Abstract
Introduction and hypothesis
We used clinical examination and transperineal 3D/4D ultrasound (US) to evaluate pelvic floor muscles (PFM) after different delivery modes.
Methods
Women were surveyed using validated questionnaires. PFM were evaluated and classified according to the Modified Oxford Scale following 3D/4D transperineal US. For statistical analysis, Kruskal–Wallis, Mann–Whitney, chi-square, and Fisher exact tests were used.
Results
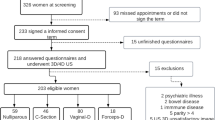
Fifty-three women were evaluated: 32 with previous vaginal delivery (VD) and 21 with cesarean section (CS) (8 nonelective and 13 elective). No significant difference among groups was observed regarding urinary incontinence (UI) after delivery (p = 0.39), loss of muscle strength referred by the patient (p = 0.48), or evaluated through digital examination (p = 0.87). No patient with elective CS had avulsion, with difference between VD and elective CS (p = 0.008). US evaluation identified no differences in bladder-neck elevation (p = 0.69) or descent (p = 0.65) , and no difference in genital hiatus size (p = 0.35), levator ani thickness (p = 0.35 –0.44), or presence of major or minor levator ani avulsion (p = 0.10).
Conclusions
We evaluated primiparous women within 12 to 24 months of delivery and found that VD was associated with PFM avulsion. There was no difference among VD and nonelective or elective CS in symptomatology or other anatomic alterations evaluated through 3D/4D transperineal US.


Similar content being viewed by others
Abbreviations
- PFD:
-
Pelvic floor dysfunction
- VD:
-
Vaginal delivery
- PFM:
-
Pelvic floor muscle
- US:
-
Ultrasound
- CS:
-
Cesarean section
- ICIQ-VS:
-
International Consultation on Incontinence Questionnaire–Vaginal Symptoms
- ICIQ-SF:
-
International Consultation on Incontinence Questionnaire–Short Form
- POP-Q:
-
Pelvic Organ Prolapse Quantification system
- BN:
-
Bladder neck
- TUI:
-
Tomographic ultrasound imaging
References
Haylen BT, Ridder DD, Freeman RM, Swift SE, Berghmans B, Lee J, et al. An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. Neurourol Urodyn. 2010;29:4–20.
Memon H, Handa VL. Pelvic floor disorders following vaginal or cesarean delivery. Curr Opin Obstet Gynecol. 2012;24(5):349–54.
Huser M, Janku P, Hudecek R, Zbozinkova Z, Bursa M, Unzeitig V, et al. Pelvic floor dysfunction after vaginal and cesarean delivery among singleton primiparas. Int J Gynecol Obstet. 2017;137(2):170–3.
Tähtinen RM, Cartwright R, Tsui JF, Aaltonen RL, Aoki Y, Cárdenas JL, et al. Long-term impact of mode of delivery on stress urinary incontinence and urgency urinary incontinence: a systematic review and meta-analysis. Eur Urol. 2016;70(1):148–58.
Alperin M, Cook M, Tuttle LJ, Esparza MC, Lieber RL. Impact of vaginal parity and aging on the architectural design of pelvic floor muscles. Am J Obstet Gynecol. 2016;215(3):312 e–1-9.
Dietz HP. Pelvic floor trauma following vaginal delivery. Curr Opin Obstet Gynecol. 2006;18:528–37.
Tan L, Shek KL, Atan IK, Rojas RG, Dietz HP. The repeatability of sonographic measures of functional pelvic floor anatomy. Int Urogynecol J. 2015;26(11):1667–72.
de Oliveira MS, Tamanini JTN, de Aguiar Cavalcanti G. Validation of the prolapse quality-of-life questionnaire (P-QoL) in Portuguese version in Brazilian women. Int Urogynecol J Pelvic Floor Dysfunct. 2009;20(10):1191–202.
Nunes Tamanini JT, Dambros M, D’Ancona CAL, Rodrigues Palma PC, Rodrigues NN. Validação para o português do “International Consultation on Incontinence Questionnaire - Short Form” (ICIQ-SF). Rev Saude Publica. 2004;38(3):438–44.
Bump RC, Mattiasson A, Bø K, Brubaker LP, DeLancey JO, Klarskov P, et al. The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol. 1996;175(1):10–7.
Laycock J, Jerwood D. Pelvic floor muscle assessment: the PERFECT scheme. Physiotherapy. 2001;87(12):631–42.
Naranjo-Ortiz C, Shek KL, Martin AJ, Dietz HP. What is normal bladder neck anatomy? Int Urogynecol J. 2016;27(6):945–50.
Shek KL, Dietz HP. The urethral motion profile: a novel method to evaluate urethral support and mobility. Aust New Zeal J Obstet Gynecol. 2008;48(3):337–42.
Albrich S, Laterza RM, Skala C, Salvatore S, Koelbl H, Naumann G. Impact of the mode of delivery on levator morphology: a prospective observational study with three-dimensional ultrasound early in the postpartum period. BJOG. 2012;119(1):51–60.
Dietz HP, Bernardo MJ, Kirby A, Shek KL. Minimal criteria for the diagnosis of avulsion of the puborectalis muscle by tomographic ultrasound. Int Urogynecol J. 2011;22(6):699–704.
Dietz HP. Pelvic floor trauma in childbirth. Aust N Z J Obstet Gynaecol. 2013;53(3):220–30.
Cassadó Garriga J, Pessarrodona Isern A, Espuña Pons M, Duran Retamal M, Felgueroso Fabrega A, Rodriguez Carballeira M, et al. Four-dimensional sonographic evaluation of avulsion of the levator ani according to delivery mode. Ultrasound Obstet Gynecol. 2011;38(6):701–6.
van Delft K, Sultan AH, Thakar R, Schwertner-Tiepelmann N, Kluivers K. The relationship between postpartum levator ani muscle avulsion and signs and symptoms of pelvic floor dysfunction. BJOG. 2014;121(9):1164–71.
Siafarikas F, Staer-Jensen J, Hilde G, Bø K, Ellström Engh M. The levator ani muscle during pregnancy and major levator ani muscle defects diagnosed postpartum: a three- and four-dimensional transperineal ultrasound study. BJOG. 2015;122(8):1083–91.
Volløyhaug I, van Grutin I, van Delft K, Sultan AH, Thakar R. Is bladder neck and urethral mobility associated with urinary incontinence and mode of delivery 4 years after childbirth? Neurourol Urodyn. 2016;9999:1–8.
Staer-Jensen J, Siafarikas F, Hilde G, Benth JS, Bo K, Engh ME. Postpartum recovery of levator hiatus and bladder neck mobility in relation to pregnancy. Obstet Gynecol. 2015;125(3):531–9.
Hannah M, Whyte H, Hewson S. Maternal outcomes at 2 years after planned cesarean section versus planned vaginal birth for breech presentation at term: the international randomized term breech trial. Am J Obstet Gynecol. 2004;191:917–27.
Jundt K, Scheer I, Schiessl B, Karl K, Friese K, Peschers U. Incontinence, bladder neck mobility, and sphincter ruptures in primiparous women. Eur J Med Res. 2010;15(6):246–52.
Dietz HP, Shek C, Clarke B. Biometry of the pubovisceral muscle and levator hiatus by three-dimensional pelvic floor ultrasound. Ultrasound Obstet Gynecol. 2005;25(6):580–5.
Shek KL, Dietz HP. Intrapartum risk factors for levator trauma. BJOG. 2010;117(12):1485–92.
Ferreira CW, Atan IK, Martin A, Shek KL, Dietz HP. Pelvic organ support several years after a first birth. Int Urogynecol J. 2017;28(10):1499–1505.
Ashton-Miller JA, DeLancey JOL. On the biomechanics of vaginal birth and common aequelae. Annu Rev Biomed Eng. 2009;11:163–76.
Asch DA, Jedrziewski MK, Christakis NA. Response rates to mail surveys published in medical journals. J Clin Epidemiol. 1997;50(10):1129–36.
Kellerman SE, Herold J. Physician response to surveys. A review of the literature. Am J Prev Med. 2001;20(1):61–7.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Rights and permissions
About this article
Cite this article
Araujo, C.C., Coelho, S.S.A., Martinho, N. et al. Clinical and ultrasonographic evaluation of the pelvic floor in primiparous women: a cross-sectional study. Int Urogynecol J 29, 1543–1549 (2018). https://doi.org/10.1007/s00192-018-3581-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-018-3581-y