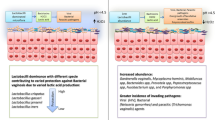
Abstract
Introduction and hypothesis
The current etiology of interstitial cystitis/painful bladder syndrome (IC/PBS) is poorly understood and multifactorial. Recent studies suggest the female urinary microbiota (FUM) contribute to IC/PBS symptoms. This study was designed to determine if the FUM, analyzed using mid-stream voided urine samples, differs between IC/PBS patients and controls.
Methods
This prospective case-controlled study compared the voided FUM of women with symptoms of urinary frequency, urgency, and bladder pain for > 6 months with the voided FUM of healthy female controls without pain. Bacterial identification was performed using 16S rRNA gene sequencing and EQUC, a validated enhanced urine culture approach. Urotype was defined by a genus present at > 50% relative abundance. If no genus was present above this threshold, the urotype was classified as ‘mixed.’ Group comparisons were performed for urotype and diversity measures.
Results
A mid-stream voided specimen was collected from 21 IC/PBS patients and 20 asymptomatic controls. The two groups had similar demographics. Urotypes did not differ between cohorts as assessed by either EQUC or 16S rRNA gene sequencing. We detected no significant differences between cohorts by alpha diversity. Cohorts also were not distinct using principle component analysis or hierarchical clustering. Detection by EQUC of bacterial species considered uropathogenic was high in both cohorts, but detection of these uropathogenic species did not differ between groups (p = 0.10).
Conclusions
Enhanced culture and DNA sequencing methods provide evidence that IC/PBS symptoms may not be related to differences in the FUM, at least not its bacterial components. Future larger studies are needed to confirm this preliminary finding.


Similar content being viewed by others
References
Bogart LM, Berry SH, Clemens JQ. Symptoms of interstitial cystitis, painful bladder syndrome and similar diseases in women: a systematic review. J Urol. 2007;177(2):450–6. https://doi.org/10.1016/j.juro.2006.09.032.
Hanno PM, Erickson D, Moldwin R, Faraday MM. Diagnosis and treatment of interstitial cystitis/bladder pain syndrome: AUA guideline amendment. J Urol. 2015;193(5):1545–53. https://doi.org/10.1016/j.juro.2015.01.086.
Wolfe AJ, Toh E, Shibata N, et al. Evidence of uncultivated bacteria in the adult female bladder. J Clin Microbiol. 2012;50(4):1376–83. https://doi.org/10.1128/JCM.05852-11.
Fouts DE, Pieper R, Szpakowski S, et al. Integrated next-generation sequencing of 16S rDNA and metaproteomics differentiate the healthy urine microbiome from asymptomatic bacteriuria in neuropathic bladder associated with spinal cord injury. J Transl Med. 2012;10:174. https://doi.org/10.1186/1479-5876-10-174.
Khasriya R, Sathiananthamoorthy S, Ismail S, et al. Spectrum of bacterial colonization associated with urothelial cells from patients with chronic lower urinary tract symptoms. J Clin Microbiol. 2013;51(7):2054–62. https://doi.org/10.1128/JCM.03314-12.
Hilt EE, McKinley K, Pearce MM, et al. Urine is not sterile: use of enhanced urine culture techniques to detect resident bacterial flora in the adult female bladder. J Clin Microbiol. 2014;52(3):871–6. https://doi.org/10.1128/JCM.02876-13.
Pearce MM, Hilt EE, Rosenfeld AB, et al. The female urinary microbiome: a comparison of women with and without urgency urinary incontinence. MBio. 2014;5(4):1283. https://doi.org/10.1128/mBio.01283-14. Accessed Jan 9, 2019.
Pearce MM, Zilliox MJ, Rosenfeld AB, et al. The female urinary microbiome in urgency urinary incontinence. Am J Obstet Gynecol. 2015;213(3):11. https://doi.org/10.1016/j.ajog.2015.07.009.
Karstens L, Asquith M, Davin S, et al. Does the urinary microbiome play a role in urgency urinary incontinence and its severity? Front Cell Infect Microbiol. 2016;6:78. https://doi.org/10.3389/fcimb.2016.00078. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4961701/.
Thomas-White KJ, Hilt EE, Fok C, et al. Incontinence medication response relates to the female urinary microbiota. Int Urogynecol J. 2016;27(5):723–33. https://doi.org/10.1007/s00192-015-2847-x.
Thomas-White KJ, Gao X, Lin H, et al. Urinary microbes and postoperative urinary tract infection risk in urogynecologic surgical patients. Int Urogynecol J. 2018;29(12):1797–805. https://doi.org/10.1007/s00192-018-3767-3.
Fok CS, Gao X, Lin H, et al. Urinary symptoms are associated with certain urinary microbes in urogynecologic surgical patients. Int Urogynecol J. 2018;29(12):1765–71. https://doi.org/10.1007/s00192-018-3732-1.
Abernethy MG, Rosenfeld A, White JR, Mueller MG, Lewicky-Gaupp C, Kenton K. Urinary microbiome and cytokine levels in women with interstitial cystitis. Obstet Gynecol. 2017;129(3):500–6. https://doi.org/10.1097/AOG.0000000000001892.
Nickel JC, Stephens A, Landis JR, et al. Assessment of the lower urinary tract microbiota during symptom flare in women with urologic chronic pelvic pain syndrome: a MAPP network study. J Urol. 2016;195(2):356–62. https://doi.org/10.1016/j.juro.2015.09.075.
Siddiqui H, Lagesen K, Nederbragt AJ, Jeansson SL, Jakobsen KS. Alterations of microbiota in urine from women with interstitial cystitis. BMC Microbiol. 2012;12:205. https://doi.org/10.1186/1471-2180-12-205.
Yuan S, Cohen DB, Ravel J, Abdo Z, Forney LJ. Evaluation of methods for the extraction and purification of DNA from the human microbiome. PLoS One. 2012;7(3):e33865. https://doi.org/10.1371/journal.pone.0033865. https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0033865.
Schloss PD, Westcott SL, Ryabin T, et al. Introducing mothur: open-source, platform-independent, community-supported software for describing and comparing microbial communities. Appl Environ Microbiol. 2009;75(23):7537–41. https://doi.org/10.1128/AEM.01541-09.
Edgar RC, Haas BJ, Clemente JC, Quince C, Knight R. UCHIME improves sensitivity and speed of chimera detection. Bioinformatics. 2011;27(16):2194–200. https://doi.org/10.1093/bioinformatics/btr381. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3150044/.
Wang Q, Garrity GM, Tiedje JM, Cole JR. Naïve bayesian classifier for rapid assignment of rRNA sequences into the new bacterial taxonomy. Appl Environ Microbiol. 2007;73(16):5261–7. https://doi.org/10.1128/AEM.00062-07. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1950982/.
Acknowledgments
We thank Mary Tulke, RN, for overseeing patient recruitment and collection of demographic and clinical data.
Funding
R01: NIH grant from NIDDK awarded to Alan J. Wolfe (R01DK104718).
Grant from ICA (Interstitial Cystitis Association) awarded to Colleen Fitzgerald, Alan Wolfe and Larissa Bresler (PI).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Supplemental Figure 1
(DOCX 176 kb)
Supplemental Figure 2
(DOCX 77 kb)
Rights and permissions
About this article
Cite this article
Bresler, L., Price, T.K., Hilt, E.E. et al. Female lower urinary tract microbiota do not associate with IC/PBS symptoms: a case-controlled study. Int Urogynecol J 30, 1835–1842 (2019). https://doi.org/10.1007/s00192-019-03942-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-019-03942-9