Abstract
This article provides an overview of the background knowledge of ferroptosis in the nervous system, as well as the key role of nuclear factor E2-related factor 2 (Nrf2) in regulating ferroptosis. The article takes Alzheimer's disease (AD), Parkinson's disease (PD), Huntington's disease (HD), and amyotrophic lateral sclerosis (ALS) as the starting point to explore the close association between Nrf2 and ferroptosis, which is of clear and significant importance for understanding the mechanism of neurodegenerative diseases (NDs) based on oxidative stress (OS). Accumulating evidence links ferroptosis to the pathogenesis of NDs. As the disease progresses, damage to the antioxidant system, excessive OS, and altered Nrf2 expression levels, especially the inhibition of ferroptosis by lipid peroxidation inhibitors and adaptive enhancement of Nrf2 signaling, demonstrate the potential clinical significance of Nrf2 in detecting and identifying ferroptosis, as well as targeted therapy for neuronal loss and mitochondrial dysfunction. These findings provide new insights and possibilities for the treatment and prevention of NDs.
Similar content being viewed by others
Introduction
Alzheimer's disease, Parkinson's disease, Huntington's disease, and amyotrophic lateral sclerosis are typical neurodegenerative diseases (NDs) (Maragakis and Rothstein 2006) that can be identified by the gradually implemented death of specifically vulnerable neurons (Abdalkader et al. 2018). Today, the global prevalence of Alzheimer's disease (AD) stands at over 50 million individuals, with projections indicating that this number will surpass 100 million by the mid-century (Jannat et al. 2019). Elderly people are more likely to develop common NDs like Alzheimer's ( AD) and Parkinson's disease, or PD, and their risk increases with age (Hou et al. 2019). Among the many risk factors for neurodegeneration, the impact of aging cannot be ignored (Wyss-Coray 2016; Dugger and Dickson 2017). With the aging of the world's population, age-related NDs have become one of the biggest problems to be solved urgently in modern society (Angelova et al. 2021). To improve patient quality of life, increase life expectancy, and lessen the burden on society, it is crucial to understand the pathogenesis of NDs and identify effective therapeutic targets. At the same time, a considerable number of studies have shown an association between the onset and progression of NDs and ferroptosis (Gallucci et al. 2008; Wu et al. 2021; Zhang et al. 2023) (Fig. 1).
Characterization of ferroptosis in neurodegenerative diseases (NDs) pathological conditions. There exists a significant correlation between ferroptosis and NDs. Ferroptosis contributes to the advancement of NDs, whereas the expression of Nrf2 and its transcriptionally regulated peptides (GSH, GPX4) decreases with aging. In contrast to the impairment of the antioxidant system, heightened levels of reactive oxygen species (ROS) and increased lipid peroxidation, combined with brain iron deposition, induce ferroptosis. Ferroptosis results in alterations in mitochondrial morphology, neuronal damage and eventual cell death. Drawing by Inkscape
As originally suggested by Dixon's groups in the year 2012 ferroptosis is now recognized as an iron-dependent type of lipid peroxidation-induced programmed cell death (Dixon et al. 2012). The morphological changes and biochemical processes that differentiate ferroptosis from other forms of programmed cell death are indicative of the unique characteristics of this process (Lee et al. 2020). Morphologically, it is characterized by ferroptosis-like nanopores in cell membrane, mitochondrial shrinkage, mitochondrial exterior membrane rupture and elevated membrane of the mitochondria density (Dixon et al. 2012; Stockwell 2022), mitochondrial ridge reduction or loss, and no significant changes in nucleus (Demuynck et al. 2021; Dong et al. 2022). In biochemical terms, iron excess, lipid peroxidation, increased ROS, and impaired antioxidant enzyme activity are the hallmarks of ferroptosis (Jiang et al. 2021). Lipid peroxidation is the procedure that happens when specific phospholipids in cell and organelle membranes attach to reactive chemicals such as reactive oxygen species, or ROS for short, and reactive nitrogen species (RNS) [mainly from the combination of polyunsaturated fatty acids with phospholipids, especially arachidonic acid and epinephric acid (AA), which can bind to phosphatidylethanolamines (PE)] to generate lipid peroxides (LOOH) (Dodson et al. 2019a). The increase of free iron leads to Fenton reaction (Fe2+ + H2O2 → Fe3+ + ·OH + OH−), resulting in ROS accumulation and non-enzymatic lipid peroxidation, which leads to the imbalance of antioxidant system and membrane integrity defect, and finally leads to ferroptosis (Forcina and Dixon 2019) (Fig. 1).
Among them, the main antioxidant systems currently involved include: the Xc−–glutathione–glutathione peroxidase 4 axis (Xc−–GSH–GPX4) (Yang et al. 2014), coenzyme Q10–ferroptosis suppressor protein1 (CoQ10–FSP1) (Doll et al. 2019), dihydroorotate dehydrogenase–ubiquinol (DOHDH–CoQ10H2) (Mao et al. 2021) and GTP cyclohydrolase1–tetrahydrobiopterin (GCH1–BH4) axis (Kraft et al. 2020). Significantly, Nrf2 regulates the transcription of the anti-ferroptosis system, encompassing crucial signaling molecules involved in these pathways. Thus, it is thought that Nrf2 is a crucial regulator of ferroptosis and peroxidation of lipids (Dodson et al. 2019a). In the following article, we emphasize how ferroptosis and the control of Nrf2 signaling are related, with its associated iron metabolism and lipid peroxidation. Based on the research on the mechanism of ferroptosis in NDs, discuss the feasible strategies and related biomarkers of Nrf2 regulatory pathway in the diagnosis and treatment of ferroptosis-driven neurodegeneration.
Iron metabolism
Iron is the most prevalent transition metal on the earth (Coby et al. 2011) and the most abundant essential metal in the organism (Wang et al. 2022b), which defines an important role in a variety of physiological processes and even in the origin of life. As a transition metal, iron has efficient electron transfer properties, thus participating in the synthesis of heme and assisting in catalyzing various biochemical reactions (Crielaard et al. 2017). According to related research, metabolic reactions involving iron or iron–sulfur clusters may have played a key role in the development of life (Bonfio et al. 2017; Varma et al. 2018). In the body, nearly half of the iron constitutes the active center of hemoglobin, thus participating in oxygen transport (Andreini et al. 2018). About 20% of the total oxygen is consumed by the relatively small brain separated by the blood–brain barrier (BBB) (Angelova et al. 2021). Furthermore, the development of synapses, myelination, and the synthesis and turnover of neurotransmitters all depend on iron-dependent protein and enzyme activity in the nervous system (Carpenter et al. 2016). Iron homeostasis profoundly affects brain development and health (Masaldan et al. 2019). The effect of iron deficiency on brain functions such as intelligence and cognition is particularly significant in the early stages of development, even when the condition is corrected (Beard and Connor 2003).
At the same time, the presence of the BBB, which separates the brain from the peripheral iron homeostatic storage, in turn influences the import of iron into the brain (Masaldan et al. 2019). Brain capillary endothelial cells (BCECs) are a major component of the BBB (Masaldan et al. 2019) (Fig. 3a), and the transferrin receptor 1 (TfR1) expressed on them is responsible for the transfer of iron into the brain (Pardridge et al. 1987; Connor et al. 2011). In vivo, free iron usually has two states: ferric (Fe3+) and ferrous (Fe2+) irons (Pan et al. 2021). Fe3+ forms a complex (holo-Tf) with transferrin (Tf) after entering the blood circulation, and binds to TfR1 on the surface of brain microvascular endothelial cells (BMECs), and then the Fe3+-containing Tf–TfR1 complex enters the BME through clathrin-mediated endocytosis (Pardridge et al. 1987; Taylor et al. 1991; McCarthy and Kosman 2012) (Table 1).
The transport mechanism of iron across BCEC is still inconclusive, but there are two possible scenarios (Masaldan et al. 2019). Classical models hold that Fe3+ released from Tf in an acidic environment created by endosomal proton pumps is reduced to Fe2+ by six transmembrane epithelial antigen-prostate 3 (STEAP3) (Ohgami et al. 2005) or duodenal cytochrome b (DCYTB) (Tulpule et al. 2009), then transported to the cytoplasm by divalent metal transporter 1 (DMT1) (De Domenico et al. 2008), while apotransferrin (apo-Tf; i.e., iron-free transferrin) and TfR1 are recovered by the cell membrane for recycling (Zheng et al. 2018; Chen et al. 2019). In this case, one of the multiple destinations of Fe2+ in BMECs is to be transported out of the cell via the secretion of ferroportin 1 (FPN1) to the brain, where it is subsequently oxidized to Fe3+ by copper cyanine (Cp) or heparin (McCarthy and Kosman 2013; Burkhart et al. 2016) (Fig. 3d). The classical model could not explain the finding of DMT1 deficiency on BMECs, so another model of transcytosis was proposed (Moos et al. 2006; Burkhart et al. 2016). In this model, holo-TF, a complex of Fe3+ with Tf, is directly transported through vesicles to abluminal site, thus released into the brain (Raub and Newton 1991; Moos et al. 2007) (Fig. 3b). The fact that in vitro nurtured bovine BCECs cycle Tf-TfR1 complexes may not result in intraendothelial breakdown in transcytosis is one argument in favor of the transcytosis paradigm (Raub and Newton 1991; Descamps et al. 1996). Yet, no additional in vivo studies support the belief that circulating Tf translocates through BCECs and enters the brain (Crowe and Morgan 1992; Strahan et al. 1992; Moos et al. 2006). In the classical model, Fe2+ is involved in a variety of biochemical processes within the BCEC, including efflux. There are two storage forms of iron in the cell: stable ferritin and active unbound iron, namely the unstable iron pool (LIP) (Ru et al. 2023). Excess reactive Fe2+ as LIP can cause ROS accumulation through Fenton reaction (Yan et al. 2021b). Finally, neurons, microglia, and astrocytes can utilize the same iron metabolism-related proteins to absorb iron across the BBB (Simpson et al. 2015; McCarthy and Kosman 2015; Bu et al. 2019; Yan and Zhang 2019) (Fig. 3d).
Astrocytes are primarily responsible for releasing iron into neurons while attenuating iron toxicity (Abbott et al. 2006; Burkhart et al. 2016). Cp is required for iron export from astrocytes (Klomp et al. 1996; Jeong and David 2006), whereas the processes associated with their iron import are unknown, and the expression level of TfR1 in these cell varies in different studies (Pelizzoni et al. 2013; Wong et al. 2014a; Zarruk et al. 2015; Belaidi and Bush 2016). DMT1 may have a facilitative effect on the transfer of iron into astrocytes (Moos and Morgan 2003; Huang et al. 2004, 2006; Lane et al. 2010; Pelizzoni et al. 2013). The concentration of iron in glial cells is higher than that in neurons, and the maintenance of iron homeostasis in the central nervous system mainly depends on astrocytes (Dusek et al. 2022), which accumulate iron and iron-containing compounds and store them efficiently in ferritin export iron (Hohnholt and Dringen 2013; Codazzi et al. 2015; Morris et al. 2018). Studies have also shown that astrocytes in the mouse brain can activate Nrf2 to resist cytotoxicity caused by iron overload (Cui et al. 2016). The neuroprotective effect mediated by Nrf2 has also been observed in various experimental models of neurodegeneration (Cuadrado et al. 2018; Yu et al. 2019) In addition, solute carrier family 39 member 14 (SLC39A14) can also transport Fe2+ intracellularly (Yu et al. 2020), and its expression is increased in astrocytes in response to inflammation and iron overload (Routhe et al. 2020) (Fig. 3d).
Iron plays an important role in the synthesis of myelin by oligodendrocytes (Benkovic and Connor 1993; Todorich et al. 2011; Belaidi and Bush 2016), and iron deficiency can cause myelination and other related diseases (Todorich et al. 2009). Oligodendrocytes may derive their iron from ferritin (Connor et al. 1995; Sanyal et al. 1996; Qi et al. 2002; Zhang et al. 2006; Todorich et al. 2011) and may take up iron primarily through endocytosis of ferritin (Masaldan et al. 2019). Age is correlated with the amount of iron in oligodendrocytes (Benkovic and Connor 1993). Also, Tf and FPN may, respectively, mediate the intracellular transit of iron and its efflux from oligodendrocytes (Moos et al. 2007).
Microglia are formed by the differentiation of circulating monocytes after they migrate to the brain (Milligan et al. 1991). During this process, iron and ferritin are released (Moos 1995; Cheepsunthorn et al. 1998) and may provide iron to oligodendrocytes (Todorich et al. 2011).
Like BMECs, iron is capable of reaching neurons by internalizing the Tf–TfR1 complex, where it is then reduced and delivered into the cytosol by DMT1 (Burdo et al. 2001). Interestingly, cellular prion protein (PrPc), which, like TfR1, has extensive expression on the outer layers of neurons forms a complex with DMT1 (Giometto et al. 1990), where DMT1 transports non-transferrin-bound iron (NTBI) into neurons and PrPc reduces Fe3+ to Fe2+ (Singh 2014; Tripathi et al. 2015). Similarly, excess iron efflux in neurons is mediated by FPN1, while Cp and hephaestin (Heph) promote the efflux of FPN and the oxidation of Fe2+ (Qian et al. 2007). Additionally, amyloid precursor protein (APP) and tau are key proteins involved in iron efflux in neurons (McCarthy et al. 2014; Belaidi et al. 2018). With the contribution of soluble tau, APP is transported to the cell membrane to stabilize FPN1 and promote iron export (Lei et al. 2012; Wong et al. 2014b) (Fig. 3d).
The antioxidant system
In the face of oxidative damage caused by iron overload, intracellular antioxidant systems prevent cell death due to lipid peroxidation. Interestingly, ferroptosis, a novel cell death phenotype initially induced by Ras and ST eradicator (erastin) and Ras selective lethal 3 (RSL3) (Dixon et al. 2012), results from disruption of intracellular redox homeostasis precisely through depletion of GSH.
GSH–GPX4 axis
Among them, the target of elastin, System Xc− cystine/glutamate antiporter is inhibited by it to induce ferroptosis (Dixon et al. 2012, 2014). System Xc− is a heterodimeric amino acid transport complex consisting of a heavy-chain 4F2hc protein (i.e., recombinant solute carrier family 3 member 2, SLC3A2) and a light-chain xCT protein (recombinant solute carrier family 7 member 11, SLC7A11) (Sato et al. 1999; Liu et al. 2021) (Table 1). SLC7A11 is a transport protein and a functional component of System Xc−, and its 12 putative transmembrane domains ensure the specificity of System Xc−. SLC3A2 is a single transmembrane regulatory protein responsible for maintaining the structural stability of System Xc− (Koppula et al. 2018). System Xc− is ubiquitously expressed in the brain, involving the blood–brain barrier and the entire brain parenchyma (Lewerenz and Maher 2011). Under oxidative conditions, in a 1:1 ratio, system Xc- facilitates the transfer of glutamate from the cell via an ATP-dependent mechanism in exchange for extracellular cystine (cysteine dimer cystine, Cys2) (Maher 2005; Cao and Dixon 2016). This process is regarded as the initial and crucial event in the induction of ferroptosis (Ou et al. 2022). Selenium-containing thioredoxin reductase (TXNRD1) rapidly reduces ingested cystine to cysteine, an essential substrate for the synthesis of GSH at the expense of NAD(P)H (Ursini and Maiorino 2020). Then, cysteine combines with glutamic acid and glycine to form GSH, and glutamate-cysteine ligase (GCL) and glutathione synthetase (GSS) are rate-limiting enzymes synthesized in these two steps, respectively (Seibt et al. 2019; Yan et al. 2022). Butythionine-(S,R)-sulfoxideimine (BSO) can induce ferroptosis by inhibiting GCL (Friedmann Angeli et al. 2014), while ferroptosis can be inhibited by α-tocopherol and DFO (Seiler et al. 2008). Among them, the pentose phosphate pathway is primarily responsible for producing NADPH. Studies have pointed out that malate 1 (ME1) reduces NADP+ to NADPH via the pentose phosphate pathway, which then affects the cystine–GSH–GPX4 antioxidant axis driven by it, thereby inhibiting ferroptosis (Fang et al. 1970). The pentose phosphate pathway's oxidative branch provides a significant amount of NADPH (Lane et al. 2021). (Fig. 3d).
The antioxidant effect of GSH is dependent on the reduction-active thiol groups on its cysteine residues (Dodson et al. 2019a). Therefore, GSH depletion by GPX4 reduces LOOH (e.g., PE-AA-OOH) to nontoxic lipid alcohols (LOH, e.g., PE-AA-OH) (Yang et al. 2014). GSSG generated by the oxidation of GSH is re-reduced to GSH under the catalysis of GSSG reductase (GSR), and NAD(P)H acts as a cofactor of GSR (Wu et al. 2011; Ammal Kaidery et al. 2019) (Fig. 3d).
FSP1–ubiquinone (CoQ10) axis
Interestingly, some cancer cell lines did not undergo ferroptosis in the presence of GPX4 inactivation, suggesting the existence of other anti-ferroptotic mechanisms (Viswanathan et al. 2017), and the FSP1–NADH–CoQ10 axis is one of them, paralleling the GPX4 pathway play a role (Bersuker et al. 2019; Doll et al. 2019). FSP1, also known as AIFM2/AMID/PRG3), is a newly discovered antagonist of ferroptosis (Cheng et al. 2023). FSP1, which is located in the mitochondria, undergoes myristoylation and is subsequently recruited into the plasma membrane. This recruitment leads to a conversion of its pro-apoptosis activity into antiferrotic effects (Bersuker et al. 2019; Doll et al. 2019). The mechanism behind this conversion is believed to involve FSP1 acting as an NAD(P)H-dependent coenzyme Q10 (also known as CoQ10 or ubiquinone) oxidoreductase at the plasma membrane. In this role, FSP1 reduces CoQ10 to its antioxidant form, ubiquinol (CoQ10H2), which then scavenges lipid peroxyl radicals (Bersuker et al. 2019; Jiang et al. 2021), and ubiquinone is synthesized via the mevalonate pathway. Or FSP1 promotes oxidative damage repair of plasma membranes (Dai et al. 2020b). In addition, FSP1 can also act as an NAD(P)H-dependent vitamin K reductase, mediating non-canonical vitamin K cycling to protect cells from harmful lipid peroxidation and ferroptosis (Mishima et al. 2022) (Fig. 3d).
The GCH1–BH4–phospholipid axis
GTP cyclohydrolase 1 (GCH1), a key enzyme in the endogenous synthesis of tetrahydrodiphosphate (BH4), is an additional ferroptosis inhibitor independent of GPX4 (Kraft et al. 2020). Synthetic BH4 is hypothesized to prevent ferroptosis by promoting the FSP1–CoQ10 axis to increase panthenol and regulating lipid peroxidation (Kraft et al. 2020; Soula et al. 2020) (Fig. 3d).
Lipid peroxidation
Although iron overload is not a necessary condition for cellular ferroptosis, it is more common for it to cause dysregulation of LIP resulting in disturbance of the intracellular redox state. LIP contains unbound iron, and its alteration is caused by: 1. Induction of ferritin autophagy, leading to the release of Fe2+ by erastin or lack of cysteine; 2. Catalysis of heme decomposition by heme oxygenase 1 (HO1/HMOX1) to produce Fe2+; 3. Mediated uptake of ferritin-bound iron by Tf–TfR1; 4. Inhibition of iron storage or iron efflux (Kakhlon and Cabantchik 2002). The process of ferroptosis, also known as labile iron(Fe)-mediated "autooxidative" non-enzymatic lipid peroxidation, is initiated when there is an excess of active unbound iron, which can either directly accelerate the creation of free radicals or create ROS through the Fenton reaction (Brown et al. 2018). However, the exact mechanism of ferroptosis remains unclear (Feng and Stockwell 2018). The accumulation of active species such as ROS will cause lipid peroxidation, and the accumulation of its products and reactive degradation products will result in ferroptosis.
Thus, the build-up of LOOH is considered an important feature of iron death, and PUFA on phospholipids is a determinant of this due to preferential oxidation (Ou et al. 2022). As a result, the PUFA transport and binding proteins involved affect how sensitive the cell membrane is to phospholipid peroxidation events (Maiorino et al. 2018; Miotto et al. 2020). Acyl-CoA synthetase long-chain family member 4 (ACSL4) and lysophosphatidylcholine acyltransferase 3 (LPCAT3) are to be accountable for activation of PUFAs to produce long-chain lipid acyl-CoA (PUFA-CoA) (Table 1), insertion of acyl groups into lysophospholipids (PUFA-PE), respectively (Yuan et al. 2016; Doll et al. 2017). Further, lipid peroxidation leads to fragmentation of PUFAs and membrane lipid damage, leading to irreversible membrane perforation and ferroptosis through a transmissible osmotic mechanism (Riegman et al. 2020). Recent studies have identified PKCβII as an important sensor of lipid peroxidation. PKCβII senses initial lipid peroxidation and amplifies it through phosphorylation and activation of ACSL4 (Zhang et al. 2022a). H2O2 produced by NADPH-cytochrome P450 reductase generates free radicals catalyzed by Fe2+ (Zhang et al. 2022a). There are also lipoxygenases (LOX) containing oxidized trivalent non-heme iron that can directly oxidize PUFA on the membrane (PUFA-PE) (Wenzel et al. 2017; Chu et al. 2019; Stockwell and Jiang 2020; Yan et al. 2021a) (Fig. 3d). Reactive lipids (RLS) generated by the peroxidation of lipids, such as malondialdehyde, or MDA, and 4-hydroxy-2-nonenal (4HNE), have been linked to the development of several disorders, such as diabetes and neurodegeneration (Ayala et al. 2014).
Nrf2
Nuclear factor E2-related factor 2 (Nrf2, encoded by the Nfe2l2 gene) is a key transcription element involved in the control of intracellular oxidative stress (OS), directly regulating more than 200 antioxidant and phase II genes (Dodson et al. 2019b; Song and Long 2020), many of its downstream target genes are involved in ferroptosis, including FTL/FTH/FPN related to iron metabolism and GPX4/SLC7A11/GCL/GSH related to antioxidant system (Dodson et al. 2019a). Nrf2, along with Nrf1, Nrf3, the NF-E2 p45 subunit and the less related factors BTB domain and CNC homologs 1 and 2 (Bach1 and Bach2), belongs to the Cap 'n' Collar (CNC)-bZIP (basic leucine zipper) family of transcription factors (Toki et al. 1997; Itoh et al. 1999). This classification is based on the high homology of Nrf2 with its cross-species orthologs, such as SKN-1 in Caenorhabditis elegans and CncC from Drosophila melanogaster (Itoh et al. 1999), divided into seven structures from Neh1 to Neh7 (Sivandzade et al. 2019) (Fig. 2). The Neh1 domain is located at the C-terminal side of the molecule, is responsible for DNA binding (Sun et al. 2009) and contains the nuclear localization signal (NLS) (Theodore et al. 2008). The Neh2 domain at the N-terminal end of Nrf2 contains two Kelch-like ECH-associated protein-1 (Keap1) binding sites (ETGE and DLG) that interact with Keap1 to negatively regulate the Nrf2 signaling pathway (Suzuki et al. 2013). Neh3 is located at the C-terminal end of the molecule and is responsible for activating the antioxidant response element (ARE) in the target gene promoter to cis-regulate the target gene (Nioi et al. 2005). Neh4 and Neh5 are involved in transactivation to enhance the transcriptional activity of Nrf2 by recruiting the "cAMP (cyclic adenosine monophosphate) response element-binding" (CREB) proteins (Kwok et al. 1994; Katoh et al. 2001; Nioi et al. 2005). Neh6, a serine-rich residue, associates with Neh2 to mediate Nrf2 ubiquitination (Chowdhry et al. 2013). The Neh7 domain, discovered later, reduces the expression of Nrf2 target genes by binding to retinoic acid receptor α (RARα) and destroying the binding of CBP (CREB-binding protein) to Neh4 and Neh5 domains, so RARα is considered a repressor of Nrf2 (Wang et al. 2013).
Nrf2 domain schematic depiction. Nrf2 comprises seven functional domains and 605 amino acid residues (Neh1–7). Neh2 located at the N-terminus has 29DLG31 and 79ETGE82 motifs, which can bind to the Keap1 homodimer of the E3-ubiquitin ligase complex Keap1–Cul3–Rbx1 to mediate its degradation. Neh4 and Neh5 bind to CREB-binding protein (CBP) and activate transcription. Neh7 binds to retinoic acid receptor alpha (RARα). Neh6 is rich in serine residues and inhibits Nrf2 by interacting with B transducin repeat-containing protein (B-TrCP). Neh1 contains a bZip motif, which can form a dimer with Maf or Bach protein, and then bind to DNA (specifically, the ARE sequences in the target gene promoter). Neh3 is the transactivation domain. Drawing by Inkscape
Under physiological conditions, Nrf2 maintains a low level in the cytoplasm, and its half-life is very short (He et al. 2020). Due to different E3-ubiquitin ligase complexes [Keap1–Cullin 3–Ring box 1 (Keap1–Cul3–Rbx1) (He et al. 2020), S-phase kinase-associated protein 1-Cullin1-Rbx1/β-transducin repeat protein (SCF/β-TrCP) (Rada et al. 2011; Chowdhry et al. 2013; Cuadrado 2015), synoviolin/Hrd1 (Wu et al. 2014) and WDR23/DDB1 and Cullin4 associated factor 11 (WDR23/DCAF11) (Lo et al. 2017)], Nrf2 undergoes ubiquitination and degradation. Specifically, the two Keap1 molecules bind to ETGE and DLG located in the Neh2 domain of Nrf2 and recruit the Cul3–Rbx1 complex to maintain normal levels of Nrf2 (Kobayashi et al. 2004; Cullinan et al. 2004; Zhang et al. 2004); The interaction of β-TrCP and Skp1–Cul1–Rbx1 complex on the Neh6 domain phosphorylated by GSK-3β can also lead to the ubiquitination and degradation of Nrf2 (Rada et al. 2011; Chowdhry et al. 2013; Cuadrado 2015); The combination of DCAF11, DDB1–Cul4–Roc1 and Neh2 (Lo et al. 2017), the upregulation of Hrd1 caused by ER stress, can also mediate the degradation of Nrf2 (Wu et al. 2014). When cells are exposed to OS, gene mutations and other factors, the degradation of Nrf2 by the above complex may be impaired, such as: pro-oxidant conditions, autophagy disorders inhibit the combination of Keap1 and Nrf2 (Jain et al. 2010; Llanos-González et al. 2020), to activate Keap1–Nrf2–ARE axis (Sova and Saso 2018; Panieri and Saso 2019).
Keap1–Nrf2–ARE axis
Keap1, which senses OS through cysteine residues, undergoes conformational changes and releases Nrf2 (Miseta and Csutora 2000). Among them, nucleophilic thiols including Keap1 cysteine sulfhydryl groups can be covalently bound to a variety of electrophile Nrf2 inducers (Prestera et al. 1993; Dinkova-Kostova et al. 2002), and this cysteine modification can sense electrophilic or oxidative conditions to activate Nrf2 (Holland et al. 2008). Keap1 can be poly-ubiquitinated by modifying its own central linker domain under specific chemical and OS conditions (Zhang et al. 2005a; Hong et al. 2005). Under stress conditions, binding of p62 to Keap1 (Hancock et al. 2012) drives the binding of microtubule-associated protein 1 A/1 B-light chain 3 (LC3), which in turn leads to Keap1 degradation (Komatsu et al. 2010). Nrf2 in turn upregulates the expression of the p62 gene by binding to its ARE sequence, thereby forming a positive feedback loop (Jain et al. 2010). Due to the suppression of its breakdown brought on by these factors, Nrf2 levels in the cytoplasm rise, increasing its translocation to the cell nucleus. (Kobayashi and Yamamoto 2005; Zhang 2006).
Nrf2, after translocating into the nucleus, forms a heterodimer with small musculoaponeurotic fibrosarcoma (Maf) proteins (in vertebrates, MafF, MafG, or MafK), specifically in the CNC-bZIP region of the Neh1 domain. This heterodimerization enables Nrf2 to bind to AREs in the upstream promoter regions of various target genes, thereby leading to their transcriptional activation (Motohashi et al. 2004; Hirotsu et al. 2012) (Fig. 3d). Expression of these target genes protects cells from ferroptosis due to lipid peroxidation by participating in the regulation of iron metabolism and antioxidant systems. Interestingly, as a key regulator of ferroptosis, Nrf2 not only has a wide range of regulation, but also has a strong regulation ability. The promoter of its gene contains two ARE-like sequences, so that the downstream target genes have a longer expression time (Kensler et al. 2007). Nrf2 plays a key role in mediating iron/heme metabolism by regulating genes such as FTH1, FTL and FPN1 (Chen et al. 2020).
Nrf2-regulated iron death mechanisms in neurodegenerative diseases. a Blood–brain barrier (BBB), astrocytes, and neurons. Brain capillary endothelial cells (BCECs) safeguard the function of the BBB. Astrocytes on the abluminal surface of BCECs promote brain iron uptake. Astrocytes are primarily responsible for releasing iron into neurons while attenuating iron toxicity. b the transcytosis model. After Fe3+ entering the blood circulation forms a complex (holo-Tf) with transferrin (Tf), it binds to TfR1 on the surface of brain microvascular endothelial cells (BMECs), and then the Tf–TfR1 complex enters BMECs through clathrin-mediated endocytosis. One of the two models of iron import across BCEC—the transcytosis model. Holo-Tf is transported directly by vesicles to extraluminal sites for release into the brain. c Nrf2 in astrocytes activates non-cell-autonomous protection of nearby neurons and alleviates oxidative stress (OS) by mediating antioxidant responses. GSH produced in the brain via activated Nrf2 pathway is predominantly derived from astrocytes, whose neuroprotective function depends on the transport of GSH precursors from astrocytes to motor neurons. d Regulation of iron in neurons and mechanisms of Nrf2-regulated ferroptosis in neurodegenerative diseases. The key components of ferroptosis are the lipid and antioxidant systems, as well as iron metabolism. metabolism of iron: The Tf–TfR1 complex carrying Fe3+ is endocytosed into neurons, Fe3+ is separated from Tf, and then reduced to Fe2+ by six transmembrane epithelial antigen-prostate 3 (STEAP3), and Fe2+ is pumped into the cytoplasm through divalent metal transporter 1 (DMT1), which is also a classic model of iron import across BCEC. Alternatively, Fe3+ reduced by cellular prion protein (PrPC) is transported into neurons by DMT1. In addition, solute carrier family 39 member 14 (SLC39A14) can also transport Fe2+ into the cell. Intracellular iron can be stored in two forms: as Fe3+ stored in ferritin or as active unbound iron called the labile iron pool (LIP). Poly-(rC)-binding protein1/2 (PCBP1/2) are in charge of transferring the iron to ferritin. In some cases, nuclear receptor coactivator 4 (NCOA4) mediates ferritin autophagy, releasing iron. Heme oxygenase 1 (HO1) catalyzes the degradation of heme and can also release Fe2+. With the aid of amyloid precursor protein (APP), which is transmitted by soluble tau protein to stabilize FPN1, elevated Fe2+ can be expelled through Ferroportin1 (FPN1)/copper cyanine (Cp) or FPN1/hephaestin (Heph). Through the IRP–IRE interaction, iron can, when overloaded, increase the expression of ferritin, FPN1, and APP, while blocking the ordinary function of furin, upregulating secretase, and speeding up the deposition of Aβ. By the Fenton reaction, excessive Fe2+ produces ROS and encourages the oxidation of PUFA on the membranes of cells (PE-PUFA), and finally triggers ferroptosis. Lipid metabolism: Lysophospholipid acyltransferase 3 (LPCAT3), long-chain fatty acid CoA ligase 4 (ACSL4), and other enzyme-sensitize membrane lipids to lipid peroxidation, which, catalyzed by lipoxygenases (LOX), accumulates PUFA-OOH, triggering ferroptosis. Antioxidant system: GSH–GPX4 axis in cytoplasm and mitochondria, ferroptosis suppressor protein 1 (FSP1)–CoQ10 axis in plasma membrane, dihydroorotate dehydrogenase (DHODH)–CoQ10H2, and GTP cyclohydrolase1–tetrahydrobiopterin (GCH1–BH4) axis in mitochondria. Mitochondrial PTEN-inducible putative kinase 1 (PINK1) expression is regulated by Nrf2 under OS conditions. Keap1–Nrf2–ARE axis: Under OS conditions, Keap1 releases Nrf2, and the increase of Nrf2 levels in the cytoplasm increases its nuclear translocation. Upon nuclear import, Nrf2 forms a heterodimer with the small muscular aponeurotic fibrosarcoma (Maf) protein, enabling Nrf2 to bind to AREs in the upstream promoter regions of a variety of target genes, leading to their transcriptional activation. Drawing by Inkscape
FTH/FTL
FTH1 (ferritin heavy chain 1) and FTL (ferritin light chain) are the two subunits that make up ferritin. Among them, FTH1 can oxidize Fe2+ to Fe3+, and FTL promotes the entry of free iron into the ferritin mineral core (Chen et al. 2020).
FPN1
Ferroportin1 (FPN1, additionally referred to as solute carrier family 40 member 1, SLC40A1) is currently the sole known cellular exporter of non-heme iron (Drakesmith et al. 2015), widely distributed in the CNS (Smith et al. 1997), and is thought to have a significant regulation influence on the iron metabolism of the CNS (Kalinina et al. 2014; Ma et al. 2020; Bao et al. 2020, 2021), which is modulated by Nrf2 transcription (Marro et al. 2010). Knockdown of Nrf2, which upregulates FPN1, prevents BMECs from transporting iron to the brain via FPN1 (Chen et al. 2020; Han et al. 2021), so it may be possible to lower Nrf2 to prevent brain iron excess (Han et al. 2021). It should be pointed out that the majority of the target genes mediated by Nrf2 function as antioxidants (Hayes and Dinkova-Kostova 2014).
FPN1 is also inhibited by hepcidin (Nemeth et al. 2004; Billesbølle et al. 2020). Hepcidin is secreted peripherally by the liver (Ganz 2013) and readily crosses the BBB. There may be a strong correlation between decreased FPN1 expression on the plasma membrane of neurons and particular kinds of glial cells (Devos et al. 2020), but the link between hepcidin levels in the brain and changes in iron levels in PD or ALS remains unclear (Nemeth et al. 2004; Jeong and David 2006).
HO1
Heme oxygenase 1 (HO1, HMOX1), responsible for catalyzing the heme's breakdown to yield equimolar levels of Fe2+, biliverdin, and CO (Loboda et al. 2016) (Fig. 3d). The antioxidant properties of biliverdin and its reduced product bilirubin [mediated by biliverdin reductase (BVR)] can inhibit ferroptosis, while the redox activity of Fe2+ promotes (Loboda et al. 2016). Therefore, the regulation of HO1 on ferroptosis is two sided and depends on cell type and background (Sun et al. 2016; Chen et al. 2020). In HT1080 fibrosarcoma cells, HO1 overexpression facilitated ferroptosis brought on by erastin (Kwon et al. 2015; Chang et al. 2018); however, knockdown of HO1 produced the same effect in renal proximal tubular cells and hepatoma cells (Sun et al. 2016; Adedoyin et al. 2018). The regulation of ferroptosis by HO1 can be influenced by a combination of HO1-catalyzed heme metabolites and other Nrf2 target proteins, including FTH1, FTL, FPN1, and BVR (Lane et al. 2021).
NQO1
NAD(P)H:quinone oxidoreductase 1 (NQO1), a classical Nrf2-regulated NAD(P)H-dependent dehydrogenase (quinone) reductase (Ross and Siegel 2017), inhibits ferroptosis (Sun et al. 2016). Using two electrons, NQO1 can effectively catalyze the conversion of ubiquinone, a quinone, to hydroquinone (Ernster 1967; Hosoda et al. 1974; Lind et al. 1982; Thor et al. 1982), and also act as a superoxide reductase to exert antioxidant effects (Siegel et al. 2004; Zhu et al. 2007). In addition, vitamin E quinone (α-tocopheryl quinone, TQ), as an endogenous quinone substrate for NQO1, can be reduced to the potent antioxidant α-tocopheryl hydroquinone (THQ) to maintain its antioxidant activity (Siegel et al. 1997), and act as a potent endogenous lipid peroxidation and ferroptosis inhibitors (Hinman et al. 2018) (Fig. 3d). NQO1 is upregulated through Nrf2 in response to OS, and elevated NQO1 associated with AD pathology is often viewed as a neuroprotective response to OS in AD (Raina et al. 1999; Wang et al. 2000; SantaCruz et al. 2004). NQO1 may also cooperate with FSP1 to exert anti-ferroptosis effect (Santoro 2020). Sensitivity of U2OS cells to RSL3 was unaffected in the absence of NQO1, however, compared to cells lacking only FSP1, cells lacking both FSP1 and NQO1 were far more sensitive (Bersuker et al. 2019).
Antioxidation system
In the antioxidant system, the target enzymes of Nrf2 are involved in glutathione synthesis and metabolism, including GCLC and its modified subunits GCLM, GSS, xCT protein (SLC7A11), which are required for the synthesis of GSH (Ishii et al. 2000; Chan and Kwong 2000; Kwak et al. 2002; Sasaki et al. 2002; Yang et al. 2005), and maintain and increase GSH levels to ensure the ferroptosis suppression effect of GPX4. In particular, in mitochondria, dihydroorotate dehydrogenase (DHODH), which uses the oxidation of dihydroorotic acid to form orotate to mediate the reduction of ubiquinone to keep ubiquinone levels in mitochondrial membranes, is also regulated by Nrf2 (Mao et al. 2021). Among the intermediate metabolites regulated by Nrf2 is the aldoketone reductase (AKR) class (Penning 2017). AKR reduces aldehydes and ketones to alcohol forms at the expense of NAD(P)H consumption (Penning 2017). 4-Hydroxynonenal (4-HNE), an outcome of the lipid peroxidation procedure (Jaganjac et al. 2020), which has cytotoxic effects such as damaging structural proteins, reducing enzyme activity, and inducing cell death (Craighead 1995), is significantly elevated in ferroptosis (Feng and Stockwell 2018). Elevated 4-HNE is found in the cerebral tissues of individuals with Alzheimer's after autopsy (Yoo et al. 2010). Possibly, 4-HNE attacks amyloid-β (Aβ) peptides and forms adducts that encourage the production of proto-fibrils and disease-associated accumulation (Siegel et al. 2007). In reaction to Nrf2 activators, AKR1C1 and AKR1C2 are continuously excessively expressed and detoxify by decreasing 4-HNE (Penning 2017). Additionally, there are Nrf2 target enzymes such as aldehyde dehydrogenase 1 family member A1 (ALDH1A1), which oxidizes aldehydes to the carboxylic acid form, and glucose 6-phosphate dehydrogenase (G6PD), which is responsible for glucose metabolism/NAPDH neurodegeneration (Thimmulappa et al. 2002; Huang et al. 2010) (Fig. 3d).
Regulation of Nrf2
As previously mentioned, in addition to Nrf2 negative regulators such as Keap1 and GSK3β, BTB domain and CNC homolog 1 (BACH1), a heme-binding transcriptional repressor of Nrf2-regulated genes (Dhakshinamoorthy et al. 2005), is stable under physiological conditions and interacts with Nrf2 Competes binding to ARE sequences to repress Nrf2 downstream target genes (Warnatz et al. 2011). In response to OS and/or elevated heme levels, BACH1 is inactivated, leading to Nrf2-induced transcriptional activation (Ogawa 2001; Suzuki et al. 2003; Sun et al. 2004). For example, HO1 expression is repressed by BACH1 at low levels of labile heme; however, an increase in labile heme causes BACH1 to degrade and thus relieves this repression (Zhang et al. 2018). The study found that for erastin-induced GLCM, xCT, FTH1, FTL, and FPN1, and other antioxidant system and iron metabolism-related proteins, BACH1 inhibited the transcription of their coding genes and promoted ferroptosis (Nishizawa et al. 2020). Activated GSK3β can also phosphorylate Fyn kinase (a member of the Src family), leading to its nuclear accumulation while Nrf2 nuclear export (Jain and Jaiswal 2007). Nrf2 can be activated by negative regulation of GSK3β, such as the activated PI3K–Akt pathway (Chowdhry et al. 2013), and AMP-activated protein kinase (AMPK). AMPK can also directly phosphorylate Nrf2 to promote its nuclear accumulation (Joo et al. 2016) (Fig. 3d).
AD
AD is a neurodegenerative disease with a complex pathological mechanism that mainly damages cortical and hippocampal neurons, characterized by senile plaques (Cheignon et al. 2018) and neurofibrillary tangles (NFT) (Wan et al. 2019). Senile plaques are derived from aggregated insoluble amyloid beta (Aβ), while intracellular NFT are formed from hyperphosphorylated microtubule-associated protein tau (Masaldan et al. 2019). However, the pathogenesis of AD cannot be fully explained by the aggregation of Aβ and tau proteins alone, and strategies to reduce the burden of Aβ have not been effective in limiting disease progression (Morris et al. 2014). Intracellular iron deposition is present and associated with these pathological features long before development (Goodman 1953; Connor et al. 1992; Smith et al. 1997, 2007; Lovell et al. 1998), Ferroptosis has been recognized as a significant factor in the death of neurons in patients with AD (Ashraf et al. 2020; Park et al. 2021). Abnormal iron elevations are more significant in the preclinical stages of AD, especially in the AD-affected cortex and hippocampus (Smith et al. 1997; Belaidi and Bush 2016). It has been proposed that the rate of cognitive deterioration brought on by A may be predicted by the amount of iron that accumulates in the hippocampus (Ayton et al. 2017). It is widely acknowledged that iron has a role in the early pathophysiology of AD (Goodman 1953).
When iron overloads, hypoxia-inducing factor α (HIFα) is degraded and down-regulates iron-regulatory protein (IRP), which binds to iron-regulatory elements (IRE) linked to iron metabolism in brain tissue, inhibits the translation of TfR1 and DMT1 and promotes the translation of ferritin, FPN1, and APP (Rogers et al. 2002; Anderson and Frazer 2017), which leads to increased iron storage and iron outflow in neurons and decreased iron intake (Meyron-Holtz et al. 2004). At this time, the balance of APP lyases called α- and β-secretases regulated by furin is disrupted, and together with the upregulation of APP, Aβ deposition is accelerated (Silvestri and Camaschella 2008; Guillemot et al. 2013). Abnormally cleaved APP no longer assists FPN1, leading to inhibition of iron export and aggravated iron accumulation (Ward et al. 2014; Greenough 2016). At elevated extracellular iron levels, soluble Aβ binds to Fe3+ and promotes its reduction to Fe2+, which is difficult to dissociate, and additional senile plaques are created as a result of the rapidly precipitation of Aβ caused by the ROS produced in this phase (Ha et al. 2007) (Fig. 3d). However, there are multiple possible pathways for iron-induced tau hyperphosphorylation in neurons: the palliative effect of insulin suggests interference with insulin signaling as a possible cause (Wan et al. 2019); iron-mediated activation of the cyclin-dependent kinase 5 (CDK5)/P25 complex and glucose Prosynthase kinase 3β (GSK3β) may also be involved (Guo et al. 2013a); excess intracellular Fe2+-induced oxygen free radical production can also be induced by activation of extracellular signal-regulated kinase 1/2 (Erk1/2) or mitogen-activated protein Kinase (MAPK) signaling pathway plays the same role (Muñoz et al. 2006; Chan and Shea 2006). In turn, the reduction of soluble tau protein levels in brains with AD inhibits FPN1 activity, exacerbating brain iron deposition (Lei et al. 2012). The participation of activated glial cells in the development of neuroinflammation is a distinctive feature of the pathology of AD (Newcombe et al. 2018; Leng and Edison 2021). Microglia activated by increased brain iron levels, possibly via pro-inflammatory cytokines that are mediated by nuclear factor-B (NF-B) (Meng et al. 2017), overexpress ferritin to remove extracellular iron (Streit et al. 2022), triggering intracellular iron retention and TNFα expression increase (Holland et al. 2018; Kenkhuis et al. 2021), eventually leading to the formation of Aβ-plaques in the permeable zone (Peters et al. 2018; Kenkhuis et al. 2021). In addition, Lf secreted by activated microglia interacts with APP to promote Aβ formation (Tsatsanis et al. 2021). Similarly, the formation of Aβ induced increased expression of the pro-inflammatory factor IL-1β in microglia in a high-iron environment (Nnah et al. 2020). Astrocytes resist high iron-induced OS by significantly increasing GSH, catalase, and manganese superoxide dismutase (Iwata-Ichikawa et al. 2002; Shih et al. 2003). However, later findings overturned the previous understanding: when astrocytes are activated, they release inflammatory cytokines and trigger OS, which promotes the production of Aβ and tau tangles and impedes the clearance of Aβ (Cai et al. 2017). Metabolites such as 4-HNE and malondialdehyde produced by iron overload-mediated enzymatic (LOX) and/or non-enzymatic (Fenton reaction) lipid peroxidation are also elevated in AD brain (Wong et al. 2014a; Yang et al. 2016), then the PUFA on the membrane is depleted (Ansari and Scheff 2010; Elharram et al. 2017). In iron metabolism, to block iron entry into the brain, knockdown of Nrf2 reduces FPN expression on BMECs and may serve as a means to avoid brain iron overload (Han et al. 2021).
However, Nrf2 plays a critical role in the regulation of the antioxidant system. Age-related decline in Nrf2 levels, particularly in the brains of patients with AD (Osama et al. 2020), could potentially signify an early occurrence of ferroptosis (Habib et al. 2015). Although OS levels ARE elevated in AD, the transcriptional activation of Nrf2 is defective and/or incomplete due to reduced nuclear entry and/or defective binding to ARE (Kraft et al. 2004; Ramsey et al. 2007). As mentioned earlier, the excessive activation of GSK3β not only mediates the degradation of Nrf2, but also participates in tau hyperphosphorylation, Aβ aggregation-related neuroinflammation (Hooper et al. 2008), making it a possible reason for the decreased Nrf2 activity in AD (Lane et al. 2021). The negative regulation for Nrf2 by BACH1 is another enabler (Di Domenico et al. 2015; Perluigi et al. 2020). In trisomy 21, BACH1 located on chromosome 21 is elevated, the target gene of Nrf2 is suppressed, and confers an increased risk of AD-like dementia (Perluigi et al. 2020). Limited studies have demonstrated that BACH1 changes occur in the AD brain (Shim et al. 2003). Interestingly, a meta-analysis showed that in the presence of increased NRF2 gene expression, 31 target genes of Nrf2 were still significantly downregulated in AD (Wang et al. 2017). In contrast, the gene encoding the sMAF protein MafF is markedly increased in AD, which may partly explain the defect in Nrf2 stimulation (Wang et al. 2017): increased MarF promotes its homodimer formation, leading to repression of Nrf2 (Igarashi et al. 1994) (Fig. 3d).
The influence of lipid peroxidation on the Nrf2 pathway is twofold (Dinkova-Kostova et al. 2017): on the one hand, the electrophilic modification of Keap1 by lipid peroxidation products such as 4-HNE can activate the Nrf2 pathway; on the other hand, excessive lipid peroxidation leads to inactivation of Nrf2-regulated antioxidant-related enzymes such as GCL, TXNRD1, and PRDX6 (Dinkova-Kostova et al. 2017), which disrupts the homeostasis of the redox system and drives ferroptosis in AD (Dodson et al. 2019a). Similarly, with changes in Nrf2, its ferroptosis-related target proteins are altered in AD (Lane et al. 2021). In AD brain, the levels of GSH, GPX, GST, GR and other antioxidant enzymes decreased, while GSSG increased (Ansari and Scheff 2010). The study discovered a beneficial association between cognitive deterioration and decreased GSH expression in the cerebral cortex of AD animal models (Karelson et al. 2001). Consequently, the amount of GSH have been suggested to be predictive of AD and moderate cognitive impairment in the frontal brain lobe and hippocampus (Mandal et al. 2015; Ayton et al. 2020). Selenium levels affect the activity of GPX4 and TXNRD1, which have been reported to be inversely connected to cognitive deterioration (Cardoso et al. 2015). And the meta-analysis confirmed that the reduction in selenium content occurs in the affected temporal cortex of the AD brain (Cardoso et al. 2017; Varikasuvu et al. 2019). In addition to the regulation of transcriptional activation of the antioxidant system, Nrf2 is also regulated in AD in other ways (Bahn et al. 2019). BACE1 is primary enzyme accountable for the production of Aβ, which plays an important role in the pathogenesis of AD (Vassar et al. 1999; Cai et al. 2001; Selkoe 2012), and can bind to the long non-coding RNA (BACE1-AS) transcribed from its complementary strand to stabilize BACE1 mRNA (Faghihi et al. 2008). Increased BACE1-AS and BACE1 expression, Aβ deposition and cognitive deficits were more pronounced in Nrf2-deficient AD mice compared with Nrf2-deficient mice and AD mice, suggesting that Nrf2 is a negative regulator of BACE1-AS and BACE1 (Bahn et al. 2019). Nrf2 inducers, such as sulforaphane from cruciferous vegetables, and tert-butylhydroquinone (tBHQ) (Kraft et al. 2004), activate Nrf2 to inhibit the expression of BACE1 and BACE1-AS through the modification of the cysteine residue of Keap1 to prevent the production of Aβ, a key pathogenic process in the early stages of AD (Dinkova-Kostova et al. 2002; Kobayashi and Yamamoto 2006; Bahn et al. 2019). Nrf2 expression in adjacent astrocytes may determine the protective effect of Nrf2 inducers on neurons (Kraft et al. 2004). Nrf2 expression in neurons, although not as likely to be dominant as in glial cells (Kraft et al. 2004; Liddell 2017), is also believed to be crucial in the body’s defense against damage from oxidization (Ramsey et al. 2007). When Nrf2 is lacking, neurons are more vulnerable to cell death caused on by oxidative stressors such H2O2 (Kraft et al. 2004); conversely, overexpression of Nrf2 can protect neurons (Lee and Johnson 2004).
PD
PD, also known as tremor paralysis, is a common motor system-specific neurodegenerative illness (Ammal Kaidery et al. 2019). The primary pathogenic features of PD are the persistent reduction of dopaminergic neurons containing neuromelanin in the substantia nigra densa (SNpc) and the formation of intracellular inclusion bodies by α-synuclein (α-Syn), i.e., Lewy bodies (Lee Mosley et al. 2006; Hustad and Aasly 2020). The following elements work together to cause PD: The biggest risk factor is age (Ammal Kaidery et al. 2019); additionally, it is believed that OS, mitochondrial malfunction, and neuroinflammation are the primary processes causing cell death in PD (Jenner and Olanow 2006; Yacoubian and Standaert 2009); meanwhile, environmental and genetic factors also affected it. In addition, abnormal iron deposits have been found in the brains of PD patients (Lhermitte et al. 1924). These factors interact with progressive PD, complicating the pathogenesis of the latter (Yang et al. 2022b).
An significant manifestation of OS is the increase of ROS and RNS levels, and mitochondria are an important source of ROS in cells (Di Meo et al. 2016). Immunohistochemical discovery of 4-HNE protein adducts provided early support for an etiological link of ROS with PD in postmortem neurons in the substantia nigra (SN) of the brain of seven PD patients (Yoritaka et al. 1996). The occurrence of OS in PD has also been demonstrated in animal models of PD (Wang et al. 2021a). As a byproduct of heroin synthesis, 1-methyl-4-phenyl-1,2,3,6- tetrahydropyridine (MPTP) has been shown to cause Parkinson-like symptoms (Langston et al. 1983; Dong et al. 2021). Further studies have found that MPTP induces cellular oxidative stress by indirectly affecting mitochondrial complex I (nicotinamide adenine dinucleotide (NADH) cytochrome c reductase) to block the electron transport chain (ETC), leading to cell death (Poirier and Barbeau 1985) (Fig. 3d).
Insecticides such as rotenone (Sharma et al. 2021), maneb, and paraquat (Ahmad et al. 2021) have similar mechanisms of action (Ammal Kaidery et al. 2019). Meta-analysis found an increased risk of developing PD after exposure to insecticides (Gunnarsson and Bodin 2019). Schapira's team is the first to identify a defect in PD brains' mitochondrial complex I, compared to other neuronal regions that are normal (Schapira et al. 1989, 1990). Further, autopsy revealed increased mutations and loss of mitochondrial DNA in tissues and blood cells of PD patients suggesting that the malfunctioning of the mitochondria is related to PD. (Coxhead et al. 2016; Pyle et al. 2016). There is mounting evidence that PD is characterized by malfunctioning mitochondria (Prasuhn et al. 2021). Mitochondrial metabolism provides brain cells with energy to maintain them survival (Nolfi-Donegan et al. 2020; Rose et al. 2020), while energy-storing ATP relies on mitochondrial respiration and electron transport chain (ETC) synthesis through oxidative phosphorylation. Among them, the complexes I–V that constitute the mitochondrial ETC are distributed in the inner mitochondrial membrane (Guo et al. 2017; Zhao et al. 2019). In PD, complex I deficiency is the main cause of ROS generation, while ROS are mainly generated in complex I and complex III (Kussmaul and Hirst 2006). Mitochondrial dysfunction produces excessive ROS, which can aggravate mitochondrial damage by attacking mitochondrial DNA, forming a vicious cycle (Elfawy and Das 2019). At the same time, damaged mitochondria can also affect energy metabolism, calcium homeostasis, and eventually induce apoptosis (Markesbery 1997; Peoples et al. 2019; Wang et al. 2021a). NADPH oxidase (NOX) is a class of ROS-producing enzymes, usually divided into seven isoforms: NOX 1 to 5 and dual oxidase (DUOX 1 to 2) (Bedard and Krause 2007). As multisubunit membrane-bound enzymes, they transfer electrons from NADPH to O2 to generate superoxide (Bedard and Krause 2007). Among them, Numerous areas of the brain and different types of brain cells express NOX2, including neurons in striatum (McCann et al. 2008; Guemez-Gamboa et al. 2011) and SN (Zawada et al. 2011; Qin et al. 2013), and compared with neurons and astrocytes, it has a higher expression in microglia More expressed, which was also confirmed in experimental models of PD and PD (Gao et al. 2002; Zhang et al. 2005b; Wu et al. 2005). Furthermore, in astrocytes, NOX4 is the major NOX isoform (Nayernia et al. 2014). Finally, dopaminergic neurons in the SN may also generate ROS through dopamine metabolism leading to neurodegenerative processes (Chinta and Andersen 2008; Hastings 2009).
In PD, OS occurrence is also associated with impaired antioxidation, which is supported by the reduction in GSH levels found in the SN of postmortem PD brains (Sofic et al. 1992), which also further increases iron content (Dexter et al. 1989), causing the formation of ROS and toxic effects on brain area (Kaur et al. 2003). In addition, significant increases in CoQ10 and 8-OHdG (nuclear DNA oxidation biomarkers) were also found in cerebrospinal fluid samples from PD patients (Isobe et al. 2010). Unlike GSH, HO1 levels are elevated in the SN of human PD brains (Schipper et al. 1998). NQO1, also a Nrf2 target enzyme, was also found to be increased in astrocytes, endothelial cells, and dopaminergic neurons in postmortem PD brains (Schipper et al. 1998). According to these postmortem results, Nrf2’s target genes are activated by enhanced nuclear import in PD brains (Fão et al. 2019).
Not only that, but there is also direct evidence that Nrf2 levels are increased in the nucleus of SN neurons in human PD patients (Ramsey et al. 2007). Nrf2 has antioxidant and neuroprotective effects (Yang et al. 2022b). H2O2 in the normal concentration range was found to mediate activation of the Nrf2 signaling pathway in glial cells, protecting dopaminergic neurons (Wang et al. 2021b). There is substantial evidence that Nrf2–ARE pathway activators show greater resistance to neurotoxins including MPTP, paraquat and rotenone in both in vivo and in vitro models (Wang et al. 2021a). Among the numerous target enzymes regulated by Nrf2, HO1 exerts neuroprotective effects against OS injury and may become a new therapeutic target for PD (Jazwa and Cuadrado 2010). Higher concentrations of HO1 are present in the serum of PD patients (Sun et al. 2021). In contrast, Downregulation of HO1 and Nrf2 causes α-synuclein aggregation (He et al. 2013). Presumption of HO1-induced neuroprotection against exposure to multiple PD-associated neurotoxins confirmed based on results from animal models and tissue culture (Kwon et al. 2019; Inose et al. 2020). A recent study found that the PI3K–AKT–glycogen synthase kinase 3 (GSK3) pathway is activated by the chemokine fractalkine (CX3CL1)–CX3CR1 axis to upregulate Nrf2 (Subbarayan et al. 2022), thereby protecting microglia proliferation from the deleterious effects of PD (Yang et al. 2022b). NF-κB, which induces the expression of multiple pro-inflammatory genes, was inhibited by Nrf2 (Cao et al. 2022). Nrf2 also regulates mitochondria-related genes, including the upregulation of the multifunctional DNA-binding protein mitochondrial transcription factor A (TFAM), which has a major impact on the expression of the mitochondrial genome, in addition to the transcriptional activation of essential function-related genes (such as NADH and NADHP formation-related enzymes, NOX) (Yang et al. 2022b). PTEN-inducible putative kinase 1 (PINK1) modulates mitochondrial quality and its expression is regulated by Nrf2 under OS conditions (Murata et al. 2015). Interestingly, PINK1 is not only associated with its stabilization on the dysfunctional mitochondrial outer membrane, but is also involved in the recruitment of p62 for mitochondrial removal (Geisler et al. 2010; Narendra et al. 2010). In a possible connection with this, an ARE element has been reported in the p62 promoter (Jain et al. 2010). Furthermore, p62 stabilizes and activates Nrf2 by interacting with Keap1, tumor suppressor genes (WTX), partner and localizer of BRCA2 (PALB2), dipeptidyl-peptidase 3 (DPP3) and CDK 20) (Komatsu et al. 2010; Fu et al. 2019). Consistent with this, it was found that Lewy bodies in the SN of early PD brains may be associated with p62 (Kuusisto et al. 2003), both in terms of oxidative damage shown by the p62 gene promoter in the frontal cortex of PD brains and in terms of p62 proteasomal degradation (Du et al. 2009) due to mutations in the parkin gene that stabilizes p62 in PD (Lesage and Brice 2009; Song et al. 2016). In addition, PI3K/Akt pathways is inhibited in dopaminergic neurons of the human PD brains (Malagelada et al. 2008). NF-kB accumulates and translocates in the nucleus and increases (Hunot et al. 1997; Soós et al. 2004; Mogi et al. 2007). The above studies indicate that p62, PI3K–Akt pathway, and NF-kB may become potential targets for the treatment of PD (Fão et al. 2019).
HD
Huntington's disease (HD) is a global autosomal dominant delayed ND (Ross and Tabrizi 2011). Mutant huntingtin (mtHtt), an important trigger and pathological feature of HD, is caused by abnormal CAG trinucleotide repeat in the huntingtin (HTT) gene, resulting in amplification of polyglutamine repeats in mtHtt (Tabrizi et al. 2019; Zgorzynska et al. 2021). The N-terminal truncated mtHtt is mismodified to form toxic soluble monomers or small oligomeric fragments with abnormal conformation and further synthesis of oligomers (Ou et al. 2022), precursors of fibrils in the cytoplasm and nucleus (DiFiglia et al. 1997; Cooper 1998; Hoffner et al. 2005). This leads to the dysfunction of the scaffolding protein Htt involved in various physiological processes such as vesicle trafficking, autophagy (Benn et al. 2008; Saudou and Humbert 2016), and eventually leads to degenerative diseases in the striatum and cortex areas of the brain (McColgan and Tabrizi 2018). Impairment of ubiquitin–proteasome (UPS) and autophagy systems affects protein degradation in HD animal models and human tissues (Ravikumar et al. 2004; Lin et al. 2013; Cortes and La Spada 2014). In addition, dysfunction of Htt also affects Brain-Derived Neurotrophic Factor (BDNF) production and inhibition of apoptotic factor activity (Gauthier et al. 2004; Zuccato and Cattaneo 2014; Saudou and Humbert 2016). These toxic macromolecules enter the nucleus of neuronal cells and bind and interact with DNA, while their amplified polyglutamine tracts cause transcriptional dysregulation of antioxidant genes in the binding areas (Hensman Moss et al. 2017; Ferrari Bardile et al. 2019; Tabrizi et al. 2020). These localized toxic fragments in cytoplasm and nucleus can damage mitochondria, resulting in reduced ATP, increased ROS, and other effects (Ayala-Peña 2013).
Compared with the complex pathological mechanism, OS, the initial onset of this HD is clear (Chen et al. 2007). Existing evidence suggests that mtHtt-activated microglia and astrocytes release cytokines that promote ROS production, with increased glutamine release from astrocytes but reduced BDNF from the same astrocytes (Ferguson et al. 2022). Specifically, mtHtt interacts with the inner and outer membranes of mitochondria, thereby blocking mitochondrial protein import (Yablonska et al. 2019), also determines cell death (Choo 2004). Lower levels of glucose metabolism and higher concentrations of lactate than normal in some regions of the HD brain (Reynolds et al. 2005; Tabrizi et al. 2020) corroborate findings of disrupted mitochondrial ultrastructure in the brain of an adolescent HD patients (Goebel et al. 1978). The selective striatal neurotoxin 3-nitropropionic acid (3-NP) can mimic the brain damage observed in HD patients by inducing OS (Brouillet et al. 2005) due to its inhibition of succinate dehydrogenase enzyme (complex II) (Damiano et al. 2010; Zuccato et al. 2010), further confirming the association between HD and mitochondria respiratory chain (Tucci et al. 2022). 3-NP is also involved in the activation of microglia and promotes the release of inflammatory cytokines that lead to neurological dysfunction and striatal neuronal death (Kim et al. 2017). Importantly, in HD, the interaction of mHTT and OS exhibited a prominent bidirectional line (Tobore 2019). OS also exerts an important influence on the mHtt accumulation in the nucleus, such as attacking the proteasome (Son et al. 2019), promoting mHtt aggregation (Goswami et al. 2006). Similarly, the mitochondrial NOX pathway and the Fe2+-involved Fenton reaction are sources of ROS (Tucci et al. 2022). Regarding the link between HD and NOX, high levels of NOX, mainly NOX2 subtypes, were found in the striatum of HD patients (Ibrahim and Abdel Rasheed 2022). Therefore, iron overload is an important factor in triggering HD (Agrawal et al. 2018). Assays in the R6/2 HD mouse model showed elevated ferritin levels in the striatum and cortex, decreased IRP and TfR, and increased FPN (Simmons et al. 2007; Chen et al. 2013). Iron supplementation to HD mice resulted in further shrinkage of the striatum and aggravation of neurodegeneration (Berggren et al. 2015). Conversely, intracerebroventricular injection of iron chelator (DFO) in R6/2 HD mice ameliorated striatal lesions (Agrawal et al. 2018). Similar positive effects were also observed in isolated HD rat brain slices, where treatment with the ferroptosis inhibitor Fer-1 and iron chelators significantly reduced neuronal death (Skouta et al. 2014). These evidences suggest a possible role for ferroptosis in HD (Ou et al. 2022). Autopsy revealed decreased plasma GSH levels (Klepac et al. 2007) and increased lipofuscin (suggesting dysregulation of lipid oxidation) in HD brains (Pérez-Severiano et al. 2000; Stoy et al. 2005; Browne and Beal 2006). Similarly, in the R6/2 HD mouse model, both mtHtt inclusions in striatal neurons and increased lipid peroxidation were found (Agrawal et al. 2018). High lipid peroxidation is a major feature of HD (Hatami et al. 2018). Low levels of GSH are also a feature of HD (Mason et al. 2013). In the 3-NP model of rats, it was found that the significant reduction of GSH was caused by downregulation of Nrf2 (Sayed et al. 2020).
Mitochondrial dysfunction, cellular antioxidants link Nrf2 to HD pathogenesis (Zgorzynska et al. 2021). Precisely through its regulatory role (e.g., GSH, GST), Nrf2 counteracts 3-NP-induced enhanced OS (Vasconcelos et al. 2019). Although the specific mechanism of Nrf2 during mtHtt formation and accumulation is in doubt (Zoungrana et al. 2022), neuroprotection and prolonged lifespan in animal models of HD through its activation of certain parts of the brain are clear (Tsvetkov et al. 2013; Zgorzynska et al. 2021). Nrf2-induced expression of p62 autophagy-associated protein and LC3 mediates rapid clearance of toxic mtHtt aggregates (Saito et al. 2020). Nrf2 reduces levels of pro-inflammatory cytokines and inflammatory mediators released by deposition of mtHtt aggregates through upregulation of HO1 (Dowling et al. 2010; Luo et al. 2018; Zgorzynska et al. 2021). The activity of NOX is also inhibited by Nrf2, which hinders ROS production (Benarroch 2017). Interestingly, Nrf2 can transcriptionally activate BDNF (Huang et al. 2020; Yao et al. 2021), while BDNF can influence Nrf2 translocation and subsequent activation to repair redox homeostasis (Bouvier et al. 2017). A study shows that naringin is neuroprotective against 3-NP-induced neurotoxicity in pheochromocytoma cells (PC12 cells) through PI3K-Akt pathway-mediated Nrf2 activation (Kulasekaran and Ganapasam 2015). In the nervous system, specific activation of Nrf2 in astrocytes can protect neurons (Calkins et al. 2010). Transplantation of Nrf2-overexpressing astrocytes and chemical activation of Nrf2 are protective against 3-NP- and malonate-induced striatal injury, respectively (Shih et al. 2005). In view of this, Nrf2 activation in astrocytes may be a viable treatment option for oxidative stress-related chronic neurodegeneration (Vargas and Johnson 2009).
ALS
Amyotrophic lateral sclerosis (ALS), also known as Lou Gehrig's disease, is the third most common neurodegenerative disorder (Chiò et al. 2013) characterized by degeneration and loss of motor neurons in the cerebral cortex, brainstem, and spinal cord (Wijesekera and Nigel Leigh 2009). Among them, sporadic ALS (sALS) accounts for about 90%, and the possible causes are speculated to be: abnormal immune system, mitochondrial dysfunction, and exposure to toxic environmental chemicals (Martin et al. 2017); the incidence of familial ALS, which accounts for approximately 10%, is related to gene mutations, typically including: Cu2+/Zn2+ superoxide dismutase 1 (SOD1) (Rosen 1993), TAR DNA-binding protein 43 (TDP-43 or TARDBP) (Sreedharan et al. 2008), fused in Sarcoma (FUS) (Vance et al. 2009), and chromosome 9 open reading frame 72 (C9orf72) gene (DeJesus-Hernandez et al. 2011), whose function related to protein homeostasis and RNA metabolism. Mouse models, which express human mutant SOD1, TDP-43, and C9orf72, can mimic ALS-related progressive symptoms and motor neuron loss (Taylor et al. 2016). The degeneration of the upper motor neurons located in the cerebral cortex and the lower motor neurons distributed in the brainstem and spinal cord correspond to different clinical manifestations (George et al. 2022). As ALS progresses, mutated protein aggregates will be released by degenerating spinal motor neuron bundles and taken up into the cytoplasm by other neurons or glial cells (Taylor et al. 2016).
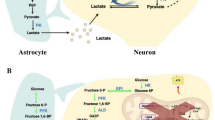
Studies have shown that the aggregation of a variety of abnormal proteins, also known as RNA-binding proteins (Blokhuis et al. 2013), including TDP or FUS, can lead to OS and neurotoxicity (Zuo et al. 2021). In neurons, the progression of ALS will affect RNA metabolism, mitochondrial function, cytoskeletal integrity, axonal transport dynamics, and cause increased neuroinflammation, glutamate excitotoxicity, ROS production (Bonafede and Mariotti 2017), while excessive OS eventually leads to neuronal meta death (Wood and Langford 2014). Gradual accumulation of cytotoxic misfolded protein aggregates and marked loss of motor neurons are similar features of the progression of sALS and fALS (Blokhuis et al. 2013). Aggregated TDP-43 blocks nucleoplasmic transport by disrupting the nuclear pore complexes (Chou et al. 2018). In ALS models, failure of oligodendrocyte precursors to differentiate and mature affects myelin formation in axons (Benarroch 2021). Given the high metabolic rate, active mitochondrial respiration, high activity of NOX, low levels of catalase and GSH, and reduced Nrf2 levels, motor neurons have increased sensitivity to OS (Baxter and Hardingham 2016; Liddell 2017; Brandes and Gray 2020; Izrael et al. 2020). Abnormal oxidative damage, such as signs of lipid peroxidation, was found in biological samples and autopsy tissues from patients with sALS or fALS (Blasco et al. 2017), and was similarly confirmed in ALS cells and animal models (Pedersen et al. 1998; Ferraiuolo et al. 2011; Johnson and Johnson 2015; Moujalled et al. 2017). In ALS mouse models and ALS patients, the GSSG/GSH ratio, an indicator of OS, was also increased (Vargas et al. 2011; Weiduschat et al. 2014; Blasco et al. 2017). Relatedly, in mutant SOD1 mice, GSH synthesis-associated System Xc− dysregulation may cause GSH depletion (Mesci et al. 2015). In particular, aggregation of SOD1 associated with some fALS was shown to be promoted by lipid peroxidation (Dantas et al. 2020). Evidence of iron accumulation was found both in the spinal cord and brain regions of ALS patients (Kasarskis et al. 1995; Moreau et al. 2018) and in neurons of ALS mouse models (Lee et al. 2015; Moreau et al. 2018). In addition, iron-binding protein abnormalities were found in the ALS mouse models (Wang et al. 2022d). Markers of ferroptosis in the blood, such as ferritin, Tf and lipid peroxides, are also associated with ALS prognosis (Devos et al. 2019). Vice versa, CuATSM, a potent inhibitor of ferroptosis (Southon et al. 2020), has a robust and reliable rescue effect in ALS mouse models (Soon et al. 2011; Roberts et al. 2014). Positive effects of two iron chelators, desferrioxamine and deferiprone, were reported for SOD1G93A mice and for SOD1G86R mice and ALS patients, respectively (Lee et al. 2015; Moreau et al. 2018). Substantial evidence links iron accumulation (Oba et al. 1993; Kasarskis et al. 1995; Jeong et al. 2009), imbalances in the antioxidant system (Chi et al. 2007; Choi et al. 2015), and lipid peroxidation (Ferrante et al. 1997; Pedersen et al. 1998), among others, to ferroptosis in ALS-affected CNS regions. Correspondingly, Nrf2, an important regulator of ferroptosis, was found to be attenuated in ALS (Kirby et al. 2005; Wood-Allum et al. 2006), and its reduced activity was shown to be a hallmark of ALS in human biosamples (von Otter et al. 2010; Bergström et al. 2014). Similarly, some studies have also found that in skeletal muscle of an ALS mouse model, increased Nrf2 levels occur at very early time points, even before the onset of movement impairments (Kraft et al. 2007), which may provide support for the hypothesis of motor neuron degeneration starting at the level of the neuromuscular junction (Pavlovskiĭ and Mikaĭlenko 1976). Whereas, lower activation levels of Nrf2 occur in spinal motor neurons and astrocytes during symptoms (Kraft et al. 2007). In NSC-34 SOD1G93A cells, overexpression of Nrf2 can significantly improve OS and reduce cell death (Nanou et al. 2013). Likewise, in SOD1G93A mice, Nrf2 levels were reduced in primary motor neuron cultures compared to wild-type mice in the same litter (Pehar et al. 2007). Interestingly, ALS progression was not significantly affected by Nrf2 loss in multiple SOD1 mouse models (SOD1G93A, SOD1G85R or SOD1H46R) (Vargas et al. 2013; Guo et al. 2013b; Hadano et al. 2016). Further, in the motor neurons of SOD1G93A mice, overexpression of Nrf2 only altered disease onset but not the survival (Vargas et al. 2013). This could be partly explained by the limited protection of Nrf2 against disease markers in backcross experiments between ALS mice and Nrf2-null mice, presumably as a result of compensatory mechanisms (Vargas et al. 2013; Guo et al. 2013b). In addition, studies on lymphoblastoid cells from ALS patients suggest that Nrf2-mediated antioxidant responses may only be present in a specific ALS, namely sALS, but this conclusion remains to be further studied (Lastres-Becker et al. 2021). Mutations in p62, also known as autophagy carrier protein SQSTM1, which can form a positive feedback loop with Nrf2, are associated with ALS and frontotemporal dementia, as previously described (Foster et al. 2020). Among them, the STGE motif contained in p62 can exhibit a high affinity for Keap1 after phosphorylation by signaling kinases such as casein kinase 1 (CK1), transforming growth factor β-activated kinase 1 (TAK1), mTORC1 and PKCσ similar to the ETGE motif of Nrf2 (Ichimura et al. 2013; Hashimoto et al. 2016; Watanabe et al. 2017; Jiang et al. 2017). Among novel genes associated with ALS, 10 SQSTM1 gene (encoding p62) mutations were found in both sporadic and familial forms of ALS, and 8 of 9 missense variants were classified as pathogenic by predictive in silico analysis (Jiménez-Villegas et al. 2021). Interestingly, in the SOD1H46R mouse model, overexpression of p62 instead accelerated the onset of ALS and resulted in shortened lifespan (Mitsui et al. 2018). Due to sporadic and SOD1-associated motor neuron degeneration in the spinal cord, Nrf2-regulated doredoxin 3 (Prx3) is downregulated, suggesting that impaired mitochondrial antioxidant defense is a replacement mechanism for intracellular OS (Wood-Allum et al. 2006). Urate (2,6,8-trioxy-purine), proposed as a prognostic factor for survival in ALS patients due to its reduced levels in the serum of ALS patients (Keizman et al. 2009), is also an important endogenous antioxidant in the body (Sautin and Johnson 2008) that activates Nrf2 by inhibiting GSK3β through Akt (Zhang et al. 2019a). As the role of non-cell-autonomous pathogenic mechanisms has come to the fore, glial cells, dominated by stellate glial cells, play a more prominent role in ALS pathology (Birger et al. 2019; Izrael et al. 2020; Van Harten et al. 2021). Nrf2 in astrocytes activates non-cell-autonomous protection of nearby neurons and improves OS by mediating antioxidant responses (Yamanaka et al. 2008; Vargas et al. 2008; Haidet-Phillips et al. 2011; Liddell 2017; Kim 2021). GSH produced by activated Nrf2 pathway in the brain is mainly derived from astrocytes (Vargas et al. 2006), whose neuroprotective function depends on the transport of GSH precursors from astrocytes to motor neurons (Andronesi et al. 2020; Aoyama 2021) (Fig. 3d). Similarly, activated Keap1–Nrf2–ARE pathways induce the expression of target genes in glial cells at a late stage but not in spinal motor neurons (Mimoto et al. 2012). In the SOD1G93A rat model, Nrf2 levels of astrocytes at the onset of ALS were found to be higher than basal levels in controls (Vargas et al. 2005; Kraft et al. 2007). In contrast, under some circumstances, astrocytes may become reactive and contribute to the neuroinflammatory response, which in turn promotes neurodegeneration (Aoyama 2021). This reactivity also occurs after brain injury (Tripathi et al. 2017), which is considered to be a trigger or a link to ALS (Anderson et al. 2018). The role of astrocytes reactivity in the pathogenesis of ALS has been demonstrated by in vitro cell co-culture (Haidet-Phillips et al. 2011; Ferraiuolo et al. 2011; Tripathi et al. 2017). Nevertheless, also in in vitro co-culture experiments (Vargas et al. 2005), overexpression or chemical activation of Nrf2 in astrocytes was found to reduce neuronal death, and consistent findings were found in ALS mouse models (Vargas et al. 2008). Other glial cells, such as microglia, can also be involved in motor neuron degeneration (Brites and Vaz 2014). Given the higher than neuronal levels of Nrf2 in astrocytes and microglia in the brain (Boas et al. 2021), activation of Nrf2-associated pathways may be a potential treatment options to suppress microglia-mediated inflammatory responses (Li et al. 2018; Saha et al. 2022).
Biomarkers and therapeutics targeting Nrf2 and ferroptosis in NDs
In NDs, increasing evidence has been found for ferroptosis, which has been used to explain the pathogenesis of NDs. During this process, detection and monitoring of ferroptotic responses inevitably became one of the research priorities. Indicators of iron homeostasis include intracellular or mitochondrial Fe2+ levels, NCOA4 (Hou et al. 2016) that mediates ferritin degradation, TFRC in cell cultures or tissues, and anti-TFRC antibodies (known as 3F3-FMA) (Feng et al. 2020) that suggest ferroptosis or related damage. Significant markers involved in lipid peroxidation include NOX, arachidonic acid lipoxygenase (ALOX) isoforms. Importantly, upregulated ACSL4 is a sensitive marker reflecting ferroptosis (Yuan et al. 2016). In addition, there are lipid peroxides (PUFA-OOH, PL-OOH) (Kagan et al. 2017) and end products [MDA (Ye et al. 2020), 4-HNE (Shintoku et al. 2017) etc.], markers of oxidative DNA damage Compound (8OH-dG) can detect and quantify the degree of lipid peroxidation in ferroptosis (Zhang et al. 2019c; Dai et al. 2020a). Some researches indicate that these biomarkers can be detected in relevant experimental models and patient tissues (Table 2).
Nfe2l2 is an iron death-associated gene, and although its pathway activation receives influence from other signaling molecules (e.g., Keap1), its over-regulated target gene reflects to some extent the increased OS damage of ferroptosis. These target genes are involved in iron metabolism, GSH metabolism, antioxidant response, etc. However, it is difficult to determine the specific effect of Nrf2 on ferroptosis based on the expression of Nrf2 target genes alone (Chen et al. 2021). For example, GSH, CoQ10 and BH4, which Nrf2 depends on for its antioxidant effect, are not conducive to the study of specific molecular mechanisms of ferroptosis due to their broad-spectrum effects (Chen et al. 2021). Nrf2-associated markers of ferroptosis require binding to others for specific detection and detection of cellular ferroptosis. Nevertheless, according to several studies (Habas et al. 2013), Nrf2 has become an important therapeutic target of NDs because of its important role in protecting neurons from OS and glutamate-induced excitotoxicity and ultimately maintaining the survival of injured neurons (Zhang et al. 2023).
As previously mentioned, brain iron deposition has been found in a variety of ND. Studies have shown that iron chelators such as DFO, deferiprone (DFP) and cyclopiroxamine (CPX) further prevent iron-dependent OS and ultimately inhibit iron death by binding to ferrous iron to reduce intracellular iron overload (Taher et al. 2017). Clinically, DFP, as an oral hydroxypyridone derivative, is used in the treatment of diseases such as Friedreich's ataxia and thalassemia (Aminzadeh-Gohari et al. 2020). The pathogenesis of several NDs also involves mitochondrial damage, and prevention of lipid peroxidation by targeted scavenging of ROS produced in mitochondria has become a new therapeutic idea (Trnka et al. 2008). Such mitochondria-targeted antioxidants include Mitoquinone (MitoQ), MitoVitE (vitamin E), MitoPBN (CoQ and phenyl tert-butyl nitrone conjugate), and MitoTEMPO (SOD mimetic). When referring to antioxidant effects, it is equally appropriate to address natural and synthetic antioxidants, such as: retinol (vitamin A), ascorbic acid (vitamin C), α-tocopherol (vitamin E) and its water-soluble derivatives trolox, N-acetylcysteine (NAC), uric acid, some of the target molecules of Nrf2 (GSH, CoQ). However, the activity of these antioxidants depends on the metabolic or redox state of the cell/organism, exerting antioxidant or pro-oxidant effects (Angelova and Müller 2006, 2009) (Table 3).
Numerous studies have reported that bioactive phytochemicals can modulate ferroptosis, with flavonoids and polyphenols antagonizing ferroptosis by participating in iron metabolism and the Nrf2 pathway (Zheng et al. 2021) (Table 3). Curcumin, a natural polyphenol, is also a effective inhibitor of ferroptosis (Kajarabille and Latunde-Dada 2019), can directly inhibit lipid peroxidation (Sreejayan and Rao 1994), and has neuroprotective effects, showing promising prospects in the prevention or treatment of neurological diseases such as HD and PD (Hong et al. 2004). Resveratrol, a stilbene polyphenol derived from grape (Vitis vinifera) skin, inhibits NF-κB (Reinisalo et al. 2015) and directly inhibits lipid peroxidation by scavenging free radicals (Tadolini and Franconi 1998).The previously mentioned sulforaphane, curcumin and resveratrol can activate Nrf2 by covalently modifying Keap1 (Cores et al. 2020), which has advantages over synthetic compounds due to its minimal side effects of antioxidant and anti-inflammatory effects. Therefore, it is widely used in the treatment of many diseases (Gugliandolo et al. 2020).
In addition to electrophilic inhibitors, Keap1 inhibitors include protein–protein interaction (PPI) inhibitors (Bono et al. 2021), which competitively inhibit the protein–protein interaction between Keap1 and Nrf2 through non-electrophilic non-covalent compounds, developed to address off-target toxicity from electrophilic compounds (Robledinos-Antón et al. 2019). A typical PPI is the clinically approved Nrf2 activator, dimethyl fumarate (DMF), for the treatment of relapsing–remitting multiple sclerosis (Blair 2019), which at nanomolar concentrations modifies specific reactive cysteine (Unni et al. 2021). Studies have shown that DMF has a protective effect on neurons from neurotoxin-induced oxidative damage and is used in animal models of AD (Ahuja et al. 2016; Lastres-Becker et al. 2016). Similarly, another novel drug that activates Nrf2 by alkylating Keap1 is 4-octyl itaconate, by which it protects primary neurons against H2O2-induced cell death (Liu et al. 2018). In addition, there are other ways to activate the Nrf2 pathway. BACH1, which suppresses the transcriptional regulation of Nrf2 by competitively binding to AREs, is also a promising therapeutic target (Hushpulian et al. 2021). p62, which promotes the degradation of Keap1 (Mizunoe et al. 2018), and GSK3β, which participates in the degradation of Nrf2, may be potential therapeutic targets. As mentioned previously, activation of GSK3β has been mentioned in various NDs and several GSK3β inhibitors have entered testing in clinical trials related to AD and ALS (Choi et al. 2020). Of note, the FDA-approved non-phenolic antioxidant edaravone has been preclinically shown to increase Nrf2 levels in ALS patients (Ohta et al. 2019; Zhang et al. 2019b). In a chronic social defeat stress (CSDS) depression model mouse, edaravone mediates the silent message regulator 2 homolog 1 (Sirt1)–Nrf2–HO1–GPX4 pathway to inhibit hippocampal neuronal ferroptosis (Dang et al. 2022) (Table 3).
Outlook and prospects
Accumulating evidence links ferroptosis to ND pathology. As the disease progresses, damage to the antioxidant system, excessive OS, and altered Nrf2 expression levels, especially the inhibition of ferroptosis by lipid peroxidation inhibitors and adaptive enhancement of Nrf2 signaling, suggest that Nrf2 is essential for the detection and identification of ferroptosis and potential clinical implications of targeted therapy for neuronal loss and dysfunction.
To better understand the correlation of ferroptosis with neurodegenerative disease, the occurrence requires the combination with other biomarkers. The lack of unique biomarkers for ferroptosis hinders its assessment in ND, limiting in-depth studies of its mechanisms in neurodegeneration and therapeutic approaches targeting ferroptosis. Therefore, finding specific biomarkers of ferroptosis is still an urgent problem to be solved.
Nrf2 is widely recognized as a major therapeutic target in ND. Some natural bioactive components act as Nrf2 activators to regulate ferroptosis. Different from classical ferroptosis regulators, they have the advantages of stable structure, higher safety and less cost. Electrophilic inhibitors of Keap1 have side effects due to off-target effects, and the resulting PPI inhibitors have been extensively studied and have broad clinical potential. Other Nrf2 activators, such as GSK3β inhibitors, may have adverse side effects by affecting other signaling and metabolic pathways. Some of these Nrf2 activators are in clinical trials, such as curcumin and resveratrol.
In addition to the requirements of safety, specificity, stability and high bioavailability, high BBB permeability is a necessary condition for Nrf2 activators to enter clinical application. For this reason, DMF remains, as of now, the only drug approved by the FDA for the neurodegenerative disease (relapsing–remitting multiple sclerosis). Conjugating relevant drugs to BBB-penetrating peptides or loading them into nanoparticles or liposomes are possible development directions (Bertrand et al. 2011; Furtado et al. 2018).
The transformation of basic research results is the current challenge. It should be pointed out that the expression of Nrf2 target genes differs between neurons and glial cells (especially astrocytes), with glial cells predominating. However, the specific mechanism of the lipid peroxide-induced cell death cascade downstream of ferroptosis is still unclear, and the regulation of Nrf2-related pathways is still one of the best ways to treat ND. In summary, we focus on iron death in a neurological context, the key regulatory role of Nrf2 on iron death, and discuss that the close link between Nrf2 and ferroptosis is of clear and important significance for understanding the mechanism of ND based on OS, characterized by neuronal loss and mitochondrial dysfunction, and represented by AD, PD, HD, and ALS, and point out the bright prospect of Nrf2-targeted therapy in the diagnosis and treatment of ND.
References
Abbott NJ, Rönnbäck L, Hansson E (2006) Astrocyte-endothelial interactions at the blood–brain barrier. Nat Rev Neurosci 7:41–53. https://doi.org/10.1038/nrn1824
Abdalkader M, Lampinen R, Kanninen KM et al (2018) Targeting Nrf2 to suppress ferroptosis and mitochondrial dysfunction in neurodegeneration. Front Neurosci 12:466. https://doi.org/10.3389/fnins.2018.00466
Adedoyin O, Boddu R, Traylor A et al (2018) Heme oxygenase-1 mitigates ferroptosis in renal proximal tubule cells. Am J Physiol Renal Physiol 314:F702–F714. https://doi.org/10.1152/ajprenal.00044.2017
Agrawal S, Fox J, Thyagarajan B, Fox JH (2018) Brain mitochondrial iron accumulates in Huntington’s disease, mediates mitochondrial dysfunction, and can be removed pharmacologically. Free Radic Biol Med 120:317–329. https://doi.org/10.1016/j.freeradbiomed.2018.04.002
Ahmad MH, Fatima M, Ali M et al (2021) Naringenin alleviates paraquat-induced dopaminergic neuronal loss in SH-SY5Y cells and a rat model of Parkinson’s disease. Neuropharmacology 201:108831. https://doi.org/10.1016/j.neuropharm.2021.108831
Ahuja M, Ammal Kaidery N, Yang L et al (2016) Distinct Nrf2 signaling mechanisms of fumaric acid esters and their role in neuroprotection against 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine-induced experimental Parkinson’s-like disease. J Neurosci 36:6332–6351. https://doi.org/10.1523/JNEUROSCI.0426-16.2016
Aminzadeh-Gohari S, Weber DD, Vidali S et al (2020) From old to new—repurposing drugs to target mitochondrial energy metabolism in cancer. Semin Cell Dev Biol 98:211–223. https://doi.org/10.1016/j.semcdb.2019.05.025
Ammal Kaidery N, Ahuja M, Thomas B (2019) Crosstalk between Nrf2 signaling and mitochondrial function in Parkinson’s disease. Mol Cell Neurosci 101:103413. https://doi.org/10.1016/j.mcn.2019.103413
Anderson GJ, Frazer DM (2017) Current understanding of iron homeostasis. Am J Clin Nutr 106:1559S-1566S. https://doi.org/10.3945/ajcn.117.155804
Anderson EN, Gochenaur L, Singh A et al (2018) Traumatic injury induces stress granule formation and enhances motor dysfunctions in ALS/FTD models. Hum Mol Genet 27:1366–1381. https://doi.org/10.1093/hmg/ddy047
Andreini C, Putignano V, Rosato A, Banci L (2018) The human iron-proteome. Metallomics 10:1223–1231. https://doi.org/10.1039/c8mt00146d
Andronesi OC, Nicholson K, Jafari-Khouzani K et al (2020) Imaging neurochemistry and brain structure tracks clinical decline and mechanisms of ALS in patients. Front Neurol 11:590573. https://doi.org/10.3389/fneur.2020.590573
Angelova P, Müller W (2006) Oxidative modulation of the transient potassium current IA by intracellular arachidonic acid in rat CA1 pyramidal neurons. Eur J Neurosci 23:2375–2384. https://doi.org/10.1111/j.1460-9568.2006.04767.x
Angelova PR, Müller WS (2009) Arachidonic acid potently inhibits both postsynaptic-type Kv4.2 and presynaptic-type Kv1.4 IA potassium channels. Eur J Neurosci 29:1943–1950. https://doi.org/10.1111/j.1460-9568.2009.06737.x
Angelova PR, Esteras N, Abramov AY (2021) Mitochondria and lipid peroxidation in the mechanism of neurodegeneration: finding ways for prevention. Med Res Rev 41:770–784. https://doi.org/10.1002/med.21712
Ansari MA, Scheff SW (2010) Oxidative stress in the progression of Alzheimer disease in the frontal cortex. J Neuropathol Exp Neurol 69:155–167. https://doi.org/10.1097/nen.0b013e3181cb5af4
Aoyama K (2021) Glutathione in the brain. Int J Mol Sci 22:5010. https://doi.org/10.3390/ijms22095010
Ashraf A, Jeandriens J, Parkes HG, So P-W (2020) Iron dyshomeostasis, lipid peroxidation and perturbed expression of cystine/glutamate antiporter in Alzheimer’s disease: evidence of ferroptosis. Redox Biol 32:101494. https://doi.org/10.1016/j.redox.2020.101494
Avci B, Günaydın C, Güvenç T et al (2021) Idebenone ameliorates rotenone-induced Parkinson’s disease in rats through decreasing lipid peroxidation. Neurochem Res 46:513–522. https://doi.org/10.1007/s11064-020-03186-w
Ayala A, Muñoz MF, Argüelles S (2014) Lipid Peroxidation: production, metabolism, and signaling mechanisms of malondialdehyde and 4-hydroxy-2-nonenal. Oxid Med Cell Longev 2014:1–31. https://doi.org/10.1155/2014/360438
Ayala-Peña S (2013) Role of oxidative DNA damage in mitochondrial dysfunction and Huntington’s disease pathogenesis. Free Radic Biol Med 62:102–110. https://doi.org/10.1016/j.freeradbiomed.2013.04.017
Ayton S, Fazlollahi A, Bourgeat P et al (2017) Cerebral quantitative susceptibility mapping predicts amyloid-β-related cognitive decline. Brain 140:2112–2119. https://doi.org/10.1093/brain/awx137
Ayton S, Wang Y, Diouf I et al (2020) Brain iron is associated with accelerated cognitive decline in people with Alzheimer pathology. Mol Psychiatry 25:2932–2941. https://doi.org/10.1038/s41380-019-0375-7
Bahn G, Park J-S, Yun UJ et al (2019) NRF2/ARE pathway negatively regulates BACE1 expression and ameliorates cognitive deficits in mouse Alzheimer’s models. Proc Natl Acad Sci 116:12516–12523. https://doi.org/10.1073/pnas.1819541116
Bao W, Zhou X, Zhou L et al (2020) Targeting miR-124/Ferroportin signaling ameliorated neuronal cell death through inhibiting apoptosis and ferroptosis in aged intracerebral hemorrhage murine model. Aging Cell 19:e13235. https://doi.org/10.1111/acel.13235
Bao W-D, Pang P, Zhou X-T et al (2021) Loss of ferroportin induces memory impairment by promoting ferroptosis in Alzheimer’s disease. Cell Death Differ 28:1548–1562. https://doi.org/10.1038/s41418-020-00685-9
Baxter PS, Hardingham GE (2016) Adaptive regulation of the brain’s antioxidant defences by neurons and astrocytes. Free Radic Biol Med 100:147–152. https://doi.org/10.1016/j.freeradbiomed.2016.06.027
Beard JL, Connor JR (2003) Iron status and neural functioning. Annu Rev Nutr 23:41–58. https://doi.org/10.1146/annurev.nutr.23.020102.075739
Bedard K, Krause K-H (2007) The NOX family of ROS-generating NADPH oxidases: physiology and pathophysiology. Physiol Rev 87:245–313. https://doi.org/10.1152/physrev.00044.2005
Belaidi AA, Bush AI (2016) Iron neurochemistry in Alzheimer’s disease and Parkinson’s disease: targets for therapeutics. J Neurochem 139:179–197. https://doi.org/10.1111/jnc.13425
Belaidi AA, Gunn AP, Wong BX et al (2018) Marked age-related changes in brain iron homeostasis in amyloid protein precursor knockout mice. Neurotherapeutics 15:1055–1062. https://doi.org/10.1007/s13311-018-0656-x
Benarroch EE (2017) Nrf2, cellular redox regulation, and neurologic implications. Neurology 88:1942–1950. https://doi.org/10.1212/wnl.0000000000003946
Benarroch E (2021) What is the role of oligodendrocytes in amyotrophic lateral sclerosis? Neurology 97:776–779. https://doi.org/10.1212/wnl.0000000000012706
Benkovic SA, Connor JR (1993) Ferritin, transferrin, and iron in selected regions of the adult and aged rat brain. J Comp Neurol 338:97–113. https://doi.org/10.1002/cne.903380108
Benn CL, Sun T, Sadri-Vakili G et al (2008) Huntingtin modulates transcription, occupies gene promoters in vivo, and binds directly to DNA in a polyglutamine-dependent manner. J Neurosci 28:10720–10733. https://doi.org/10.1523/jneurosci.2126-08.2008
Berggren KL, Chen J, Fox J et al (2015) Neonatal iron supplementation potentiates oxidative stress, energetic dysfunction and neurodegeneration in the R6/2 mouse model of Huntington’s disease. Redox Biol 4:363–374. https://doi.org/10.1016/j.redox.2015.02.002
Bergström P, von Otter M, Nilsson S et al (2014) Association of NFE2L2 and KEAP1 haplotypes with amyotrophic lateral sclerosis. Amyotrophic Lat Sclerosis Frontotemp Degener 15:130–137. https://doi.org/10.3109/21678421.2013.839708
Bersuker K, Hendricks JM, Li Z et al (2019) The CoQ oxidoreductase FSP1 acts parallel to GPX4 to inhibit ferroptosis. Nature 575:688–692. https://doi.org/10.1038/s41586-019-1705-2
Bertrand Y, Currie J-C, Poirier J et al (2011) Influence of glioma tumour microenvironment on the transport of ANG1005 via low-density lipoprotein receptor-related protein 1. Br J Cancer 105:1697–1707. https://doi.org/10.1038/bjc.2011.427
Billesbølle CB, Azumaya CM, Kretsch RC et al (2020) Structure of hepcidin-bound ferroportin reveals iron homeostatic mechanisms. Nature 586:807–811. https://doi.org/10.1038/s41586-020-2668-z
Birger A, Ben-Dor I, Ottolenghi M et al (2019) Human iPSC-derived astrocytes from ALS patients with mutated C9ORF72 show increased oxidative stress and neurotoxicity. EBioMedicine 50:274–289. https://doi.org/10.1016/j.ebiom.2019.11.026
Blair HA (2019) Dimethyl fumarate: a review in relapsing-remitting MS. Drugs 79:1965–1976. https://doi.org/10.1007/s40265-019-01229-3
Blasco H, Garcon G, Patin F et al (2017) Panel of oxidative stress and inflammatory biomarkers in ALS: a pilot study. Can J Neurol Sci/j Can Des Sci Neurol 44:90–95. https://doi.org/10.1017/cjn.2016.284
Blokhuis AM, Groen EJN, Koppers M et al (2013) Protein aggregation in amyotrophic lateral sclerosis. Acta Neuropathol (berl) 125:777–794. https://doi.org/10.1007/s00401-013-1125-6
Boas SM, Joyce KL, Cowell RM (2021) The NRF2-dependent transcriptional regulation of antioxidant defense pathways: relevance for cell type-specific vulnerability to neurodegeneration and therapeutic intervention. Antioxidants 11:8. https://doi.org/10.3390/antiox11010008
Bonafede R, Mariotti R (2017) ALS pathogenesis and therapeutic approaches: the role of mesenchymal stem cells and extracellular vesicles. Front Cell Neurosci 11:80. https://doi.org/10.3389/fncel.2017.00080
Bonfio C, Valer L, Scintilla S et al (2017) UV-light-driven prebiotic synthesis of iron-sulfur clusters. Nat Chem 9:1229–1234. https://doi.org/10.1038/nchem.2817
Bono S, Feligioni M, Corbo M (2021) Impaired antioxidant KEAP1-NRF2 system in amyotrophic lateral sclerosis: NRF2 activation as a potential therapeutic strategy. Mol Neurodegener 16:71. https://doi.org/10.1186/s13024-021-00479-8
Bouvier E, Brouillard F, Molet J et al (2017) Nrf2-dependent persistent oxidative stress results in stress-induced vulnerability to depression. Mol Psychiatry 22:1701–1713. https://doi.org/10.1038/mp.2016.144
Brandes MS, Gray NE (2020) NRF2 as a therapeutic target in neurodegenerative diseases. ASN Neuro 12:1759091419899782. https://doi.org/10.1177/1759091419899782
Brites D, Vaz AR (2014) Microglia centered pathogenesis in ALS: insights in cell interconnectivity. Front Cell Neurosci 8:117. https://doi.org/10.3389/fncel.2014.00117
Brouillet E, Jacquard C, Bizat N, Blum D (2005) 3-Nitropropionic acid: a mitochondrial toxin to uncover physiopathological mechanisms underlying striatal degeneration in Huntington’s disease. J Neurochem 95:1521–1540. https://doi.org/10.1111/j.1471-4159.2005.03515.x
Brown CW, Amante JJ, Mercurio AM (2018) Cell clustering mediated by the adhesion protein PVRL4 is necessary for α6β4 integrin-promoted ferroptosis resistance in matrix-detached cells. J Biol Chem 293:12741–12748. https://doi.org/10.1074/jbc.ra118.003017
Browne SE, Beal MF (2006) Oxidative damage in Huntington’s disease pathogenesis. Antioxid Redox Signal 8:2061–2073. https://doi.org/10.1089/ars.2006.8.2061
Bu X-L, Xiang Y, Guo Y (2019) The role of iron in amyotrophic lateral sclerosis. Adv Exp Med Biol 1173:145–152. https://doi.org/10.1007/978-981-13-9589-5_8
Burdo JR, Menzies SL, Simpson IA et al (2001) Distribution of divalent metal transporter 1 and metal transport protein 1 in the normal and Belgrade rat. J Neurosci Res 66:1198–1207. https://doi.org/10.1002/jnr.1256
Burkhart A, Skjørringe T, Johnsen KB et al (2016) Expression of iron-related proteins at the neurovascular unit supports reduction and reoxidation of iron for transport through the blood–brain barrier. Mol Neurobiol 53:7237–7253. https://doi.org/10.1007/s12035-015-9582-7
Cai H, Wang Y, McCarthy D et al (2001) BACE1 is the major beta-secretase for generation of Abeta peptides by neurons. Nat Neurosci 4:233–234. https://doi.org/10.1038/85064
Cai Z, Wan C-Q, Liu Z (2017) Astrocyte and Alzheimer’s disease. J Neurol 264:2068–2074. https://doi.org/10.1007/s00415-017-8593-x
Calkins MJ, Vargas MR, Johnson DA, Johnson JA (2010) Astrocyte-specific overexpression of Nrf2 protects striatal neurons from mitochondrial complex II inhibition. Toxicol Sci 115:557–568. https://doi.org/10.1093/toxsci/kfq072
Cao JY, Dixon SJ (2016) Mechanisms of ferroptosis. Cell Mol Life Sci 73:2195–2209. https://doi.org/10.1007/s00018-016-2194-1
Cao B, Zhang Y, Chen J et al (2022) Neuroprotective effects of liraglutide against inflammation through the AMPK/NF-κB pathway in a mouse model of Parkinson’s disease. Metab Brain Dis 37:451–462. https://doi.org/10.1007/s11011-021-00879-1
Cardoso BR, Roberts BR, Bush AI, Hare DJ (2015) Selenium, selenoproteins and neurodegenerative diseases. Metallomics 7:1213–1228. https://doi.org/10.1039/c5mt00075k
Cardoso BR, Hare DJ, Lind M et al (2017) The APOE ε4 allele is associated with lower selenium levels in the brain: implications for Alzheimer’s disease. ACS Chem Neurosci 8:1459–1464. https://doi.org/10.1021/acschemneuro.7b00014
Carpenter KLH, Li W, Wei H et al (2016) Magnetic susceptibility of brain iron is associated with childhood spatial IQ. Neuroimage 132:167–174. https://doi.org/10.1016/j.neuroimage.2016.02.028
Chan JY, Kwong M (2000) Impaired expression of glutathione synthetic enzyme genes in mice with targeted deletion of the Nrf2 basic-leucine zipper protein. Biochim Biophys Acta (BBA) Gene Struct Express 1517:19–26. https://doi.org/10.1016/s0167-4781(00)00238-4
Chan A, Shea TB (2006) Dietary and genetically-induced oxidative stress alter tau phosphorylation: influence of folate and apolipoprotein E deficiency. J Alzheimers Dis 9:399–405. https://doi.org/10.3233/jad-2006-9405
Chang Y, Kong Q, Shan X et al (2008) Messenger RNA oxidation occurs early in disease pathogenesis and promotes motor neuron degeneration in ALS. PLoS ONE 3:e2849. https://doi.org/10.1371/journal.pone.0002849
Chang L-C, Chiang S-K, Chen S-E et al (2018) Heme oxygenase-1 mediates BAY 11–7085 induced ferroptosis. Cancer Lett 416:124–137. https://doi.org/10.1016/j.canlet.2017.12.025
Chaturvedi RK, Calingasan NY, Yang L et al (2010) Impairment of PGC-1alpha expression, neuropathology and hepatic steatosis in a transgenic mouse model of huntington’s disease following chronic energy deprivation. Hum Mol Genet 19:3190–3205. https://doi.org/10.1093/hmg/ddq229
Cheepsunthorn P, Palmer C, Connor JR (1998) Cellular distribution of ferritin subunits in postnatal rat brain. J Comp Neurol 400:73–86
Cheignon C, Tomas M, Bonnefont-Rousselot D et al (2018) Oxidative stress and the amyloid beta peptide in Alzheimer’s disease. Redox Biol 14:450–464. https://doi.org/10.1016/j.redox.2017.10.014
Chen C-M, Wu Y-R, Cheng M-L et al (2007) Increased oxidative damage and mitochondrial abnormalities in the peripheral blood of Huntington’s disease patients. Biochem Biophys Res Commun 359:335–340. https://doi.org/10.1016/j.bbrc.2007.05.093
Chen J, Marks E, Lai B et al (2013) Iron accumulates in Huntington’s disease neurons: protection by deferoxamine. PLoS ONE 8:e77023. https://doi.org/10.1371/journal.pone.0077023
Chen Z, Jiang R, Chen M et al (2019) Multi-copper ferroxidase deficiency leads to iron accumulation and oxidative damage in astrocytes and oligodendrocytes. Sci Rep 9:9437. https://doi.org/10.1038/s41598-019-46019-9
Chen X, Yu C, Kang R, Tang D (2020) Iron metabolism in ferroptosis. Front Cell Dev Biol. https://doi.org/10.3389/fcell.2020.590226
Chen X, Comish PB, Tang D, Kang R (2021) Characteristics and Biomarkers of Ferroptosis. Front Cell Dev Biol 9:637162. https://doi.org/10.3389/fcell.2021.637162
Cheng H, Wang P, Wang N et al (2023) Neuroprotection of NRF2 against ferroptosis after traumatic brain injury in mice. Antioxidants 12:731. https://doi.org/10.3390/antiox12030731
Chi L, Ke Y, Luo C et al (2007) Depletion of reduced glutathione enhances motor neuron degeneration in vitro and in vivo. Neuroscience 144:991–1003. https://doi.org/10.1016/j.neuroscience.2006.09.064
Chinta SJ, Andersen JK (2008) Redox imbalance in Parkinson’s disease. Biochim Biophys Acta (BBA) General Subj 1780:1362–1367. https://doi.org/10.1016/j.bbagen.2008.02.005
Chiò A, Logroscino G, Traynor BJ et al (2013) Global epidemiology of amyotrophic lateral sclerosis: a systematic review of the published literature. Neuroepidemiology 41:118–130. https://doi.org/10.1159/000351153
Choi IY, Lee P, Statland J et al (2015) Reduction in cerebral antioxidant, glutathione (GSH), in patients with ALS: A preliminary study (P6.105). Neurology 84:1
Choi H-J, Cha SJ, Lee J-W et al (2020) Recent advances on the role of GSK3β in the pathogenesis of amyotrophic lateral sclerosis. Brain Sci 10:675. https://doi.org/10.3390/brainsci10100675
Choo YS (2004) Mutant huntingtin directly increases susceptibility of mitochondria to the calcium-induced permeability transition and cytochrome c release. Hum Mol Genet 13:1407–1420. https://doi.org/10.1093/hmg/ddh162
Chou C-C, Zhang Y, Umoh ME et al (2018) TDP-43 pathology disrupts nuclear pore complexes and nucleocytoplasmic transport in ALS/FTD. Nat Neurosci 21:228–239. https://doi.org/10.1038/s41593-017-0047-3
Chowdhry S, Zhang Y, McMahon M et al (2013) Nrf2 is controlled by two distinct β-TrCP recognition motifs in its Neh6 domain, one of which can be modulated by GSK-3 activity. Oncogene 32:3765–3781. https://doi.org/10.1038/onc.2012.388
Chu B, Kon N, Chen D et al (2019) ALOX12 is required for p53-mediated tumour suppression through a distinct ferroptosis pathway. Nat Cell Biol 21:579–591. https://doi.org/10.1038/s41556-019-0305-6
Coby AJ, Picardal F, Shelobolina E et al (2011) Repeated anaerobic microbial redox cycling of iron. Appl Environ Microbiol 77:6036–6042. https://doi.org/10.1128/aem.00276-11
Codazzi F, Pelizzoni I, Zacchetti D, Grohovaz F (2015) Iron entry in neurons and astrocytes: a link with synaptic activity. Front Mol Neurosci 8:18. https://doi.org/10.3389/fnmol.2015.00018
Connor JR, Snyder BS, Beard JL et al (1992) Regional distribution of iron and iron-regulatory proteins in the brain in aging and Alzheimer’s disease. J Neurosci Res 31:327–335. https://doi.org/10.1002/jnr.490310214
Connor JR, Pavlick G, Karli D et al (1995) A histochemical study of iron-positive cells in the developing rat brain. J Comp Neurol 355:111–123. https://doi.org/10.1002/cne.903550112
Connor JR, Ponnuru P, Wang X-S et al (2011) Profile of altered brain iron acquisition in restless legs syndrome. Brain 134:959–968. https://doi.org/10.1093/brain/awr012
Cooper J (1998) Truncated N-terminal fragments of huntingtin with expanded glutamine repeats form nuclear and cytoplasmic aggregates in cell culture. Hum Mol Genet 7:783–790. https://doi.org/10.1093/hmg/7.5.783
Cores Á, Piquero M, Villacampa M et al (2020) NRF2 regulation processes as a source of potential drug targets against neurodegenerative diseases. Biomolecules 10:904. https://doi.org/10.3390/biom10060904
Cortes CJ, La Spada AR (2014) The many faces of autophagy dysfunction in Huntington’s disease: from mechanism to therapy. Drug Discovery Today 19:963–971. https://doi.org/10.1016/j.drudis.2014.02.014
Coxhead J, Kurzawa-Akanbi M, Hussain R et al (2016) Somatic mtDNA variation is an important component of Parkinson’s disease. Neurobiol Aging 38:217.e1-217.e6. https://doi.org/10.1016/j.neurobiolaging.2015.10.036
Craighead JE (1995) Pathology of environmental and occupational diseases. Mosby, London
Crielaard BJ, Lammers T, Rivella S (2017) Targeting iron metabolism in drug discovery and delivery. Nat Rev Drug Disc 16:400–423. https://doi.org/10.1038/nrd.2016.248
Crowe A, Morgan EH (1992) Iron and transferrin uptake by brain and cerebrospinal fluid in the rat. Brain Res 592:8–16. https://doi.org/10.1016/0006-8993(92)91652-u
Cuadrado A (2015) Structural and functional characterization of Nrf2 degradation by glycogen synthase kinase 3/β-TrCP. Free Radic Biol Med 88:147–157. https://doi.org/10.1016/j.freeradbiomed.2015.04.029
Cuadrado A, Kügler S, Lastres-Becker I (2018) Pharmacological targeting of GSK-3 and NRF2 provides neuroprotection in a preclinical model of tauopathy. Redox Biol 14:522–534. https://doi.org/10.1016/j.redox.2017.10.010
Cui Z, Zhong Z, Yang Y et al (2016) Ferrous iron induces Nrf2 expression in mouse brain astrocytes to prevent neurotoxicity. J Biochem Mol Toxicol 30:396–403. https://doi.org/10.1002/jbt.21803
Cullinan SB, Gordan JD, Jin J et al (2004) The Keap1-BTB protein is an adaptor that bridges Nrf2 to a Cul3-based E3 ligase: oxidative stress sensing by a Cul3-Keap1 ligase. Mol Cell Biol 24:8477–8486. https://doi.org/10.1128/mcb.24.19.8477-8486.2004
Dai E, Han L, Liu J et al (2020a) Ferroptotic damage promotes pancreatic tumorigenesis through a TMEM173/STING-dependent DNA sensor pathway. Nat Commun 11:6339. https://doi.org/10.1038/s41467-020-20154-8
Dai E, Zhang W, Cong D et al (2020b) AIFM2 blocks ferroptosis independent of ubiquinol metabolism. Biochem Biophys Res Commun 523:966–971. https://doi.org/10.1016/j.bbrc.2020.01.066
Damiano M, Galvan L, Déglon N, Brouillet E (2010) Mitochondria in Huntington’s disease. Biochim Biophys Acta (BBA) Mol Basis Dis 1802:52–61. https://doi.org/10.1016/j.bbadis.2009.07.012
Dang R, Wang M, Li X et al (2022) Edaravone ameliorates depressive and anxiety-like behaviors via Sirt1/Nrf2/HO-1/Gpx4 pathway. J Neuroinflamm 19:41. https://doi.org/10.1186/s12974-022-02400-6
Dantas LS, Viviani LG, Inague A et al (2020) Lipid aldehyde hydrophobicity affects apo-SOD1 modification and aggregation. Free Radical Biol Med 156:157–167. https://doi.org/10.1016/j.freeradbiomed.2020.05.011
De Domenico I, McVey Ward D, Kaplan J (2008) Regulation of iron acquisition and storage: consequences for iron-linked disorders. Nat Rev Mol Cell Biol 9:72–81. https://doi.org/10.1038/nrm2295
DeJesus-Hernandez M, Mackenzie IR, Boeve BF et al (2011) Expanded GGGGCC hexanucleotide repeat in noncoding region of C9ORF72 causes chromosome 9p-linked FTD and ALS. Neuron 72:245–256. https://doi.org/10.1016/j.neuron.2011.09.011
Demuynck R, Efimova I, Naessens F, Krysko DV (2021) Immunogenic ferroptosis and where to find it? J Immunother Cancer 9:e003430. https://doi.org/10.1136/jitc-2021-003430
Descamps L, Dehouck MP, Torpier G, Cecchelli R (1996) Receptor-mediated transcytosis of transferrin through blood–brain barrier endothelial cells. Am J Physiol Heart Circul Physiol 270:H1149–H1158. https://doi.org/10.1152/ajpheart.1996.270.4.h1149
Devos D, Moreau C, Kyheng M et al (2019) A ferroptosis-based panel of prognostic biomarkers for Amyotrophic Lateral Sclerosis. Sci Rep 9:2918. https://doi.org/10.1038/s41598-019-39739-5
Devos D, Devos D, Cabantchik ZI et al (2020) Conservative iron chelation for neurodegenerative diseases such as Parkinson’s disease and amyotrophic lateral sclerosis. J Neural Transm 127:189–203. https://doi.org/10.1007/s00702-019-02138-1
Dexter DT, Wells FR, Lee AJ et al (1989) Increased nigral iron content and alterations in other metal ions occurring in brain in Parkinson’s disease. J Neurochem 52:1830–1836. https://doi.org/10.1111/j.1471-4159.1989.tb07264.x
Dhakshinamoorthy S, Jain AK, Bloom DA, Jaiswal AK (2005) Bach1 competes with Nrf2 leading to negative regulation of the antioxidant response element (ARE)-mediated NAD(P)H:quinone oxidoreductase 1 gene expression and induction in response to antioxidants. J Biol Chem 280:16891–16900. https://doi.org/10.1074/jbc.m500166200
Di Domenico F, Pupo G, Mancuso C et al (2015) Bach1 overexpression in Down syndrome correlates with the alteration of the HO-1/BVR-a system: insights for transition to Alzheimer’s disease. J Alzheimers Dis 44:1107–1120. https://doi.org/10.3233/jad-141254
Di Meo S, Reed TT, Venditti P, Victor VM (2016) Role of ROS and RNS sources in physiological and pathological conditions. Oxid Med Cell Longev 2016:1–44. https://doi.org/10.1155/2016/1245049
DiFiglia M, Sapp E, Chase KO et al (1997) Aggregation of huntingtin in neuronal intranuclear inclusions and dystrophic neurites in brain. Science 277:1990–1993. https://doi.org/10.1126/science.277.5334.1990
Dinkova-Kostova AT, Holtzclaw WD, Cole RN et al (2002) Direct evidence that sulfhydryl groups of Keap1 are the sensors regulating induction of phase 2 enzymes that protect against carcinogens and oxidants. Proc Natl Acad Sci 99:11908–11913. https://doi.org/10.1073/pnas.172398899
Dinkova-Kostova AT, Kostov RV, Canning P (2017) Keap1, the cysteine-based mammalian intracellular sensor for electrophiles and oxidants. Arch Biochem Biophys 617:84–93. https://doi.org/10.1016/j.abb.2016.08.005
Dixon SJ, Lemberg KM, Lamprecht MR et al (2012) Ferroptosis: an iron-dependent form of nonapoptotic cell death. Cell 149:1060–1072. https://doi.org/10.1016/j.cell.2012.03.042
Dixon SJ, Patel DN, Welsch M et al (2014) Pharmacological inhibition of cystine-glutamate exchange induces endoplasmic reticulum stress and ferroptosis. Elife 3:e02523. https://doi.org/10.7554/elife.02523
Dodson M, Castro-Portuguez R, Zhang DD (2019a) NRF2 plays a critical role in mitigating lipid peroxidation and ferroptosis. Redox Biol 23:101107. https://doi.org/10.1016/j.redox.2019.101107
Dodson M, de la Vega MR, Cholanians AB et al (2019b) Modulating NRF2 in disease: timing is everything. Annu Rev Pharmacol Toxicol 59:555–575. https://doi.org/10.1146/annurev-pharmtox-010818-021856
Doll S, Proneth B, Tyurina YY et al (2017) ACSL4 dictates ferroptosis sensitivity by shaping cellular lipid composition. Nat Chem Biol 13:91–98. https://doi.org/10.1038/nchembio.2239
Doll S, Freitas FP, Shah R et al (2019) FSP1 is a glutathione-independent ferroptosis suppressor. Nature 575:693–698. https://doi.org/10.1038/s41586-019-1707-0
Dong H, Zhang J, Rong H et al (2021) Paeoniflorin and plycyrrhetinic acid synergistically alleviate MPP+/MPTP-induced oxidative stress through Nrf2-dependent glutathione biosynthesis mechanisms. ACS Chem Neurosci 12:1100–1111. https://doi.org/10.1021/acschemneuro.0c00544
Dong X, Tan Y, Zhuang D et al (2022) Global characteristics and trends in research on ferroptosis: a data-driven bibliometric study. Oxid Med Cell Longev 2022:1–12. https://doi.org/10.1155/2022/8661864
Dowling RJO, Topisirovic I, Fonseca BD, Sonenberg N (2010) Dissecting the role of mTOR: lessons from mTOR inhibitors. Biochim Biophys Acta (BBA) Prot Proteom 1804:433–439. https://doi.org/10.1016/j.bbapap.2009.12.001
Drakesmith H, Nemeth E, Ganz T (2015) Ironing out ferroportin. Cell Metab 22:777–787. https://doi.org/10.1016/j.cmet.2015.09.006
Du Y, Wooten MC, Wooten MW (2009) Oxidative damage to the promoter region of SQSTM1/p62 is common to neurodegenerative disease. Neurobiol Dis 35:302–310. https://doi.org/10.1016/j.nbd.2009.05.015
Dugger BN, Dickson DW (2017) Pathology of neurodegenerative diseases. Csh Perspect Biol 9:a028035. https://doi.org/10.1101/cshperspect.a028035
Dusek P, Hofer T, Alexander J et al (2022) Cerebral iron deposition in neurodegeneration. Biomolecules 12:714. https://doi.org/10.3390/biom12050714
Elfawy HA, Das B (2019) Crosstalk between mitochondrial dysfunction, oxidative stress, and age related neurodegenerative disease: etiologies and therapeutic strategies. Life Sci 218:165–184. https://doi.org/10.1016/j.lfs.2018.12.029
Elharram A, Czegledy NM, Golod M et al (2017) Deuterium-reinforced polyunsaturated fatty acids improve cognition in a mouse model of sporadic Alzheimer’s disease. Febs J 284:4083–4095. https://doi.org/10.1111/febs.14291
Ernster L (1967) [56] DT diaphorase. In: Methods in enzymology. Elsevier, London, pp 309–317
Faghihi MA, Modarresi F, Khalil AM et al (2008) Expression of a noncoding RNA is elevated in Alzheimer’s disease and drives rapid feed-forward regulation of beta-secretase. Nat Med 14:723–730. https://doi.org/10.1038/nm1784
Fang X, Zhang J, Li Y et al (1970) Malic enzyme 1 as a novel anti-ferroptotic regulator in hepatic ischemia/reperfusion injury. Adv Sci. https://doi.org/10.1002/advs.202205436
Fão L, Mota SI, Rego AC (2019) Shaping the Nrf2-ARE-related pathways in Alzheimer’s and Parkinson’s diseases. Ageing Res Rev 54:100942. https://doi.org/10.1016/j.arr.2019.100942
Feng H, Stockwell BR (2018) Unsolved mysteries: How does lipid peroxidation cause ferroptosis? Plos Biol 16:e2006203. https://doi.org/10.1371/journal.pbio.2006203
Feng H, Schorpp K, Jin J et al (2020) Transferrin receptor is a specific ferroptosis marker. Cell Rep 30:3411-3423.e7. https://doi.org/10.1016/j.celrep.2020.02.049
Ferguson MW, Kennedy CJ, Palpagama TH et al (2022) Current and possible future therapeutic options for Huntington’s disease. J Central Nervous Syst Dis 14:117957352210925. https://doi.org/10.1177/11795735221092517
Ferraiuolo L, Kirby J, Grierson AJ et al (2011) Molecular pathways of motor neuron injury in amyotrophic lateral sclerosis. Nat Rev Neurol 7:616–630. https://doi.org/10.1038/nrneurol.2011.152
Ferrante RJ, Shinobu LA, Schulz JB et al (1997) Increased 3-nitrotyrosine and oxidative damage in mice with a human copper/zinc superoxide dismutase mutation. Ann Neurol 42:326–334. https://doi.org/10.1002/ana.410420309
Ferrari Bardile C, Garcia-Miralles M, Caron NS et al (2019) Intrinsic mutant HTT-mediated defects in oligodendroglia cause myelination deficits and behavioral abnormalities in Huntington disease. Proc Natl Acad Sci USA 116:9622–9627. https://doi.org/10.1073/pnas.1818042116
Forcina GC, Dixon SJ (2019) GPX4 at the crossroads of lipid homeostasis and ferroptosis. Proteomics 19:1800311. https://doi.org/10.1002/pmic.201800311
Foster AD, Downing P, Figredo E et al (2020) ALS-associated TBK1 variant p.G175S is defective in phosphorylation of p62 and impacts TBK1-mediated signalling and TDP-43 autophagic degradation. Mol Cell Neurosci 108:103539. https://doi.org/10.1016/j.mcn.2020.103539
Friedmann Angeli JP, Schneider M, Proneth B et al (2014) Inactivation of the ferroptosis regulator Gpx4 triggers acute renal failure in mice. Nat Cell Biol 16:1180–1191. https://doi.org/10.1038/ncb3064
Fu J, Xiong Z, Huang C et al (2019) Hyperactivity of the transcription factor Nrf2 causes metabolic reprogramming in mouse esophagus. J Biol Chem 294:327–340. https://doi.org/10.1074/jbc.ra118.005963
Furtado D, Björnmalm M, Ayton S et al (2018) Overcoming the blood–brain barrier: the role of nanomaterials in treating neurological diseases. Adv Mater 30:1801362. https://doi.org/10.1002/adma.201801362
Gallucci M, Limbucci N, Catalucci A, Caulo M (2008) Neurodegenerative diseases. Radiol Clin North Am 46:799–817. https://doi.org/10.1016/j.rcl.2008.06.002
Ganz T (2013) Systemic iron homeostasis. Physiol Rev 93:1721–1741. https://doi.org/10.1152/physrev.00008.2013
Gao H-M, Hong J-S, Zhang W, Liu B (2002) Distinct role for microglia in rotenone-induced degeneration of dopaminergic neurons. J Neurosci 22:782–790. https://doi.org/10.1523/jneurosci.22-03-00782.2002
Gao Y, Li J, Wu Q et al (2021) Tetrahydroxy stilbene glycoside ameliorates Alzheimer’s disease in APP/PS1 mice via glutathione peroxidase related ferroptosis. Int Immunopharmacol 99:108002. https://doi.org/10.1016/j.intimp.2021.108002
Gauthier LR, Charrin BC, Borrell-Pagès M et al (2004) Huntingtin controls neurotrophic support and survival of neurons by enhancing BDNF vesicular transport along microtubules. Cell 118:127–138. https://doi.org/10.1016/j.cell.2004.06.018
Geisler S, Holmström KM, Skujat D et al (2010) PINK1/Parkin-mediated mitophagy is dependent on VDAC1 and p62/SQSTM1. Nat Cell Biol 12:119–131. https://doi.org/10.1038/ncb2012
George M, Tharakan M, Culberson J et al (2022) Role of Nrf2 in aging, Alzheimer’s and other neurodegenerative diseases. Ageing Res Rev 82:101756. https://doi.org/10.1016/j.arr.2022.101756
Giometto B, Bozza F, Argentiero V et al (1990) Transferrin receptors in rat central nervous system. An immunocytochemical study. J Neurol Sci 98:81–90. https://doi.org/10.1016/0022-510x(90)90183-n
Goebel HH, Heipertz R, Scholz W et al (1978) Juvenile Huntington chorea: clinical, ultrastructural, and biochemical studies. Neurology 28:23–23. https://doi.org/10.1212/wnl.28.1.23
Goodman L (1953) Alzheimer’s disease; a clinico-pathologic analysis of twenty-three cases with a theory on pathogenesis. J Nerv Ment Dis 118:97–130
Goswami A, Dikshit P, Mishra A et al (2006) Oxidative stress promotes mutant huntingtin aggregation and mutant huntingtin-dependent cell death by mimicking proteasomal malfunction. Biochem Biophys Res Commun 342:184–190. https://doi.org/10.1016/j.bbrc.2006.01.136
Greenough MA (2016) The role of presenilin in protein trafficking and degradation-implications for metal homeostasis. J Mol Neurosci 60:289–297. https://doi.org/10.1007/s12031-016-0826-4
Guemez-Gamboa A, Estrada-Sánchez AM, Montiel T et al (2011) Activation of NOX2 by the stimulation of ionotropic and metabotropic glutamate receptors contributes to glutamate neurotoxicity in vivo through the production of reactive oxygen species and calpain activation. J Neuropathol Exp Neurol 70:1020–1035. https://doi.org/10.1097/NEN.0b013e3182358e4e
Gugliandolo A, Bramanti P, Mazzon E (2020) Activation of Nrf2 by natural bioactive compounds: A promising approach for stroke? Int J Mol Sci 21:4875. https://doi.org/10.3390/ijms21144875
Guillemot J, Canuel M, Essalmani R et al (2013) Implication of the proprotein convertases in iron homeostasis: proprotein convertase 7 sheds human transferrin receptor 1 and furin activates hepcidin. Hepatology 57:2514–2524. https://doi.org/10.1002/hep.26297
Gunnarsson L-G, Bodin L (2019) Occupational exposures and neurodegenerative diseases—a systematic literature review and meta-analyses. Int J Environ Res Public Health 16:337. https://doi.org/10.3390/ijerph16030337
Guo C, Wang P, Zhong M-L et al (2013a) Deferoxamine inhibits iron induced hippocampal tau phosphorylation in the Alzheimer transgenic mouse brain. Neurochem Int 62:165–172. https://doi.org/10.1016/j.neuint.2012.12.005
Guo Y, Zhang Y, Wen D et al (2013b) The modest impact of transcription factor Nrf2 on the course of disease in an ALS animal model. Lab Invest 93:825–833. https://doi.org/10.1038/labinvest.2013.73
Guo R, Zong S, Wu M et al (2017) Architecture of human mitochondrial respiratory megacomplex I2III2IV2. Cell 170:1247-1257.e12. https://doi.org/10.1016/j.cell.2017.07.050
Ha C, Ryu J, Park CB (2007) Metal ions differentially influence the aggregation and deposition of Alzheimer’s beta-amyloid on a solid template. Biochemistry 46:6118–6125. https://doi.org/10.1021/bi7000032
Habas A, Hahn J, Wang X, Margeta M (2013) Neuronal activity regulates astrocytic Nrf2 signaling. Proc Natl Acad Sci 110:18291–18296. https://doi.org/10.1073/pnas.1208764110
Habib E, Linher-Melville K, Lin H-X, Singh G (2015) Expression of xCT and activity of system xc(-) are regulated by NRF2 in human breast cancer cells in response to oxidative stress. Redox Biol 5:33–42. https://doi.org/10.1016/j.redox.2015.03.003
Hadano S, Mitsui S, Pan L et al (2016) Functional links between SQSTM1 and ALS2 in the pathogenesis of ALS: cumulative impact on the protection against mutant SOD1-mediated motor dysfunction in mice. Hum Mol Genet 25:3321–3340. https://doi.org/10.1093/hmg/ddw180
Haidet-Phillips AM, Hester ME, Miranda CJ et al (2011) Astrocytes from familial and sporadic ALS patients are toxic to motor neurons. Nat Biotechnol 29:824–828. https://doi.org/10.1038/nbt.1957
Han K, Jin X, Guo X et al (2021) Nrf2 knockout altered brain iron deposition and mitigated age-related motor dysfunction in aging mice. Free Radic Biol Med 162:592–602. https://doi.org/10.1016/j.freeradbiomed.2020.11.019
Hancock R, Bertrand HC, Tsujita T et al (2012) Peptide inhibitors of the Keap1-Nrf2 protein-protein interaction. Free Radic Biol Med 52:444–451. https://doi.org/10.1016/j.freeradbiomed.2011.10.486
Hashimoto K, Simmons AN, Kajino-Sakamoto R et al (2016) TAK1 regulates the Nrf2 antioxidant system through modulating p62/SQSTM1. Antioxid Redox Signal 25:953–964. https://doi.org/10.1089/ars.2016.6663
Hastings TG (2009) The role of dopamine oxidation in mitochondrial dysfunction: implications for Parkinson’s disease. J Bioenerg Biomembr 41:469–472. https://doi.org/10.1007/s10863-009-9257-z
Hatami A, Zhu C, Relaño-Gines A et al (2018) Deuterium-reinforced linoleic acid lowers lipid peroxidation and mitigates cognitive impairment in the Q140 knock in mouse model of Huntington’s disease. Febs J 285:3002–3012. https://doi.org/10.1111/febs.14590
Hayes JD, Dinkova-Kostova AT (2014) The Nrf2 regulatory network provides an interface between redox and intermediary metabolism. Trends Biochem Sci 39:199–218. https://doi.org/10.1016/j.tibs.2014.02.002
He Q, Song N, Jia F et al (2013) Role of α-synuclein aggregation and the nuclear factor E2-related factor 2/heme oxygenase-1 pathway in iron-induced neurotoxicity. Int J Biochem Cell Biol 45:1019–1030. https://doi.org/10.1016/j.biocel.2013.02.012
He F, Ru X, Wen T (2020) NRF2, a transcription factor for stress response and beyond. Int J Mol Sci 21:4777. https://doi.org/10.3390/ijms21134777
Hensman Moss DJ, Flower MD, Lo KK et al (2017) Huntington’s disease blood and brain show a common gene expression pattern and share an immune signature with Alzheimer’s disease. Sci Rep 7:44849. https://doi.org/10.1038/srep44849
Hinman A, Holst CR, Latham JC et al (2018) Vitamin E hydroquinone is an endogenous regulator of ferroptosis via redox control of 15-lipoxygenase. PLoS ONE 13:e0201369. https://doi.org/10.1371/journal.pone.0201369
Hirotsu Y, Katsuoka F, Funayama R et al (2012) Nrf2-MafG heterodimers contribute globally to antioxidant and metabolic networks. Nucleic Acids Res 40:10228–10239. https://doi.org/10.1093/nar/gks827
Hoffner G, Island M-L, Djian P (2005) Purification of neuronal inclusions of patients with Huntington’s disease reveals a broad range of N-terminal fragments of expanded huntingtin and insoluble polymers. J Neurochem 95:125–136. https://doi.org/10.1111/j.1471-4159.2005.03348.x
Hohnholt MC, Dringen R (2013) Uptake and metabolism of iron and iron oxide nanoparticles in brain astrocytes. Biochem Soc Trans 41:1588–1592. https://doi.org/10.1042/bst20130114
Holland R, Hawkins AE, Eggler AL et al (2008) Prospective type 1 and type 2 disulfides of Keap1 protein. Chem Res Toxicol 21:2051–2060. https://doi.org/10.1021/tx800226m
Holland R, McIntosh AL, Finucane OM et al (2018) Inflammatory microglia are glycolytic and iron retentive and typify the microglia in APP/PS1 mice. Brain Behav Immun 68:183–196. https://doi.org/10.1016/j.bbi.2017.10.017
Hong J, Bose M, Ju J et al (2004) Modulation of arachidonic acid metabolism by curcumin and related beta-diketone derivatives: effects on cytosolic phospholipase A(2), cyclooxygenases and 5-lipoxygenase. Carcinogenesis 25:1671–1679. https://doi.org/10.1093/carcin/bgh165
Hong F, Sekhar KR, Freeman ML, Liebler DC (2005) Specific patterns of electrophile adduction trigger Keap1 ubiquitination and Nrf2 activation. J Biol Chem 280:31768–31775. https://doi.org/10.1074/jbc.m503346200
Hooper C, Killick R, Lovestone S (2008) The GSK3 hypothesis of Alzheimer’s disease. J Neurochem 104:1433–1439. https://doi.org/10.1111/j.1471-4159.2007.05194.x
Hosoda S, Nakamura W, Hayashi K (1974) Properties and reaction mechanism of DT diaphorase from rat liver. J Biol Chem 249:6416–6423
Hou W, Xie Y, Song X et al (2016) Autophagy promotes ferroptosis by degradation of ferritin. Autophagy 12:1425–1428. https://doi.org/10.1080/15548627.2016.1187366
Hou Y, Dan X, Babbar M et al (2019) Ageing as a risk factor for neurodegenerative disease. Nat Rev Neurol 15:565–581. https://doi.org/10.1038/s41582-019-0244-7
Huang E, Ong WY, Connor JR (2004) Distribution of divalent metal transporter-1 in the monkey basal ganglia. Neuroscience 128:487–496. https://doi.org/10.1016/j.neuroscience.2004.06.055
Huang E, Ong W-Y, Go M-L, Connor JR (2006) Upregulation of iron regulatory proteins and divalent metal transporter-1 isoforms in the rat hippocampus after kainate induced neuronal injury. Exp Brain Res 170:376–386. https://doi.org/10.1007/s00221-005-0220-x
Huang J, Tabbi-Anneni I, Gunda V, Wang L (2010) Transcription factor Nrf2 regulates SHP and lipogenic gene expression in hepatic lipid metabolism. Am J Physiol Gastrointestinal Liver Physiol 299:G1211–G1221. https://doi.org/10.1152/ajpgi.00322.2010
Huang Y, Wang Y, Gao Y et al (2020) BDNF and its multirole function in neurogenesis, synaptic transmission and neurodegenerative diseases. Nano LIFE 10:2040007. https://doi.org/10.1142/s1793984420400073
Hunot S, Brugg B, Ricard D et al (1997) Nuclear translocation of NF-κB is increased in dopaminergic neurons of patients with Parkinson disease. Proc Natl Acad Sci 94:7531–7536. https://doi.org/10.1073/pnas.94.14.7531
Hushpulian DM, Ammal Kaidery N, Ahuja M et al (2021) Challenges and limitations of targeting the keap1-Nrf2 pathway for neurotherapeutics: bach1 de-repression to the rescue. Front Aging Neurosci 13:673205. https://doi.org/10.3389/fnagi.2021.673205
Hustad E, Aasly JO (2020) Clinical and imaging markers of prodromal Parkinson’s disease. Front Neurol 11:395. https://doi.org/10.3389/fneur.2020.00395
Ibrahim WW, Abdel Rasheed NO (2022) Diapocynin neuroprotective effects in 3-nitropropionic acid Huntington’s disease model in rats: emphasis on Sirt1/Nrf2 signaling pathway. Inflammopharmacol 30:1745–1758. https://doi.org/10.1007/s10787-022-01004-z
Ichimura Y, Waguri S, Sou Y-S et al (2013) Phosphorylation of p62 activates the Keap1-Nrf2 pathway during selective autophagy. Mol Cell 51:618–631. https://doi.org/10.1016/j.molcel.2013.08.003
Igarashi K, Kataokat K, Itoh K et al (1994) Regulation of transcription by dimerization of erythroid factor NF-E2 p45 with small Maf proteins. Nature 367:568–572. https://doi.org/10.1038/367568a0
Ikram M, Saeed K, Khan A et al (2019) Natural dietary supplementation of curcumin protects mice brains against ethanol-induced oxidative stress-mediated neurodegeneration and memory impairment via Nrf2/TLR4/RAGE signaling. Nutrients 11:1082. https://doi.org/10.3390/nu11051082
Inose Y, Izumi Y, Takada-Takatori Y et al (2020) Protective effects of Nrf2-ARE activator on dopaminergic neuronal loss in Parkinson disease model mice: possible involvement of heme oxygenase-1. Neurosci Lett 736:135268. https://doi.org/10.1016/j.neulet.2020.135268
Ishii T, Itoh K, Takahashi S et al (2000) Transcription factor Nrf2 coordinately regulates a group of oxidative stress-inducible genes in macrophages. J Biol Chem 275:16023–16029. https://doi.org/10.1074/jbc.275.21.16023
Isobe C, Abe T, Terayama Y (2010) Levels of reduced and oxidized coenzyme Q-10 and 8-hydroxy-2′-deoxyguanosine in the cerebrospinal fluid of patients with living Parkinson’s disease demonstrate that mitochondrial oxidative damage and/or oxidative DNA damage contributes to the neurodegenerative process. Neurosci Lett 469:159–163. https://doi.org/10.1016/j.neulet.2009.11.065
Itoh K, Wakabayashi N, Katoh Y et al (1999) Keap1 represses nuclear activation of antioxidant responsive elements by Nrf2 through binding to the amino-terminal Neh2 domain. Genes Dev 13:76–86. https://doi.org/10.1101/gad.13.1.76
Iwata-Ichikawa E, Kondo Y, Miyazaki I et al (2002) Glial cells protect neurons against oxidative stress via transcriptional up-regulation of the glutathione synthesis. J Neurochem 72:2334–2344. https://doi.org/10.1046/j.1471-4159.1999.0722334.x
Izrael M, Slutsky SG, Revel M (2020) Rising stars: astrocytes as a therapeutic target for ALS disease. Front Neurosci 14:824. https://doi.org/10.3389/fnins.2020.00824
Jaganjac M, Milkovic L, Gegotek A et al (2020) The relevance of pathophysiological alterations in redox signaling of 4-hydroxynonenal for pharmacological therapies of major stress-associated diseases. Free Radic Biol Med 157:128–153. https://doi.org/10.1016/j.freeradbiomed.2019.11.023
Jain AK, Jaiswal AK (2007) GSK-3beta acts upstream of Fyn kinase in regulation of nuclear export and degradation of NF-E2 related factor 2. J Biol Chem 282:16502–16510. https://doi.org/10.1074/jbc.M611336200
Jain A, Lamark T, Sjøttem E et al (2010) p62/SQSTM1 is a target gene for transcription factor NRF2 and creates a positive feedback loop by inducing antioxidant response element-driven gene transcription. J Biol Chem 285:22576–22591. https://doi.org/10.1074/jbc.m110.118976
Jannat S, Balupuri A, Ali MY et al (2019) Inhibition of β-site amyloid precursor protein cleaving enzyme 1 and cholinesterases by pterosins via a specific structure−activity relationship with a strong BBB permeability. Exp Mol Med 51:1–18. https://doi.org/10.1038/s12276-019-0205-7
Jazwa A, Cuadrado A (2010) Targeting heme oxygenase-1 for neuroprotection and neuroinflammation in neurodegenerative diseases. Curr Drug Targets 11:1517–1531. https://doi.org/10.2174/1389450111009011517
Jelinek A, Heyder L, Daude M et al (2018) Mitochondrial rescue prevents glutathione peroxidase-dependent ferroptosis. Free Radic Biol Med 117:45–57. https://doi.org/10.1016/j.freeradbiomed.2018.01.019
Jenner P, Olanow CW (2006) The pathogenesis of cell death in Parkinson’s disease. Neurology 66:S24–S36. https://doi.org/10.1212/wnl.66.10_suppl_4.s24
Jeong SY, David S (2006) Age-related changes in iron homeostasis and cell death in the cerebellum of ceruloplasmin-deficient mice. J Neurosci 26:9810–9819. https://doi.org/10.1523/jneurosci.2922-06.2006
Jeong SY, Rathore KI, Schulz K et al (2009) Dysregulation of iron homeostasis in the CNS contributes to disease progression in a mouse model of amyotrophic lateral sclerosis. J Neurosci off J Soc Neurosci 29:610–619. https://doi.org/10.1523/jneurosci.5443-08.2009
Jiang X, Bao Y, Liu H et al (2017) VPS34 stimulation of p62 phosphorylation for cancer progression. Oncogene 36:6850–6862. https://doi.org/10.1038/onc.2017.295
Jiang X, Stockwell BR, Conrad M (2021) Ferroptosis: mechanisms, biology and role in disease. Nat Rev Mol Cell Biol 22:266–282. https://doi.org/10.1038/s41580-020-00324-8
Jiménez-Villegas J, Ferraiuolo L, Mead RJ et al (2021) NRF2 as a therapeutic opportunity to impact in the molecular roadmap of ALS. Free Radic Biol Med 173:125–141. https://doi.org/10.1016/j.freeradbiomed.2021.07.022
Jing W, Yang J-J, Cao Y et al (2020) Iron overload contributes to general anaesthesia-induced neurotoxicity and cognitive deficits. J Neuroinflamm 17:110. https://doi.org/10.1186/s12974-020-01777-6
Johnson DA, Johnson JA (2015) Nrf2—a therapeutic target for the treatment of neurodegenerative diseases. Free Radic Biol Med 88:253–267. https://doi.org/10.1016/j.freeradbiomed.2015.07.147
Joo MS, Kim WD, Lee KY et al (2016) AMPK facilitates nuclear accumulation of Nrf2 by phosphorylating at serine 550. Mol Cell Biol 36:1931–1942. https://doi.org/10.1128/mcb.00118-16
Kagan VE, Mao G, Qu F et al (2017) Oxidized arachidonic and adrenic PEs navigate cells to ferroptosis. Nat Chem Biol 13:81–90. https://doi.org/10.1038/nchembio.2238
Kajarabille N, Latunde-Dada GO (2019) Programmed cell-death by ferroptosis: antioxidants as mitigators. Int J Mol Sci 20:4968. https://doi.org/10.3390/ijms20194968
Kakhlon O, Cabantchik ZI (2002) The labile iron pool: characterization, measurement, and participation in cellular processes(1). Free Radic Biol Med 33:1037–1046. https://doi.org/10.1016/s0891-5849(02)01006-7
Kalinina EV, Chernov NN, Novichkova MD (2014) Role of glutathione, glutathione transferase, and glutaredoxin in regulation of redox-dependent processes. Biochemistry (MOSC) 79:1562–1583. https://doi.org/10.1134/s0006297914130082
Karelson E, Bogdanovic N, Garlind A et al (2001) The cerebrocortical areas in normal brain aging and in Alzheimer’s disease: noticeable differences in the lipid peroxidation level and in antioxidant defense. Neurochem Res 26:353–361. https://doi.org/10.1023/a:1010942929678
Karuppagounder SS, Alin L, Chen Y et al (2018) N-acetylcysteine targets 5 lipoxygenase-derived, toxic lipids and can synergize with prostaglandin E2 to inhibit ferroptosis and improve outcomes following hemorrhagic stroke in mice. Ann Neurol 84:854–872. https://doi.org/10.1002/ana.25356
Kasarskis EJ, Tandon L, Lovell MA, Ehmann WD (1995) Aluminum, calcium, and iron in the spinal cord of patients with sporadic amyotrophic lateral sclerosis using laser microprobe mass spectroscopy: a preliminary study. J Neurol Sci 130:203–208. https://doi.org/10.1016/0022-510x(95)00037-3
Katoh Y, Itoh K, Yoshida E et al (2001) Two domains of Nrf2 cooperatively bind CBP, a CREB binding protein, and synergistically activate transcription: synergistic activation of Nrf2 by CBP. Genes Cells 6:857–868. https://doi.org/10.1046/j.1365-2443.2001.00469.x
Kaur D, Yantiri F, Rajagopalan S et al (2003) Genetic or pharmacological iron chelation prevents MPTP-induced neurotoxicity in vivo: a novel therapy for Parkinson’s disease. Neuron 37:899–909. https://doi.org/10.1016/s0896-6273(03)00126-0
Keizman D, Ish-Shalom M, Berliner S et al (2009) Low uric acid levels in serum of patients with ALS: further evidence for oxidative stress? J Neurol Sci 285:95–99. https://doi.org/10.1016/j.jns.2009.06.002
Kenkhuis B, Somarakis A, De Haan L et al (2021) Iron loading is a prominent feature of activated microglia in Alzheimer’s disease patients. Acta Neuropathol Commun 9:27. https://doi.org/10.1186/s40478-021-01126-5
Kensler TW, Wakabayashi N, Biswal S (2007) Cell survival responses to environmental stresses via the Keap1-Nrf2-ARE pathway. Annu Rev Pharmacol Toxicol 47:89–116. https://doi.org/10.1146/annurev.pharmtox.46.120604.141046
Kim K (2021) Glutathione in the nervous system as a potential therapeutic target to control the development and progression of amyotrophic lateral sclerosis. Antioxidants 10:1011. https://doi.org/10.3390/antiox10071011
Kim E-J, Jang M, Lee MJ et al (2017) Schisandra chinensis stem ameliorates 3-nitropropionic acid-induced striatal toxicity via activation of the Nrf2 pathway and inhibition of the MAPKs and NF-κB pathways. Front Pharmacol 8:673. https://doi.org/10.3389/fphar.2017.00673
Kirby J, Halligan E, Baptista MJ et al (2005) Mutant SOD1 alters the motor neuronal transcriptome: implications for familial ALS. Brain 128:1686–1706. https://doi.org/10.1093/brain/awh503
Klepac N, Relja M, Klepac R et al (2007) Oxidative stress parameters in plasma of Huntington’s disease patients, asymptomatic Huntington’s disease gene carriers and healthy subjects : a cross-sectional study. J Neurol 254:1676–1683. https://doi.org/10.1007/s00415-007-0611-y
Klomp LW, Farhangrazi ZS, Dugan LL, Gitlin JD (1996) Ceruloplasmin gene expression in the murine central nervous system. J Clin Invest 98:207–215. https://doi.org/10.1172/jci118768
Kobayashi M, Yamamoto M (2005) Molecular mechanisms activating the Nrf2-Keap1 pathway of antioxidant gene regulation. Antioxid Redox Signal 7:385–394. https://doi.org/10.1089/ars.2005.7.385
Kobayashi M, Yamamoto M (2006) Nrf2-Keap1 regulation of cellular defense mechanisms against electrophiles and reactive oxygen species. Adv Enzyme Regul 46:113–140. https://doi.org/10.1016/j.advenzreg.2006.01.007
Kobayashi A, Kang M-I, Okawa H et al (2004) Oxidative stress sensor Keap1 functions as an adaptor for Cul3-based E3 ligase to regulate proteasomal degradation of Nrf2. Mol Cell Biol 24:7130–7139. https://doi.org/10.1128/mcb.24.16.7130-7139.2004
Komatsu M, Kurokawa H, Waguri S et al (2010) The selective autophagy substrate p62 activates the stress responsive transcription factor Nrf2 through inactivation of Keap1. Nat Cell Biol 12:213–223. https://doi.org/10.1038/ncb2021
Koppula P, Zhang Y, Zhuang L, Gan B (2018) Amino acid transporter SLC7A11/xCT at the crossroads of regulating redox homeostasis and nutrient dependency of cancer. Cancer Commun 38:12. https://doi.org/10.1186/s40880-018-0288-x
Kraft AD, Johnson DA, Johnson JA (2004) Nuclear factor E2-related factor 2-dependent antioxidant response element activation by tert-butylhydroquinone and sulforaphane occurring preferentially in astrocytes conditions neurons against oxidative insult. J Neurosci 24:1101–1112. https://doi.org/10.1523/jneurosci.3817-03.2004
Kraft A, Resch J, Johnson D, Johnson J (2007) Activation of the Nrf2-ARE pathway in muscle and spinal cord during ALS-like pathology in mice expressing mutant SOD1. Exp Neurol 207:107–117. https://doi.org/10.1016/j.expneurol.2007.05.026
Kraft VAN, Bezjian CT, Pfeiffer S et al (2020) GTP Cyclohydrolase 1/Tetrahydrobiopterin Counteract Ferroptosis through Lipid Remodeling. ACS Cent Sci 6:41–53. https://doi.org/10.1021/acscentsci.9b01063
Kulasekaran G, Ganapasam S (2015) Neuroprotective efficacy of naringin on 3-nitropropionic acid-induced mitochondrial dysfunction through the modulation of Nrf2 signaling pathway in PC12 cells. Mol Cell Biochem 409:199–211. https://doi.org/10.1007/s11010-015-2525-9
Kussmaul L, Hirst J (2006) The mechanism of superoxide production by NADH:ubiquinone oxidoreductase (complex I) from bovine heart mitochondria. Proc Natl Acad Sci 103:7607–7612. https://doi.org/10.1073/pnas.0510977103
Kuusisto E, Parkkinen L, Alafuzoff I (2003) Morphogenesis of Lewy bodies: dissimilar incorporation of alpha-synuclein, ubiquitin, and p62. J Neuropathol Exp Neurol 62:1241–1253. https://doi.org/10.1093/jnen/62.12.1241
Kwak M-K, Itoh K, Yamamoto M, Kensler TW (2002) Enhanced expression of the transcription factor Nrf2 by cancer chemopreventive agents: role of antioxidant response element-like sequences in the nrf2 promoter. Mol Cell Biol 22:2883–2892. https://doi.org/10.1128/mcb.22.9.2883-2892.2002
Kwok RPS, Lundblad JR, Chrivia JC et al (1994) Nuclear protein CBP is a coactivator for the transcription factor CREB. Nature 370:223–226. https://doi.org/10.1038/370223a0
Kwon M-Y, Park E, Lee S-J, Chung SW (2015) Heme oxygenase-1 accelerates erastin-induced ferroptotic cell death. Oncotarget 6:24393–24403. https://doi.org/10.18632/oncotarget.5162
Kwon SH, Lee SR, Park YJ et al (2019) Suppression of 6-hydroxydopamine-induced oxidative stress by hyperoside via activation of Nrf2/HO-1 signaling in dopaminergic neurons. Int J Mol Sci 20:5832. https://doi.org/10.3390/ijms20235832
Lane DJR, Robinson SR, Czerwinska H et al (2010) Two routes of iron accumulation in astrocytes: ascorbate-dependent ferrous iron uptake via the divalent metal transporter (DMT1) plus an independent route for ferric iron. Biochem J 432:123–132. https://doi.org/10.1042/bj20101317
Lane DJR, Metselaar B, Greenough M et al (2021) Ferroptosis and NRF2: an emerging battlefield in the neurodegeneration of Alzheimer’s disease. Essays Biochem 65:925–940. https://doi.org/10.1042/ebc20210017
Langston JW, Ballard P, Tetrud JW, Irwin I (1983) Chronic Parkinsonism in humans due to a product of meperidine-analog synthesis. Science 219:979–980. https://doi.org/10.1126/science.6823561
Lastres-Becker I, García-Yagüe AJ, Scannevin RH et al (2016) Repurposing the NRF2 activator dimethyl fumarate as therapy against synucleinopathy in Parkinson’s disease. Antioxid Redox Signal 25:61–77. https://doi.org/10.1089/ars.2015.6549
Lastres-Becker I, Porras G, Arribas-Blázquez M et al (2021) Molecular alterations in sporadic and SOD1-ALS immortalized lymphocytes: towards a personalized therapy. Int J Mol Sci 22:3007. https://doi.org/10.3390/ijms22063007
Lee J-M, Johnson JA (2004) An important role of Nrf2-ARE pathway in the cellular defense mechanism. Bmb Rep 37:139–143. https://doi.org/10.5483/bmbrep.2004.37.2.139
Lee JK, Shin JH, Gwag BJ, Choi E-J (2015) Iron accumulation promotes TACE-mediated TNF-α secretion and neurodegeneration in a mouse model of ALS. Neurobiol Dis 80:63–69. https://doi.org/10.1016/j.nbd.2015.05.009
Lee J, You JH, Kim M-S, Roh J-L (2020) Epigenetic reprogramming of epithelial-mesenchymal transition promotes ferroptosis of head and neck cancer. Redox Biol 37:101697. https://doi.org/10.1016/j.redox.2020.101697
Lee Mosley R, Benner EJ, Kadiu I et al (2006) Neuroinflammation, oxidative stress and the pathogenesis of Parkinson’s disease. Clin Neurosci Res 6:261–281. https://doi.org/10.1016/j.cnr.2006.09.006
Lei P, Ayton S, Finkelstein DI et al (2012) Tau deficiency induces Parkinsonism with dementia by impairing APP-mediated iron export. Nat Med 18:291–295. https://doi.org/10.1038/nm.2613
Leng F, Edison P (2021) Neuroinflammation and microglial activation in Alzheimer disease: Where do we go from here? Nat Rev Neurol 17:157–172. https://doi.org/10.1038/s41582-020-00435-y
Lesage S, Brice A (2009) Parkinson’s disease: from monogenic forms to genetic susceptibility factors. Hum Mol Genet 18:R48–R59. https://doi.org/10.1093/hmg/ddp012
Lewerenz J, Maher P (2011) Control of redox state and redox signaling by neural antioxidant systems. Antioxid Redox Ing 14:1449–1465. https://doi.org/10.1089/ars.2010.3600
Lhermitte J, Kraus WM, McAlpine D (1924) Original papers: on the occurrence of abnormal deposits of iron in the brain in Parkinsonism with special reference to its localisation. J Neurol Neurosurg Psychiatry 1–5:195–208. https://doi.org/10.1136/jnnp.s1-5.19.195
Li C, Chen T, Zhou H et al (2018) Schisantherin a attenuates neuroinflammation in activated microglia: role of Nrf2 activation through ERK phosphorylation. Cell Physiol Biochem 47:1769–1784. https://doi.org/10.1159/000491059
Liddell J (2017) Are astrocytes the predominant cell type for activation of Nrf2 in aging and neurodegeneration? Antioxidants 6:65. https://doi.org/10.3390/antiox6030065
Lin J-T, Chang W-C, Chen H-M et al (2013) Regulation of feedback between protein kinase A and the proteasome system worsens Huntington’s disease. Mol Cell Biol 33:1073–1084. https://doi.org/10.1128/mcb.01434-12
Lind C, Hochstein P, Ernster L (1982) DT-diaphorase as a quinone reductase: a cellular control device against semiquinone and superoxide radical formation. Arch Biochem Biophys 216:178–185. https://doi.org/10.1016/0003-9861(82)90202-8
Liu H, Feng Y, Xu M et al (2018) Four-octyl itaconate activates Keap1-Nrf2 signaling to protect neuronal cells from hydrogen peroxide. Cell Commun Signal 16:81. https://doi.org/10.1186/s12964-018-0294-2
Liu M, Zhu W, Pei D (2021) System Xc−: a key regulatory target of ferroptosis in cancer. Invest New Drugs 39:1123–1131. https://doi.org/10.1007/s10637-021-01070-0
Llanos-González E, Henares-Chavarino ÁA, Pedrero-Prieto CM et al (2020) Interplay between mitochondrial oxidative disorders and proteostasis in Alzheimer’s disease. Front Neurosci 13:1444. https://doi.org/10.3389/fnins.2019.01444
Lo JY, Spatola BN, Curran SP (2017) WDR23 regulates NRF2 independently of KEAP1. Plos Genet 13:e1006762. https://doi.org/10.1371/journal.pgen.1006762
Loboda A, Damulewicz M, Pyza E et al (2016) Role of Nrf2/HO-1 system in development, oxidative stress response and diseases: an evolutionarily conserved mechanism. Cell Mol Life Sci 73:3221–3247. https://doi.org/10.1007/s00018-016-2223-0
Lovell MA, Robertson JD, Teesdale WJ et al (1998) Copper, iron and zinc in Alzheimer’s disease senile plaques. J Neurol Sci 158:47–52. https://doi.org/10.1016/s0022-510x(98)00092-6
Luo J-F, Shen X-Y, Lio CK et al (2018) Activation of Nrf2/HO-1 pathway by nardochinoid C inhibits inflammation and oxidative stress in lipopolysaccharide-stimulated macrophages. Front Pharmacol 9:911. https://doi.org/10.3389/fphar.2018.00911
Ma H, Jiang T, Tang W et al (2020) Transplantation of platelet-derived mitochondria alleviates cognitive impairment and mitochondrial dysfunction in db/db mice. Clin Sci 134:2161–2175. https://doi.org/10.1042/cs20200530
Maher P (2005) The effects of stress and aging on glutathione metabolism. Ageing Res Rev 4:288–314. https://doi.org/10.1016/j.arr.2005.02.005
Maiorino M, Conrad M, Ursini F (2018) GPx4, lipid peroxidation, and cell death: discoveries, rediscoveries, and open issues. Antioxid Redox Signal 29:61–74. https://doi.org/10.1089/ars.2017.7115
Malagelada C, Jin ZH, Greene LA (2008) RTP801 is induced in Parkinson’s disease and mediates neuron death by inhibiting Akt phosphorylation/activation. J Neurosci 28:14363–14371. https://doi.org/10.1523/jneurosci.3928-08.2008
Mandal PK, Saharan S, Tripathi M, Murari G (2015) Brain glutathione levels–a novel biomarker for mild cognitive impairment and Alzheimer’s disease. Biol Psychiatry 78:702–710. https://doi.org/10.1016/j.biopsych.2015.04.005
Mao C, Liu X, Zhang Y et al (2021) DHODH-mediated ferroptosis defence is a targetable vulnerability in cancer. Nature 593:586–590. https://doi.org/10.1038/s41586-021-03539-7
Maragakis NJ, Rothstein JD (2006) Mechanisms of disease: astrocytes in neurodegenerative disease. Nat Clin Pract Neuro 2:679–689. https://doi.org/10.1038/ncpneuro0355
Markesbery WR (1997) Oxidative stress hypothesis in Alzheimer’s disease. Free Radic Biol Med 23:134–147. https://doi.org/10.1016/s0891-5849(96)00629-6
Marro S, Chiabrando D, Messana E et al (2010) Heme controls ferroportin1 (FPN1) transcription involving Bach1, Nrf2 and a MARE/ARE sequence motif at position -7007 of the FPN1 promoter. Haematologica 95:1261–1268. https://doi.org/10.3324/haematol.2009.020123
Martin S, Al Khleifat A, Al-Chalabi A (2017) What causes amyotrophic lateral sclerosis? Research 6:371. https://doi.org/10.12688/f1000research.10476.1
Masaldan S, Bush AI, Devos D et al (2019) Striking while the iron is hot: iron metabolism and ferroptosis in neurodegeneration. Free Radic Biol Med 133:221–233. https://doi.org/10.1016/j.freeradbiomed.2018.09.033
Mason RP, Casu M, Butler N et al (2013) Glutathione peroxidase activity is neuroprotective in models of Huntington’s disease. Nat Genet 45:1249–1254. https://doi.org/10.1038/ng.2732
McCann SK, Dusting GJ, Roulston CL (2008) Early increase of Nox4 NADPH oxidase and superoxide generation following endothelin-1-induced stroke in conscious rats. J Neurosci Res 86:2524–2534. https://doi.org/10.1002/jnr.21700
McCarthy RC, Kosman DJ (2012) Mechanistic analysis of iron accumulation by endothelial cells of the BBB. Biometals 25:665–675. https://doi.org/10.1007/s10534-012-9538-6
McCarthy RC, Kosman DJ (2013) Ferroportin and exocytoplasmic ferroxidase activity are required for brain microvascular endothelial cell iron efflux. J Biol Chem 288:17932–17940. https://doi.org/10.1074/jbc.m113.455428
McCarthy RC, Kosman DJ (2015) Iron transport across the blood–brain barrier: development, neurovascular regulation and cerebral amyloid angiopathy. Cell Mol Life Sci 72:709–727. https://doi.org/10.1007/s00018-014-1771-4
McCarthy RC, Park Y, Kosman DJ (2014) sAPP modulates iron efflux from brain microvascular endothelial cells by stabilizing the ferrous iron exporter ferroportin. EMBO Rep 15:809–815. https://doi.org/10.15252/embr.201338064
McColgan P, Tabrizi SJ (2018) Huntington’s disease: a clinical review. Eur J Neurol 25:24–34. https://doi.org/10.1111/ene.13413
Meng FX, Hou JM, Sun TS (2017) In vivo evaluation of microglia activation by intracranial iron overload in central pain after spinal cord injury. J Orthop Surg Res 12:75. https://doi.org/10.1186/s13018-017-0578-z
Mesci P, Zaïdi S, Lobsiger CS et al (2015) System xC- is a mediator of microglial function and its deletion slows symptoms in amyotrophic lateral sclerosis mice. Brain 138:53–68. https://doi.org/10.1093/brain/awu312
Meyron-Holtz EG, Ghosh MC, Iwai K et al (2004) Genetic ablations of iron regulatory proteins 1 and 2 reveal why iron regulatory protein 2 dominates iron homeostasis. Embo J 23:386–395. https://doi.org/10.1038/sj.emboj.7600041
Milligan CE, Cunningham TJ, Levitt P (1991) Differential immunochemical markers reveal the normal distribution of brain macrophages and microglia in the developing rat brain. J Comp Neurol 314:125–135. https://doi.org/10.1002/cne.903140112
Mimoto T, Miyazaki K, Morimoto N et al (2012) Impaired antioxydative Keap1/Nrf2 system and the downstream stress protein responses in the motor neuron of ALS model mice. Brain Res 1446:109–118. https://doi.org/10.1016/j.brainres.2011.12.064
Miotto G, Rossetto M, Di Paolo ML et al (2020) Insight into the mechanism of ferroptosis inhibition by ferrostatin-1. Redox Biol 28:101328. https://doi.org/10.1016/j.redox.2019.101328
Miseta A, Csutora P (2000) Relationship between the occurrence of cysteine in proteins and the complexity of organisms. Mol Biol Evol 17:1232–1239. https://doi.org/10.1093/oxfordjournals.molbev.a026406
Mishima E, Ito J, Wu Z et al (2022) A non-canonical vitamin K cycle is a potent ferroptosis suppressor. Nature 608:778–783. https://doi.org/10.1038/s41586-022-05022-3
Mitsui S, Otomo A, Nozaki M et al (2018) Systemic overexpression of SQSTM1/p62 accelerates disease onset in a SOD1H46R-expressing ALS mouse model. Mol Brain 11:30. https://doi.org/10.1186/s13041-018-0373-8
Mizunoe Y, Kobayashi M, Sudo Y et al (2018) Trehalose protects against oxidative stress by regulating the Keap1-Nrf2 and autophagy pathways. Redox Biol 15:115–124. https://doi.org/10.1016/j.redox.2017.09.007
Mogi M, Kondo T, Mizuno Y, Nagatsu T (2007) p53 protein, interferon-γ, and NF-κB levels are elevated in the Parkinsonian brain. Neurosci Lett 414:94–97. https://doi.org/10.1016/j.neulet.2006.12.003
Moos T (1995) Developmental profile of non-heme iron distribution in the rat brain during ontogenesis. Dev Brain Res 87:203–213. https://doi.org/10.1016/0165-3806(95)00077-q
Moos T, Morgan EH (2003) The significance of the mutated divalent metal transporter (DMT1) on iron transport into the Belgrade rat brain. J Neurochem 88:233–245. https://doi.org/10.1046/j.1471-4159.2003.02142.x
Moos T, Skjoerringe T, Gosk S, Morgan EH (2006) Brain capillary endothelial cells mediate iron transport into the brain by segregating iron from transferrin without the involvement of divalent metal transporter 1. J Neurochem 98:1946–1958. https://doi.org/10.1111/j.1471-4159.2006.04023.x
Moos T, Nielsen TR, Skjørringe T, Morgan EH (2007) Iron trafficking inside the brain. J Neurochem 103:1730–1740. https://doi.org/10.1111/j.1471-4159.2007.04976.x
Moreau C, Danel V, Devedjian JC et al (2018) Could conservative iron chelation lead to neuroprotection in amyotrophic lateral sclerosis? Antioxid Redox Signaling 29:742–748. https://doi.org/10.1089/ars.2017.7493
Morris GP, Clark IA, Vissel B (2014) Inconsistencies and controversies surrounding the amyloid hypothesis of Alzheimer’s disease. Acta Neuropathol Commun 2:135. https://doi.org/10.1186/s40478-014-0135-5
Morris G, Berk M, Carvalho AF et al (2018) Why should neuroscientists worry about iron? The emerging role of ferroptosis in the pathophysiology of neuroprogressive diseases. Behav Brain Res 341:154–175. https://doi.org/10.1016/j.bbr.2017.12.036
Motohashi H, Katsuoka F, Engel JD, Yamamoto M (2004) Small Maf proteins serve as transcriptional cofactors for keratinocyte differentiation in the Keap1-Nrf2 regulatory pathway. Proc Natl Acad Sci USA 101:6379–6384. https://doi.org/10.1073/pnas.0305902101
Moujalled D, Grubman A, Acevedo K et al (2017) TDP-43 mutations causing amyotrophic lateral sclerosis are associated with altered expression of RNA-binding protein hnRNP K and affect the Nrf2 antioxidant pathway. Hum Mol Genet 26:1732–1746. https://doi.org/10.1093/hmg/ddx093
Muñoz P, Zavala G, Castillo K et al (2006) Effect of iron on the activation of the MAPK/ERK pathway in PC12 neuroblastoma cells. Biol Res 39:189–190. https://doi.org/10.4067/s0716-97602006000100021
Murata H, Takamatsu H, Liu S et al (2015) NRF2 regulates PINK1 expression under oxidative stress conditions. PLoS ONE 10:e0142438. https://doi.org/10.1371/journal.pone.0142438
Nanou A, Higginbottom A, Valori CF et al (2013) Viral delivery of antioxidant genes as a therapeutic strategy in experimental models of amyotrophic lateral sclerosis. Mol Ther 21:1486–1496. https://doi.org/10.1038/mt.2013.115
Narendra D, Kane LA, Hauser DN et al (2010) p62/SQSTM1 is required for Parkin-induced mitochondrial clustering but not mitophagy; VDAC1 is dispensable for both. Autophagy 6:1090–1106. https://doi.org/10.4161/auto.6.8.13426
Nayernia Z, Jaquet V, Krause K-H (2014) New insights on NOX enzymes in the central nervous system. Antioxid Redox Signal 20:2815–2837. https://doi.org/10.1089/ars.2013.5703
Nemeth E, Tuttle MS, Powelson J et al (2004) Hepcidin regulates cellular iron efflux by binding to ferroportin and inducing its internalization. Science 306:2090–2093. https://doi.org/10.1126/science.1104742
Newcombe EA, Camats-Perna J, Silva ML et al (2018) Inflammation: the link between comorbidities, genetics, and Alzheimer’s disease. J Neuroinflamm 15:276. https://doi.org/10.1186/s12974-018-1313-3
Nioi P, Nguyen T, Sherratt PJ, Pickett CB (2005) The carboxy-terminal Neh3 domain of Nrf2 is required for transcriptional activation. Mol Cell Biol 25:10895–10906. https://doi.org/10.1128/mcb.25.24.10895-10906.2005
Nishizawa H, Matsumoto M, Shindo T et al (2020) Ferroptosis is controlled by the coordinated transcriptional regulation of glutathione and labile iron metabolism by the transcription factor BACH1. J Biol Chem 295:69–82. https://doi.org/10.1074/jbc.ra119.009548
Nnah IC, Lee C, Wessling-Resnick M (2020) Iron potentiates microglial interleukin-1β secretion induced by amyloid-β. J Neurochem 154:177–189. https://doi.org/10.1111/jnc.14906
Nolfi-Donegan D, Braganza A, Shiva S (2020) Mitochondrial electron transport chain: oxidative phosphorylation, oxidant production, and methods of measurement. Redox Biol 37:101674. https://doi.org/10.1016/j.redox.2020.101674
Oba H, Araki T, Ohtomo K et al (1993) Amyotrophic lateral sclerosis: T2 shortening in motor cortex at MR imaging. Radiology 189:843–846. https://doi.org/10.1148/radiology.189.3.8234713
Ogawa K (2001) Heme mediates derepression of Maf recognition element through direct binding to transcription repressor Bach1. Embo J 20:2835–2843. https://doi.org/10.1093/emboj/20.11.2835
Ohgami RS, Campagna DR, Greer EL et al (2005) Identification of a ferrireductase required for efficient transferrin-dependent iron uptake in erythroid cells. Nat Genet 37:1264–1269. https://doi.org/10.1038/ng1658
Ohta Y, Nomura E, Shang J et al (2019) Enhanced oxidative stress and the treatment by edaravone in mice model of amyotrophic lateral sclerosis. J Neurosci Res 97:607–619. https://doi.org/10.1002/jnr.24368
Osama A, Zhang J, Yao J et al (2020) Nrf2: a dark horse in Alzheimer’s disease treatment. Ageing Res Rev 64:101206. https://doi.org/10.1016/j.arr.2020.101206
Ou M, Jiang Y, Ji Y et al (2022) Role and mechanism of ferroptosis in neurological diseases. Mol Metab 61:101502. https://doi.org/10.1016/j.molmet.2022.101502
Pan Q, Luo Y, Xia Q, He K (2021) Ferroptosis and liver fibrosis. Int J Med Sci 18:3361–3366. https://doi.org/10.7150/ijms.62903
Panieri E, Saso L (2019) Potential applications of NRF2 inhibitors in cancer therapy. Oxid Med Cell Longev 2019:1–34. https://doi.org/10.1155/2019/8592348
Pardridge WM, Eisenberg J, Yang J (1987) Human blood–brain barrier transferrin receptor. Metabolis 36:892–895. https://doi.org/10.1016/0026-0495(87)90099-0
Park MW, Cha HW, Kim J et al (2021) NOX4 promotes ferroptosis of astrocytes by oxidative stress-induced lipid peroxidation via the impairment of mitochondrial metabolism in Alzheimer’s diseases. Redox Biol 41:101947. https://doi.org/10.1016/j.redox.2021.101947
Pavlovskiĭ DP, Mikaĭlenko ET (1976) Use of hemostatic preparations in obstetrical hemorrhages. Pediatriia Akusherstvo I Ginekologiia 1976:33–37
Pedersen WA, Fu W, Keller JN et al (1998) Protein modification by the lipid peroxidation product 4-hydroxynonenal in the spinal cords of amyotrophic lateral sclerosis patients. Ann Neurol 44:819–824. https://doi.org/10.1002/ana.410440518
Pehar M, Vargas MR, Robinson KM et al (2007) Mitochondrial superoxide production and nuclear factor erythroid 2-related factor 2 activation in p75 neurotrophin receptor-induced motor neuron apoptosis. J Neurosci 27:7777–7785. https://doi.org/10.1523/jneurosci.0823-07.2007
Pelizzoni I, Zacchetti D, Campanella A et al (2013) Iron uptake in quiescent and inflammation-activated astrocytes: a potentially neuroprotective control of iron burden. Biochim Biophys Acta (BBA) Mol Basis Dis 1832:1326–1333. https://doi.org/10.1016/j.bbadis.2013.04.007
Penning TM (2017) Aldo-keto reductase regulation by the Nrf2 system: implications for stress response, chemotherapy drug resistance, and carcinogenesis. Chem Res Toxicol 30:162–176. https://doi.org/10.1021/acs.chemrestox.6b00319
Peoples JN, Saraf A, Ghazal N et al (2019) Mitochondrial dysfunction and oxidative stress in heart disease. Exp Mol Med 51:1–13. https://doi.org/10.1038/s12276-019-0355-7
Pérez-Severiano F, Rıos C, Segovia J (2000) Striatal oxidative damage parallels the expression of a neurological phenotype in mice transgenic for the mutation of Huntington’s disease. Brain Res 862:234–237. https://doi.org/10.1016/s0006-8993(00)02082-5
Perluigi M, Tramutola A, Pagnotta S et al (2020) The BACH1/Nrf2 axis in brain in down syndrome and transition to Alzheimer disease-like neuropathology and dementia. Antioxidants 9:779. https://doi.org/10.3390/antiox9090779
Peters DG, Pollack AN, Cheng KC et al (2018) Dietary lipophilic iron alters amyloidogenesis and microglial morphology in Alzheimer’s disease knock-in APP mice. Metall Integr Biometal Sci 10:426–443. https://doi.org/10.1039/c8mt00004b
Poirier J, Barbeau A (1985) 1-Methyl-4-phenyl-pyridinium-induced inhibition of nicotinamide adenosine dinucleotide cytochrome c reductase. Neurosci Lett 62:7–11. https://doi.org/10.1016/0304-3940(85)90276-9
Prasuhn J, Davis RL, Kumar KR (2021) Targeting mitochondrial impairment in Parkinson’s disease: challenges and opportunities. Front Cell Dev Biol 8:615461. https://doi.org/10.3389/fcell.2020.615461
Prestera T, Holtzclaw WD, Zhang Y, Talalay P (1993) Chemical and molecular regulation of enzymes that detoxify carcinogens. Proc Natl Acad Sci 90:2965–2969. https://doi.org/10.1073/pnas.90.7.2965
Pyle A, Anugrha H, Kurzawa-Akanbi M et al (2016) Reduced mitochondrial DNA copy number is a biomarker of Parkinson’s disease. Neurobiol Aging 38:216.e7-216.e10. https://doi.org/10.1016/j.neurobiolaging.2015.10.033
Qi Y, Jamindar TM, Dawson G (2002) Hypoxia alters iron homeostasis and induces ferritin synthesis in oligodendrocytes. J Neurochem 64:2458–2464. https://doi.org/10.1046/j.1471-4159.1995.64062458.x
Qi D, Chen P, Bao H et al (2023) Dimethyl fumarate protects against hepatic ischemia-reperfusion injury by alleviating ferroptosis via the NRF2/SLC7A11/HO-1 axis. Cell Cycle 22:818–828. https://doi.org/10.1080/15384101.2022.2155016
Qian Z-M, Chang Y-Z, Zhu L et al (2007) Development and iron-dependent expression of hephaestin in different brain regions of rats. J Cell Biochem 102:1225–1233. https://doi.org/10.1002/jcb.21352
Qin L, Liu Y, Hong J-S, Crews FT (2013) NADPH oxidase and aging drive microglial activation, oxidative stress, and dopaminergic neurodegeneration following systemic LPS administration. Glia 61:855–868. https://doi.org/10.1002/glia.22479
Rada P, Rojo AI, Chowdhry S et al (2011) SCF/β-TrCP promotes glycogen synthase kinase 3-dependent degradation of the Nrf2 transcription factor in a keap1-independent manner. Mol Cell Biol 31:1121–1133. https://doi.org/10.1128/mcb.01204-10
Raina AK, Templeton DJ, Deak JC et al (1999) Quinone reductase (NQO1), a sensitive redox indicator, is increased in Alzheimer’s disease. Redox Rep 4:23–27. https://doi.org/10.1179/135100099101534701
Ramsey CP, Glass CA, Montgomery MB et al (2007) Expression of Nrf2 in neurodegenerative diseases. J Neuropathol Exp Neurol 66:75–85. https://doi.org/10.1097/nen.0b013e31802d6da9
Raub TJ, Newton CR (1991) Recycling kinetics and transcytosis of transferrin in primary cultures of bovine brain microvessel endothelial cells. J Cell Physiol 149:141–151. https://doi.org/10.1002/jcp.1041490118
Ravikumar B, Vacher C, Berger Z et al (2004) Inhibition of mTOR induces autophagy and reduces toxicity of polyglutamine expansions in fly and mouse models of Huntington disease. Nat Genet 36:585–595. https://doi.org/10.1038/ng1362
Reinisalo M, Kårlund A, Koskela A et al (2015) Polyphenol stilbenes: molecular mechanisms of defence against oxidative stress and aging-related diseases. Oxid Med Cell Longev 2015:1–24. https://doi.org/10.1155/2015/340520
Reynolds NC, Prost RW, Mark LP (2005) Heterogeneity in 1H-MRS profiles of presymptomatic and early manifest Huntington’s disease. Brain Res 1031:82–89. https://doi.org/10.1016/j.brainres.2004.10.030
Riegman M, Sagie L, Galed C et al (2020) Ferroptosis occurs through an osmotic mechanism and propagates independently of cell rupture. Nat Cell Biol 22:1042–1048. https://doi.org/10.1038/s41556-020-0565-1
Roberts BR, Lim NKH, McAllum EJ et al (2014) Oral treatment with Cu(II)(atsm) increases mutant SOD1 in vivo but protects motor neurons and improves the phenotype of a transgenic mouse model of amyotrophic lateral sclerosis. J Neurosci 34:8021–8031. https://doi.org/10.1523/jneurosci.4196-13.2014
Robledinos-Antón N, Fernández-Ginés R, Manda G, Cuadrado A (2019) Activators and inhibitors of NRF2: a review of their potential for clinical development. Oxid Med Cell Longev 2019:1–20. https://doi.org/10.1155/2019/9372182
Rogers JT, Randall JD, Cahill CM et al (2002) An iron-responsive element type II in the 5′-untranslated region of the Alzheimer’s amyloid precursor protein transcript. J Biol Chem 277:45518–45528. https://doi.org/10.1074/jbc.m207435200
Rose J, Brian C, Pappa A et al (2020) Mitochondrial metabolism in astrocytes regulates brain bioenergetics, neurotransmission and redox balance. Front Neurosci 14:536682. https://doi.org/10.3389/fnins.2020.536682
Rosen DR (1993) Mutations in Cu/Zn superoxide dismutase gene are associated with familial amyotrophic lateral sclerosis. Nature 364:362. https://doi.org/10.1038/364362c0
Ross D, Siegel D (2017) Functions of NQO1 in cellular protection and CoQ10 metabolism and its potential role as a redox sensitive molecular switch. Front Physiol. https://doi.org/10.3389/fphys.2017.00595
Ross CA, Tabrizi SJ (2011) Huntington’s disease: from molecular pathogenesis to clinical treatment. Lancet Neurol 10:83–98. https://doi.org/10.1016/s1474-4422(10)70245-3
Routhe LJ, Andersen IK, Hauerslev LV et al (2020) Astrocytic expression of ZIP14 (SLC39A14) is part of the inflammatory reaction in chronic neurodegeneration with iron overload. Glia 68:1810–1823. https://doi.org/10.1002/glia.23806
Ru Q, Li Y, Xie W et al (2023) Fighting age-related orthopedic diseases: focusing on ferroptosis. Bone Res 11:12. https://doi.org/10.1038/s41413-023-00247-y
Saha S, Buttari B, Profumo E et al (2022) A perspective on Nrf2 signaling pathway for neuroinflammation: a potential therapeutic target in Alzheimer’s and Parkinson’s diseases. Front Cell Neurosci 15:787258. https://doi.org/10.3389/fncel.2021.787258
Saito Y, Yako T, Otsu W et al (2020) A triterpenoid Nrf2 activator, RS9, promotes LC3-associated phagocytosis of photoreceptor outer segments in a p62-independent manner. Free Radic Biol Med 152:235–247. https://doi.org/10.1016/j.freeradbiomed.2020.03.012
SantaCruz KS, Yazlovitskaya E, Collins J et al (2004) Regional NAD(P)H:quinone oxidoreductase activity in Alzheimer’s disease. Neurobiol Aging 25:63–69. https://doi.org/10.1016/s0197-4580(03)00117-9
Santoro MM (2020) The antioxidant role of non-mitochondrial CoQ10: mystery solved! Cell Metab 31:13–15. https://doi.org/10.1016/j.cmet.2019.12.007
Sanyal B, Polak PE, Szuchet S (1996) Differential expression of the heavy-chain ferritin gene in non-adhered and adhered oligodendrocytes. J Neurosci Res 46:187–197. https://doi.org/10.1002/(sici)1097-4547(19961015)46:2%3c187::aid-jnr6%3e3.0.co;2-d
Sasaki H, Sato H, Kuriyama-Matsumura K et al (2002) Electrophile response element-mediated induction of the cystine/glutamate exchange transporter gene expression. J Biol Chem 277:44765–44771. https://doi.org/10.1074/jbc.m208704200
Sato H, Tamba M, Ishii T, Bannai S (1999) Cloning and expression of a plasma membrane cystine/glutamate exchange transporter composed of two distinct proteins. J Biol Chem 274:11455–11458. https://doi.org/10.1074/jbc.274.17.11455
Saudou F, Humbert S (2016) The biology of huntingtin. Neuron 89:910–926. https://doi.org/10.1016/j.neuron.2016.02.003
Sautin YY, Johnson RJ (2008) Uric acid: the oxidant-antioxidant paradox. Nucl Nucl Nucl Acids 27:608–619. https://doi.org/10.1080/15257770802138558
Sayed NH, Fathy N, Kortam MA et al (2020) Vildagliptin ATTENUATES Huntington’s disease through activation of GLP-1 receptor/PI3K/Akt/BDNF pathway in 3-nitropropionic acid rat model. Neurotherapeutics 17:252–268. https://doi.org/10.1007/s13311-019-00805-5
Schapira AHV, Cooper JM, Dexter D et al (1989) Mitochondrial complex I deficiency in Parkinson’s disease. Lancet 333:1269. https://doi.org/10.1016/s0140-6736(89)92366-0
Schapira AHV, Cooper JM, Dexter D et al (1990) Mitochondrial complex I deficiency in Parkinson’s disease. J Neurochem 54:823–827. https://doi.org/10.1111/j.1471-4159.1990.tb02325.x
Schipper HM, Liberman A, Stopa EG (1998) Neural heme oxygenase-1 expression in idiopathic Parkinson’s disease. Exp Neurol 150:60–68. https://doi.org/10.1006/exnr.1997.6752
Seibt TM, Proneth B, Conrad M (2019) Role of GPX4 in ferroptosis and its pharmacological implication. Free Radic Biol Med 133:144–152. https://doi.org/10.1016/j.freeradbiomed.2018.09.014
Seiler A, Schneider M, Förster H et al (2008) Glutathione peroxidase 4 senses and translates oxidative stress into 12/15-lipoxygenase dependent- and AIF-mediated cell death. Cell Metab 8:237–248. https://doi.org/10.1016/j.cmet.2008.07.005
Selkoe DJ (2012) Preventing Alzheimer’s disease. Science 337:1488–1492. https://doi.org/10.1126/science.1228541
Shao L, Dong C, Geng D et al (2021) Ginkgolide B protects against cognitive impairment in senescence-accelerated p8 mice by mitigating oxidative stress, inflammation and ferroptosis. Biochem Biophys Res Commun 572:7–14. https://doi.org/10.1016/j.bbrc.2021.07.081
Sharma N, Khurana N, Muthuraman A, Utreja P (2021) Pharmacological evaluation of vanillic acid in rotenone-induced Parkinson’s disease rat model. Eur J Pharmacol 903:174112. https://doi.org/10.1016/j.ejphar.2021.174112
Shih AY, Johnson DA, Wong G et al (2003) Coordinate regulation of glutathione biosynthesis and release by Nrf2-expressing glia potently protects neurons from oxidative stress. J Neurosci 23:3394–3406. https://doi.org/10.1523/jneurosci.23-08-03394.2003
Shih AY, Imbeault S, Barakauskas V et al (2005) Induction of the Nrf2-driven antioxidant response confers neuroprotection during mitochondrial stress in vivo. J Biol Chem 280:22925–22936. https://doi.org/10.1074/jbc.m414635200
Shim KS, Ferrando-Miguel R, Lubec G (2003) Aberrant protein expression of transcription factors BACH1 and ERG, both encoded on chromosome 21, in brains of patients with Down syndrome and Alzheimer’s disease. J Neural Transm Suppl 67:39–49. https://doi.org/10.1007/978-3-7091-6721-2_3
Shintoku R, Takigawa Y, Yamada K et al (2017) Lipoxygenase-mediated generation of lipid peroxides enhances ferroptosis induced by erastin and RSL3. Cancer Sci 108:2187–2194. https://doi.org/10.1111/cas.13380
Siegel D, Bolton EM, Burr JA et al (1997) The reduction of alpha-tocopherolquinone by human NAD(P)H: quinone oxidoreductase: the role of alpha-tocopherolhydroquinone as a cellular antioxidant. Mol Pharmacol 52:300–305. https://doi.org/10.1124/mol.52.2.300
Siegel D, Gustafson DL, Dehn DL et al (2004) NAD(P)H:quinone oxidoreductase 1: role as a superoxide scavenger. Mol Pharmacol 65:1238–1247. https://doi.org/10.1124/mol.65.5.1238
Siegel SJ, Bieschke J, Powers ET, Kelly JW (2007) The oxidative stress metabolite 4-hydroxynonenal promotes Alzheimer protofibril formation. Biochemistry 46:1503–1510. https://doi.org/10.1021/bi061853s
Silvestri L, Camaschella C (2008) A potential pathogenetic role of iron in Alzheimer’s disease. J Cell Mol Med 12:1548–1550. https://doi.org/10.1111/j.1582-4934.2008.00356.x
Simmons DA, Casale M, Alcon B et al (2007) Ferritin accumulation in dystrophic microglia is an early event in the development of Huntington’s disease. Glia 55:1074–1084. https://doi.org/10.1002/glia.20526
Simpson IA, Ponnuru P, Klinger ME et al (2015) A novel model for brain iron uptake: introducing the concept of regulation. J Cereb Blood Flow Metab 35:48–57. https://doi.org/10.1038/jcbfm.2014.168
Singh N (2014) The role of iron in prion disease and other neurodegenerative diseases. PLoS Pathog 10:e1004335. https://doi.org/10.1371/journal.ppat.1004335
Sivandzade F, Bhalerao A, Cucullo L (2019) Cerebrovascular and neurological disorders: protective role of NRF2. Int J Mol Sci 20:3433. https://doi.org/10.3390/ijms20143433
Skouta R, Dixon SJ, Wang J et al (2014) Ferrostatins inhibit oxidative lipid damage and cell death in diverse disease models. J Am Chem Soc 136:4551–4556. https://doi.org/10.1021/ja411006a
Smith MA, Harris PLR, Sayre LM, Perry G (1997) Iron accumulation in Alzheimer disease is a source of redox-generated free radicals. Proc Natl Acad Sci 94:9866–9868. https://doi.org/10.1073/pnas.94.18.9866
Smith CD, Chebrolu H, Wekstein DR et al (2007) Brain structural alterations before mild cognitive impairment. Neurology 68:1268–1273. https://doi.org/10.1212/01.wnl.0000259542.54830.34
Sofic E, Lange KW, Jellinger K, Riederer P (1992) Reduced and oxidized glutathione in the substantia nigra of patients with Parkinson’s disease. Neurosci Lett 142:128–130. https://doi.org/10.1016/0304-3940(92)90355-b
Son S, Bowie LE, Maiuri T et al (2019) High-mobility group box 1 links sensing of reactive oxygen species by huntingtin to its nuclear entry. J Biol Chem 294:1915–1923. https://doi.org/10.1074/jbc.RA117.001440
Song X, Long D (2020) Nrf2 and ferroptosis: a new research direction for neurodegenerative diseases. Front Neurosci 14:267. https://doi.org/10.3389/fnins.2020.00267
Song P, Li S, Wu H et al (2016) Parkin promotes proteasomal degradation of p62: implication of selective vulnerability of neuronal cells in the pathogenesis of Parkinson’s disease. Protein Cell 7:114–129. https://doi.org/10.1007/s13238-015-0230-9
Soon CPW, Donnelly PS, Turner BJ et al (2011) Diacetylbis(N(4)-methylthiosemicarbazonato) copper(II) (CuII(atsm)) protects against peroxynitrite-induced nitrosative damage and prolongs survival in amyotrophic lateral sclerosis mouse model. J Biol Chem 286:44035–44044. https://doi.org/10.1074/jbc.m111.274407
Soós J, Engelhardt JI, Siklós L et al (2004) The expression of PARP, NF-κB and parvalbumin is increased in Parkinson disease. NeuroReport 15:1715–1718. https://doi.org/10.1097/01.wnr.0000136175.51954.ce
Soula M, Weber RA, Zilka O et al (2020) Metabolic determinants of cancer cell sensitivity to canonical ferroptosis inducers. Nat Chem Biol 16:1351–1360. https://doi.org/10.1038/s41589-020-0613-y
Southon A, Szostak K, Acevedo KM et al (2020) CuII (atsm) inhibits ferroptosis: implications for treatment of neurodegenerative disease. Br J Pharmacol 177:656–667. https://doi.org/10.1111/bph.14881
Sova M, Saso L (2018) Design and development of Nrf2 modulators for cancer chemoprevention and therapy: a review. Drug Des Dev Ther 12:3181–3197. https://doi.org/10.2147/dddt.s172612
Sreedharan J, Blair IP, Tripathi VB et al (2008) TDP-43 mutations in familial and sporadic amyotrophic lateral sclerosis. Science (new York) 319:1668–1672. https://doi.org/10.1126/science.1154584
Sreejayan, Rao MN (1994) Curcuminoids as potent inhibitors of lipid peroxidation. J Pharm Pharmacol 46:1013–1016. https://doi.org/10.1111/j.2042-7158.1994.tb03258.x
Stockwell BR (2022) Ferroptosis turns 10: emerging mechanisms, physiological functions, and therapeutic applications. Cell 185:2401–2421. https://doi.org/10.1016/j.cell.2022.06.003
Stockwell BR, Jiang X (2020) The chemistry and biology of ferroptosis. Cell Chem Biol 27:365–375. https://doi.org/10.1016/j.chembiol.2020.03.013
Stoy N, Mackay GM, Forrest CM et al (2005) Tryptophan metabolism and oxidative stress in patients with Huntington’s disease. J Neurochem 93:611–623. https://doi.org/10.1111/j.1471-4159.2005.03070.x
Strahan ME, Crowe A, Morgan EH (1992) Iron uptake in relation to transferrin degradation in brain and other tissues of rats. Am J Physiol Regul Integr Compar Physiol 263:R924–R929. https://doi.org/10.1152/ajpregu.1992.263.4.r924
Streit WJ, Rotter J, Winter K et al (2022) Droplet degeneration of hippocampal and cortical neurons signifies the beginning of neuritic plaque formation. J Alzheimers Dis 85:1701–1720. https://doi.org/10.3233/jad-215334
Subbarayan MS, Joly-Amado A, Bickford PC, Nash KR (2022) CX3CL1/CX3CR1 signaling targets for the treatment of neurodegenerative diseases. Pharmacol Ther 231:107989. https://doi.org/10.1016/j.pharmthera.2021.107989
Sun J, Brand M, Zenke Y et al (2004) Heme regulates the dynamic exchange of Bach1 and NF-E2-related factors in the Maf transcription factor network. Proc Natl Acad Sci 101:1461–1466. https://doi.org/10.1073/pnas.0308083100
Sun Z, Chin YE, Zhang DD (2009) Acetylation of Nrf2 by p300/CBP augments promoter-specific DNA binding of Nrf2 during the antioxidant response. Mol Cell Biol 29:2658–2672. https://doi.org/10.1128/MCB.01639-08
Sun X, Ou Z, Chen R et al (2016) Activation of the p62-Keap1-NRF2 pathway protects against ferroptosis in hepatocellular carcinoma cells. Hepatology 63:173–184. https://doi.org/10.1002/hep.28251
Sun W, Zheng J, Ma J et al (2021) Increased plasma heme oxygenase-1 levels in patients with early-stage Parkinson’s disease. Front Aging Neurosci 13:621508. https://doi.org/10.3389/fnagi.2021.621508
Suzuki H, Tashiro S, Sun J et al (2003) Cadmium induces nuclear export of Bach1, a transcriptional repressor of heme oxygenase-1 gene. J Biol Chem 278:49246–49253. https://doi.org/10.1074/jbc.m306764200
Suzuki T, Motohashi H, Yamamoto M (2013) Toward clinical application of the Keap1-Nrf2 pathway. Trends Pharmacol Sci 34:340–346. https://doi.org/10.1016/j.tips.2013.04.005
Tabrizi SJ, Leavitt BR, Landwehrmeyer GB et al (2019) Targeting huntingtin expression in patients with Huntington’s disease. N Engl J Med 380:2307–2316. https://doi.org/10.1056/nejmoa1900907
Tabrizi SJ, Flower MD, Ross CA, Wild EJ (2020) Huntington disease: new insights into molecular pathogenesis and therapeutic opportunities. Nat Rev Neurol 16:529–546. https://doi.org/10.1038/s41582-020-0389-4
Tadolini B, Franconi F (1998) Carvedilol inhibition of lipid peroxidation. A new antioxidative mechanism. Free Radical Res 29:377–387. https://doi.org/10.1080/10715769800300421
Taher AT, Saliba AN, Kuo KH et al (2017) Safety and pharmacokinetics of the oral iron chelator SP-420 in β-thalassemia. Am J Hematol 92:1356–1361. https://doi.org/10.1002/ajh.24914
Taylor EM, Crowe A, Morgan EH (1991) Transferrin and iron uptake by the brain: effects of altered iron status. J Neurochem 57:1584–1592. https://doi.org/10.1111/j.1471-4159.1991.tb06355.x
Taylor JP, Brown RH, Cleveland DW (2016) Decoding ALS: from genes to mechanism. Nature 539:197–206. https://doi.org/10.1038/nature20413
Theodore M, Kawai Y, Yang J et al (2008) Multiple nuclear localization signals function in the nuclear import of the transcription factor Nrf2. J Biol Chem 283:8984–8994. https://doi.org/10.1074/jbc.m709040200
Thimmulappa RK, Mai KH, Srisuma S et al (2002) Identification of Nrf2-regulated genes induced by the chemopreventive agent sulforaphane by oligonucleotide microarray. Cancer Res 62:5196–5203
Thor H, Smith MT, Hartzell P et al (1982) The metabolism of menadione (2-methyl-1,4-naphthoquinone) by isolated hepatocytes. A study of the implications of oxidative stress in intact cells. J Biol Chem 257:12419–12425
Tian Y, Lu J, Hao X et al (2020) FTH1 inhibits ferroptosis through ferritinophagy in the 6-OHDA model of Parkinson’s disease. Neurotherapeutics 17:1796–1812. https://doi.org/10.1007/s13311-020-00929-z
Tobore TO (2019) Towards a comprehensive understanding of the contributions of mitochondrial dysfunction and oxidative stress in the pathogenesis and pathophysiology of Huntington’s disease. J Neurosci Res 97:1455–1468. https://doi.org/10.1002/jnr.24492
Todorich B, Pasquini JM, Garcia CI et al (2009) Oligodendrocytes and myelination: the role of iron. Glia 57:467–478. https://doi.org/10.1002/glia.20784
Todorich B, Zhang X, Connor JR (2011) H-ferritin is the major source of iron for oligodendrocytes. Glia 59:927–935. https://doi.org/10.1002/glia.21164
Toki T, Itoh J, Kitazawa J et al (1997) Human small Maf proteins form heterodimers with CNC family transcription factors and recognize the NF-E2 motif. Oncogene 14:1901–1910. https://doi.org/10.1038/sj.onc.1201024
Tripathi AK, Haldar S, Qian J et al (2015) Prion protein functions as a ferrireductase partner for ZIP14 and DMT1. Free Radic Biol Med 84:322–330. https://doi.org/10.1016/j.freeradbiomed.2015.03.037
Tripathi P, Rodriguez-Muela N, Klim JR et al (2017) Reactive astrocytes promote ALS-like degeneration and intracellular protein aggregation in human motor neurons by disrupting autophagy through TGF-β1. Stem Cell Rep 9:667–680. https://doi.org/10.1016/j.stemcr.2017.06.008
Trnka J, Blaikie FH, Smith RAJ, Murphy MP (2008) A mitochondria-targeted nitroxide is reduced to its hydroxylamine by ubiquinol in mitochondria. Free Radic Biol Med 44:1406–1419. https://doi.org/10.1016/j.freeradbiomed.2007.12.036
Tsatsanis A, McCorkindale AN, Wong BX et al (2021) The acute phase protein lactoferrin is a key feature of Alzheimer’s disease and predictor of Aβ burden through induction of APP amyloidogenic processing. Mol Psychiatry 26:5516–5531. https://doi.org/10.1038/s41380-021-01248-1
Tsvetkov AS, Arrasate M, Barmada S et al (2013) Proteostasis of polyglutamine varies among neurons and predicts neurodegeneration. Nat Chem Biol 9:586–592. https://doi.org/10.1038/nchembio.1308
Tucci P, Lattanzi R, Severini C, Saso L (2022) Nrf2 pathway in Huntington’s disease (HD): What is its role? IJMS 23:15272. https://doi.org/10.3390/ijms232315272
Tulpule K, Robinson SR, Bishop GM, Dringen R (2009) Uptake of ferrous iron by cultured rat astrocytes. J Neurosci Res 88:563–571. https://doi.org/10.1002/jnr.22217
Unni S, Deshmukh P, Krishnappa G et al (2021) Structural insights into the multiple binding modes of Dimethyl Fumarate (DMF) and its analogs to the Kelch domain of Keap1. Febs J 288:1599–1613. https://doi.org/10.1111/febs.15485
Ursini F, Maiorino M (2020) Lipid peroxidation and ferroptosis: the role of GSH and GPx4. Free Radic Biol Med 152:175–185. https://doi.org/10.1016/j.freeradbiomed.2020.02.027
Van Harten ACM, Phatnani H, Przedborski S (2021) Non-cell-autonomous pathogenic mechanisms in amyotrophic lateral sclerosis. Trends Neurosci 44:658–668. https://doi.org/10.1016/j.tins.2021.04.008
Van Roon-Mom WM, Pepers BA, ’T Hoen PA et al (2008) Mutant huntingtin activates nrf2-responsive genes and impairs dopamine synthesis in a PC12 model of Huntington’s disease. BMC Mol Biol 9:84. https://doi.org/10.1186/1471-2199-9-84
Vance C, Rogelj B, Hortobágyi T et al (2009) Mutations in FUS, an RNA processing protein, cause familial amyotrophic lateral sclerosis type 6. Science (new York) 323:1208–1211. https://doi.org/10.1126/science.1165942
Vargas MR, Johnson JA (2009) The Nrf2-ARE cytoprotective pathway in astrocytes. Expert Rev Mol Med 11:e17. https://doi.org/10.1017/s1462399409001094
Vargas MR, Pehar M, Cassina P et al (2005) Fibroblast growth factor-1 induces heme oxygenase-1 via nuclear factor erythroid 2-related factor 2 (Nrf2) in spinal cord astrocytes: consequences for motor neuron survival. J Biol Chem 280:25571–25579. https://doi.org/10.1074/jbc.M501920200
Vargas MR, Pehar M, Cassina P et al (2006) Increased glutathione biosynthesis by Nrf2 activation in astrocytes prevents p75NTR-dependent motor neuron apoptosis. J Neurochem 97:687–696. https://doi.org/10.1111/j.1471-4159.2006.03742.x
Vargas MR, Johnson DA, Sirkis DW et al (2008) Nrf2 activation in astrocytes protects against neurodegeneration in mouse models of familial amyotrophic lateral sclerosis. J Neurosci 28:13574–13581. https://doi.org/10.1523/jneurosci.4099-08.2008
Vargas MR, Johnson DA, Johnson JA (2011) Decreased glutathione accelerates neurological deficit and mitochondrial pathology in familial ALS-linked hSOD1(G93A) mice model. Neurobiol Dis 43:543–551. https://doi.org/10.1016/j.nbd.2011.04.025
Vargas MR, Burton NC, Gan L et al (2013) Absence of Nrf2 or its selective overexpression in neurons and muscle does not affect survival in ALS-linked mutant hSOD1 mouse models. PLoS ONE 8:e56625. https://doi.org/10.1371/journal.pone.0056625
Varikasuvu SR, Prasad VS, Kothapalli J, Manne M (2019) Brain selenium in Alzheimer’s disease (BRAIN SEAD study): a systematic review and meta-analysis. Biol Trace Elem Res 189:361–369. https://doi.org/10.1007/s12011-018-1492-x
Varma SJ, Muchowska KB, Chatelain P, Moran J (2018) Native iron reduces CO2 to intermediates and end-products of the acetyl-CoA pathway. Nat Ecol Evol 2:1019–1024. https://doi.org/10.1038/s41559-018-0542-2
Vasconcelos AR, Dos Santos NB, Scavone C, Munhoz CD (2019) Nrf2/ARE pathway modulation by dietary energy regulation in neurological disorders. Front Pharmacol 10:33. https://doi.org/10.3389/fphar.2019.00033
Vassar R, Bennett BD, Babu-Khan S et al (1999) Beta-secretase cleavage of Alzheimer’s amyloid precursor protein by the transmembrane aspartic protease BACE. Science 286:735–741. https://doi.org/10.1126/science.286.5440.735
Viswanathan VS, Ryan MJ, Dhruv HD et al (2017) Dependency of a therapy-resistant state of cancer cells on a lipid peroxidase pathway. Nature 547:453–457. https://doi.org/10.1038/nature23007
von Otter M, Landgren S, Nilsson S et al (2010) Nrf2-encoding NFE2L2 haplotypes influence disease progression but not risk in Alzheimer’s disease and age-related cataract. Mech Ageing Dev 131:105–110. https://doi.org/10.1016/j.mad.2009.12.007
Wan W, Cao L, Kalionis B et al (2019) Iron deposition leads to hyperphosphorylation of tau and disruption of insulin signaling. Front Neurol 10:607. https://doi.org/10.3389/fneur.2019.00607
Wang Y, Santa-Cruz K, DeCarli C, Johnson JA (2000) NAD(P)H:quinone oxidoreductase activity is increased in hippocampal pyramidal neurons of patients with Alzheimer’s disease. Neurobiol Aging 21:525–531. https://doi.org/10.1016/s0197-4580(00)00114-7
Wang H, Liu K, Geng M et al (2013) RXRα inhibits the NRF2-ARE signaling pathway through a direct interaction with the Neh7 domain of NRF2. Cancer Res 73:3097–3108. https://doi.org/10.1158/0008-5472.CAN-12-3386
Wang Q, Li W-X, Dai S-X et al (2017) Meta-analysis of Parkinson’s disease and Alzheimer’s disease revealed commonly impaired pathways and dysregulation of NRF2-dependent genes. J Alzheimers Dis 56:1525–1539. https://doi.org/10.3233/jad-161032
Wang Y, Gao L, Chen J et al (2021a) Pharmacological modulation of Nrf2/HO-1 signaling pathway as a therapeutic target of Parkinson’s disease. Front Pharmacol 12:757161. https://doi.org/10.3389/fphar.2021.757161
Wang Y, Zhang X, Chen F et al (2021b) LRRK2-NFATc2 pathway associated with neuroinflammation may be a potential therapeutic target for Parkinson’s disease. J Inflamm Res 14:2583–2586. https://doi.org/10.2147/JIR.S301531
Wang C, Chen S, Guo H et al (2022a) Forsythoside a mitigates Alzheimer’s-like pathology by inhibiting ferroptosis-mediated neuroinflammation via nrf2/GPX4 axis activation. Int J Biol Sci 18:2075–2090. https://doi.org/10.7150/ijbs.69714
Wang F, Wang J, Shen Y et al (2022b) Iron Dyshomeostasis and ferroptosis: a new Alzheimer’s disease hypothesis? Front Aging Neurosci 14:830569. https://doi.org/10.3389/fnagi.2022.830569
Wang L, An H, Yu F et al (2022c) The neuroprotective effects of paeoniflorin against MPP+-induced damage to dopaminergic neurons via the akt/nrf2/GPX4 pathway. J Chem Neuroanat 122:102103. https://doi.org/10.1016/j.jchemneu.2022.102103
Wang T, Tomas D, Perera ND et al (2022d) Ferroptosis mediates selective motor neuron death in amyotrophic lateral sclerosis. Cell Death Differ 29:1187–1198. https://doi.org/10.1038/s41418-021-00910-z
Ward RJ, Zucca FA, Duyn JH et al (2014) The role of iron in brain ageing and neurodegenerative disorders. Lancet Neurol 13:1045–1060. https://doi.org/10.1016/s1474-4422(14)70117-6
Warnatz H-J, Schmidt D, Manke T et al (2011) The BTB and CNC homology 1 (BACH1) target genes are involved in the oxidative stress response and in control of the cell cycle. J Biol Chem 286:23521–23532. https://doi.org/10.1074/jbc.m111.220178
Watanabe Y, Tsujimura A, Taguchi K, Tanaka M (2017) HSF1 stress response pathway regulates autophagy receptor SQSTM1/p62-associated proteostasis. Autophagy 13:133–148. https://doi.org/10.1080/15548627.2016.1248018
Weiduschat N, Mao X, Hupf J et al (2014) Motor cortex glutathione deficit in ALS measured in vivo with the J-editing technique. Neurosci Lett 570:102–107. https://doi.org/10.1016/j.neulet.2014.04.020
Wenzel SE, Tyurina YY, Zhao J et al (2017) PEBP1 wardens ferroptosis by enabling lipoxygenase generation of lipid death signals. Cell 171:628-641.e26. https://doi.org/10.1016/j.cell.2017.09.044
Wijesekera LC, Nigel Leigh P (2009) Amyotrophic lateral sclerosis. Orphanet J Rare Dis 4:3. https://doi.org/10.1186/1750-1172-4-3
Wong BX, Ayton S, Lam LQ et al (2014a) A comparison of ceruloplasmin to biological polyanions in promoting the oxidation of Fe(2+) under physiologically relevant conditions. Biochim Biophys Acta (BBA) Gen Subj 1840:3299–3310. https://doi.org/10.1016/j.bbagen.2014.08.006
Wong BX, Tsatsanis A, Lim LQ et al (2014b) β-Amyloid precursor protein does not possess ferroxidase activity but does stabilize the cell surface ferrous iron exporter ferroportin. PLoS ONE 9:e114174. https://doi.org/10.1371/journal.pone.0114174
Wood LK, Langford SJ (2014) Motor neuron disease: a chemical perspective. J Med Chem 57:6316–6331. https://doi.org/10.1021/jm5001584
Wood-Allum CA, Barber SC, Kirby J et al (2006) Impairment of mitochondrial anti-oxidant defence in SOD1-related motor neuron injury and amelioration by ebselen. Brain J Neurol 129:1693–1709. https://doi.org/10.1093/brain/awl118
Wu X-F, Block ML, Zhang W et al (2005) The role of microglia in paraquat-induced dopaminergic neurotoxicity. Antioxid Redox Signal 7:654–661. https://doi.org/10.1089/ars.2005.7.654
Wu KC, Cui JY, Klaassen CD (2011) Beneficial role of Nrf2 in regulating NADPH generation and consumption. Toxicol Sci 123:590–600. https://doi.org/10.1093/toxsci/kfr183
Wu T, Zhao F, Gao B et al (2014) Hrd1 suppresses Nrf2-mediated cellular protection during liver cirrhosis. Genes Dev 28:708–722. https://doi.org/10.1101/gad.238246.114
Wu H, Wang Y, Tong L et al (2021) Global research trends of ferroptosis: a rapidly evolving field with enormous potential. Front Cell Dev Biol 9:646311. https://doi.org/10.3389/fcell.2021.646311
Wyss-Coray T (2016) Ageing, neurodegeneration and brain rejuvenation. Nature 539:180–186. https://doi.org/10.1038/nature20411
Yablonska S, Ganesan V, Ferrando LM et al (2019) Mutant huntingtin disrupts mitochondrial proteostasis by interacting with TIM23. Proc Natl Acad Sci 116:16593–16602. https://doi.org/10.1073/pnas.1904101116
Yacoubian TA, Standaert DG (2009) Targets for neuroprotection in Parkinson’s disease. Biochim Biophys Acta (BBA) Mol Basis Dis 1792:676–687. https://doi.org/10.1016/j.bbadis.2008.09.009
Yamanaka K, Chun SJ, Boillee S et al (2008) Astrocytes as determinants of disease progression in inherited amyotrophic lateral sclerosis. Nat Neurosci 11:251–253. https://doi.org/10.1038/nn2047
Yan N, Zhang J-J (2019) The emerging roles of ferroptosis in vascular cognitive impairment. Front Neurosci 13:811. https://doi.org/10.3389/fnins.2019.00811
Yan B, Ai Y, Sun Q et al (2021a) Membrane damage during ferroptosis is caused by oxidation of phospholipids catalyzed by the oxidoreductases POR and CYB5R1. Mol Cell 81:355-369.e10. https://doi.org/10.1016/j.molcel.2020.11.024
Yan H, Pan Y, Liao X et al (2021b) Significantly enhanced Fenton-based oxidation processes with CuS–Cu9S8 as co-catalyst by accelerating the Fe3+/Fe2+ cycles. Appl Surf Sci 559:149952. https://doi.org/10.1016/j.apsusc.2021.149952
Yan R, Xie E, Li Y et al (2022) The structure of erastin-bound xCT-4F2hc complex reveals molecular mechanisms underlying erastin-induced ferroptosis. Cell Res 32:687–690. https://doi.org/10.1038/s41422-022-00642-w
Yang H, Magilnick N, Lee C et al (2005) Nrf1 and Nrf2 regulate rat glutamate-cysteine ligase catalytic subunit transcription indirectly via NF-kappaB and AP-1. Mol Cell Biol 25:5933–5946. https://doi.org/10.1128/mcb.25.14.5933-5946.2005
Yang WS, SriRamaratnam R, Welsch ME et al (2014) Regulation of ferroptotic cancer cell death by GPX4. Cell 156:317–331. https://doi.org/10.1016/j.cell.2013.12.010
Yang WS, Kim KJ, Gaschler MM et al (2016) Peroxidation of polyunsaturated fatty acids by lipoxygenases drives ferroptosis. Proc Natl Acad Sci 113:E4966-4975. https://doi.org/10.1073/pnas.1603244113
Yang C, Han M, Li R et al (2021) Curcumin nanoparticles inhibiting Ferroptosis for the enhanced treatment of intracerebral hemorrhage. Int J Nanomed 16:8049–8065. https://doi.org/10.2147/ijn.s334965
Yang S, Pei T, Xiong Q et al (2022a) Salidroside attenuates neuronal ferroptosis by activating the Nrf2/HO1 signaling pathway in Aβ1-42-induced Alzheimer’s disease mice and glutamate-injured HT22 cells. Chin Med 17:1–18. https://doi.org/10.1186/s13020-022-00634-3
Yang X, Yang R, Zhang F (2022b) Role of Nrf2 in Parkinson’s disease: toward new perspectives. Front Pharmacol 13:919233. https://doi.org/10.3389/fphar.2022.919233
Yao W, Lin S, Su J et al (2021) Activation of BDNF by transcription factor Nrf2 contributes to antidepressant-like actions in rodents. Transl Psychiatry 11:140. https://doi.org/10.1038/s41398-021-01261-6
Ye LF, Chaudhary KR, Zandkarimi F et al (2020) Radiation-induced lipid peroxidation triggers Ferroptosis and synergizes with Ferroptosis inducers. ACS Chem Biol 15:469–484. https://doi.org/10.1021/acschembio.9b00939
Yoo M-H, Gu X, Xu X-M et al (2010) Delineating the role of glutathione peroxidase 4 in protecting cells against lipid hydroperoxide damage and in Alzheimer’s disease. Antioxid Redox Signal 12:819–827. https://doi.org/10.1089/ars.2009.2891
Yoritaka A, Hattori N, Uchida K et al (1996) Immunohistochemical detection of 4-hydroxynonenal protein adducts in Parkinson disease. Proc Natl Acad Sci 93:2696–2701. https://doi.org/10.1073/pnas.93.7.2696
Yu H, Yuan B, Chu Q et al (2019) Protective roles of isoastilbin against Alzheimer’s disease via nrf2-mediated antioxidation and anti-apoptosis. Int J Mol Med 43:1406–1416. https://doi.org/10.3892/ijmm.2019.4058
Yu Y, Jiang L, Wang H et al (2020) Hepatic transferrin plays a role in systemic iron homeostasis and liver ferroptosis. Blood 136:726–739. https://doi.org/10.1182/blood.2019002907
Yuan H, Li X, Zhang X et al (2016) Identification of ACSL4 as a biomarker and contributor of ferroptosis. Biochem Biophys Res Commun 478:1338–1343. https://doi.org/10.1016/j.bbrc.2016.08.124
Zarruk JG, Berard JL, Passos Dos Santos R et al (2015) Expression of iron homeostasis proteins in the spinal cord in experimental autoimmune encephalomyelitis and their implications for iron accumulation. Neurobiol Dis 81:93–107. https://doi.org/10.1016/j.nbd.2015.02.001
Zawada WM, Banninger GP, Thornton J et al (2011) Generation of reactive oxygen species in 1-methyl-4-phenylpyridinium (MPP+) treated dopaminergic neurons occurs as an NADPH oxidase-dependent two-wave cascade. J Neuroinflamm 8:129. https://doi.org/10.1186/1742-2094-8-129
Zeng X, An H, Yu F et al (2021) Benefits of iron chelators in the treatment of Parkinson’s disease. Neurochem Res 46:1239–1251. https://doi.org/10.1007/s11064-021-03262-9
Zgorzynska E, Dziedzic B, Walczewska A (2021) An overview of the Nrf2/ARE pathway and its role in neurodegenerative diseases. Int J Mol Sci 22:9592. https://doi.org/10.3390/ijms22179592
Zhang DD (2006) Mechanistic studies of the Nrf2-Keap1 signaling pathway. Drug Metab Rev 38:769–789. https://doi.org/10.1080/03602530600971974
Zhang DD, Lo S-C, Cross JV et al (2004) Keap1 is a redox-regulated substrate adaptor protein for a Cul3-dependent ubiquitin ligase complex. Mol Cell Biol 24:10941–10953. https://doi.org/10.1128/mcb.24.24.10941-10953.2004
Zhang DD, Lo S-C, Sun Z et al (2005a) Ubiquitination of Keap1, a BTB-Kelch substrate adaptor protein for Cul3, targets Keap1 for degradation by a proteasome-independent pathway. J Biol Chem 280:30091–30099. https://doi.org/10.1074/jbc.m501279200
Zhang W, Wang T, Pei Z et al (2005b) Aggregated alpha-synuclein activates microglia: a process leading to disease progression in Parkinson’s disease. Faseb J 19:533–542. https://doi.org/10.1096/fj.04-2751com
Zhang X, Surguladze N, Slagle-Webb B et al (2006) Cellular iron status influences the functional relationship between microglia and oligodendrocytes. Glia 54:795–804. https://doi.org/10.1002/glia.20416
Zhang X, Guo J, Wei X et al (2018) Bach1: function, regulation, and involvement in disease. Oxid Med Cell Longev 2018:1–8. https://doi.org/10.1155/2018/1347969
Zhang C, Yang Y, Liang W et al (2019a) Neuroprotection by urate on the mutant hSOD1-related cellular and Drosophila models of amyotrophic lateral sclerosis: Implication for GSH synthesis via activating Akt/GSK3β/Nrf2/GCLC pathways. Brain Res Bull 146:287–301. https://doi.org/10.1016/j.brainresbull.2019.01.019
Zhang M, Teng C, Wu F et al (2019b) Edaravone attenuates traumatic brain injury through anti-inflammatory and anti-oxidative modulation. Exp Ther Med 18:467–474. https://doi.org/10.3892/etm.2019.7632
Zhang Y, Tan H, Daniels JD et al (2019c) Imidazole ketone erastin induces Ferroptosis and slows tumor growth in a mouse lymphoma model. Cell Chem Biol 26:623-633.e9. https://doi.org/10.1016/j.chembiol.2019.01.008
Zhang H-L, Hu B-X, Li Z-L et al (2022a) PKCβII phosphorylates ACSL4 to amplify lipid peroxidation to induce ferroptosis. Nat Cell Biol 24:88–98. https://doi.org/10.1038/s41556-021-00818-3
Zhang X, Wu S, Guo C et al (2022b) Vitamin E exerts neuroprotective effects in pentylenetetrazole kindling epilepsy via suppression of Ferroptosis. Neurochem Res 47:739–747. https://doi.org/10.1007/s11064-021-03483-y
Zhang R-F, Zeng M, Lv N et al (2023) Ferroptosis in neurodegenerative diseases: inhibitors as promising candidate mitigators. Eur Rev Med Pharmacol Sci 27:46–65. https://doi.org/10.26355/eurrev_202301_30852
Zhao X, Sun G, Ting S-M et al (2015) Cleaning up after ICH: the role of Nrf2 in modulating microglia function and hematoma clearance. J Neurochem 133:144–152. https://doi.org/10.1111/jnc.12974
Zhao R, Jiang S, Zhang L, Yu Z (2019) Mitochondrial electron transport chain, ROS generation and uncoupling (review). Int J Mol Med 44:3–15. https://doi.org/10.3892/ijmm.2019.4188
Zheng J, Jiang R, Chen M et al (2018) Multi-copper ferroxidase-deficient mice have increased brain iron concentrations and learning and memory deficits. J Nutr 148:643–649. https://doi.org/10.1093/jn/nxy012
Zheng K, Dong Y, Yang R et al (2021) Regulation of ferroptosis by bioactive phytochemicals: implications for medical nutritional therapy. Pharmacol Res 168:105580. https://doi.org/10.1016/j.phrs.2021.105580
Zhu H, Jia Z, Mahaney JE et al (2007) The highly expressed and inducible endogenous NAD(P)H:quinone oxidoreductase 1 in cardiovascular cells acts as a potential superoxide scavenger. Cardiovasc Toxicol 7:202–211. https://doi.org/10.1007/s12012-007-9001-z
Zhu H, Huang J, Chen Y et al (2022) Resveratrol pretreatment protects neurons from oxygen–glucose deprivation/reoxygenation and ischemic injury through inhibiting ferroptosis. Biosci Biotechnol Biochem 86:704–716. https://doi.org/10.1093/bbb/zbac048
Zoungrana LI, Krause-Hauch M, Wang H et al (2022) The interaction of mTOR and Nrf2 in neurogenesis and its implication in neurodegenerative diseases. Cells 11:2048. https://doi.org/10.3390/cells11132048
Zuccato C, Cattaneo E (2014) Huntington’s disease. Handb Exp Pharmacol 220:357–409. https://doi.org/10.1007/978-3-642-45106-5_14
Zuccato C, Valenza M, Cattaneo E (2010) Molecular mechanisms and potential therapeutical targets in Huntington’s disease. Physiol Rev 90:905–981. https://doi.org/10.1152/physrev.00041.2009
Zuo X, Zhou J, Li Y et al (2021) TDP-43 aggregation induced by oxidative stress causes global mitochondrial imbalance in ALS. Nat Struct Mol Biol 28:132–142. https://doi.org/10.1038/s41594-020-00537-7
Funding
This work was supported by the National Natural Science Foundation of China (Grant No. 81673227) and the Natural Science Foundation of Hunan Province (Grant No. 2020JJ4080).
Author information
Authors and Affiliations
Contributions
Writing—original draft preparation, reviewing and editing, YX; Conceptualization, XS; Supervision, funding acquisition and manuscript revision, DL.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Xiang, Y., Song, X. & Long, D. Ferroptosis regulation through Nrf2 and implications for neurodegenerative diseases. Arch Toxicol 98, 579–615 (2024). https://doi.org/10.1007/s00204-023-03660-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00204-023-03660-8