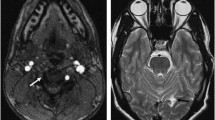
Abstract
Introduction
The purpose of this study was to analyse MR imaging features and lesion patterns as defined by compromised vascular territories, correlating them to different clinical syndromes and aetiological aspects.
Methods
In a 19.8-year period, clinical records and magnetic resonance imaging (MRI) features of 55 consecutive patients suffering from spinal cord ischemia were evaluated.
Results
Aetiologies of infarcts were arteriosclerosis of the aorta and vertebral arteries (23.6 %), aortic surgery or interventional aneurysm repair (11 %) and aortic and vertebral artery dissection (11 %), and in 23.6 %, aetiology remained unclear. Infarcts occurred in 38.2 % at the cervical and thoracic level, respectively, and 49 % of patients suffered from centromedullar syndrome caused by anterior spinal artery ischemia. MRI disclosed hyperintense pencil-like lesion pattern on T2WI in 98.2 %, cord swelling in 40 %, enhancement on post-contrast T1WI in 42.9 % and always hyperintense signal on diffusion-weighted imaging (DWI) when acquired.
Conclusion
The most common clinical feature in spinal cord ischemia is a centromedullar syndrome, and in contrast to anterior spinal artery ischemia, infarcts in the posterior spinal artery territory are rare. The exclusively cervical location of the spinal sulcal artery syndrome seems to be a likely consequence of anterior spinal artery duplication which is observed preferentially here.












Similar content being viewed by others
References
Novy J, Carruzzo A, Maeder P, Bogousslavsky J (2006) Spinal cord ischemia. Clinical and imaging patterns, pathogenesis and outcomes in 27 patients. Arch Neurol 63:1113–1120
Turnbull IM, Brieg A, Hassler O (1966) Blood supply of cervical spinal cord in man. A microangiographic cadaver study. J Neurosurg 24:951–965
Lazorthes G (1972) Pathology, classification and clinical aspects of vascular diseases in spinal cord. In: Vinken PJ, Bruyn GW (eds) Handbook of clinical neurology, vol 12. North Holland, Amsterdam, pp 492–506
Thron A (ed) (1989) Vascularisation of the spinal cord. Springer, Heidelberg
Martirosyan N, Feuerstein J, Theodore N, Cavalcanti D, Spetzler R, Preul M (2011) Blood supply and vascular reactivity of the spinal cord under normal and pathological conditions. J Neurosurg Spine 15:238–251
Crum B, Mokri B, Fulgham J (2000) Spinal manifestations of vertebral artery dissection. Neurology 55:304–306
Weidauer S, Gartenschläger M, Claus D (1999) Spinal sulcal artery syndrome due to bilateral vertebral artery dissection. J Neurol Neurosurg Psychiatry 67:550–551
Weidauer S, Nichtweiss M, Lanfermann H, Zanella FE (2002) Spinal cord infarction: MR imaging and clinical features in 16 cases. Neuroradiology 44:851–857
Bergqvist C, Goldberg HI, Thorarensen O, Bird SJ (1997) Posterior cervical spinal cord infarction following vertebral artery dissection. Neurology 48:1112–1115
Laufs H, Weidauer S, Heller C, Lorenz M, Neumann-Haefelin T (2004) Hemi-spinal cord infarction due to vertebral artery dissection in congenital afibrinogenemia. Neurology 63:1522–1523
Goldsmith P, Rowe D, Jäger R, Kapoor R (1998) Focal vertebral artery dissection causing Brown–Séquard’s syndrome. J Neurol Neurosurg Psychiatry 64:415–416
Richard S, Abdallah R, Chanson A, Foscolo S, Baillot PA, Ducrocq X (2014) Unilateral posterior cervical spinal cord infarction due to spontaneous vertebral artery dissection. J Spinal Cord Med 37:233–236
Cheng MY, Lyu RK, Chang YJ, Chen RS, Huang CC, Wu T, Lee TH, Lu SC, Ro LS (2008) Spinal cord infarction in Chinese patients. Clinical features, risk factors, imaging and prognosis. Cerebrovasc Dis 26:502–508
Walden JE, Castillo M (2012) Sildenafil-induced cervical spinal cord infarction. AJNR Am J Neuroradiol 33:E32–E33
Tosi L, Rigoli G, Beltramello A (1996) Fibrocartilaginous embolism of the spinal cord: a clinical and pathogenetic reconsideration. J Neurol Neurosurg Psychiatry 60:55–60
Mikulis DJ, Ogilvy S, McKee A, Davis KR, Ojeman RG (1992) Spinal cord infarction and fibrocartilagenous emboli. AJNR Am J Neurorad 13:155–160
Masson C, Boukriche Y, Berthelot JL, Colombani JM (2001) Vertebra, rib and spinal cord infarction caused by probable fibrocartilaginous embolism. Cerebrovasc Dis 12:142–143
Piao YS, Lu DH, Su YY, Yang XP (2009) Anterior spinal cord infarction caused by fibrocartilaginous embolism. Neuropathology 29:172–175
Manara R, Calderone M, Severino MS, Citton V, Toldo I, Laverda AM, Sartori S (2010) Spinal cord infarction due to fibrocartilaginous embolization: the role of diffusion weighted imaging and short-tau inversion recovery frequencies. J Child Neurol 25:1024–1028
Furtner M, Felber S, Poewe W (2005) Spinal fibrocartilaginous embolism. Nervenarzt 76:1246–1249
Mull M (2005) Acute spinal cord ischemia: diagnosis without therapeutic options? Clin Neuroradiol 15:79–88
Orme HT, Smith AG, Nagel MA, Bert RJ, Mickelson TS, Gilden DH (2007) VZV spinal cord infarction identified by diffusion-weighted MRI (DWI). Neurology 69:398–400
Katramados AM, Rabah R, Adams MD, Huq AHMM, Mitsias PD (2008) Longitudinal myelitis, aseptic meningitis, and conus medullaris infarction as presenting manifestations of pediatric systemic lupus erythematosus. Lupus 17:332–336
Márquez JC, Granados AM, Castillo M (2012) MRI of cervical spinal cord infarction in a patient with sickle cell disease. Clin Imaging 36:595–598
Gilden D, Cohrs RJ, Mahalingam R, Nagel MA (2009) Varicella zoster virus vasculopathies: diverse clinical manifestations, laboratory features, pathogenesis and treatment. Lancet Neurol 8:731–740
Di Lazzaro V, Restuccia D, Oliveiro A, Profice P, Nardone R, Valeriani M, Colosimo C, Tartaglione T, Della Corte F, Pennisi MA, Tonali P (1997) Ischaemic myelopathy associated with cocaine: clinical, neurophysiological and neuroradiological features. J Neurol Neurosurg Psychiatry 63:531–533
Qureshi AI, Akbar MS, Czander E, Safdar K, Janssen RS, Frankel MR (1997) Crack cocaine use and stroke in young patients. Neurology 48:341–345
Masson C, Pruvo JP, Maeder JF, Cordonnier C, Touzé E, De La Sayette V, Giroud M, Mas JL, Leys D, Study Group on Spinal Cord Infarction of the French Neurovascular Society (2004) Spinal cord infarction. Clinical and magnetic resonance imaging findings and short term outcome. J Neurol Neurosurg Psychiatry 75:1431–1435
Kumral E, Polat F, Güllüoglu H, Uzunköprü C, Tuncel R, Alpaydin S (2011) Spinal ischemic stroke: clinical and radiological findings and short-term outcome. Eur J Neurol 18:232–239
Berg P, Kaufmann D, van Marrewijk CD, Buth J (2001) Spinal cord ischemia after stent-graft treatment for infrarenal abdominal aortic aneurysms. Analysis of the Eurostar data base. Eur J Vasc Endovasc Surg 4:342–347
Gawenda M, Zähringer M, Görg C, Südkamp M, Haupt WF, Koebke J et al (2005) The dilemma of spinal ischemia—interdisciplinary strategies for spinal cord protection during aortic surgery. Dtsch Arztebl 102:163–171
Tanaka H, Minatoya K, Matsuda H, Sasaki H, Iba Y, Oda T, Kobayashi J (2014) Embolism is emerging as a major cause of spinal cord injury after descending and thoracoabdominal aortic repair with a contemporary approach: magnetic resonance findings of spinal cord injury. Interact Cardiovasc Thorac Surg 19:205–210
Hennedige T, Chow W, Ng YY, Chung-Tsing GC, Lim TCC, Kei PL (2012) MRI in spinal cord compression sickness. J Med Imaging Radiat Oncol 56:282–288
Lipper MH, Goldstein JH, Do HM (1998) Brown–Séquard syndrome of the cervical spinal cord after chiropractic manipulation. AJNR Am J Neuroradiol 19:1349–1352
Brouwers PJ, Kottink EJ, Simon MA, Prevo RL (2001) A cervical anterior spinal artery syndrome after diagnostic blockade of the right C6-nerve root. Pain 91:397–399
Dafotakis M, Fink GR, Schlangen C, Block F, Sparing R, Thron A (2008) Acute spinal cord ischemia following deep injection therapy of the neck. Nervenarzt 79:927–931
Popescu A, Lai D, Lu A, Gardner K (2013) Stroke following epidural injections—case report and review of literature. J Neuroimaging 23:118–121
Lyders EM, Morris PP (2009) A case of spinal cord infarction following lumbar transforaminal epidural steroid injection: MR imaging and angiographic findings. AJNR Am J Neuroradiol 30:1691–1693
Weber P, Vogel T, Bitterling H, Utzschneider S, von Schulze PC, Birkenmaier C (2009) Spinal cord infarction after operative stabilisation of the thoracic spine in a patient with tuberculous spondylodiscitis and sickle cell trait. Spine 34:E294–E297
Legatt AD, Fried SJ, Amaral TD, Sarwahi V, Moguilevitch M (2014) Loss of lower limb motor evoked potentials and spinal cord injury during the initial exposure in scoliosis surgery. J Clin Neurophysiol 31:e1–e5
Kashiwazaki D, Ushikoshi S, Asano T, Kuroda S, Houkin K (2013) Long-term clinical and radiological results of endovascular internal trapping in vertebral artery dissection. Neuroradiology 55:201–206
Matsubara N, Miyachi S, Okamaoto T, Izumi T, Asai T, Yamanouchi T, Ota K, Oda K, Wakabayashi T (2013) Spinal cord infarction is an unusual complication of intracranial neurovascular intervention. Interv Neuroradiol 19:500–505
Lui H, Koyanagi I, Chiba H, Wanibuchi M, Honmou O, Yamaki T, Houkin K (2009) Spinal cord infarct as the initial clinical presentation of intravascular malignant lymphomatosis. J Clin Neurosci 6:570–573
Krishna V, Lazaridis C, Ellegala D, Glazier S, Kindy M, Spampinato M, Chalela JA (2012) Spinal cord infarction associated with subarachnoid haemorrhage. Clin Neurol Neurosurg 114:1030–1032
Sato K, Roccatagliata L, Depuydt S, Rodesch G (2012) Multiple aneurysms of the thoracic spinal cord arteries presenting with spinal infarction and subarachnoid haemorrhage: case report and literature review. Neurosurgery 71:E1053–E1058
ÓFarrell R, Thornton J, Brennan P, Brett F, Cunningham AJ (2000) Spinal cord infarction and tetraplegia: rare complications of meningococcal meningitis. Br J Anaesth 84:514–517
Kastenbauer S, Winkler F, Fesl G, Schiel X, Ostermann H, Yousry TA, Pfister HW (2001) Acute severe spinal cord dysfunction in bacterial meningitis in adults. Arch Neurol 58:806–810
Shuster A, Franchetto A (2011) Surfer’s myelopathy—an unusual cause of acute spinal ischemia: a case report and review of the literature. Emerg Radiol 18:57–60
Breslow LA, Ichord RN, Zimmerman RA, Smith SE, Licht DJ (2008) Role of diffusion MRI in diagnosis of spinal cord infarction in children. Neuropediatrics 39:188–191
Nedeltchev K, Loher TJ, Stepper F, Arnold M, Schroth G, Mattle HP, Sturzenegger M (2004) Long-term outcome of acute spinal cord ischemia syndrome. Stroke 35:560–565
Krings T, Lasjaunias PL, Hans FJ, Mull M, Nijenhuis RJ, Alvarez H, Backes WH, Reinges MH, Rodesch G, Gilsbach JM, Thron AK (2007) Imaging in spinal vascular disease. Neuroimag Clin N Am 17:57–72
Marcel C, Kremer S, Jeantroux J, Blanc F, Dietemann JL, De Sèze J (2010) Diffusion-weighted imaging in noncompressive myelopathies: a 33-patient prospective study. J Neurol 257:1438–1445
Do-Dai DD, Brooks MK, Goldkamp A, Erbay S, Bhadelia RA (2010) Magnetic resonance imaging of intramedullary spinal cord lesions: a pictorial review. Curr Probl Diagn Radiol 39:160–185
Goh C, Desmond PM, Phal PM (2014) MRI in transverse myelitis. J Magn Reson Imaging. doi:10.1002/jmri.24563
Iwasaki M, Yano S, Aoyama T, Hida K, Iwasaki Y (2011) Acute onset intramedullary spinal cord abscess with spinal artery occlusion: a case report and review. Eur Spine J 20(2):S294–S301
Krings T (2010) Vascular malformations of the spine and spinal cord. Clin Neuroradiol 20:5–24
Thron A, Mull M, Gilsbach J (2003) Arteriovenous fistula of the spinal dura—a rare albeit treatable cause of paraplegia. Dtsch Arztebl 100:949–953
Mull M, Nijenhuis RJ, Backes WH, Krings T, Wilmink JT, Thron A (2007) Value and limitations of contrast-enhanced MR angiography in spinal arteriovenous malformations and dural arteriovenous fistulas. AJNR Am J Neuroradiol 28:1249–1258
Schmalstieg WF, Weinshenker BG (2010) Approach to acute or subacute myelopathy. Neurology 75(1):S2–S8
West TW, Hess C, Cree BA (2012) Acute transverse myelitis: demyelinating, inflammatory, and infectious myelopathies. Semin Neurol 32:97–113
Transverse Myelitis Consortium Working Group (2002) Proposed diagnostic criteria and nosology of acute transverse myelitis. Neurology 59:499–505
Nichtweiß M, Hattingen E, Weidauer S (2015) Diseases of the spinal cord—novel imaging, diagnosis and treatment. In: Hattingen E, Weidauer S, Setzer M, Klein J, Vrionis K (eds) Inflammation of the spinal cord. Springer, Heidelberg, pp 315–368
Kimura A, Tan CF, Wakida K, Saio M, Hozumi I, Inuzuka T, Takahashi H (2007) Venous congestive myelopathy of the cervical spinal cord: an autopsy case showing a rapidly progressive clinical course. Neuropathology 27:284–289
Pillai SK, Subramaniam T, Rao GG (2011) Spinal stroke in older people secondary to dural arteriovenous fistula. BMJ Case Rep. doi:10.1136/brc.06.2011.4373
Atkinson JL, Miller GM, Krauss WE, Marsh WR, Piepgras DG, Atkinson PP, Brown RD Jr, Lane JL (2001) Clinical and radiographic features of dural arteriovenous fistula, a treatable cause of myelopathy. Mayo Clin Proc 76:1120–1130
Weidauer S, Dettmann E, Krakow K, Lanfermann H (2002) Diffusion-weighted MRI of spinal cord infarction—description of two cases and review of the literature. Nervenarzt 73:999–1003
Lanfermann H, Pilatus U, Weidauer S (2004) Diffusion-weighted MRI of the spinal cord in spinal stroke. Riv Neuroradiol 17:309–313
Weidauer S, Nichtweiß M, Berkefeld J (2015) Diseases of the spinal cord—novel imaging, diagnosis and treatment. In: Hattingen E, Weidauer S, Setzer M, Klein J, Vrionis K (eds) Spinal cord infarction. Springer, Heidelberg, pp 435–452
Mercier P, Brassier G, Fournier D, Hentati N, Pasco-Papon A, Papon X (1997) Predictability of the cervical origin of the anterior spinal artery. Interv Neuroradiol 20:283–288
Kaneki M, Inoue K, Shimizu T, Mannen T (1994) Infarction of the unilateral posterior horn and lateral column of the spinal cord with sparing of posterior columns: demonstration by MRI. J Neurol Neurosurg Psychiatry 57:629–631
Berg D, Mullges W, Klotzenburg M, Bendszus M, Reiners K (1998) Man-in-the-barrel syndrome caused by cervical spinal cord infarction. Acta Neurol Scand 97:417–419
Stapf C, Mohr JP, Straschill M, Mast H, Marx P (2000) Acute bilateral arm paresis. Cerebrovasc Dis 10:239–243
Pullicino P (1994) Bilateral upper limb amyotrophy and watershed infarcts from vertebral artery dissection. Stroke 25:1870–1872
Caplan LR, Zarins ZK, Hemmati M (1985) Spontaneous dissection of the extracranial vertebral arteries. Stroke 16:1030–1038
Murata K, Ikeda K, Muto M, Hirajama T, Kano O, Iwasaki Y (2012) A case of posterior spinal artery syndrome in the cervical cord: a review of the clinicoradiological literature. Intern Med 51:803–807
Gelfan S, Tarlov IM (1955) Differential vulnerability of spinal cord structures to anoxia. J Neurophysiol 18:170–188
Hundsberger T, Thömke F, Hopf HC, Fitzek C (1998) Symmetrical infarction of the cervical spinal cord due to spontaneous bilateral vertebral artery dissection. Stroke 29:1742
Robertson CE, Brown RD Jr, Wijdicks EFM, Rabinstein AA (2012) Recovery after spinal cord infarcts. Neurology 78:114–121
Lebouteux MV, Franques J, Guillevin R, Delmont E, Lenglet T, Bede P, Desnuelle C, Pouget J, Pascal-Mousselard H, Pradat PF (2014) Revisiting the spectrum of lower motor neuron diseases with snake eyes appearance on magnetic resonance imaging. Eur J Neurol 21:1233–1241
Salvador de la Barrera S, Barca-Buyo A, Montoto-Marqués A, Ferreiro-Velasco E, Cidoncha-Dans M, Rodriguez-Sotillo A (2001) Spinal cord infarction: prognosis and recovery in a series of 36 patients. Spinal Cord 39:520–525
Thurnher MM, Cartes-Zumelzu F, Mueller-Mang C (2007) Demyelinating and infectious diseases of the spinal cord. Neuroimag Clin N Am 17:37–55
Urban P, Gawehn J, Ringel K (2005) “Man-in-the-barrel” syndrome. Clin Neuroradiol 15:190–194
Kim MJ, Jang MH, Choi MS, Kang SY, Kim JY, Kwon KH, Kang IW, Cho SJ (2014) Atypical anterior spinal artery infarction due to left vertebral artery occlusion presenting with bilateral hand weakness. J Clin Neurol 10:171–173
Desai JA, Melanson M (2011) Teaching neuroimages: anterior horn cell hyperintensity in Hirayama disease. Neurology 77:e73
Hirayama K (2000) Juvenile muscular atrophy of the upper extremity (Hirayama disease). Intern Med 39:283–290
Jellinger KA (1997) Spinal cord watershed. Neurology 48:1474
Gailloud P, Gregg L, Galan P, Becker D, Prado C (2014) Periconal arterial anastomotic circle and posterior lumbosacral watershed zone of the spinal cord. J Neurointervent Surg. doi:10.1136/neurintsurg-2014-011408
Wildgruber D, Kuntz R, Kermer P, BArtel J, Fetter M, Dichgans J (1999) Elsberg syndrome due to infarction of the conus medullaris associated with a prothrombin mutation. J Neurol 246:507–508
Bammer R, Fazekas F, Augustin M, Simbrunner J, Strasser-Fuchs S, Seifert T, Stollberger R, Hartung HP (2000) Diffusion weighted MR imaging of the spinal cord. Am J Neuroradiol 21:587–591
Nogueira RG, Ferreira R, Grant E, Maier SE, Koroshetz WJ, Gonzales RG, Sheth KN (2012) Restricted diffusion in spinal cord infarction demonstrated by magnetic resonance line scan diffusion imaging. Stroke 43:532–535
Tanenbaum LN (2013) Clinical applications of diffusion imaging in the spine. Magn Reson Imaging Clin N Am 21:299–320
Thurnher MM, Law M (2009) Diffusion-weighted imaging, diffusion-tensor imaging, and fiber tractography of the spinal cord. Magn Reson Imaging Clin N Am 17:225–244
Andre JB, Zaharchuk G, Saritas E, Komakula S, Shankaranarayan A, Banerjee S, Rosenberg J, Nishimura DG, Fischbein NJ (2012) Clinical evaluation of reduced field-of-view diffusion-weighted imaging of the cervical and thoracic spine and spinal cord. AJNR Am J Neuroradiol 33:1860–1866
Yuh W, Marsh EE, Wang AK, Russel JW, Chiang F, Koci TM, Ryals TJ (1992) MR imaging of spinal cord and vertebral body infarction. AJNR Am J Neuroradiol 13:145–154
Alblas CL, Bouvy WH, Lycklama À Nijeholt GJ, Boiten J (2012) Acute spinal-cord ischemia: evolution of MRI findings. J Clin Neurol 8:218–223
Holland NR (2013) Acute myelopathy with normal imaging. J Child Neurol 28:648–650
Amano Y, Machida T, Kumazaki T (1998) Spinal cord infarcts with contrast enhancement of the cauda equina: two cases. Neuroradiology 40:669–672
Kastenbauer S, Brüning R, Pfister HW (2005) Gadolinium enhancement of the cauda equine following ischemia of the lumbar cord. Nervenarzt 76:479–481
Diehn FE, Hunt CH, Lehman VT, Schwartz KM, Eckel LJ, Black DF, Wood CP, Kotsenas AL, Wald JT, Hocker SE (2013) Vertebral body infarct and ventral cauda equine enhancement: two confirmatory findings of acute spinal cord infarct. J Neuroimaging. doi:10.1111/jon.12058
Pravatà E, Cereda C, Gabutti A, Distefano D, Cianfoni A (2014) Late-onset cauda equina contrast enhancement: a rare magnetic resonance imaging finding in subacute spinal cord infarction. Spine J. doi:10.1016/j.spinee.2014.08003
Kobayashi M, Kanai T (2013) Vertebral body infarction revealed by diffusion-weighted magnetic resonance imaging. J Neurol 260:1160–1162
Cheng MY, Lyu RK, Chang YJ, Chen CM, Chen ST, Wai YY, Ro LS (2009) Concomitant spinal cord and vertebral body infarction is highly associated with aortic pathology: a clinical and magnetic resonance imaging study. J Neurol 256:1418–1426
Collongues N, Marignier R, Zéphir H, Papeix C, Blanc F, Ritleng C et al (2010) Neuromyelitis optica in France. A multicenter study of 125 patients. Neurology 74:736–742
de Seze J, Stojkovic T, Breteau G, Lucas C, Michon-Pasturel U, Gauvrit JY, Hachulla E, Mounier-Vehier F, Pruvo JP, Leys D, Destée A, Hatron PY, Vermersch P (2001) Acute myelopathies. Clinical, laboratory and outcome profiles in 79 cases. Brain 124:1509–1521
Scott TF (2007) Nosology of idiopathic transverse myelitis syndromes. Acta Neurol Scand 115:371–376
Montalban X, Tintoré M, Swanton J, Barkhof F, Fazekas F, Fillipi M, Frederiksen J, Kappos L, Palace J, Polman C, Rovaris M, de Stefano N, Thompson A, Yousry T, Rovira A, Miller DH (2010) MRI criteria for MS in patients with clinically isolated syndromes. Neurology 74:427–434
Polman CH, Reingold SC, Banwell B, Clanet M, Cohen JA, Filippi M, Fujihara K, Havrdova E, Hutchinson M, Kappos L, Lublin FD, Montalban X, O’Connor P, Sandberg-Wollheim M, Thompson AJ, Waubant E, Weinshenker B, Wolinsky JS (2011) Diagnostic criteria for multiple sclerosis: 2010 revisions to the McDonald criteria. Ann Neurol 69:292–302
Oppenheimer DR (1978) The cervical cord in multiple sclerosis. Neuropath Appl Neurob 4:151–162
Thurnher MM, Bammer R (2006) Diffusion-weighted MR imaging (DWI) in spinal cord ischemia. Neuroradiology 48:795–801
Gailloud P, Ponti A, Gregg L, Pardo CA, Fasel HJ (2014) Focal compression of the upper left thoracic intersegmental arteries as a potential cause of spinal cord ischemia. AJNR Am J Neuroradiol 35:1226–1231
Reynolds JM, Belvadi YS, Kane AG, Poulopoulos M (2014) Thoracic disc herniation leads to anterior spinal artery syndrome demonstrated by diffusion-weighted magnetic resonance imaging (DWI): a case report and literature review. Spine J 14:e17–e22
Martínez-Lage JF, Almagro MJ, Izura V, Serrano C, Ruiz-Espejo AM, Sánchez-del-Rincón I (2009) Cervical spinal cord infarction after posterior fossa surgery: a case-based update. Childs Nerv Syst 25:1541–1546
Tong CKW, Chen JCH, Cochrane DD (2012) Spinal cord infarction remote from maximal compression in a patient with Morquio syndrome. J Neurosurg Pediatr 9:608–612
Solanki GA, Martin KW, Theroux MC, Lampe C, White KK, Shediac R, Lampe CG, Beck M, Mackenzie WG, Hendriksz CJ, Harmatz PR (2013) Spinal involvement in mucopolysaccharidosis IVA (Morquio-Brailsford or Morquiou A syndrome): presentation, diagnosis and management. J Inherit Metab Dis 36:339–355
Fernandez-Torron R, Palma JA, Riverol M, Irimia P, Martinez-Vila E (2012) Brown-Séquard syndrome after endovascular embolization of vertebral hemangioma. Spinal Cord 50:636–637
Ethical standards and patient consent
We declare that due to the retrospective nature of this study, we did not apply for Ethics Committee approval.
Conflict of interest
We declare that we have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Weidauer, S., Nichtweiß, M., Hattingen, E. et al. Spinal cord ischemia: aetiology, clinical syndromes and imaging features. Neuroradiology 57, 241–257 (2015). https://doi.org/10.1007/s00234-014-1464-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-014-1464-6