Abstract
Introduction and hypothesis
This study describes a technique to quantify muscle fascicle directions in the levator ani (LA) and tests the null hypothesis that the in vivo fascicle directions for each LA subdivision subtend the same parasagittal angle relative to a horizontal reference axis.
Methods
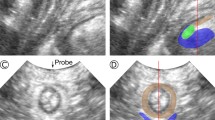
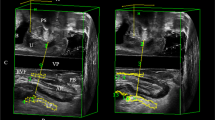
Visible muscle fascicle direction in the each of the three LA muscle subdivisions, the pubovisceral (PVM; synonymous with pubococcygeal), puborectal (PRM), and iliococcygeal (ICM) muscles, as well as the external anal sphincter (EAS), were measured on 3-T sagittal MRI images in a convenience sample of 14 healthy women in whom muscle fascicles were visible. Mean ± standard deviation (SD) angle values relative to the horizontal were calculated for each muscle subdivision. Repeated measures ANOVA and post-hoc paired t tests were used to compare muscle groups.
Results
Pubovisceral muscle fiber inclination was 41 ± 8.0°, PRM was −19 ± 10.1°, ICM was 33 ± 8.8°, and EAS was −43 ± 6.4°. These fascicle directions were statistically different (p < 0.001). Pairwise comparisons among levator subdivisions showed angle differences of 60° between PVM and PRM, and 52° between ICM and PRM. An 84° difference existed between PVM and EAS. The smallest angle difference between levator divisions was between PVM and ICM 8°. The difference between PRM and EAS was 24°. All pairwise comparisons were significant (p < 0.001).
Conclusions
The null hypothesis that muscle fascicle inclinations are similar in the three subdivisions of the levator ani and the external anal sphincter was rejected. The largest difference in levator subdivision inclination, 60°, was found between the PVM and PRM.



Similar content being viewed by others
Notes
In the rest of this paper we use the term muscle “fiber” instead of muscle fascicle because the term muscle “fiber” is more commonly used in the clinical literature. Given the assumption that the direction of the fiber is collinear with its fascicle as visualized on MRI this seems acceptable.
References
DeLancey JO, Morgan DM, Fenner DE, Kearney R, Guire K, Miller JM, Hussain H, Umek W, Hsu Y, Ashton-Miller JA (2007) Comparison of levator ani muscle defects and function in women with and without pelvic organ prolapse. Obstet Gynecol 109(2 Pt 1):295–302
Dietz HP, Simpson JM (2008) Levator trauma is associated with pelvic organ prolapse. BJOG 115(8):979–984
Terminologia Anatomica: International Anatomical Terminology. Stuttgart: Thieme, 1998. http://www.unifr.ch/ifaa/
Lawson J (1974) Pelvic anatomy. I. Pelvic floor muscles. Ann R Coll Surg Engl 54:244–252
Margulies RU, Huebner M, DeLancey JO (2007) Origin and insertion points involved in levator ani muscle defects. Am J Obstet Gynecol 196:251–255
DeLancey JO, Sørensen HC, Lewicky-Gaupp C, Smith TM (2012) Comparison of the puborectal muscle on MRI in women with POP and levator ani defects with those with normal support and no defect. Int Urogynecol J 23(1):73–77. doi:10.1007/s00192-011-1527-8
MacIntosh BR, Gardiner PF, McComas AJ (2006) Muscle architecture and muscle fiber anatomy; Chapter 11: Muscle contraction, p 151–174. In: Skeletal muscle: form and function. Human Kinetics, Champaign, IL, pp 3–21
Law YM, Fielding JR (2008) MRI of pelvic floor dysfunction: review. AJR Am J Roentgenol 191 (6 Suppl):S45–S53
Morris VC, Murray MP, DeLancey JO, Ashton-Miller JA (2012) A comparison of the effect of age on levator ani and obturator internus muscle cross-sectional areas and volumes in nulliparous women. Neurourol Urodyn 31(4):481–486
Margulies RU, Hsu Y, Kearney R, Stein T, Umek WH, DeLancey JO (2006) Appearance of the levator ani muscle subdivisions in magnetic resonance images. Obstet Gynecol 107(5):1064–1069
Zijat FM, Froeling M, van der Paardt MP, Lakeman MME, Bipat S, Montauban van Swijndregt AD, Strijkers GJ, Nederveen AJ, Stoker J (2011) Feasibility of diffusion tensor imaging (DTI) with fibre tractography of the normal female pelvic floor. Eur Radiol 21:1243–1249
Brandão S, Da Roza T, Parente M, Ferreira HA, Mascarenhas T, Ramos I, Jorge RN (2012) Magnetic resonance tractography as a means to evaluate pubovisceral muscle fibers. Abstract 293 IUGA Brisbane
Rousset P, Delmas V, Buy JN, Rahmouni A, Vadrot D, Deux JF (2012) In vivo visualization of the levator ani muscle subdivisions using MR fiber tractography with diffusion tensor imaging. J Anat 221(3):221–228. doi:10.1111/j.1469-7580.2012.01538.x
Clark NA, Brincat CA, Yousuf AA, DeLancey JO (2010) Levator defects affect perineal position independently of prolapse status. Am J Obstet Gynecol 203(6):595.e17–595.e22
Guaderrama NM, Nager CW, Liu J, Pretorius DH, Mittal RK (2005) The vaginal pressure profile. Neurourol Urodyn 24(3):243–247
Miller JM, Brandon C, Jacobson JA, Low LK, Zielinski R, Ashton-Miller J, Delancey JO (2010) MRI findings in patients considered high risk for pelvic floor injury studied serially after vaginal childbirth. AJR Am J Roentgenol 195(3):786–791. doi:10.2214/AJR.09.3508
Brandon C, Jacobson J, Low L, Park L, DeLancey JO, Miller J (2012) Pubic bone injuries in primiparous women: magnetic resonance imaging in detection and differential diagnosis of structural injury. Ultrasound Obstet Gynecol 39(4):444–451
Hsu Y, Fenner DE, Weadock WJ, DeLancey JO (2005) Magnetic resonance imaging and 3-dimensional analysis of external anal sphincter anatomy. Obstet Gynecol 106(6):1259–1265
Betschart C, Chen L, Ashton-Miller JA, DeLancey JO (2013) On pelvic reference lines and the MR evaluation of genital prolapse: a proposal for standardization using the Pelvic Inclination Correction System. Int Urogynecol J 24(9):1421–1428
Raizada V, Bhargava V, Jung SA, Karstens A, Pretorius D, Krysl P, Mittal RK (2010) Dynamic assessment of the vaginal high-pressure zone using high-definition manometery, 3-dimensional ultrasound, and magnetic resonance imaging of the pelvic floor muscles. Am J Obstet Gynecol 203(2):172.e1–8
Lewicky-Gaupp C, Yousuf A, Larson KA, Fenner DE, DeLancey JO (2010) Structural position of the posterior vagina and pelvic floor in women with and without posterior vaginal prolapse. Am J Obstet Gynecol 202(5):497.e1–497.e6
Hsu Y, Chen L, Huebner M, Ashton-Miller JA, DeLancey JO (2006) Quantification of levator ani cross-sectional area differences between women with and those without prolapse. Obstet Gynecol 108(4):879–883
Kearney R, Sawhney R, DeLancey JO (2004) Levator ani muscle anatomy evaluated by origin-insertion pairs. Obstet Gynecol 104(1):168–173
Roberts WH, Harrison CW, Mitchell DA, Fischer HF (1988) The levator ani muscle and the nerve supply of its puborectalis component. Clin Anat 1:256–283
Janda S, van der Helm FC, de Blok SB (2003) Measuring morphological parameters of the pelvic floor for finite element modeling purposes. J Biomech 36(6):749–757
Richter K (1966) Lebendige Anatomie der Vagina. Geburtshilfe Frauenheilkd 26:1213–1223
Rociu E, Stoker J, Eijkemans MJ, Laméris JS (2000) Normal anal sphincter anatomy and age- and sex-related variations at high-spatial-resolution endoanal MR imaging. Radiology 217(2):395–401
Zacharin RF (1977) “A Chinese anatomy”—the supporting tissues of the Chinese and Occidental female compared and contrasted. Aust N Z J Obstet Gynaecol 17:1–11
Hodgson JA, Finni T, Lai AM, Edgerton VR, Sinha S (2006) Influence of structure on the tissue dynamics of the human soleus muscle observed in MRI studies during isometric contractions. J Morphol 267(5):584–601
Chen L, Hsu Y, Ashton-Miller JA, DeLancey JO (2006) Measurement of the pubic portion of the levator ani muscle in women with unilateral defects in 3-D models from MR images. Int J Gynecol Obstet 92(3):234–241
Acknowledgements
We gratefully acknowledge the intellectual contribution of Catherine Brandon, MD, Musculoskeletal Division, Department of Radiology, University of Michigan, and her assistance in obtaining the high-quality MR images for this study, and Prof. Burkhardt Seifert, Division of Biostatistics, University of Zurich, for his contribution to the data analysis.
Institutional review board approval
IRB University of Michigan 2005-0011 (EMRLD) and IRB 1999-0395.
Funding
EMRLD (Evaluating Maternal Recovery from Labor & Delivery) funded by NIH ORWH SCOR P50 HD044406, OPAL II funded by RO1 HD 38665; grant to CB from the Swiss National Science Foundation.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Betschart, C., Kim, J., Miller, J.M. et al. Comparison of muscle fiber directions between different levator ani muscle subdivisions: in vivo MRI measurements in women. Int Urogynecol J 25, 1263–1268 (2014). https://doi.org/10.1007/s00192-014-2395-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-014-2395-9