Abstract
Summary
Bone strength estimates are important for fracture prevention. This study compared bone strength changes in postmenopausal women with low bone mass who were assigned to 12 months of exercise, a bone medication, or control. Exercise and bone medications benefited structure at the hip. Structure should be considered in fracture prevention research.
Purpose
Exercise and bisphosphonates reduce fracture risk, but their impact on estimates of bone strength remains uncertain. This study compared changes in tibial bone strength using peripheral quantitative computed tomography (pQCT) and hip structure analysis (HSA) outcomes from dual-energy X-ray absorptiometry (DXA) scans in postmenopausal women with low bone mass assigned to 12 months of exercise, risedronate, or control.
Methods
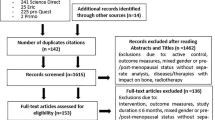
In this RCT, 276 postmenopausal women within 6 years of menopause were randomly assigned to three groups: exercise (92), risedronate (91), or control (93). Exercise included weighted jogging and progressive resistance exercises; risedronate treatment was 150 mg monthly; all groups received calcium and vitamin D. pQCT and DXA images were obtained at baseline and 6 and 12 months and compared between groups over time.
Results
Participants had a mean (± SD) age of 54.5 (± 3.2) years with an average of 36.7 (± 40.7) months postmenopause. No significant differences were found between groups for the change in pQCT outcomes (volumetric bone mineral density, area, and strength estimates). At 12 months, mean percent differences (95% CI) in HSA measures between exercise and controls were as follows: intertrochanteric, cross-sectional area 2.25% (0.28, 4.12) (p = .03), cross-sectional moment of inertia (CSMI) 5.67% (1.47, 9.87) (p < .01), and section modulus (SM) 4.38% (1.02, 7.74) (p = .01), and narrow neck, average cortical thickness 2.37% (−0.08, 4.83) (p = .031). Mean percent differences (95% CI) in HSA measures between risedronate and control were as follows: intertrochanteric, CSMI 4.28% (−0.24, 8.81) (p = .03) and SM 3.35% (−0.21, 6.91) (p = .03), and shaft, subperiosteal width 0.82% (0.05, 1.58) (p = .047), CSMI 2.53% (0.88, 4.18) (p = .004), and SM 1.57% (0.34, 2.8) (p = .008). Exercise maintained neck-shaft angle compared to both control 1.27% (0.13, 2.41) (p = .04) and risedronate 1.31% (0.23, 2.39) (p = .03). All other differences for changes in HSA outcomes over time were not significantly different between the exercise and risedronate groups.
Conclusion
Exercise and bisphosphonates may influence structural and strength estimates at the hip, but not at peripheral sites (tibia). Neither exercise nor bisphosphonates were found to be superior in improving estimates of hip bone strength.

Similar content being viewed by others
Data availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Reid IR (2020) A broader strategy for osteoporosis interventions. Nat Rev Endocrinol 16(6):333–339
Sarafrazi N, Wambogo EA, Shepherd JA (2021) Osteoporosis or low bone mass in older adults: United States, 2017-2018. NCHS Data Brief 405:1–8
Cecchi F et al (2018) Predictors of recovering ambulation after hip fracture inpatient rehabilitation. BMC Geriatr 18(1):201
Guzon-Illescas O et al (2019) Mortality after osteoporotic hip fracture: incidence, trends, and associated factors. J Orthop Surg Res 14(1):203–203
Downey C, Kelly M, Quinlan JF (2019) Changing trends in the mortality rate at 1-year post hip fracture - a systematic review. World J Orthop 10(3):166–175
Eriksen EF (2012) Treatment of osteopenia. Rev Endocr Metab Disord 13(3):209–223
Kling JM, Clarke BL, Sandhu NP (2014) Osteoporosis prevention, screening, and treatment: a review. J Women's Health 23(7):563–572
de Souto Barreto P et al (2019) Association of long-term exercise training with risk of falls, fractures, hospitalizations, and mortality in older adults: a systematic review and meta-analysis. JAMA Intern Med 179(3):394–405
Fonseca H et al (2014) Bone quality: the determinants of bone strength and fragility. Sports Med 44(1):37–53
Kerr D et al (1996) Exercise effects on bone mass in postmenopausal women are site-specific and load-dependent. J Bone Miner Res 11(2):218–225
Bandaru S et al (2020) Do patients that fracture with normal DXA-measured BMD have normal bone? Arch Osteoporos 15(1):70
Schuit SC et al (2004) Fracture incidence and association with bone mineral density in elderly men and women: the Rotterdam study. Bone 34(1):195–202
Bouxsein ML, Seeman E (2009) Quantifying the material and structural determinants of bone strength. Best Pract Res Clin Rheumatol 23(6):741–753
Tella SH, Gallagher JC (2014) Prevention and treatment of postmenopausal osteoporosis. J Steroid Biochem Mol Biol 142:155–170
Bonnick SL et al (2009) DXA-based hip structural analysis of once-weekly bisphosphonate-treated postmenopausal women with low bone mass. Osteoporos Int 20(6):911–921
Hans D et al (2023) Long-term effect of denosumab on bone microarchitecture as assessed by tissue thickness-adjusted trabecular bone score in postmenopausal women with osteoporosis: results from FREEDOM and its open-label extension. Osteoporos Int 34(6):1075–1084. https://doi.org/10.1007/s00198-023-06708-8
Watson SL et al (2018) High-intensity resistance and impact training improves bone mineral density and physical function in postmenopausal women with osteopenia and osteoporosis: the LIFTMOR randomized controlled trial. J Bone Miner Res 33(2):211–220
Kemmler W et al (2020) Effects of different types of exercise on bone mineral density in postmenopausal women: a systematic review and meta-analysis. Calcif Tissue Int 107(5):409–439
Shojaa M et al (2020) Effects of dynamic resistance exercise on bone mineral density in postmenopausal women: a systematic review and meta-analysis with special emphasis on exercise parameters. Osteoporos Int 31(8):1427–1444
Mohammad Rahimi GR et al (2020) The impact of different modes of exercise training on bone mineral density in older postmenopausal women: a systematic review and meta-analysis research. Calcif Tissue Int 106(6):577–590
Polidoulis I, Beyene J, Cheung AM (2012) The effect of exercise on pQCT parameters of bone structure and strength in postmenopausal women--a systematic review and meta-analysis of randomized controlled trials. Osteoporos Int 23(1):39–51
Hamilton CJ, Swan VJD, Jamal SA (2010) The effects of exercise and physical activity participation on bone mass and geometry in postmenopausal women: a systematic review of pQCT studies. Osteoporos Int 21(1):11–23
Uusi-Rasi K et al (2003) Effect of alendronate and exercise on bone and physical performance of postmenopausal women: a randomized controlled trial. Bone 33(1):132–143
Karinkanta S et al (2009) Maintenance of exercise-induced benefits in physical functioning and bone among elderly women. Osteoporos Int 20(4):665–674
Adami S et al (1999) Site-specific effects of strength training on bone structure and geometry of ultradistal radius in postmenopausal women. J Bone Miner Res 14(1):120–124
Shevroja E et al (2021) DXA parameters, trabecular bone score (TBS) and bone mineral density (BMD), in fracture risk prediction in endocrine-mediated secondary osteoporosis. Endocrine 74(1):20–28
Waltman N et al (2022) Bone-loading exercises versus risedronate for the prevention of osteoporosis in postmenopausal women with low bone mass: a randomized controlled trial. Osteoporos Int 33(2):475–486
Bilek LD et al (2016) Protocol for a randomized controlled trial to compare bone-loading exercises with risedronate for preventing bone loss in osteopenic postmenopausal women. BMC Womens Health 16(1):59
Waltman N et al (2021) Promoting adherence to bone-loading exercises in postmenopausal women with low bone mass. J Am Assoc Nurse Pract 34(1):50–61. https://doi.org/10.1097/JXX.0000000000000564
Blew RM et al (2014) Standardizing evaluation of pQCT image quality in the presence of subject movement: qualitative versus quantitative assessment. Calcif Tissue Int 94(2):202–211
Davidson M, de Morton N (2007) A systematic review of the Human activity profile. Clin Rehabil 21(2):151–162
Beck TJ (2007) Extending DXA beyond bone mineral density: understanding hip structure analysis. Curr Osteoporos Rep 5(2):49–55
Kemmler W et al (2002) Exercise effects on fitness and bone mineral density in early postmenopausal women: 1-year EFOPS results. Med Sci Sports Exerc 34(12):2115–2123
Flores LE et al (2022) Risedronate or exercise for lean mass preservation during menopause: secondary analysis of a randomized controlled trial. JCSM Rapid Commun 5(2):154–161
Beck, T. Hip structural analysis (HSA) program (BMD and structural geometry methodology) as used to create NHANES III dataset. 2002 [cited 2021 Nov 8, 2021]. https://wwwn.cdc.gov/nchs/data/nhanes3/17a/hip_methods.pdf.
Kaptoge S et al (2008) Prediction of incident hip fracture risk by femur geometry variables measured by hip structural analysis in the study of osteoporotic fractures. J Bone Miner Res 23(12):1892–1904
Ahlborg HG et al (2005) Contribution of hip strength indices to hip fracture risk in elderly men and women. J Bone Miner Res 20(10):1820–1827
Pellikaan P et al (2018) Ranking of osteogenic potential of physical exercises in postmenopausal women based on femoral neck strains. PLoS One 13(4):e0195463
Zhu K et al (2023) Relationships between longitudinal changes in body composition and bone mineral density in middle-to-older aged Australians. Osteoporos Int 34(9):1601–1611. https://doi.org/10.1007/s00198-023-06773-z
Pazianas M, van der Geest S, Miller P (2014) Bisphosphonates and bone quality. BoneKEy Rep 3:529–529
Takada J et al (2011) Hip structure analysis of bisphosphonate-treated Japanese postmenopausal women with osteoporosis. J Bone Miner Metab 29(4):458–465
van Londen GJ et al (2008) Effect of risedronate on hip structural geometry: a 1-year, double-blind trial in chemotherapy-induced postmenopausal women. Bone 43(2):274–278
Wang J et al (2013) Trabecular plate loss and deteriorating elastic modulus of femoral trabecular bone in intertrochanteric hip fractures. Bone Res 1(1):346–354
Kistler-Fischbacher M et al (2022) High-intensity exercise and geometric indices of hip bone strength in postmenopausal women on or off bone medication: The MEDEX-OP Randomised Controlled Trial. Calcif Tissue Int 111(3):256–266
Nagaraj N et al (2019) Longitudinal changes in hip geometry in relation to the final menstrual period: Study of Women’s Health Across the Nation (SWAN). Bone 122:237–245
Acknowledgements
The authors acknowledge the excellent work and contributions of the study team including Dr. Melissa Manzer, Kara Smith, Mel Meisinger, Cherie Kimble, and Nebraska Medicine Department of Radiology Staff. Language learning models (LLMs) were used to assess grammar and readability.
Funding
Research reported in this publication was supported by the National Institute of Nursing Research of the National Institutes of Health under award number R01NR015029.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
None.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Blay, R., Flores, L., Kupzyk, K. et al. Twelve-month resistance and impact exercise program or risedronate provides a relative benefit to hip bone structure in postmenopausal women: results from a randomized controlled trial. Osteoporos Int 35, 877–891 (2024). https://doi.org/10.1007/s00198-023-07008-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-023-07008-x