy D (2012) B-type natriuretic peptide and amino-terminal pro-B-type natriuretic peptide in pediatric patients with pulmonary arterial hypertension. Congenit Heart Dis 7(3):259–267
Bernus A, Wagner BD, Accurso F et al. (2009) Brain natriuretic peptide levels in managing pediatric patients with pulmonary arterial hypertension. Chest 135(3):745–751
Galie N, Manes A, Palazzini M et al (2008) Management of pulmonary arterial hypertension associated with congenital systemic-to-pulmonary shunts and Eisenmenger’s syndrome. Drugs 68:1049–1066
Kubo T, Kitaoka H, Okawa M et al (2010) Serum cardiac troponin I is related to increased left ventricular wall thickness, left ventricular dysfunction, and male gender in hypertrophic cardiomyopathy. Clin Cardiol 33:E1–E7
Petersen SE, Jerosch-Herold M, Hudsmith LE et al (2007) Evidence for microvascular dysfunction in hypertrophic cardiomyopathy: new insights from multiparametric magnetic resonance imaging. Circulation 115:2418–2425
Galderisi M (2007) Epicardial coronary vessels and coronary microcirculation in pressure overload hypertrophy: a complex interaction. Am J Hypertens 20:285–286.
Apple FS (2009) A new season for cardiac troponin assays: it’s time to keep a scorecard. Clin Chem 55:7 1303–1306
Xu RY, Zhu XF, Yang Y, Ye P (2013) High-sensitive cardiac troponin T. J Geriatr Cardiol 10:102–109
Colvin KL, Dufva MJ, Delaney RP, Ivy DD, Stenmark KR, Yeager M (2014) Biomarkers for pediatric pulmonary arterial hypertension—a call to collaborate. Front Pediatr 2:1–12
Zelniker T, Uhlmann L, Spaich S, Friedrich J, Preusch MR, Meyer FJ et al. (2015) Novel biomarkers for risk stratification in pulmonary arterial hypertension. ERJ Open Res 1:00008-2015
Eggers KM, Lindahl B (2017) Application of cardiac troponin in cardiovascular diseases other than acute coronary syndrome. Clin Chem 63:223–235
Sugimoto M, Ota K, Kajihama A, Nakau K et al (2011) Volume overload and pressure overload due to left-to-right shunt- induced myocardial injury: evaluation using a highly sensitive cardiac troponin I assay in children with congenital heart disease. Circ J 75:2213–2219
Eerola A, Jokinen EO, Savukoski TI et al (2013) Cardiac troponin I in congenital heart defects with pressure or volume overload. Scand Cardiovasc J 47:154–159
Filusch A, Giannitsis E, Katus HA, Meyer FJ (2010) High-sensitive troponin T: a novel biomarker for prognosis and disease severity in patients with pulmonary arterial hypertension. Clin Sci 119:207–213
Apple FS (1999) Clinical and analytical standardization ıssues confronting cardiac troponin I. Clin Chem 45(1):18–20
Labugger R, Organ L, Collier C et al (2000) Extensive troponin I and T modification detected in serum from patients with acute myocardial infarction. Circulation 102:1221–1226
Tate JR, Heathcote D, Rayfield J, Hickman PE (1999) The lack of standardization of cardiac troponin I assay systems. Clin Chim Acta 284:141–149
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interest.
Rights and permissions
About this article
Cite this article
Kayali, S., Ertugrul, I., Yoldas, T. et al. Sensitive Cardiac Troponins: Could They Be New Biomarkers in Pediatric Pulmonary Hypertension Due to Congenital Heart Disease?. Pediatr Cardiol 39, 718–725 (2018). https://doi.org/10.1007/s00246-018-1811-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-018-1811-1