Abstract
Introduction and hypothesis
We hypothesized whether a non-episiotomy protocol or administration of selective episiotomy as an intrapartum intervention would modify the incidence of obstetric anal sphincter injuries (OASIS).
Methods
We registered this systematic review with the PROSPERO database (CRD42018111018). Prospective randomized controlled trials (RCTs) were included from databases until February 2019. The primary outcome was OASIS, and the secondary outcomes were any perineal trauma, duration of the second stage of labor, instrumental delivery, and post-partum hemorrhage. The risk of bias (Cochrane Handbook) and the Grading of Recommendations, Assessment, Development and Evaluations (GRADE) criteria were used to assess the RCTs.
Results
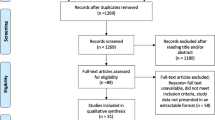
A total of 1,833 results (PubMed 650, SCOPUS 1,144, Cochrane Library 33, LILACS 6) were obtained. However, only 2 studies fulfilled the criteria for quantitative analysis and meta-analysis (n = 574). The non-episiotomy arm included two episiotomies (1.7% of deliveries), whereas the selective episiotomy included 33 episiotomies (21.4%). Performance of selective episiotomy demonstrated no difference compared with that of the non-episiotomy group with regard to OASIS (OR = 0.46 [0.15–1.39]; n = 543; I2 = 0%,p = 0.17), any perineal trauma (OR = 0.90 [0.61–1.33]; I2 = 0%, n = 546, p = 0.59), instrumental delivery (OR = 1.40 [0.80–2.45]; I2 = 0%, n = 545, p = 0.24), duration of the second stage of labor (MD = -3.71 [−21.56, 14.14]; I2 = 72%,n = 546, p = 0.68), perineal pain (MD = 0.59 [0.01–1.17]; I2 = 0%,p = 0.05), and post-partum hemorrhage (OR = 1.75 [0.87–3.54]; I2 = 0%,n = 546,p = 0.12). The evaluated studies displayed a low risk of bias in at least four of the seven categories analyzed. GRADE demonstrated a low certainty for severe perineal tears, postpartum hemorrhage, duration of the second stage of labor, and a moderate certainty for any perineal tear.
Conclusions
There was no significant difference between non-episiotomy and selective episiotomy regarding OASIS. No RCT was able to confirm a benefit of the non-performance of episiotomies in the non-episiotomy arm.



Similar content being viewed by others
References
Sioutis D, Thakar R, Sultan AH. Overdiagnosis and rising rate of obstetric anal sphincter injuries (OASIS): time for reappraisal. Ultrasound Obstet Gynecol. 2017;50(5):642–7.
Dietz HP, Pardey J, Murray H. Pelvic floor and anal sphincter trauma should be key performance indicators of maternity services. Int Urogynecol J. 2015;26(1):29–32.
Hartmann K, Viswanathan M, Palmieri R, Gartlehner G, Thorp J Jr, Lohr KN. Outcomes of routine episiotomy: a systematic review. JAMA. 2005;293(17):2141–8.
Verghese TS, Champaneria R, Kapoor DS, Latthe PM. Obstetric anal sphincter injuries after episiotomy: systematic review and meta-analysis. Int Urogynecol J. 2016;27(10):1459–67.
Lund NS, Persson LK, Jango H, Gommesen D, Westergaard HB. Episiotomy in vacuum-assisted delivery affects the risk of obstetric anal sphincter injury: a systematic review and meta-analysis. Eur J Obstet Gynecol Reprod Biol. 2016;207:193–9.
Gonzalez-Diaz E, Fernandez Fernandez C, Gonzalo Orden JM, Fernandez CA. Which characteristics of the episiotomy and perineum are associated with a lower risk of obstetric anal sphincter injury in instrumental deliveries. Eur J Obstet Gynecol Reprod Biol. 2019;233:127–33.
Lins VML, Katz L, Vasconcelos FBL, Coutinho I, Amorim MM. Factors associated with spontaneous perineal lacerations in deliveries without episiotomy in a university maternity hospital in the city of Recife, Brazil: a cohort study. J Matern Fetal Neonatal Med. 2019;32(18):3062–7.
Shmueli A, Gabbay Benziv R, Hiersch L, et al. Episiotomy—risk factors and outcomes. J Matern Fetal Neonatal Med. 2017;30(3):251–6.
McDonald EA, Gartland D, Small R, Brown SJ. Dyspareunia and childbirth: a prospective cohort study. BJOG. 2015;122(5):672–9.
Panic N, Leoncini E, De Belvis G, Ricciardi W, Boccia S. Evaluation of the endorsement of the preferred reporting items for systematic reviews and meta-analysis (PRISMA) statement on the quality of published systematic review and meta-analyses. PLoS One. 2013;8(12):e83138.
Liberati A, Altman DG, Tetzlaff J, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. PLoS Med. 2009;6(7):e1000100.
Booth A, Moher D, Ghersi D, et al. The nuts and bolts of PROSPERO: an international prospective register of systematic reviews. Syst Rev. 2012;1(1):2.
Higgins JP, Green S. Cochrane handbook for systematic reviews of interventions, vol 4. Wiley, New York; 2011.
Guyatt GH, Oxman AD, Vist G, et al. GRADE guidelines: 4. Rating the quality of evidence—study limitations (risk of bias). J Clin Epidemiol. 2011;64(4):407–15.
Sagi-Dain L, Bahous R, Caspin O, Kreinin-Bleicher I, Gonen R, Sagi S. No episiotomy versus selective lateral/mediolateral episiotomy (EPITRIAL): an interim analysis. Int Urogynecol J. 2018;29(3):415–23.
Amorim MM, Coutinho IC, Melo I, Katz L. Selective episiotomy vs. implementation of a non-episiotomy protocol: a randomized clinical trial. Reprod Health. 2017;14(1):55.
Gachon B, Fradet Menard C, Pierre F, Fritel X. Does the implementation of a restrictive episiotomy policy for operative deliveries increase the risk of obstetric anal sphincter injury? Arch Gynecol Obstet. 2019;300(1):87–94.
Smith LA, Price N, Simonite V, Burns EE. Incidence of and risk factors for perineal trauma: a prospective observational study. BMC Pregnancy Childbirth. 2013;13:59.
LaCross A, Groff M, Smaldone A. Obstetric anal sphincter injury and anal incontinence following vaginal birth: a systematic review and meta-analysis. J Midwifery Womens Health. 2015;60(1):37–47.
Oliveira LS, Brito LG, Quintana SM, Duarte G, Marcolin AC. Perineal trauma after vaginal delivery in healthy pregnant women. Sao Paulo Med J. 2014;132(4):231–8.
Peppe MV, Stefanello J, Infante BF, Kobayashi MT, Baraldi CO, Brito LGO. Perineal trauma in a low-risk maternity with high prevalence of upright position during the second stage of labor. Rev Bras Ginecol Obstet. 2018;40(7):379–83.
Monteiro MVD, Pereira GMV, Aguiar RAP, Azevedo RL, Correia MD, Reis ZSN. Risk factors for severe obstetric perineal lacerations. Int Urogynecol J. 2016;27(1):61–7.
Evers EC, Blomquist JL, McDermott KC, Handa VL. Obstetrical anal sphincter laceration and anal incontinence 5–10 years after childbirth. Am J Obstet Gynecol. 2012;207(5):425.e1–6.
Committee on Practice Bulletins—Obstetrics. ACOG Practice Bulletin no. 154: operative vaginal delivery. Obstet Gynecol. 2015;126(5):e56–65.
RCOG. Operative vaginal delivery. Green-top guideline 26. London: RCOG; 2011.
Martin JA, Hamilton BE, Osterman MJ, Curtin SC, Matthews TJ. Births: final data for 2013. Natl Vital Stat Rep. 2015;64(1):1–65.
Frankman EA, Wang L, Bunker CH, Lowder JL. Episiotomy in the United States: has anything changed? Am J Obstet Gynecol. 2009;200(5):573.e1–7.
Simic M, Cnattingius S, Petersson G, Sandstrom A, Stephansson O. Duration of second stage of labor and instrumental delivery as risk factors for severe perineal lacerations: population-based study. BMC Pregnancy Childbirth. 2017;17(1):72.
Gurol-Urganci I, Cromwell DA, Edozien LC, et al. Third- and fourth-degree perineal tears among primiparous women in England between 2000 and 2012: time trends and risk factors. BJOG. 2013;120(12):1516–25.
Rouse DJ, Weiner SJ, Bloom SL, et al. Second-stage labor duration in nulliparous women: relationship to maternal and perinatal outcomes. Am J Obstet Gynecol. 2009;201(4):357.e1–7.
Gimovsky AC, Berghella V. Randomized controlled trial of prolonged second stage: extending the time limit vs usual guidelines. Am J Obstet Gynecol. 2016;214(3):361.e1–6.
Sveinsdottir E, Gottfredsdottir H, Vernhardsdottir AS, Tryggvadottir GB, Geirsson RT. Effects of an intervention program for reducing severe perineal trauma during the second stage of labor. Birth. 2019;46(2):371–8.
ACOG. Practice bulletin: clinical management guidelines for obstetrician–Gynecologists number 76, October 2006: postpartum hemorrhage. Obstet Gynecol. 2006;108(4):1039–47.
Tuncalp O, Souza JP, Gulmezoglu M. New WHO recommendations on prevention and treatment of postpartum hemorrhage. Int J Gynaecol Obstet. 2013;123(3):254–6.
World Health Organization. WHO recommendations for the prevention and treatment or postpartum haemorrhage: evidence base. Geneva: World Health Organization. 2012.
Dahlke JD, Mendez-Figueroa H, Maggio L, et al. Prevention and management of postpartum hemorrhage: a comparison of 4 national guidelines. Am J Obstet Gynecol. 2015;213(1):76.e1–10.
Jiang H, Qian X, Carroli G, Garner P. Selective versus routine use of episiotomy for vaginal birth. Cochrane Database Syst Rev. 2017;2:CD000081.
De Jonge A, van Diem MT, Scheepers PL, van der Pal-de Bruin KM, Lagro-Janssen AL. Increased blood loss in upright birthing positions originates from perineal damage. BJOG. 2007;114(3):349–55.
Gupta JK, Sood A, Hofmeyr GJ, Vogel JP. Position in the second stage of labour for women without epidural anaesthesia. Cochrane Database Syst Rev. 2017;5:CD002006.
Walker KF, Kibuka M, Thornton JG, Jones NW. Maternal position in the second stage of labour for women with epidural anaesthesia. Cochrane Database Syst Rev. 2018;11:CD008070.
Funding
Coordenação de Aperfeiçoamento de Pessoal de Nível Superior (CAPES) code 001.
Author information
Authors and Affiliations
Contributions
G.M. Pereira: project development, data extraction/analysis, manuscript writing/editing; L.G. Brito: project development, data analysis, manuscript writing/editing; R.S. Hosoume: data extraction, manuscript writing/editing; M.V. Monteiro, C.R. Juliato: data analysis and manuscript editing.
Corresponding author
Ethics declarations
Conflicts of interests
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Pereira, G.M.V., Hosoume, R.S., de Castro Monteiro, M.V. et al. Selective episiotomy versus no episiotomy for severe perineal trauma: a systematic review with meta-analysis. Int Urogynecol J 31, 2291–2299 (2020). https://doi.org/10.1007/s00192-020-04308-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-020-04308-2