Abstract
Introduction
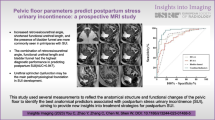
Vaginal delivery can lead to pelvic floor disorders. Many authors have described pelvic floor injuries that can predict future defects such as urinary incontinence and pelvic organ prolapse. We propose the assessment of urinary stress incontinence and its association with levator ani muscle (LAM) microtrauma (>20% in the levator hiatus area during Valsalva) and macrotraumas (avulsion) identified by 3/4D transperineal ultrasound (3D-TpUS) 36 months post-partum.
Materials and methods
This was a prospective observational study including 168 nulliparous women. All patients included were nulliparous with singleton gestation in cephalic presentation, at ≥37 weeks and were recruited on the first day after delivery. Thirty-six months after delivery, 3D-TpUS was carried out to identify LAM lesions (macro or micro). Clinical assessment of urinary stress incontinence (USI) was based on the ICIQ-UI-SF test; a simple stress test and urodynamic test were carried out in the same visit.
Results
A total of 105 nulliparous women were studied (51 spontaneous deliveries [SpD] and 54 vacuum-assisted deliveries [VD]). Microtraumas were identified in 35.3% of SpD and 20.4% of VD. Macrotraumas (avulsion) were identified in 9.8% of SpD and 35.2% of VD (p = 0.006). No differences were found in USI between study groups or in relation to the identification of LAM defects (19.2% in the no lesion group, 25% in the macrotrauma and 13.8% in the microtrauma groups; p = not significant). Nor were significant differences found in the results from the different study groups in the International Consultation on Incontinence Modular Questionnaire Urinary Incontinence Short Form (ICIQ-UI SF) test (12.7±2.2 in the no lesion group, 12.5±4.2 in the macrotrauma and 13.25±4.8 in the microtrauma groups; p = NS).
Conclusion
No difference was observed in USI between patients with and without LAM lesions (microtrauma or macrotrauma) 36 months post-delivery.



Similar content being viewed by others
References
Boyles SH, Weber AM, Meyn L. Procedures for pelvic organ prolapse in the United States, 1979–1997. Am J Obstet Gynecol. 2003;188:108–15.
Anger JT, Saigal CS, Litwin MS. Urologic Diseases of America Project. The prevalence of urinary incontinence among community dwelling adult women: results from the National Health and Nutrition Examination Survey. J Urol. 2006;175:601–4.
Dannecker C, Anthuber C. The effects of childbirth on the pelvic-floor. J Perinat Med. 2000;28:175–84.
Dietz HP, Simpson JM. Levator trauma is associated with pelvic organ prolapse. BJOG. 2008;115:979–84.
DeLancey JO, Kearney R, Chou Q, Speights S, Binno S. The appearance of levator ani muscle abnormalities in magnetic resonance images after vaginal delivery. Obstet Gynecol. 2003;101:46–53.
Peschers UM, Schaer GN, DeLancey JO, Schuessler B. Levator ani function before and after childbirth. Br J Obstet Gynaecol. 1997;104:1004–8.
Sze EH, Sherard GB, Dolezal JM. Pregnancy, labor, delivery and pelvic organ prolapse. Obstet Gynecol. 2002;100:981–6.
Dolan LM, Hosker GL, Mallett VT, Allen RE, Smith AR. Stress incontinence and pelvic floor neurophysiology 15 years after the first delivery. BJOG. 2003;110:1107–14.
Shek K, Dietz HP. Intrapartum risk factors for levator trauma. BJOG. 2010;117:1485–92.
Dietz HP, Lanzarone V. Levator trauma after vaginal delivery. Obstet Gynecol. 2005;106:707–12.
García-Mejido JA, Gutierrez-Palomino L, Borrero C, Valdivieso P, Fernandez-Palacin A, Sainz-Bueno JA. Factors that influence the development of avulsion of the levator ani muscle in eutocic deliveries: 3-4D transperineal ultrasound study. J Matern Fetal Neonatal Med. 2015;4:1–4.
Salter SA, Batra RS, Rohrer TE, Kohli N, Kimball AB. Striae and pelvic relaxation: two disorders of connective tissue with a strong association. J Invest Dermatol. 2006;126:1745–8.
Albrich SB, Laterza RM, Skala C, Salvatore S, Koelbl H, Naumann G. Impact of mode of delivery on levator morphology: a prospective observational study with three dimensional ultrasound early in the postpartum period. BJOG. 2012;119(1):51–60.
Shek K, Dietz H. The effect of childbirth on hiatal dimensions. Obstet Gynecol. 2009;113:1272–8.
Steensma AB, Konstantinovic ML, Burger CW, de Ridder D, Timmerman D, Deprest J. Prevalence of major levator abnormalities in symptomatic patients with an underactive pelvic floor contraction. Int Urogynecol J. 2010;21(7):861–7.
Unger CA, Weinstein MM, Pretorius DH. Pelvic floor imaging. Obstet Gynecol Clin N Am. 2011;38(1):23–43.
Kruger JA, Heap SW, Murphy BA, Dietz HP. Pelvic floor function in nulliparous women using three-dimensional ultrasound and magnetic resonance imaging. Obstet Gynecol. 2008;111:631–8.
Schwertner-Tiepelmann N, Thakar R, Sultan AH, Tunn R. Obstetric levator ani muscle injuries: current status. Ultrasound Obstet Gynecol. 2012;39(4):372–83. doi:10.1002/uog.11080.
Dietz HP, Shek C, Clarke B. Biometry of the pubovisceral muscle and levator hiatus by three-dimensional pelvic floor ultrasound. Ultrasound Obstet Gynecol. 2005;25:580–85.
Braekken IH, Majida M, Engh ME, Bø K. Test-retest reliability of pelvic floor muscle contraction measured by 4D ultrasound. Neurourol Urodyn. 2009;28:68–73.
Timmermans L, De Mol J, Mélot C, Falez F. Correlation between ICIQ-UI-SF score and personality testing results over a urinary incontinent population. Prog Urol. 2016;26(4):230–6. doi:10.1016/j.purol.2015.11.003.
Avery K, Donovan J, Peters TJ, Shaw C, Gotoh M, Abrams P. ICIQ: a brief and robust measure for evaluating the symptoms and impact of urinary incontinence. Neurourol Urodyn. 2004;23(4):322–30.
Van Brummen HJ, Bruinse HW, van de Pol G, Heintz AP, van der Vaart CH. Bothersome lower urinary tract symptoms 1 year after first delivery: prevalence and effect of childbirth. BJU Int. 2006;98:89–95.
Dickie KJ, Shek KL, Dietz HP. The relationship between urethral mobility and parity. BJOG. 2010;117(10):1220–4.
Falkert A, Willmann A, Endress E, Meint P, Seelbach-Göbel B. Three-dimensional ultrasound of pelvic floor: is there a correlation with delivery mode and persisting pelvic floor disorders 18–24 months after first delivery? Ultrasound Obstet Gynecol. 2013;41:204–9.
Oversand S, Atan IK, Shek KL, Dietz HP. The association of urinary and anal incontinence with measures of pelvic floor muscle contractility. Ultrasound Obstet Gynecol. 2015;47(5):642–5.
Santoro GA, Wieczorek AP, Dietz HP, Mellgren A, Sultan A, Shobeiri SA, et al. State of the art: an integrated approach to pelvic floor ultrasonography. Ultrasound Obstet Gynecol. 2011;37:381–96.
Eisenberg VH, Chantarasorn V, Shek KL, Dietz HP. Does levator ani injury affect cystocele type? Ultrasound Obstet Gynecol. 2010;36:618–23.
Wu QK, MAO XY, Luo LM, Ying T, Li Q, Teng YC. Characteristics of pelvic diaphragm hiatus in pregnant women with stress urinary incontinence detected by transperineal three-dimensional ultrasound. Zhonghua Fu Chan Ke Za Zhi. 2010;45(5):326–30.
Stachowicz N, Stachowicz S, Smolen A, Morawska D, Kotarski J. Sonographic evaluation of the levator ani muscle in women with stress urinary incontinence. Ginekol Pol. 2012;83(9):669–73.
Hantoushzadeh S, Javadian P, Shariat M, Salmanian B, Ghazizadeh S, Aghssa M. Stress urinary incontinence: pre-pregnancy history and effects of mode of delivery on its postpartum persistency. Int J Urogynecol. 2011;22(6):651–5. doi:10.1007/s00192-010-1335-6.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflicts of interest
None.
Rights and permissions
About this article
Cite this article
García Mejido, J.A., Valdivieso Mejias, P., Fernández Palacín, A. et al. Evaluation of isolated urinary stress incontinence according to the type of levator ani muscle lesion using 3/4D transperineal ultrasound 36 months post-partum. Int Urogynecol J 28, 1019–1026 (2017). https://doi.org/10.1007/s00192-016-3208-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-016-3208-0