Abstract
Introduction and hypothesis
Persistent postpartum voiding dysfunction (P-PPVD) is defined as the inability to empty the bladder properly 72 h after delivery despite the use of intermittent urinary catheterization. Our aim was to find predictive factors for P-PPVD and to compare its urogynecologic outcomes with transient dysfunctions.
Materials and methods
A case-control study was performed in a university hospital center between January 2018 and April 2019. The case group included women diagnosed with P-PPVD after vaginal delivery, and the control group included women with PPVD that resolved before 72 h. Patients were followed up at 12 weeks and 12 months postpartum, including an ultrasound assessment of the levator ani muscle (LAM).
Results
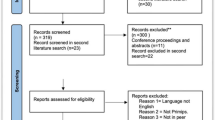
Of 2308 deliveries, 1894 (81%) were vaginal, 75 (3.85%) presented PPVD, and 1 lasted > 72 h (0.69% P-PPVD). LAM avulsion (OR 6.3, 95% CI 1.24–32.01) was the only independent risk factor for P-PPVD found. No significant differences in urogynecologic symptoms between transient and persistent PPVD were found in the short and the long term, except that women with P-PPVD had a lower prevalence of urinary incontinence at 12 weeks postpartum.
Conclusions
PPVD is a common, self-limited event, but in 17.3% of cases persists > 3 days. Levator ani muscle avulsion acts as an independent risk factor for P-PPVD. Early diagnosis and appropriate treatment of P-PPVD can help minimize any clinical implications for long-term urogynecologic disorders.


Similar content being viewed by others
Abbreviations
- PPVD:
-
postpartum voiding dysfunction
- PVR:
-
postvoid residual bladder volume
- P-PPVD:
-
persistent postpartum voiding dysfunction
- CIC:
-
clean intermittent catheterization
- ICIQ-UI SF:
-
International Consultation on Incontinence Questionnaire-Urinary Incontinence Short Form
- B-SAQ:
-
Bladder Control Self-assessment Questionnarie
- UDI-6:
-
Urinary Distress Inventory-6
- LAM:
-
levator ani muscle
- POP:
-
pelvic organ prolapse
- CI:
-
confidence interval
- OR:
-
odds ratio
- OASIS:
-
obstetric anal sphincter injury
References
Yip S, Brieger G, Hin L, Chung T. Urinary retention in the postpartum period: the relationship between obstetric factors and postpartum postvoid residual bladder volume. Acta Obstet Gynecol Scand. 1997;76:667–72.
Mulder F, Hakvoort R, Bruin J, Janszen E, Van der Post J, Roovers J. Long-term micturition problems of asymptomatic postpartum urinary retention: a prospective case-control study. Int Urogynecol J. 2018;29:481–8.
Cavkaytar S, Kokanali M, Baylas A, Topçu H, Laleli B, Tasçi Y. Posptartum urinary retention after vaginal delivery: assessment of risk factors in a case-control study. J Turk Ger Gynecol Assoc. 2014;15:140–3.
Perú G, González-Díaz E, Fernández-Fernández C, Fernández-Corona A. Prevalence of postpartum voiding dysfunction and related risk factors. Urology. 2020.
Glavind K, Bjork J. Incidence and treatment of urinar y retention postpartum. Int Urogynecol J Pelvic Floor Dysfunct. 2003;14:119–21.
Choe W, Kwang N, Atan I, Lim P. Acceptable postvoid residual urine volume after vaginal delivery and its association with various obstetric parameters. Obstet Gynecol Int. 2018. p. 1–7.
Liang C, Chang S, Tseng L, Hsieh C, Chung C, Cheng P. Postpartum urinary retention: assessment of contributing factors and long-term clinical impact. Aust NZJ Obstet Gynaecol. 2002;42:365–8.
Carley M, Carly J, Vasdey G, Lesnick T, Webb M, Ramin K, et al. Factors that are associated with clinically overt postpartum urinary retention after vaginal delivery. Am J Obstet Gyencol. 2002;187:430–3.
Groutz A, Gordon D, Wolman I, Jaffa A, Kupferminc M, Lessing J. Persistent postpartum urinary retention in contemporary obstetric practice. Definition, prevalence and clinical implications. J Reprod Med. 2001;46(1):44–8.
Groutz A, Levin I, Gold R, Pauzner D, Lessing J, Gordon D. Protracted postpartum urinary retention: the importance of early diagnosis and timely intervention. Neurourol Urodyn. 2011;30(1):83–6.
Mevorach Zussman N, Gonen N, Kovo M, Miremberg H, Bar J, Condrea A, et al. Protracted postpartum urinary retention—a long-term problema or a transient condition? Int Urogynecol J. 2020 Mar;31(3):513–9.
Mulder F, Hakvoort R, Bruin J, Van der Post J, Roovers J. Comparison of clean intermittent and transurethral indwelling catheterization for the treatment of over urinary retention after vaginal delivery: a multicenter randomized controlled clincal trial. Int Urogynecol J. 2018;29:1281–7.
Asimakopoulos A, De Nunzio C, Kocjancic E, Tubaro A, Rosier P, Finazzi-Agro E. Measurement of post-void residual urine. Neurourol Urodyn. 2016;35(1):55–7.
González-Díaz E, García-Mejido J, Martín-Martínez A, Fernández-Fernández C, Ortega I, Medina M, et al. Are there differences in the damage to the pelvic floor between Malmstrom's and kiwi omnicup vacuums? A multicenter study. Neurourol Urodyn. 2019;39(1):190–6.
Shek K, Dietz H. Intrapartum risk factors for levator trauma. BJOG. 2010;117:1485–92.
Weinstein M, Jung S, Pretorius D, Nager C, Den Boer D, Mittal R. The reliability of puborectalis muscle measurements with 3-dimensional ultrasound imaging. Am J Obstet Gynecol. 2007;197(68):168.
Dietz H, Bernando M, Kirby A, Shek K. Minimal criteria for the diagnosis of avulsion of the puborectalis muscle by tomographic ultrasound. Int Urogynecol J. 2011;22:699–704.
Grupo de trabajo de la Guía de Práctica Clínica sobre Atención al Parto Normal. Guía de Práctica Clínica sobre la Atención al Parto Normal. Plan de Calidad para el Sistema Nacional de Salud del Ministerio de Sanidad y Política Social. Guías de Práctica Clínica en el SNS: OSTEBA. 2010;2009/01.
Mulder F, Shoffelmeer M, Hakvoort R, Limpens J, Mol B, Van der Post J, et al. Risk factors for postpartum urinary retention: a systematic review and meta-analysis. BJOG. 2012;119:1440–6.
Lim J. Postpartum voiding dysfunction and urinary retention. Aust NZ J Obstet Gynaecol. 2010;50:502–5.
Ching-Chung L, Shuenn-Dhy C, Ling-Hong T, Ching C, Chao-Lun C, Po-Jen C. Postpartum urinary retention: assessment of contributory factors and long term clinical impact. Aust NZ J Obstet Gyencol. 2002;42:365–8.
Teo R, Punter J, Abrams K, Mayne C, Tincello D. Clinically overt postpartum urinary retention after vaginal delivery: a retrospective case-control study. Int Urogynecol J Pelvic. 2007;18(5):521–4.
Albrich S, Laterza R, Skala C, Salvatore S, Koelbl H, Naumann G. Impact of mode of delivery on levator morphology: a prospective observational study with three-dimensional ultrasound early in the postpartum period. BJOG. 2011;119:51–61.
Falkert A, Endress E, Weigl M, Seelbach-Gober B. Three-dimensional ultrasound of the pelvic floor 2 days after first delivery: influence of constitutional and obstetric factors. Ultrasound Obstet Gynecol. 2010;35:583–8.
Dietz H, Kirby A, Shek K, Bedwell P. Does avulsion of the puborectalis muscle affect bladder function? Int Urogynecol J. 2009;20:967–72.
Dietz H, Haylen B, Vancaillie T. Female pelvic organ prolapse and voiding function. Int Urogynecol J. 2002;13(5):284–8.
Eisenberg V, Chantarsorn V, Shek K, Dietz H. Does levator ani injury affect cystocele type? Ultrasound Obstet Gynecol. 2010;36:618–23.
Duenas Garcia O, Rico H, Gorbea-Sánchez V, Herrerias-Canedo T. Bladder rupture caused by postpartum urinary retention. Obstet Gynecol. 2008;112:481–2.
Yip S, Sahota D, Chang A, Chung T. Four-year follow-up of women who were diagnosed to have postpartum urinary retention. Am J Obstet Gynecol. 2002;187(3):648–52.
Andolf E, Iosin C, Jörgensen C, Rhydström H. Insidious urinary retention after vaginal delivery: prevalence and symptoms at follow-up in a population-based study. Gynecol Obstet Invest. 1994;38:51–3.
Author information
Authors and Affiliations
Contributions
• E Gonzalez Diaz: Conception and design, Data collection, Data analysis, Manuscript writing.
• G Perú Biurrun: Manuscript writing.
• C Fernandez Fernandez: Supervision.
• A Fernandez Corona: Supervision.
All authors assisted in critical revision of the manuscript and have read and approved the final version of the article.
Corresponding author
Ethics declarations
Conflict of interest
None.
Details of ethics approval
Approval for the study was given by the local Research Ethics Board (Comité Ético de Investigación Clínica de León).
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 15 kb)
Rights and permissions
About this article
Cite this article
Gonzalez-Díaz, E., Biurrun, G.P. Levator ani muscle avulsion: a risk factor for persistent postpartum voiding dysfunction. Int Urogynecol J 31, 2327–2335 (2020). https://doi.org/10.1007/s00192-020-04412-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-020-04412-3