Abstract
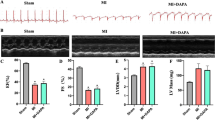
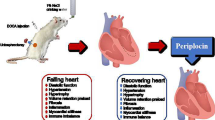
The objective of this study is to examine the effect of empagliflozin on cardiac function in rats with chronic heart failure and the possible mechanism. Forty 6-week-old male SD rats were randomly divided into the control group, empagliflozin treatment group, and sham-operated group. SD rats in the control group and empagliflozin treatment group were subjected to ligation of the anterior descending coronary artery to induce an acute myocardial infarction model. SD rats in the sham-operated group were only subjected to threading of the anterior descending branch of the coronary artery without ligation. On the second day after surgery, the control group and sham operation group were given physiological saline by gavage, while the empagliflozin treatment group was given empagliflozin (30 mg/kg/day) by gavage. Sixteen weeks later, cardiac function, intracellular reactive oxygen species (ROS) levels, mitochondrial membrane potential (MMP), serum brain natriuretic peptide, hypersensitive C-reactive protein (hs-CRP), iNOS expression levels, and myocardial morphological changes were observed. Compared with that in the control group, heart function in the empagliflozin-treated group was significantly improved, MMP was increased, intracellular ROS levels were decreased, and NT-proBNP and hs-CRP were significantly reduced, and HE staining showed that the cell oedema was less than that in the control group, tissue arrangement was more orderly, and iNOS expression was inhibited. Empagliflozin can improve cardiac function in rats with chronic heart failure, and the mechanism may involve inhibiting inflammation, reducing myocardial oxidative stress, and improving myocardial fibrosis.



Similar content being viewed by others
Data availability
All source data for this study are available upon reasonable request from the authors.
References
Böhm M, Anker SD, Butler J et al (2021) Empagliflozin improves cardiovascular and renal outcomes in heart failure irrespective of systolic blood pressure. J Am Coll Cardiol 78:1337–1348. https://doi.org/10.1016/j.jacc.2021.07.049
Böhm M, Butler J, Filippatos G et al (2022) Empagliflozin improves outcomes in patients with heart failure and preserved ejection fraction irrespective of age. J Am Coll Cardiol 80:1–18. https://doi.org/10.1016/j.jacc.2022.04.040
Bonner C, Kerr-Conte J, Gmyr V et al (2015) Inhibition of the glucose transporter SGLT2 with dapagliflozin in pancreatic alpha cells triggers glucagon secretion. Nat Med 21:512–7. https://doi.org/10.1038/nm.3828
Briasoulis A, Androulakis E, Christophides T et al (2016) The role of inflmmation and cell death in the pathogenesis, progression and treatment of heart failure. Heart Fail Rev 21:169–176. https://doi.org/10.1007/s10741-016-9533-z
Canton M, Neverova I, Menabo R et al (2004) Evidence of myofibrillar protein oxidation induced by postischemic reperfusion in isolated rat hearts. Am J Physiol Heart Circ Physiol 286:H870–H877. https://doi.org/10.1152/ajpheart.00714.2003
Ferrannini E, Muscelli E, Frascerra S et al (2014) Metabolic response to sodium-glucose cotransporter 2 inhibition in type 2 diabetic patients. J Clin Invest 124:499–508. https://doi.org/10.1172/JCI72227
Giordano FJ (2005) Oxygen, oxidative stress, hypoxia, and heart failure. J Clin Invest 115:500–508. https://doi.org/10.1172/JCI24408
Habal MV, Liu PP, Austin PC et al (2014) Association of heart rate at hospital discharge with mortality and hospitalizations in patients with heart failure. Circ Heart Fail 7:12–20. https://doi.org/10.1161/CIRCHEARTFAILURE.113.000429
Halliwell B (2006) Reactive species and antioxidants. Redox biology is a fundamental theme of aerobic life. Plant Physiol 141:312–322. https://doi.org/10.1104/pp.106.077073
Hao G, Wang X, Chen Z et al (2019) Prevalence of heart failure and left ventricular dysfunction in China: the China Hypertension Survey, 2012–2015. Eur J Heart Fail 21:1329–1337. https://doi.org/10.1002/ejhf.1629
Hu ST, Gao RL, Liu LS et al (2019) Summary of the 2018 report on cardiovascular diseases in China. Chin Circ J 34:209–220
Kalluri SR, Bhutta TH, Hannoodee H et al (2021) Do SGLT2 inhibitors improve cardio-renal outcomes in patients with type II diabetes mellitus: a systematic review. Cureus 13:e17668. https://doi.org/10.7759/cureus.17668
Kataoka H (2019) Biochemical determinants of changes in plasma volume after decongestion therapy for worsening heart failure. J Card Fail 25:213–217. https://doi.org/10.1016/j.cardfail.2018.09.014
Kwon SH, Pimentel DR, Remondino A et al (2003) H2O2 regulates cardiac myocyte phenotype via concentration-dependent activation of distinct kinase pathways. J Mol Cell Cardiol 35:615–621. https://doi.org/10.1016/s0022-2828(03)00084-1
Lee TM, Chang NC, Lin SZ (2017) Dapagliflozin, a selective SGLT2 inhibitor, attenuated cardiac fibrosis by regulating the macrophage polarization via STAT3 signaling in infarcted rat hearts. Free Radic Biol Med 104:298–310. https://doi.org/10.1016/j.freeradbiomed.2017.01.035
Li WW, Olshansky B (2011) Inflammatory cytokines and nitric oxide in heart failure and potential modulation by vagus nerve stimulation. Heart Fail Rev 16:137–45. https://doi.org/10.1007/s10741-010-9184-4
Mende CW (2022) Chronic kidney disease and SGLT2 inhibitors: a review of the evolving treatment landscape. Adv Ther 39:148–164. https://doi.org/10.1007/s12325-021-01994-2
Murphy SP, Ibrahim NE, Januzzi JL Jr (2020) Heart failure with reduced ejection fraction: a review. JAMA 324:488–504. https://doi.org/10.1001/jama.2020.10262
Ohara K, Masuda T, Murakami T et al (2019) Effects of the sodium-glucose cotransporter 2 inhibitor dapagliflflozin on flfluid distribution: a comparison study with furosemide and tolvaptan. Nephrology (Carlton) 24:904–911. https://doi.org/10.1111/nep.13552
Packer M, Anker SD, Butler J et al (2020) Cardiovascular and renal outcomes with empagliflozin in heart failure. N Engl J Med 383:1413–1424. https://doi.org/10.1056/NEJMoa2022190
Palmieri V, Innocenti F, Guzzo A et al (2015) Left ventricular systolic longitudinal function as predictor of outcome in patients with sepsis. Circ Cardiovasc Imaging 8:e003865. https://doi.org/10.1161/CIRCIMAGING.115.003865
Perry RJ, Rabin-Court A, Song JD et al (2019) Dehydration and insulinopenia are necessary and sufficient for euglycemic ketoacidosis in SGLT2 inhibitor-treated rats. Nat Commun 10(1):548. https://doi.org/10.1038/s41467-019-08466-w
Ridker PM, Everett BM, Thuren T et al (2017) Antiinflammatory therapy with canakinumab for atherosclerotic disease. N Engl J Med 377:1119–1131. https://doi.org/10.1056/NEJMoa1707914
Sabri A, ByronK L, Samarel AM et al (1998) Hydrogen peroxide activates mitogen-activated protein kinases and Na+-H+ exchange in neonatal rat cardiac myocytes. Circ Res 82:1053–1062. https://doi.org/10.1161/01.res.82.10.1053
Simpson J, Jhund PS, Lund LH et al (2020) Prognostic models derived in PARADIGM-HF and validated in AT-MOSPHERE and the Swedish Heart Failure Registry to predict mortality and morbidity in chronic heart failure. JAMA Cardiol 5:432–441. https://doi.org/10.1001/jamacardio.2019.5850
Tanajak P, Sa-Nguanmoo P, Sivasinprasasn S et al (2018) Cardioprotection of dapagliflozin and vildagliptin in rats with cardiac ischemia-reperfusion injury. J Endocrinol 236:69–84. https://doi.org/10.1530/JOE-17-0457
Tang H, Li D, Wang TS et al (2016) Effect of sodium-glucose cotransporter 2 inhibitors on diabetic ketoacidosis among patients with type 2 diabetes: a meta-analysis of randomized controlled trials. Diabetes Care 39(8):e123–124. https://doi.org/10.2337/dc16-0885
Testani JM, Chen J, McCauley BD et al (2010) Kimmel SE, Shannon RP. Potential effects of aggressive decongestion during the treatment of decompensated heart failure on renal function and survival. Circulation 122:265–272. https://doi.org/10.1161/CIRCULATIONAHA.109.933275
Uchmanowicz I, Lee CS, Vitale C et al (2020) Frailty and the risk of all-cause mortality and hospitalization in chronic heart failure:a meta-analysis. ESC Heart Fail 7:3427–3437. https://doi.org/10.1002/ehf2.12827
Umar S, van der Laarse A (2010) Nitric oxide and nitric oxide synthase isoforms in the normal, hypertrophic, and failing heart. Mol Cell Biochem 333:191–201. https://doi.org/10.1007/s11010-009-0219-x
Wilhelmi MH, Leyh RG, Wilhelmi M et al (2005) Upregulation of endothelial adhesion molecules in hearts with congestive and ischemic cardiomyopathy: immunohistochemical evaluation of inflammatory endothelial cell activation. Eur J Cardiothorac Surg 27:122–127. https://doi.org/10.1016/j.ejcts.2004.09.027
Wu HQ, Zhu Q, Cai M et al (2014) Effect of inhibiting malonyl-CoA decarboxylase on cardiac remodeling after myocardial infarction in rats. Cardiology 127:236–244. https://doi.org/10.1159/000356471
Wu Y, Yao YM, Lu ZQ (2019) Mitochondrial quality control mechanisms as potential therapeutic targets in sepsis-induced multiple organ failure. J Mol Med (Berl) 97:451–462. https://doi.org/10.1007/s00109-019-01756-2
Yokono M, Takasu T, Hayashizaki Y et al (2014) SGLT2 selective inhibitor ipragliflozin reduces body fat mass by increasing fatty acid oxidation in high-fat diet-induced obese rats. Eur J Pharmacol 727:66–74. https://doi.org/10.1016/j.ejphar.2014.01.040
Zannad F, Ferreira JP, Pocock SJ et al (2020) SGLT2 inhibitors in patients with heart failure with reduced ejection fraction: a meta-analysis of the EMPEROR-Reduced and DAPA-HF trials. Lancet 396:819–829. https://doi.org/10.1016/S0140-6736(20)31824-9
Funding
This work was supported by Shandong Province Medical and Health Technology Development Plan Project.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by Zhenzhen Wang, QianLiu, Xiaofang Wang, Pengpeng Wang, Fenglei Zhang, and Zhuwen Wang. The first draft of the manuscript was written by Zhenzhen Wang and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript. The authors declare that all data were generated in-house and that no paper mill was used.
Corresponding author
Ethics declarations
Ethical approval
The animal experiment was carried out in strict accordance with the “Regulations on the Management of Experimental Animals” issued by the State Council of the People’s Republic of China. This experiment was approved by the Experimental Animal Ethics Committee of the Second Affiliated Hospital of Chongqing Medical University.
Informed consent
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, Z., Liu, Q., Wang, X. et al. Empagliflozin improves cardiac function in rats with chronic heart failure. Naunyn-Schmiedeberg's Arch Pharmacol 397, 1037–1044 (2024). https://doi.org/10.1007/s00210-023-02655-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-023-02655-7